 Back
BackPatient Assessment and Consultation in Self-Care and Nonprescription Medications
Study Guide - Smart Notes

Introduction to Patient Assessment and Consultation
Overview
Patient assessment and consultation are critical components of pharmacy practice, especially in the context of self-care and nonprescription medications. Pharmacists must utilize effective communication skills, understand social determinants of health, and systematically assess patient needs to ensure safe and effective therapy.
Communication Skills in Patient Encounters
Essential Communication Skills
Questioning Skills: Use open-ended questions to gather information and closed-ended questions for clarification. Avoid leading questions to prevent bias.
Listening Skills: Practice active listening and pay attention to nonverbal cues.
Empathetic Responding: Listen, identify, and understand patient concerns to build trust and rapport.
Self-Care Communication Tips
Know your surroundings and remove physical barriers.
Smile, maintain eye contact, and speak clearly.
Remain calm, be patient, and explain the process to the patient.
Have resources readily available for reference.
Communication Barriers and Accommodations
Visual Impairment: Provide information in large print or audio format.
Hearing Impairment: Use written communication or sign language interpreters.
Language Barriers: Utilize translation services or bilingual staff.
Cultural Differences: Show cultural sensitivity and adapt communication style.
Health Illiteracy: Use simple language and visual aids.
Social Determinants of Health (SDOH)
Impact on Self-Care
Social determinants of health are conditions in the environments where people are born, live, learn, work, play, and age that affect health outcomes and risks. These factors can significantly impact a patient's ability to engage in self-care.
Economic Stability: Affects ability to afford medications and healthcare services.
Education Access and Quality: Influences health literacy and understanding of medical instructions.
Health Care Access and Quality: Determines availability of medical advice and products.
Neighborhood and Built Environment: Impacts access to pharmacies and safe environments for health management.
Social and Community Context: Shapes support systems and cultural attitudes toward self-care.

Approaches to Culturally Diverse Patient Care
LEARN Model
Listen: Hear the patient’s perspective.
Explain: Share your own perspective.
Acknowledge: Recognize differences and similarities.
Recommend: Suggest treatment options.
Negotiate: Agree on a treatment plan.
Patient Explanatory Model (PEM) – 4 C’s
What do you call the problem?
What do you think caused the problem?
How do you cope with the problem?
What concerns do you have?
Purpose and Process of Patient Assessment
Goals of Assessment
Determine a patient’s drug-related needs.
Prioritize goals of therapy.
Identify drug-related problems.
Drug-Related Needs of Patients
Each medication must have an appropriate indication.
Drug therapy must be effective and safe.
Untreated indications should be addressed.
The treatment plan must be one with which the patient can comply.
Systematic Patient Consultation Process
Steps in Patient Consultation
Gather information
Identify the problem
Determine exclusions for self-treatment
Identify possible solutions
Select the optimal solution
Prepare and implement a plan
Educate the patient
Patient-Specific and Medication-Specific Variables
Patient-Specific: Age, gender, medication history, medical conditions, allergies, social history, economic status, patient preference.
Medication-Specific: Dosage forms, active/inactive ingredients, adverse effects, potential interactions, efficacy, flavor, price.
Assessment Methods: QuEST, SCHOLAR-MAC, and PQRSTA
QuEST Process
Quickly and accurately assess the patient
Establish that the patient is an appropriate self-care candidate
Suggest appropriate self-care strategies
Talk with the patient
SCHOLAR-MAC
Symptoms
Characteristics
History
Onset
Location
Aggravating factors
Remitting factors
Medications
Allergies
Conditions
PQRSTA
Precipitating
Quality
Relief
Site and Severity
Temporal factors
Associated symptoms
Pharmacists’ Patient Care Process
Model Overview
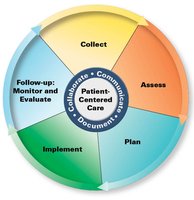
The Pharmacists’ Patient Care Process is a systematic approach to patient-centered care, integrating assessment, planning, implementation, and follow-up.
Collect
Assess
Plan
Implement
Follow-up: Monitor and Evaluate
Patient Triage and Referral
Triage Options
Send to emergency department or call 911
Refer to physician or other medical care
Continue prescription therapy
Recommend nonprescription therapy
Do not provide pharmacologic treatment
When to Refer
Symptoms are too severe or require a definitive diagnosis
Symptoms are minor but persistent with no clear cause
Symptoms repeatedly return with no clear cause
Pharmacist is in doubt about the patient’s condition
Product Recommendations and Counseling
Key Counseling Points
Active ingredient(s), purpose, uses, warnings, directions, and other information
Monitoring parameters, duration of therapy, onset of action
Nonpharmacologic therapy and follow-up process
When to seek additional medical care and what to expect
Resources for Nonprescription Product Information
DailyMed
Manufacturer websites
Retail websites (use cautiously)
The actual product packaging
Documentation in Patient Care
Importance and Methods
Documentation provides evidence, supports follow-up, and is necessary for reimbursement.
Methods include electronic databases and paper forms or charts.
Medication Therapy Management (MTM) and Nonprescription Products
Comprehensive Medication Review (CMR)
Should include prescription medications, immunizations, nonprescription medications, herbal products, and dietary supplements.
Case Studies: Application of Patient Assessment
Case 1: Young Woman with Cold Symptoms
Assessment using PQRSTA: Stuffy nose, sore throat, congestion, started yesterday, no other medical problems, takes birth control and multivitamin.
Recommendation: Decongestant (pseudoephedrine), NSAID or acetaminophen for sore throat, assess alcohol use, avoid unnecessary combination products.
Case 2: Man with Knee Pain and Stomach Irritation
Assessment using PQRSTA: Knee pain (achy, stiff), stomach irritation (burning after eating), uses ibuprofen and Zantac, has high cholesterol, takes Lipitor and multivitamin.
Recommendation: Assess alcohol use, consider switching from ibuprofen to acetaminophen, refer to physician for stomach irritation, discuss diet and smoking status.
Appendix: Nonprescription Medication Consultation Form
The Nonprescription Medication Consultation Form is a structured tool for collecting patient information, assessing symptoms, and documenting outcomes and follow-up.

Example Sections:
Patient information and condition being treated
Chronic medical conditions and current medications
Symptom analysis (PQRSTA)
Outcome and follow-up documentation
