 Back
BackPharynx, Esophagus, and Stomach: Structure and Function in Digestion
Study Guide - Smart Notes

Pharynx and Esophagus
Pharynx: Structure and Function
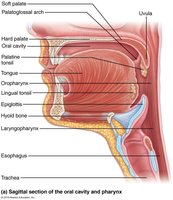
The pharynx is a muscular tube that serves as a passageway for food from the mouth to the esophagus. It is lined with stratified squamous epithelium and contains mucus-producing glands to facilitate the movement of food and protect tissues.
Food Pathway: Food passes from the mouth into the oropharynx, then the laryngopharynx.
Muscle Layers: The pharynx has two external muscle layers that contract to force food into the esophagus.
Epithelium: Stratified squamous epithelium protects against abrasion.
Mucus: Mucus lubricates and protects the lining.
Esophagus: Structure and Function
The esophagus is a flat, muscular tube extending from the laryngopharynx to the stomach. It is normally collapsed except when propelling food. The esophagus passes through the diaphragm at the esophageal hiatus and joins the stomach at the cardial orifice.
Gastroesophageal Sphincter: This sphincter keeps the orifice closed when food is not being swallowed, preventing acid reflux.
Mucus Cells: Mucus cells on both sides of the sphincter protect the esophagus from stomach acid.
Acid Reflux: Occurs when the sphincter is weak or relaxed, allowing stomach acid to enter the esophagus.
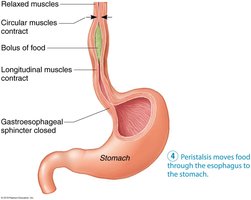
Digestive Function: Propulsion and Swallowing
The primary function of the pharynx and esophagus is propulsion—moving food from the mouth to the stomach. This process begins with swallowing, which involves coordinated activity of 22 muscle groups and occurs in two phases:
Buccal Phase: Voluntary contraction of the tongue to push food into the pharynx.
Pharyngeal-Esophageal Phase: Involuntary phase controlled by the vagus nerve and the swallowing center in the medulla and lower pons.
Stomach
Anatomy of the Stomach
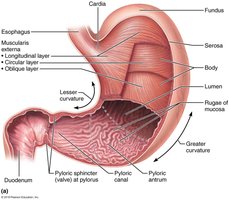
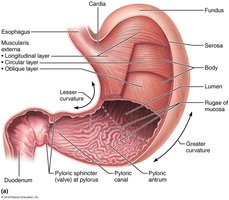
The stomach is a temporary storage site for food and initiates the chemical breakdown of proteins. It converts the bolus of food into chyme and can expand from a volume of about 50 mL when empty to up to 4 liters when full. The stomach mucosa forms folds called rugae when empty.
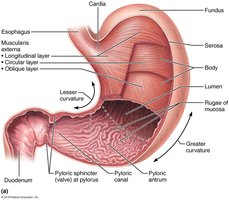
Major Regions:
Cardia: Surrounds the cardial orifice.
Fundus: Dome-shaped region below the diaphragm.
Body: Mid-portion of the stomach.
Pyloric Part: Narrows into the pyloric canal and connects to the duodenum via the pyloric sphincter.
Curvatures:
Greater Curvature: Convex lateral surface.
Lesser Curvature: Concave medial surface.
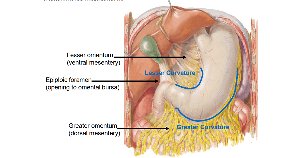
Mesenteries: Greater and lesser omentum extend from the curvatures to other digestive organs and the abdominal wall.
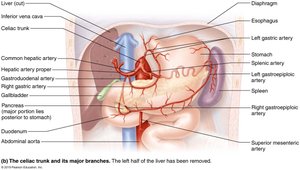
Stomach Blood Supply and Innervation
The stomach receives autonomic nervous system (ANS) input from both sympathetic and parasympathetic fibers. Its blood supply comes from the celiac trunk (gastric and splenic branches) and veins of the hepatic portal system.
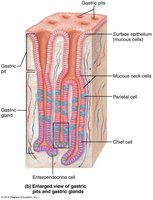
Microscopic Anatomy of the Stomach
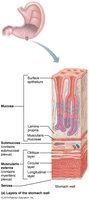
The stomach wall contains all four basic layers, with a unique muscularis externa that includes a third, oblique layer. This arrangement allows the stomach to churn, mix, and move chyme, increasing the physical breakdown of food.
