 Back
BackNervous and Muscular Systems: Structure, Function, and Physiology
Study Guide - Smart Notes

Nervous Tissue and the Nervous System
Classification of the Nervous System
The nervous system is a complex network responsible for coordinating body activities. It is divided into two major parts:
Central Nervous System (CNS): Consists of the brain and spinal cord; acts as the main control center for processing information.
Peripheral Nervous System (PNS): Composed of all neural tissue outside the CNS, including nerves and ganglia; connects the CNS to limbs and organs.
Organs of the CNS and PNS
CNS: Brain and spinal cord.
PNS: Cranial nerves (12 pairs), spinal nerves (31 pairs), ganglia, and sensory receptors.
Types of Nerves
Cranial Nerves: 12 pairs, emerge from the brain.
Spinal Nerves: 31 pairs, emerge from the spinal cord.
Characteristics of Neurons
Excitable cells that transmit electrical signals.
Long-lived, amitotic (do not divide), and have a high metabolic rate.
Specialized for communication via action potentials and neurotransmitters.
Major Parts of a Neuron and Their Functions
Cell Body (Soma): Contains the nucleus and organelles; metabolic center.
Dendrites: Receive incoming signals from other neurons.
Axon: Conducts electrical impulses away from the cell body.
Major Parts of an Axon
Axon Hillock: Initiates action potentials.
Axon Terminals: Release neurotransmitters to communicate with other cells.
Myelin Sheath: Insulating layer that increases the speed of impulse conduction.
Nodes of Ranvier: Gaps in the myelin sheath where action potentials are regenerated.
Function of Myelin Sheath
Insulates axons, allowing for faster transmission of electrical impulses (saltatory conduction).
Produced by oligodendrocytes in the CNS and Schwann cells in the PNS.
Myelinated vs. Unmyelinated Axons
Myelinated Axons: Conduct impulses rapidly due to saltatory conduction.
Unmyelinated Axons: Conduct impulses more slowly via continuous conduction.
Gray Matter vs. White Matter in the Brain
Gray Matter: Contains neuron cell bodies, dendrites, and unmyelinated axons; located on the outer surface (cortex) of the brain and inner part of the spinal cord.
White Matter: Composed mainly of myelinated axons; found deeper in the brain and outer part of the spinal cord.
Axon Diameter and Speed of Impulse Propagation
Larger diameter axons conduct impulses faster due to lower resistance to current flow.
Speed is also increased by myelination.
Repair in CNS vs. PNS
CNS: Limited ability to repair due to inhibitory factors and lack of growth-promoting environment.
PNS: Schwann cells promote axon regeneration, allowing some repair after injury.
The Central Nervous System (CNS)
Functions of the CNS
Integrates sensory information and coordinates voluntary and involuntary responses.
Responsible for higher functions such as thought, memory, and emotion.
Major Parts of the Brain
Cerebrum: Largest part; responsible for higher brain functions.
Diencephalon: Includes thalamus and hypothalamus; relays sensory information and controls autonomic functions.
Brain Stem: Includes midbrain, pons, and medulla oblongata; controls basic life functions.
Cerebellum: Coordinates movement and balance.
Protection of the CNS
Bony Protection: Skull protects the brain; vertebral column protects the spinal cord.
Meninges: Three connective tissue layers (dura mater, arachnoid mater, pia mater) surround the CNS.
Cerebrospinal Fluid (CSF): Cushions and nourishes the CNS.
Blood-Brain Barrier: Regulates passage of substances from blood into the brain.
Space Containing CSF
Subarachnoid Space: Located between the arachnoid mater and pia mater; filled with CSF.
Importance of Sufficient Blood Flow in the Brain
Ensures delivery of oxygen and nutrients; lack of blood flow can cause brain damage within minutes.
Blood-Brain Barrier
A selective barrier formed by endothelial cells of brain capillaries; protects the brain from harmful substances.
Cerebrospinal Fluid (CSF)
Definition: Clear, colorless fluid produced by the choroid plexus.
Functions: Cushions the brain, removes waste, and provides nutrients.
Characteristics: Low protein, few cells, similar to plasma but with different ion concentrations.
