 Back
BackMuscles and Muscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue Overview
Types of Muscle Tissue
Muscle tissue is essential for movement and comprises nearly half of the body's mass. It transforms chemical energy (ATP) into mechanical energy, enabling force generation. There are three main types of muscle tissue, each with distinct characteristics and functions:
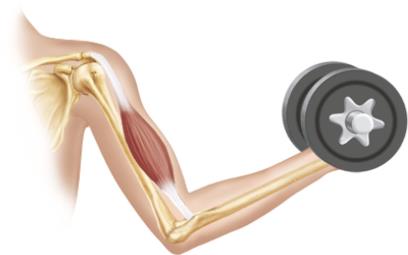
Skeletal Muscle: Attached to bones and skin, responsible for voluntary movements, striated, and contracts rapidly but tires easily.
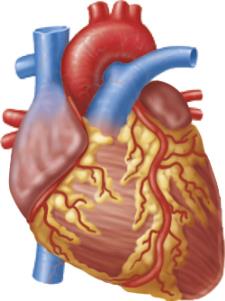
Cardiac Muscle: Found only in the heart, striated, involuntary, and contracts at a steady rate due to the heart's pacemaker.
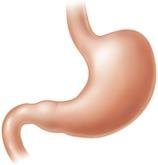
Smooth Muscle: Located in the walls of hollow organs (e.g., stomach, bladder), non-striated, involuntary, and contracts slowly.
Characteristic | Skeletal | Cardiac | Smooth |
|---|---|---|---|
Body Location | Attached to bones/skin | Heart walls | Walls of hollow organs |
Cell Shape | Long, cylindrical, multinucleate, striated | Branching, uni/binucleate, striated | Spindle-shaped, uninucleate, non-striated |
Control | Voluntary | Involuntary | Involuntary |
Characteristics of Muscle Tissue
Excitability: Ability to receive and respond to stimuli.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched.
Elasticity: Ability to recoil to resting length.
Functions of Muscle Tissue
Produce movement (locomotion, manipulation, pumping blood, digestion)
Maintain posture and body position
Stabilize joints
Generate heat during contraction
Skeletal Muscle Structure
Organization and Connective Tissue Sheaths
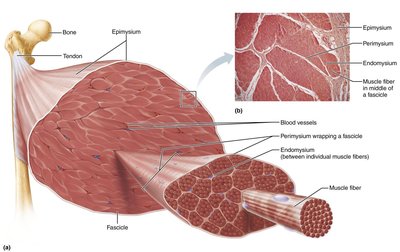
Skeletal muscle is an organ composed of muscle fibers, nerves, blood vessels, and connective tissue sheaths. These sheaths support and reinforce the muscle:
Epimysium: Surrounds the entire muscle (dense irregular connective tissue).
Perimysium: Surrounds fascicles (bundles of muscle fibers).
Endomysium: Surrounds each individual muscle fiber (areolar connective tissue).
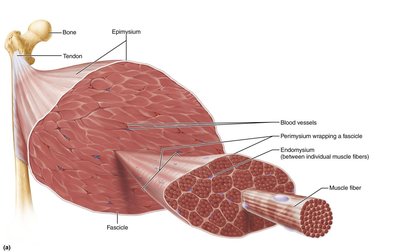
Muscle Attachments
Direct (fleshy) attachment: Epimysium fused to periosteum of bone or perichondrium of cartilage.
Indirect attachment: Connective tissue wrappings extend beyond muscle as a tendon or aponeurosis.