Muscularis Externa: Circular, longitudinal, and oblique layers of smooth muscle.
Mucosa: Simple columnar epithelium composed of mucous cells that secrete alkaline mucus.
Gastric Pits: Lead into gastric glands that produce gastric juice.
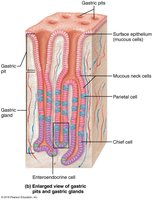
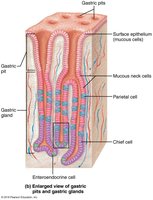
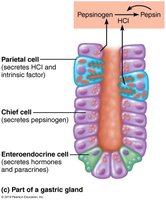
Gastric Gland Cells and Their Functions
Gastric glands contain several types of secretory cells, each with specialized functions:
Mucous Neck Cells: Secrete thin, acidic mucus (function not fully understood).
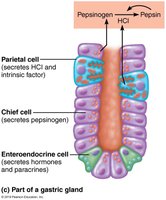
Parietal Cells: Secrete hydrochloric acid (HCl, pH 1.5–3.5) to denature proteins, activate pepsin, and kill bacteria. Also secrete intrinsic factor, a glycoprotein required for vitamin B12 absorption in the small intestine.
Chief Cells: Secrete pepsinogen (inactive enzyme), which is activated to pepsin by HCl and pepsin itself (positive feedback). Also secrete lipases, contributing to lipid digestion.
Enteroendocrine Cells: Secrete chemical messengers (paracrines and hormones such as somatostatin and gastrin).
Stomach Protection: Mucosal Barrier
The stomach is protected from its acidic environment by a mucosal barrier formed by three factors:
Thick Layer of Bicarbonate-Rich Mucus: Neutralizes acid near the stomach lining.
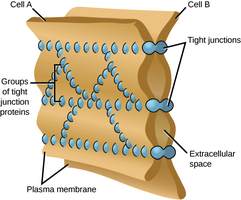
Tight Junctions Between Epithelial Cells: Prevent gastric juice from seeping between cells.
Rapid Cell Turnover: Damaged epithelial cells are quickly replaced by stem cells; surface cells are replaced every 3–6 days.

Digestive Processes in the Stomach
Functions of the Stomach
The stomach performs several key digestive functions:
Breakdown of Food: Both mechanical and chemical digestion.
Holding of Food: Temporary storage before passage to the small intestine.
Delivery of Chyme: Gradual release of chyme to the small intestine.
Denaturation of Proteins: Via HCl.
Enzymatic Digestion: Pepsin digests proteins.
Intrinsic Factor Secretion: Essential for vitamin B12 absorption.
Regulation of Gastric Secretion
Gastric mucosa secretes more than 3 liters of gastric juice per day, regulated by neural and hormonal mechanisms:
Neural Mechanisms: Vagus nerve increases secretion; sympathetic stimulation decreases secretion.
Hormonal Mechanisms: Gastrin stimulates HCl secretion.
Phases of Gastric Secretion:
Cephalic (Reflex) Phase: Triggered by sight, smell, taste, or thought of food.
Gastric Phase: Initiated by food entry into the stomach.
Intestinal Phase: Begins as chyme enters the duodenum.
Regulation of Gastric Motility and Emptying
The stomach responds to filling by stretching to accommodate incoming food. Peristaltic waves move food toward the pylorus, and distension and gastrin increase the force of contraction. Gastric emptying is regulated by the duodenum, which prevents overfilling by controlling the amount of chyme entering.
Gastric Emptying Time: Typically about 4 hours; increased fatty chyme can extend this to 6 hours or more.
Carbohydrate-Rich Chyme: Moves quickly through the duodenum.
Cell Type | Secretion | Function |
|---|---|---|
Mucous Neck Cell | Thin acidic mucus | Unknown |
Parietal Cell | HCl, Intrinsic Factor | Protein denaturation, B12 absorption |
Chief Cell | Pepsinogen, Lipases | Protein and lipid digestion |
Enteroendocrine Cell | Hormones (somatostatin, gastrin) | Regulation of digestion |
Example: Acid reflux is a common disorder caused by weakness or relaxation of the gastroesophageal sphincter, allowing stomach acid to enter the esophagus and cause irritation.
Additional info: The notes have been expanded to include definitions, examples, and a summary table for clarity and completeness.