Brain Surface Features
Gyrus (Gyri): Elevated ridges on the brain surface.
Sulcus (Sulci): Shallow grooves between gyri.
Fissure: Deep grooves that separate large brain regions.
Lobes of the Cerebrum
Frontal, Parietal, Temporal, Occipital, and Insula (deep within the lateral sulcus).
Sensory, Motor, and Association Areas in the Cerebrum
Sensory Areas: Receive and interpret sensory information.
Motor Areas: Control voluntary muscle movements.
Association Areas: Integrate information for complex functions (e.g., reasoning, language).
Association Areas and Their Functions
Prefrontal Cortex: Planning, decision-making, personality.
Wernicke's Area: Language comprehension.
Broca's Area: Speech production.
Major Parts of the Diencephalon and Their Functions
Thalamus: Relay station for sensory information.
Hypothalamus: Regulates homeostasis, endocrine functions, and autonomic nervous system.
Epithalamus: Contains pineal gland; involved in sleep-wake cycles.
Parts of the Brain Stem and Their Functions
Midbrain: Visual and auditory reflexes.
Pons: Relays information between cerebrum and cerebellum; regulates breathing.
Medulla Oblongata: Controls vital functions (heart rate, breathing, blood pressure).
Functions and Major Parts of the Cerebellum
Functions: Coordinates voluntary movements, balance, and posture.
Major Parts: Two hemispheres, vermis (central region), and cerebellar cortex.
Functions of the Spinal Cord
Conducts sensory and motor information between the body and brain.
Integrates reflexes.
Sensory vs. Motor Tracts in the Spinal Cord
Sensory (Ascending) Tracts: Carry sensory information to the brain.
Motor (Descending) Tracts: Carry motor commands from the brain to the body.
The Peripheral Nervous System (PNS)
Spinal Nerve Plexuses
Cervical Plexus: Supplies neck and diaphragm.
Brachial Plexus: Supplies upper limbs.
Lumbar Plexus: Supplies lower abdomen and thigh.
Sacral Plexus: Supplies pelvis and lower limbs.
Reflexes
Definition: Rapid, automatic response to a stimulus.
Example: Knee-jerk (patellar) reflex.
Cranial Nerves: Numbers, Names, Types, and Functions
Number | Name | Type | Function |
|---|---|---|---|
I | Olfactory | Sensory | Smell |
II | Optic | Sensory | Vision |
III | Oculomotor | Motor | Eye movement, pupil constriction |
IV | Trochlear | Motor | Eye movement |
V | Trigeminal | Both | Facial sensation, chewing |
VI | Abducens | Motor | Eye movement |
VII | Facial | Both | Facial expression, taste |
VIII | Vestibulocochlear | Sensory | Hearing, balance |
IX | Glossopharyngeal | Both | Taste, swallowing |
X | Vagus | Both | Visceral sensation, parasympathetic control |
XI | Accessory | Motor | Head and shoulder movement |
XII | Hypoglossal | Motor | Tongue movement |
Sensation vs. Perception
Sensation: Detection of stimuli by sensory receptors.
Perception: Interpretation of sensory information by the brain.
Touch and Pressure Receptors
Meissner's Corpuscles: Detect light touch.
Pacinian Corpuscles: Detect deep pressure and vibration.
Merkel Discs: Detect steady pressure.
Referred Pain
Definition: Pain perceived at a location other than the site of the painful stimulus, due to shared neural pathways.
Example: Pain from a heart attack felt in the left arm.
Proprioception and Proprioceptors
Proprioception: Sense of body position and movement.
Proprioceptors: Sensory receptors located in muscles, tendons, and joints.
Autonomic Nervous System (ANS)
Overview of the ANS
The Autonomic Nervous System (ANS) is a division of the peripheral nervous system that regulates involuntary physiological processes, including heart rate, blood pressure, respiration, digestion, and sexual arousal. It operates largely below the level of consciousness and is essential for maintaining homeostasis.
Somatic Nervous System vs. ANS: The somatic nervous system controls voluntary movements via skeletal muscles, while the ANS controls involuntary functions of smooth muscle, cardiac muscle, and glands.