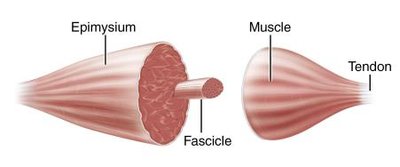
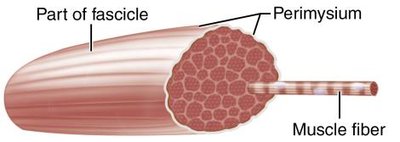
Levels of Skeletal Muscle Organization
Level | Description | Connective Tissue |
|---|---|---|
Muscle (organ) | Hundreds to thousands of muscle cells, blood vessels, nerves | Epimysium |
Fascicle | Bundle of muscle cells | Perimysium |
Muscle fiber (cell) | Elongated, multinucleate cell, striated | Endomysium |
Microscopic Anatomy of Skeletal Muscle
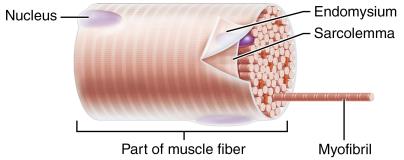
Muscle Fiber Components
Sarcolemma: Plasma membrane of muscle fiber
Sarcoplasm: Cytoplasm of muscle fiber, contains glycosomes (glycogen storage) and myoglobin (O2 storage)
Myofibrils: Densely packed, rodlike elements responsible for muscle contraction
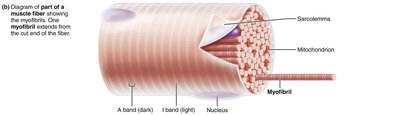

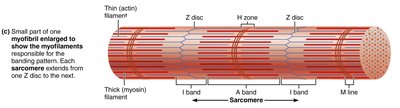
Myofibril Structure
Striations: Alternating dark (A bands) and light (I bands) regions
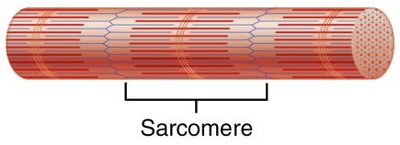
Sarcomere: Smallest contractile unit, extends from Z disc to Z disc
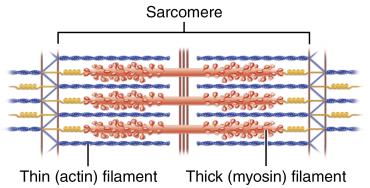
Myofilaments: Thick (myosin) and thin (actin) filaments arranged in a hexagonal pattern
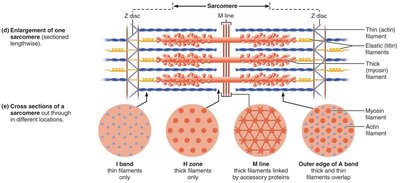
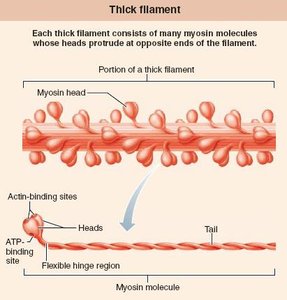
Key Proteins in Myofibrils
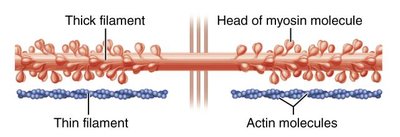
Myosin: Forms thick filaments, has heads for cross-bridge formation
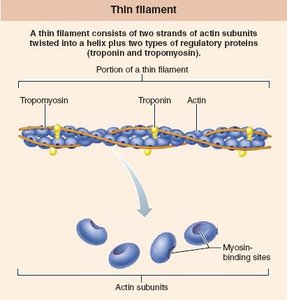
Actin: Forms thin filaments, contains binding sites for myosin
Tropomyosin and Troponin: Regulatory proteins on thin filaments
Titin: Provides elasticity and stabilizes thick filaments
Dystrophin: Links thin filaments to sarcolemma
Skeletal Muscle Physiology
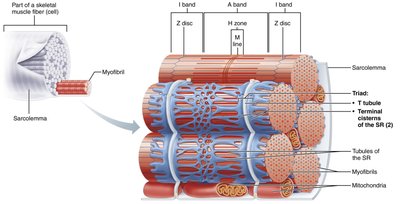
Sarcoplasmic Reticulum (SR) and T Tubules
The SR is a network of smooth endoplasmic reticulum that stores and releases Ca2+. T tubules are invaginations of the sarcolemma that transmit action potentials deep into the muscle fiber, ensuring coordinated contraction.
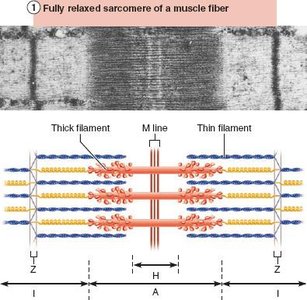
Sliding Filament Model of Contraction
During contraction, thin filaments slide past thick filaments, increasing overlap. Myosin heads bind to actin, forming cross-bridges, and pull the thin filaments toward the center of the sarcomere. This process shortens the muscle fiber without changing the length of the filaments.
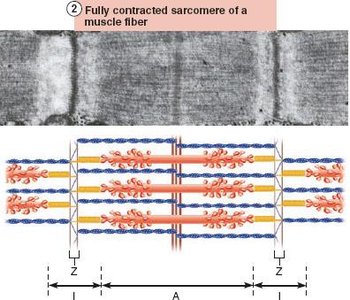
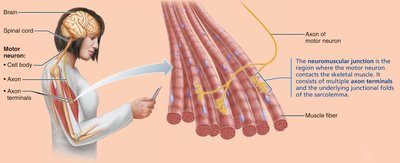
Neuromuscular Junction and Muscle Excitation
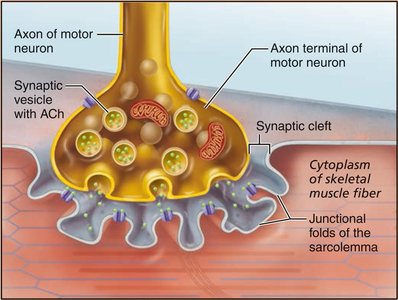
The neuromuscular junction (NMJ) is the site where a motor neuron stimulates a muscle fiber. The process involves:
Action potential arrives at axon terminal.
