 Back
BackMuscles and Muscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Overview of Muscle Tissue
Types of Muscle Tissue
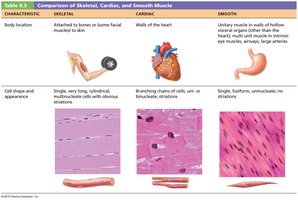
Muscle tissue is specialized for contraction and is responsible for movement in the body. There are three main types of muscle tissue, each with distinct characteristics and functions:
Skeletal Muscle: Attached to bones and skin, responsible for voluntary movements, striated, and multinucleated.
Cardiac Muscle: Found only in the walls of the heart, striated, involuntary, and branched cells connected by intercalated discs.
Smooth Muscle: Located in the walls of hollow organs (e.g., stomach, bladder), non-striated, involuntary, and spindle-shaped cells.
Muscle Tissue Characteristics
Excitability (Responsiveness): Ability to receive and respond to stimuli.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched.
Elasticity: Ability to recoil to resting length after stretching.
Functions of Muscle Tissue
Movement: Locomotion and manipulation of the environment.
Posture: Maintaining body position.
Joint Stabilization: Supporting and stabilizing joints.
Heat Generation: Muscle contractions produce heat to maintain body temperature.
Additional Functions: Protect organs, form valves, control pupil size, and cause goosebumps.
Skeletal Muscle Anatomy
Structural Organization
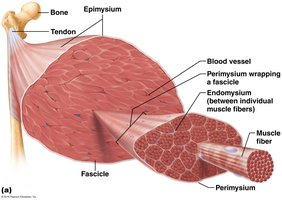
Skeletal muscle is an organ composed of muscle tissue, connective tissue, blood vessels, and nerves. It is organized into several hierarchical levels:
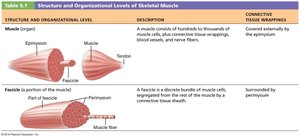
Muscle (organ) – Surrounded by epimysium.
Fascicle (bundle of fibers) – Surrounded by perimysium.
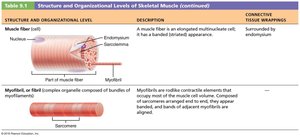
Muscle fiber (cell) – Surrounded by endomysium.
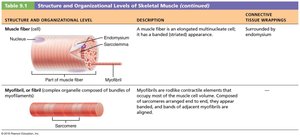
Myofibril – Contractile element within muscle fiber.
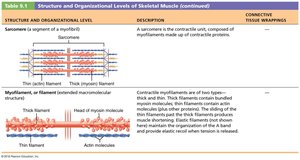
Sarcomere – Functional contractile unit within myofibril.
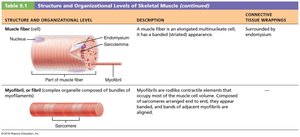
Connective Tissue Sheaths
Epimysium: Dense irregular connective tissue surrounding the entire muscle.
Perimysium: Fibrous connective tissue surrounding fascicles.
Endomysium: Fine areolar connective tissue surrounding each muscle fiber.
Muscle Attachments
Origin: Attachment to immovable or less movable bone.
Insertion: Attachment to movable bone.
Direct Attachment: Epimysium fused to periosteum or perichondrium.
Indirect Attachment: Connective tissue wrappings extend as tendon or aponeurosis.
Muscle Fiber Microanatomy
Muscle Fiber Structure
Skeletal muscle fibers are long, cylindrical, multinucleated cells containing specialized organelles for contraction:
Sarcolemma: Plasma membrane of muscle fiber.
Sarcoplasm: Cytoplasm containing glycosomes (glycogen storage) and myoglobin (O2 storage).
Myofibrils: Densely packed, rodlike elements responsible for muscle contraction and striations.
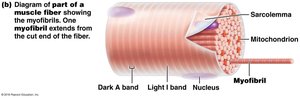

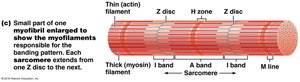
Myofibril Structure
Striations: Alternating dark (A bands) and light (I bands) regions.
Sarcomere: Smallest contractile unit, extends from Z disc to Z disc.
Myofilaments: Thick (myosin) and thin (actin) filaments arranged in a hexagonal pattern.