Dual Innervation: Most organs receive input from both sympathetic and parasympathetic divisions, allowing precise regulation.
Preganglionic and Postganglionic Neurons
Preganglionic Neuron: The first neuron in the autonomic pathway; its cell body is in the CNS and its axon synapses with the postganglionic neuron in an autonomic ganglion.
Postganglionic Neuron: The second neuron; its cell body is in the ganglion and its axon extends to the effector organ.
Sympathetic and Parasympathetic Divisions
Feature | Sympathetic | Parasympathetic |
|---|---|---|
Origin | Thoracolumbar (T1-L2) | Craniosacral (Brainstem, S2-S4) |
Ganglia Location | Near spinal cord (paravertebral) | Near or within target organs |
Neurotransmitters | Acetylcholine (preganglionic), Norepinephrine (postganglionic) | Acetylcholine (both) |
General Function | Fight or flight | Rest and digest |
Role of the Adrenal Medulla
The adrenal medulla acts as a modified sympathetic ganglion. Preganglionic sympathetic fibers stimulate it to release epinephrine and norepinephrine into the bloodstream, amplifying sympathetic effects.
Autonomic Ganglia
Sympathetic Ganglia: Paravertebral (sympathetic chain) and prevertebral (collateral) ganglia.
Parasympathetic Ganglia: Terminal ganglia located near or within target organs.
Cholinergic and Adrenergic Receptors
Cholinergic Receptors: Bind acetylcholine. Two types:
Nicotinic: Found on all postganglionic neurons and adrenal medulla cells; always excitatory.
Muscarinic: Found on all parasympathetic target organs; can be excitatory or inhibitory.
Adrenergic Receptors: Bind norepinephrine and epinephrine. Two main types:
Alpha (α) receptors
Beta (β) receptors
Autonomic Plexuses and Reflexes
Autonomic Plexuses: Networks of sympathetic and parasympathetic fibers that innervate organs (e.g., cardiac, pulmonary, celiac plexuses).
Autonomic Reflexes: Involuntary responses mediated by the ANS (e.g., baroreceptor reflex for blood pressure regulation).
Neurotransmitters: Acetylcholine and Norepinephrine
Acetylcholine (ACh): Released by all preganglionic neurons and parasympathetic postganglionic neurons.
Norepinephrine (NE): Released by most sympathetic postganglionic neurons.
Autonomic Tone
Refers to the baseline level of activity in the sympathetic and parasympathetic divisions, allowing for rapid adjustments in organ function.
Sympathetic and Parasympathetic Responses
Sympathetic: Increases heart rate, dilates pupils, inhibits digestion, stimulates glucose release.
Parasympathetic: Decreases heart rate, constricts pupils, stimulates digestion, promotes energy storage.
Special Senses
Olfaction (Sense of Smell)
Anatomy of Receptors: Olfactory receptors are located in the olfactory epithelium of the nasal cavity.
Odor Threshold: The minimum concentration of a substance required to be detected as an odor.
Adaptation: Decreased sensitivity to odors with prolonged exposure.
Olfactory Pathway: Olfactory nerves → olfactory bulb → olfactory tract → olfactory cortex (temporal lobe).
Gustation (Sense of Taste)
Anatomy of Taste Buds: Taste buds are located on papillae of the tongue, soft palate, and pharynx.
Basic Taste Sensations: Sweet, sour, salty, bitter, umami.
Gustatory Pathway: Taste receptor cells → cranial nerves VII, IX, X → medulla oblongata → thalamus → gustatory cortex.
Vision
Accessory Structures: Eyelids, eyelashes, lacrimal apparatus, extrinsic eye muscles.
Three Layers of the Eyeball:
Fibrous Tunic: Sclera and cornea.
Vascular Tunic: Choroid, ciliary body, iris.
Nervous Tunic: Retina.
Convex and Concave Lenses: Convex lenses converge light (used to correct hyperopia), concave lenses diverge light (used to correct myopia).
Myopia (Nearsightedness): Image focuses in front of retina; corrected with concave lenses.
