 Back
BackMuscles and Muscle Tissue: Structure, Function, and Contraction
Study Guide - Smart Notes

Muscle Tissue Overview
Introduction to Muscle Tissue
Muscle tissue is essential for movement, posture, joint stabilization, and heat generation in the human body. It transforms chemical energy (ATP) into mechanical energy, producing force and movement. There are three main types of muscle tissue: skeletal, cardiac, and smooth.
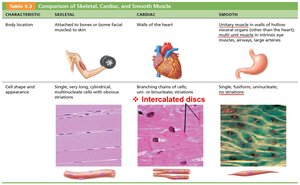
Skeletal muscle: Voluntary, striated, attached to bones, responsible for body movement.
Cardiac muscle: Involuntary, striated, found only in the heart, responsible for pumping blood.
Smooth muscle: Involuntary, non-striated, found in walls of hollow organs, responsible for movements like peristalsis.
Special Characteristics of Muscle Tissue
Key Properties
Excitability (responsiveness): Ability to receive and respond to stimuli by changing membrane potential.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched beyond resting length.
Elasticity: Ability to recoil to resting length after stretching.
Functions of Muscle Tissue
Movement: Muscles contract to produce movement of the body and substances within the body.
Posture and Position: Muscles maintain posture and body position through continuous adjustments.
Joint Stabilization: Muscle tone stabilizes joints.
Heat Generation: Muscle activity produces heat, important for maintaining body temperature.
Gross and Microscopic Anatomy of Skeletal Muscle
Organization of Skeletal Muscle
Skeletal muscle is an organ composed of muscle fibers, nerves, blood vessels, and connective tissue sheaths. Each muscle is served by an artery, veins, and a nerve. Muscle fibers are grouped into bundles called fascicles.
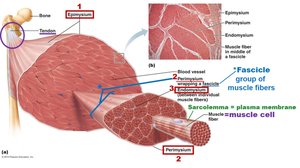
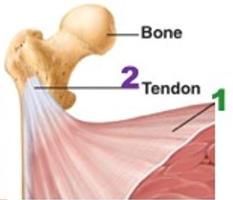
Muscle Attachments
Origin: Attachment to the immovable or less movable bone.
Insertion: Attachment to the movable bone.
Direct attachment: Epimysium fuses to periosteum of bone or perichondrium of cartilage.
Indirect attachment: Connective tissue wrappings extend beyond muscle as tendons (rope-like) or aponeuroses (sheet-like).
Microscopic Anatomy of a Muscle Fiber
Muscle fibers are long, cylindrical cells with multiple peripheral nuclei and abundant mitochondria for ATP production. They contain glycosomes (glycogen storage) and myoglobin (oxygen storage).
Myofibrils and Sarcomeres
Myofibrils are rod-like structures that run parallel to the muscle fiber's length and make up about 80% of cell volume. They are composed of repeating units called sarcomeres, the smallest contractile units of muscle fibers.
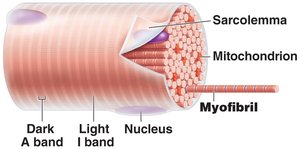
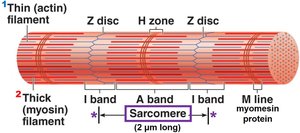
Sarcomere: Region between two Z discs; contains thick (myosin) and thin (actin) filaments.
Striations: Alternating dark (A bands) and light (I bands) due to arrangement of myofilaments.
Thick and Thin Filaments
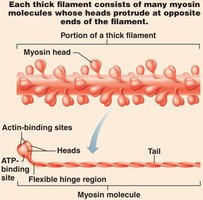
Thick filaments: Composed of myosin molecules with heads that form cross-bridges during contraction.
Thin filaments: Composed of actin, tropomyosin, and troponin. Tropomyosin blocks myosin-binding sites on actin; troponin binds actin, tropomyosin, and Ca2+.
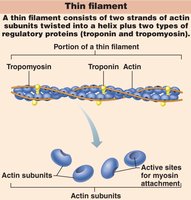
Sarcoplasmic Reticulum and T Tubules
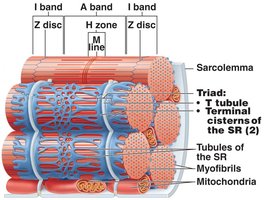
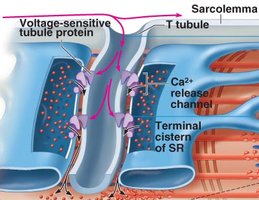
The sarcoplasmic reticulum (SR) stores and releases Ca2+ for muscle contraction. T tubules are invaginations of the sarcolemma that conduct action potentials deep into the muscle fiber, ensuring every myofibril is activated simultaneously. The triad consists of a T tubule and two terminal cisternae of the SR.