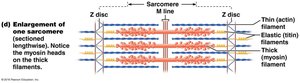
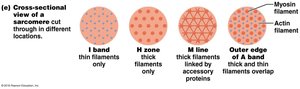
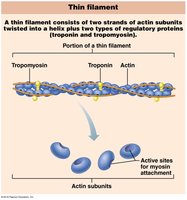
Molecular Composition of Myofilaments
Thick Filaments: Composed of myosin molecules with heads that form cross bridges during contraction.
Thin Filaments: Composed of actin, tropomyosin, and troponin. Actin subunits provide binding sites for myosin heads.
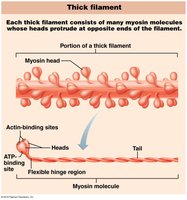
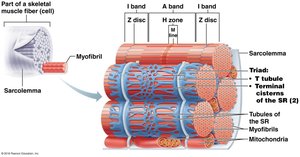
Sarcoplasmic Reticulum and T Tubules
Sarcoplasmic Reticulum (SR): Stores and releases Ca2+ for muscle contraction.
T Tubules: Invaginations of the sarcolemma that transmit action potentials deep into the muscle fiber.
Triad: Structure formed by a T tubule and two terminal cisterns of the SR.
Sliding Filament Model of Contraction
Mechanism of Contraction
Muscle contraction occurs when thin filaments slide past thick filaments, increasing their overlap without changing filament length. This process is initiated by the formation of cross bridges between actin and myosin heads.
Shortening: Z discs are pulled toward the M line, I bands shorten, H zones disappear, and A bands move closer together.

Muscle Fiber Contraction: The Neuromuscular Junction and Action Potential
Neuromuscular Junction (NMJ)
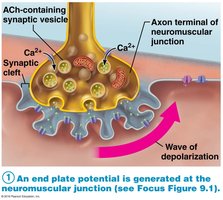
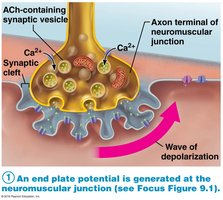
The NMJ is the site where a motor neuron communicates with a muscle fiber to initiate contraction. It consists of the axon terminal, synaptic cleft, and junctional folds of the sarcolemma.
Neurotransmitter: Acetylcholine (ACh) is released from synaptic vesicles and binds to receptors on the sarcolemma, triggering an action potential.
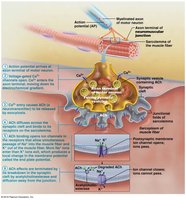
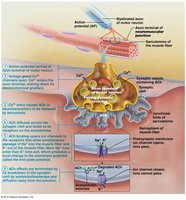
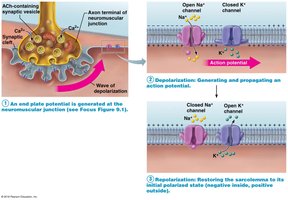
Generation of an Action Potential
End Plate Potential: Local depolarization caused by Na+ influx.
Depolarization: If threshold is reached, voltage-gated Na+ channels open, generating an action potential.
Repolarization: K+ channels open, restoring resting membrane potential.
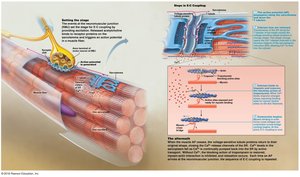
Excitation-Contraction (E-C) Coupling
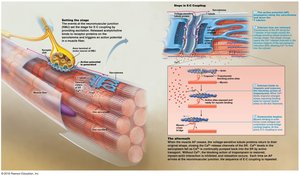
Linking Action Potential to Contraction
Excitation-contraction coupling describes the sequence of events by which an action potential leads to muscle contraction. The action potential travels along the sarcolemma and T tubules, triggering Ca2+ release from the SR, which initiates contraction.
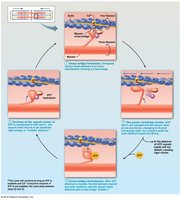
Cross Bridge Cycle
Formation: Myosin head attaches to actin.
Power Stroke: Myosin head pivots, pulling actin filament toward M line.
Detachment: ATP binds to myosin, causing detachment from actin.
Cocking: ATP hydrolysis re-energizes myosin head.
Whole Muscle Contraction
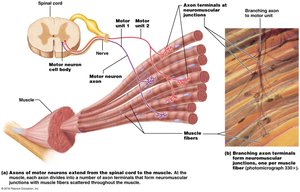
Motor Units and Muscle Twitch
Motor Unit: A motor neuron and all the muscle fibers it innervates.