Hyperopia (Farsightedness): Image focuses behind retina; corrected with convex lenses.
Astigmatism: Irregular curvature of cornea or lens causing blurred vision.
Structure of Retina: Contains photoreceptors (rods and cones), bipolar cells, ganglion cells.
Rods and Cones: Rods detect dim light; cones detect color and detail.
Dark and Light Adaptation: Adjustment of eyes to changes in light intensity.
Visual Pathway: Retina → optic nerve → optic chiasm → optic tract → thalamus → visual cortex.
Cataracts: Clouding of the lens, leading to decreased vision.
Glaucoma: Increased intraocular pressure damaging the optic nerve.
Hearing and Equilibrium
Anatomy of the Ear:
External Ear: Auricle, external auditory canal, tympanic membrane.
Middle Ear: Auditory ossicles (malleus, incus, stapes), auditory tube.
Inner Ear: Cochlea (hearing), vestibule and semicircular canals (equilibrium).
Auditory Pathway: Cochlear hair cells → cochlear nerve → brainstem → thalamus → auditory cortex.
Physiology of Equilibrium:
Static Equilibrium: Sensed by the vestibule; detects head position relative to gravity.
Dynamic Equilibrium: Sensed by semicircular canals; detects rotational movements.
Meniere’s Disease: Disorder of the inner ear causing vertigo, tinnitus, and hearing loss.
Example: When you stand up quickly, your autonomic reflexes adjust blood pressure to prevent dizziness (baroreceptor reflex). When you enter a dark room, your eyes undergo dark adaptation, increasing sensitivity to light.
Muscle Tissue Types
Overview of Muscle Tissue
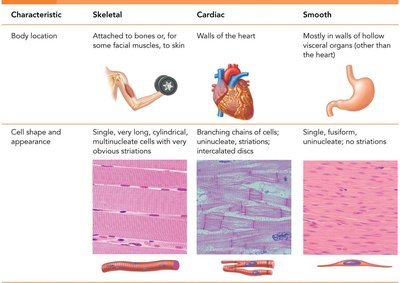
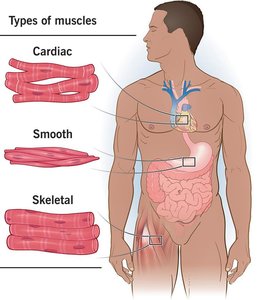
Muscle tissue is specialized for contraction and is essential for movement, posture, and various bodily functions. There are three main types of muscle tissue: skeletal, cardiac, and smooth muscle, each with distinct structures and functions.
Skeletal Muscle: Attached to bones and skin, responsible for voluntary movements, striated, and multinucleated.
Cardiac Muscle: Found only in the heart, responsible for pumping blood, striated, involuntary, and contains intercalated discs.
Smooth Muscle: Located in walls of hollow organs (except the heart), non-striated, involuntary, and spindle-shaped cells.
Functions and Characteristics of Muscle Tissue
Excitability (Responsiveness): Ability to receive and respond to stimuli.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched.
Elasticity: Ability to recoil to resting length after stretching.
Movement of bones or fluids (e.g., blood)
Maintaining posture and body position
Stabilizing joints
Heat generation (especially skeletal muscle)
Additional: Protects organs, forms valves, controls pupil size, causes "goosebumps"

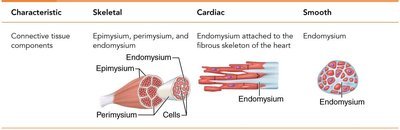
Connective Tissue Wrappings of Skeletal Muscle
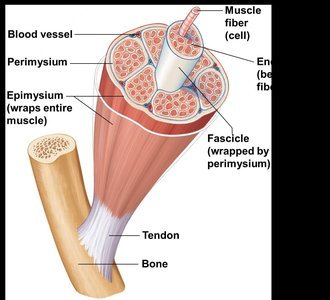
Skeletal muscles are organized into bundles and surrounded by connective tissue layers that provide support and transmit force.
Endomysium: Areolar connective tissue surrounding each muscle fiber (cell).