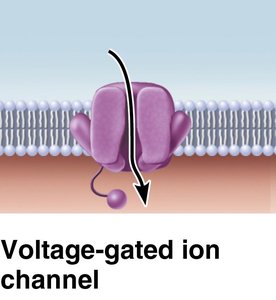
Voltage-gated Ca2+ channels open, Ca 2+ enters neuron.
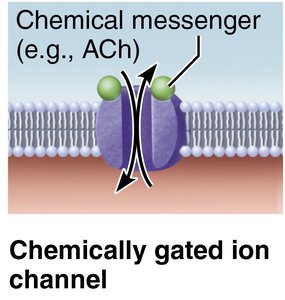
Ca 2+ triggers release of acetylcholine (ACh) into synaptic cleft.
ACh binds to receptors on sarcolemma, opening Na+ channels and generating an end plate potential.
Acetylcholinesterase degrades ACh, ending the signal.
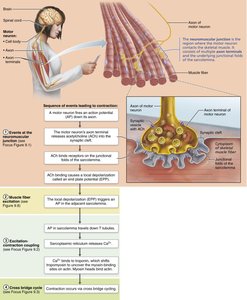
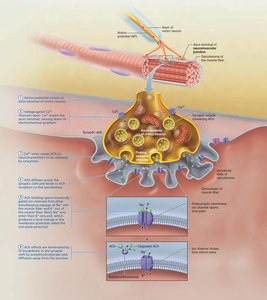
Action Potential and Excitation-Contraction Coupling
An action potential (AP) is generated and propagated along the sarcolemma and down T tubules, triggering Ca2+ release from the SR. This Ca2+ binds to troponin, moving tropomyosin and allowing myosin to bind actin, initiating contraction.
Cross Bridge Cycle
Cross bridge formation: Myosin head attaches to actin.
Power stroke: Myosin head pivots, pulling actin filament.
Cross bridge detachment: ATP binds to myosin, causing detachment.
Cocking of myosin head: ATP hydrolysis re-energizes the myosin head.
Whole Muscle Contraction
Motor Units and Muscle Twitch
Motor Unit: A motor neuron and all the muscle fibers it innervates. Smaller units allow fine control.
Muscle Twitch: Response of a muscle to a single stimulus, consisting of latent, contraction, and relaxation phases.
Graded Muscle Responses
Strength and duration of contraction can be varied by changing the frequency and strength of stimulation.
Temporal (wave) summation: Increased frequency of stimulation increases tension.
Recruitment: Increasing stimulus strength recruits more motor units.
Types of Contractions
Isotonic: Muscle changes length (concentric: shortens; eccentric: lengthens).
Isometric: Muscle tension increases, but length does not change.
Energy for Muscle Contraction
ATP Regeneration Pathways
Direct phosphorylation: Creatine phosphate donates phosphate to ADP to form ATP (short duration, ~15 seconds).
Anaerobic pathway: Glycolysis and lactic acid formation (no oxygen required, short-term energy).
Aerobic pathway: Aerobic respiration in mitochondria (requires oxygen, long-term energy).
Equation for direct phosphorylation:
Muscle Fatigue and Recovery
Muscle fatigue: Inability to contract despite continued stimulation, often due to ionic imbalances, increased inorganic phosphate, or decreased ATP/glycogen.
Excess postexercise oxygen consumption (EPOC): Oxygen required to restore muscle to pre-exercise state.
Factors Affecting Muscle Contraction
Frequency of stimulation
Number of muscle fibers recruited
Size of muscle fibers
Degree of muscle stretch (length-tension relationship)
Muscle Fiber Types
Type | Speed | ATP Pathway | Myoglobin | Fatigue | Best Suited For |
|---|---|---|---|---|---|
Slow Oxidative | Slow | Aerobic | High | Resistant | Endurance, posture |
Fast Oxidative | Fast | Aerobic/Some Anaerobic | High | Intermediate | Sprinting, walking |
Fast Glycolytic | Fast | Anaerobic | Low | Fatigable | Short, intense movements |
Smooth Muscle
Structure and Function
Found in walls of hollow organs (except heart)
Spindle-shaped, uninucleate, non-striated
Arranged in longitudinal and circular layers
Contracts via sliding filament mechanism, but regulated by calmodulin (not troponin)
Types of Smooth Muscle
Unitary (visceral): Most common, found in hollow organs, electrically coupled by gap junctions
Multi unit: Found in large airways, arteries, arrector pili, and iris; few gap junctions, independent fibers
Development and Aging of Muscle
All muscle tissues develop from myoblasts (embryonic mesoderm cells)
Cardiac and smooth muscle can regenerate to some extent; skeletal muscle has limited regeneration
With age, muscle mass decreases (sarcopenia), but regular exercise can slow this process