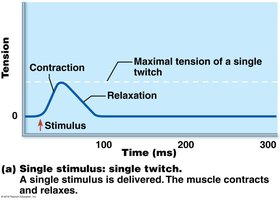
Muscle Twitch: Response of a muscle to a single stimulus, consisting of latent, contraction, and relaxation periods.
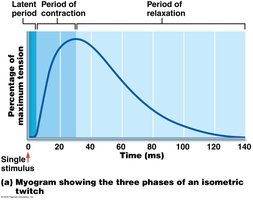
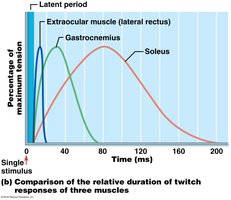
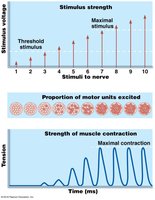
Graded Muscle Responses
Frequency Summation: Increased frequency of stimulation leads to wave summation and tetanus.
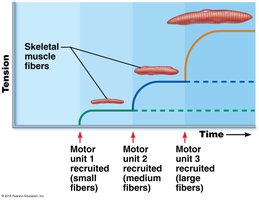
Strength Summation (Recruitment): Increased stimulus strength recruits more motor units for greater force.
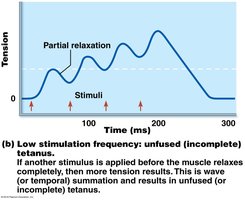
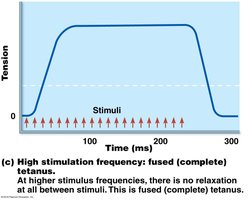
Muscle Tone
Muscle tone is the constant, slightly contracted state of all muscles, maintained by spinal reflexes. It keeps muscles firm, healthy, and ready to respond.
Energy for Muscle Contraction
ATP Regeneration Pathways
Direct Phosphorylation: Creatine phosphate donates a phosphate to ADP to form ATP.
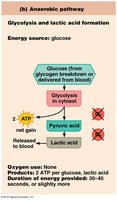
Anaerobic Glycolysis: Glucose is broken down to pyruvic acid and lactic acid, producing ATP without oxygen.
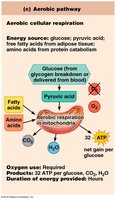
Aerobic Respiration: Glucose is completely broken down in the presence of oxygen, producing CO2, H2O, and a large amount of ATP.

Muscle Fatigue and Recovery
Muscle Fatigue: Inability to contract despite continued stimulation, often due to ionic imbalances.
Excess Postexercise Oxygen Consumption (EPOC): Oxygen required to restore muscle to pre-exercise state.
Factors Affecting Force, Velocity, and Duration of Contraction
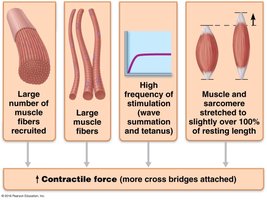
Force of Contraction
Number of muscle fibers recruited
Size of muscle fibers
Frequency of stimulation
Degree of muscle stretch (optimal sarcomere length: 80–120% of resting length)
Velocity and Duration of Contraction
Muscle Fiber Type: Slow oxidative, fast oxidative, and fast glycolytic fibers differ in speed, endurance, and metabolic pathways.
Load: Heavier loads decrease contraction velocity and duration.
Recruitment: More motor units increase contraction speed and duration.
Smooth Muscle
Microscopic Structure and Function
Spindle-shaped, uninucleate, non-striated cells
Arranged in longitudinal and circular layers in hollow organs
Contraction causes peristalsis (movement of substances through organs)
Contraction Mechanism
Ca2+ binds to calmodulin (not troponin)
Myosin light chain kinase phosphorylates myosin, enabling cross bridge formation
Contraction is slow, sustained, and energy-efficient
Types of Smooth Muscle
Unitary (Visceral) Smooth Muscle: Found in hollow organs, electrically coupled by gap junctions, can contract spontaneously.
Multiunit Smooth Muscle: Found in large airways, arteries, arrector pili, and iris; fibers act independently, controlled by autonomic nerves and hormones.
Characteristic | Skeletal | Cardiac | Smooth |
|---|---|---|---|
Body Location | Attached to bones or skin | Walls of the heart | Walls of hollow organs (except heart) |
Cell Shape & Appearance | Long, cylindrical, multinucleate, striated | Branching chains, uni- or binucleate, striated | Single, fusiform, uninucleate, non-striated |