Perimysium: Fibrous connective tissue wrapping around a fascicle (bundle of muscle fibers).
Epimysium: Dense irregular connective tissue covering the entire muscle.
Tendons: Cordlike structures connecting muscle to bone, mostly collagen fibers.
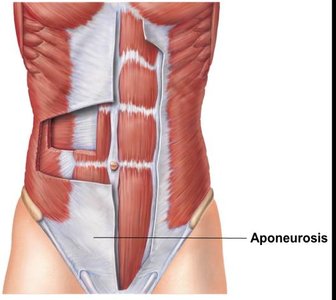
Aponeuroses: Sheetlike structures attaching muscles indirectly to bones or other muscles.
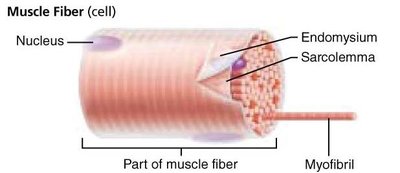
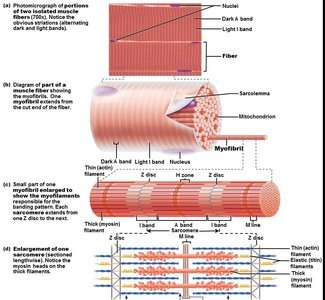
Skeletal Muscle Structure and Microscopic Anatomy
Each skeletal muscle fiber is a long, cylindrical cell containing multiple nuclei and specialized organelles for contraction.
Sarcolemma: Specialized plasma membrane of muscle fiber.
Myofibrils: Long organelles inside muscle cell, responsible for striations.
Sarcomere: The contractile unit, extending from one Z disc to another.
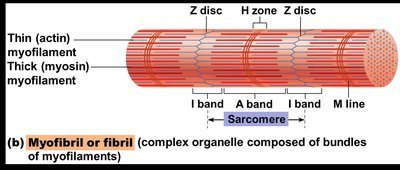

Myofilaments
Thin Filaments: Composed of actin proteins, anchored to Z discs.
Thick Filaments: Composed of myosin proteins, contain ATPase enzymes and myosin heads (cross bridges).
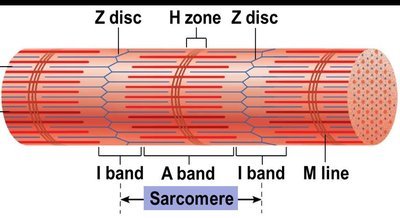
The arrangement of thin and thick filaments creates the characteristic banding pattern of skeletal muscle.
Sarcoplasmic Reticulum (SR)
Specialized smooth endoplasmic reticulum that stores and releases calcium ions, essential for muscle contraction.
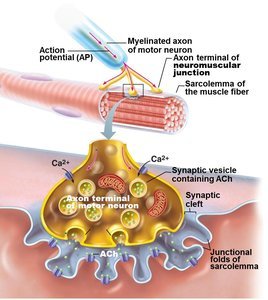
The Nerve Stimulus and Action Potential
Muscle contraction is initiated by stimulation from a motor neuron at the neuromuscular junction.
Motor Unit: One motor neuron and all the muscle fibers it stimulates.
Neuromuscular Junction: Site where the axon terminal of a motor neuron communicates with the sarcolemma of a muscle fiber.
Neurotransmitter: Acetylcholine (ACh) is released to stimulate muscle contraction.
Synaptic Cleft: Gap between nerve and muscle, filled with interstitial fluid.

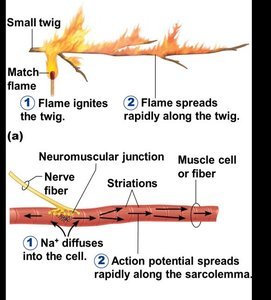
Transmission of Nerve Impulse
The action potential generated at the neuromuscular junction spreads along the sarcolemma, triggering muscle contraction.

Muscle Contraction: Sliding Filament Model and Cross Bridge Cycling
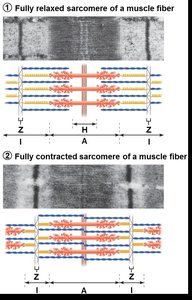
Sliding Filament Model
Muscle contraction occurs when myosin heads bind to actin, forming cross bridges and pulling thin filaments toward the center of the sarcomere. This process shortens the muscle fiber.