Sliding Filament Model of Contraction
Mechanism of Contraction
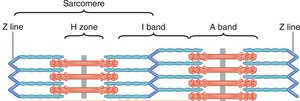
Muscle contraction occurs when myosin heads bind to actin, pulling thin filaments toward the M line, shortening the sarcomere and the muscle fiber. This process is powered by ATP hydrolysis.
Neuromuscular Junction and Muscle Excitation
Neuromuscular Junction (NMJ)
The NMJ is the site where a motor neuron communicates with a muscle fiber. It consists of the axon terminal, synaptic cleft, and the motor end plate (sarcolemma).
Release of acetylcholine (ACh) from the neuron triggers an action potential in the muscle fiber.
ACh binds to receptors, causing local depolarization (end plate potential).
Generation of an Action Potential
End plate potential: Local depolarization due to Na+ influx.
Depolarization: If threshold is reached, voltage-gated Na+ channels open, generating an action potential.
Repolarization: K+ efflux restores resting membrane potential.
Excitation-Contraction (E-C) Coupling
Linking Excitation to Contraction
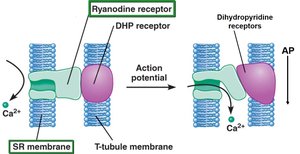
E-C coupling is the process by which an action potential triggers Ca2+ release from the SR, leading to cross-bridge cycling and muscle contraction. Dihydropyridine receptors (voltage sensors) and ryanodine receptors (Ca2+ channels) are key components.
Cross-Bridge Cycle
Cross-bridge formation: Myosin head binds to actin.
Power stroke: Myosin head pivots, pulling actin filament.
Cross-bridge detachment: ATP binds to myosin, causing detachment.
Cocking of myosin head: ATP hydrolysis re-energizes the myosin head.
This cycle continues as long as Ca2+ and ATP are available.
Motor Units and Muscle Twitch
Motor Unit
A motor unit consists of a motor neuron and all the muscle fibers it innervates. Motor units vary in size and control the precision and strength of muscle contraction.
Small motor units: Fine control (e.g., fingers, eyes).
Large motor units: Powerful movements (e.g., thighs, hips).
Muscle Twitch
A muscle twitch is the response of a motor unit to a single action potential. It consists of three phases:
Latent period: E-C coupling, no tension.
Contraction period: Cross-bridge cycling, tension rises.
Relaxation period: Ca2+ reentry into SR, tension falls.
Graded Muscle Responses
Summation and Recruitment
Temporal (wave) summation: Increased frequency of stimulation increases force of contraction.
Recruitment (multiple motor unit summation): Increased stimulus strength recruits more motor units, increasing force.
Types of Muscle Contractions
Isotonic vs. Isometric Contractions
Isotonic contractions: Muscle changes length (concentric = shortens, eccentric = lengthens).
Isometric contractions: Muscle does not change length; tension increases but does not exceed load.
Muscle Metabolism
ATP Generation Pathways
Direct phosphorylation: Creatine phosphate donates phosphate to ADP to form ATP.
Anaerobic pathway: Glycolysis produces ATP and lactate without oxygen.
Aerobic respiration: Uses oxygen to produce ATP from glucose, pyruvate, fatty acids, and amino acids.
Muscle fibers are classified as oxidative (aerobic) or glycolytic (anaerobic) based on their primary ATP-generating pathway.
Muscle Fatigue
Muscle fatigue is the physiological inability to contract, often due to ionic imbalances, increased inorganic phosphate, decreased ATP, and altered Ca2+ regulation. It prevents complete depletion of ATP and protects muscle integrity.
Factors Affecting Force, Velocity, and Duration of Contraction
Number of cross-bridges formed (affected by muscle fiber size, frequency of stimulation, degree of muscle stretch, and number of motor units recruited).
Load: Heavier loads decrease velocity and duration of contraction.
Muscle fiber type: Fast/slow, oxidative/glycolytic fibers influence contraction speed and endurance.
Summary Table: Comparison of Muscle Types
Characteristic | Skeletal | Cardiac | Smooth |
|---|---|---|---|
Location | Attached to bones or skin | Walls of the heart | Walls of hollow organs |
Cell shape & appearance | Long, cylindrical, multinucleate, striated | Branching chains, uni- or binucleate, striated, intercalated discs | Single, fusiform, uninucleate, no striations |
Control | Voluntary | Involuntary | Involuntary |

Additional info: This guide covers the structure, function, and physiology of muscle tissue, focusing on skeletal muscle, but also comparing cardiac and smooth muscle. It includes the molecular basis of contraction, neuromuscular transmission, and the metabolic pathways that fuel muscle activity.