In the relaxed state, thin and thick filaments overlap only at the ends of the A band.
During contraction, the H zone and I bands shorten, Z discs move closer, and the muscle shortens.
Cross Bridge Cycling
ATP is required for cross bridge detachment and re-cocking of the myosin head.
Absence of ATP (as in rigor mortis) prevents detachment, causing muscle stiffness after death.
Graded Response and Muscle Tension
Muscle fiber contraction is "all or none"—a fiber contracts fully or not at all.
Graded responses occur when different numbers of fibers contract, producing varying degrees of muscle tension.
Tetanus is a sustained, smooth contraction resulting from rapid stimulation.
Types of Muscle Contractions
Isometric Contractions: Muscle tension increases, but the muscle does not shorten or produce movement (e.g., pushing against a wall).
Isotonic Contractions: Muscle shortens and movement occurs (e.g., bending the knee).
Muscle Tone: Continuous, partial contraction of muscles keeps them healthy and ready to respond.
Energy for Muscle Contraction
Direct Phosphorylation: Creatine phosphate donates a phosphate to ADP to form ATP.
Aerobic Respiration: Uses oxygen to generate ATP from glucose; efficient but slower.
Anaerobic Glycolysis: Generates ATP quickly without oxygen, producing lactic acid as a byproduct.
ATP is the immediate source of energy for muscle contraction, but muscle fibers store only small amounts, requiring continuous regeneration during activity.
Muscle Fatigue and Oxygen Deficit
Fatigue occurs due to ionic imbalances, lactic acid accumulation, and decreased ATP supply.
After exercise, oxygen deficit is repaid by rapid, deep breathing to restore normal metabolic conditions.
Smooth Muscle Structure and Function
Location and Organization
Smooth muscle is found in the walls of most hollow organs (except the heart) and is organized in two layers: longitudinal and circular. This arrangement allows for peristalsis, the coordinated contraction and relaxation that moves substances through organs.
Microscopic Structure
Spindle-shaped, uninucleate cells without striations.
SR is less developed; most Ca2+ influx is from outside the cell.
No sarcomeres, myofibrils, or T tubules.
Innervation and Myofilaments
Innervated by autonomic nerve fibers at diffuse junctions.
Varicosities release neurotransmitters into the extracellular space.
Thick to thin filament ratio is lower than in skeletal muscle; calmodulin binds Ca2+ instead of troponin.
Dense bodies anchor filaments, analogous to Z discs in skeletal muscle.
Contraction and Regulation of Smooth Muscle
Slow, synchronized contractions; cells are electrically coupled by gap junctions.
Some cells are self-excitatory and act as pacemakers.
Contraction is triggered by increased intracellular Ca2+, primarily from the extracellular space.
ATP is required for contraction; relaxation requires Ca2+ detachment from calmodulin and active transport out of the cell.
Regulation and Special Features
Regulated by nerves, hormones, and local chemical changes.
Stress-relaxation response allows adaptation to stretching (e.g., in the bladder).
Smooth muscle can undergo hyperplasia (increase in cell number), unlike skeletal muscle.
Developmental Aspects and Disorders of Muscle Tissue
All muscle tissue develops from myoblasts.
Cardiac and skeletal muscle become amitotic after birth; smooth muscle retains regenerative ability.
With aging, muscle fibers are lost and replaced by connective tissue, leading to decreased strength and mass.
Muscular System Disorders
Fibromyalgia: Chronic inflammation of muscles and connective tissues, cause unknown.
Hernia: Protrusion of an organ through a muscle wall, often due to muscle weakness or strain.
Duchenne Muscular Dystrophy: Inherited disease causing muscle degeneration due to lack of dystrophin.
Myasthenia Gravis: Autoimmune disease where acetylcholine receptors are attacked, leading to muscle weakness and possible respiratory failure.
Additional info: Some explanations and examples have been expanded for clarity and completeness.
