 Back
BackReproductive System and Human Development: ANP College Study Guide
Study Guide - Smart Notes

Reproductive System
Male and Female Gonads
The gonads are the primary reproductive organs responsible for producing gametes and hormones. In males, the gonad is the testis, which produces sperm and testosterone. In females, the gonad is the ovary, which produces ova and hormones such as estrogens and progesterone.
Sperm and Testosterone: Sperm are male gametes, and testosterone is a steroid hormone crucial for male sex characteristics and spermatogenesis.
Estrogens: Responsible for female sex characteristics and regulation of the menstrual cycle.
Progesterone: Prepares the body for pregnancy and supports fetal development.
Meiosis vs. Mitosis
Cell division is essential for reproduction and growth. Mitosis produces diploid cells (46 chromosomes), while meiosis produces haploid gametes (23 chromosomes).
Mitosis: Produces two genetically identical daughter cells, maintaining genetic consistency.
Meiosis: Produces four genetically unique haploid cells, ensuring genetic diversity.
Fertilization and Zygote Formation
Fertilization occurs when a sperm cell fuses with a secondary oocyte, forming a zygote with 46 chromosomes. This marks the beginning of a new individual's development.
Spermatogenesis and Sperm Cell Structure
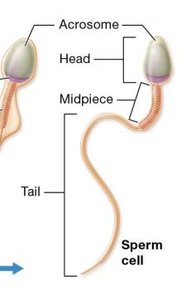
Spermatogenesis is the process of sperm cell development within the seminiferous tubules of the testes. The mature sperm cell has distinct structural regions:
Head: Contains the nucleus and acrosome (enzymes for fertilization).
Midpiece: Packed with mitochondria for energy.
Tail: Flagellum for motility.
Seminiferous Tubule Cell Types
Spermatogenic cells: Form sperm through spermatogenesis.
Sustentacular (Nurse) cells: These cells provide structural support and nourishment to developing sperm cells. They form the blood-testis barrier, which protects sperm from the immune system, and secrete substances that aid in sperm development.
Interstitial (Leydig) cells: Produce testosterone.
Myoid cells: Contract to move sperm and fluids.
Sperm Pathway and Maturation
Sperm travel from the seminiferous tubules → straight tubules → rete testis → efferent ductules → epididymis (site of maturation and storage).
Epididymis: Long, coiled tube with head, body, and tail regions; sperm mature and are stored here.
Male Accessory Glands
Seminal Vesicles: Produce seminal fluid (60-70% of semen; contains fructose, prostaglandins, proteins).
Prostate Gland: Contributes enzymes, citrate, PSA, and antimicrobial chemicals.
Bulbourethral Glands: Produce mucus-like fluid to lubricate and neutralize urethra.
Hormonal Regulation of Spermatogenesis
Testosterone production is regulated by the hypothalamic-pituitary-gonadal (HPG) axis:
GnRH (hypothalamus) → LH & FSH (anterior pituitary)
LH stimulates Leydig cells (testosterone production)
FSH stimulates sustentacular cells (inhibin and ABP production)
Male Sexual Response
Erection: Parasympathetic control; increased blood flow to erectile tissues.
Ejaculation: Sympathetic control; emission and expulsion of semen.
Orgasm: Coincides with ejaculation, followed by a refractory period.
Effects of Testosterone
Growth and maintenance of reproductive organs
Development of secondary sex characteristics
Bone density, muscle growth, libido
Female Reproductive System
Internal Genitalia
Ovaries: Produce ova and hormones.
Uterine Tubes: Transport oocyte; site of fertilization.
Uterus: Site of implantation and fetal development.
Vagina: Copulatory organ; passageway for menstrual flow and childbirth.
Oogenesis and Follicle Development
Oogenesis begins before birth and continues until menopause. Follicle development progresses from primordial → primary → secondary → vesicular follicles.
Astresia: Degeneration of non-viable oocytes.
Ovarian Cycle
Follicular Phase: Days 1-14; follicle maturation.
Ovulation: Day 14; LH surge triggers release of oocyte.
Luteal Phase: Days 15-28; corpus luteum produces progesterone.
Female HPG Axis and Hormonal Feedback
GnRH (hypothalamus) → LH & FSH (anterior pituitary)
LH stimulates thecal cells (androgen production)
FSH stimulates granulosa cells (estrogen, inhibin production)
Negative Feedback: Estrogen and inhibin inhibit GnRH, LH, FSH.
Positive Feedback: High estrogen triggers LH surge (ovulation).
Uterine Cycle and Menstruation
The uterine cycle consists of three phases:
Phase | Days | Events |
|---|---|---|
Menstrual | 1-5 | Shedding of stratum functionalis; myometrial contractions |
Proliferative | 6-14 | Regeneration and thickening of endometrium; ovulation at end |
Secretory | 15-28 | Endometrium prepares for implantation; corpus luteum active |
Female Sexual Response
Blood engorgement of vaginal mucosa, vestibule, breasts
Clitoris and nipples become erect
Orgasm: uterine contractions, no refractory period
Contraception Methods
Abstinence: No intercourse
Rhythm Method: Avoid intercourse during fertile periods
Withdrawal: Withdraw before ejaculation
Barrier Methods: Condoms, diaphragms, cervical caps
Hormonal Methods: Birth control pills, vaginal rings, injections
IUD: Prevents fertilization
Surgical: Tubal ligation, vasectomy
Sexually Transmitted Infections (STIs)
Bacterial: Chlamydia, Gonorrhea, Syphilis
Viral: HPV, Herpes Simplex Virus
Parasitic: Trichomoniasis
Human Development
Pregnancy and Gestation
Pregnancy: From conception to birth
Gestation: Lasts about 280 days (40 weeks)
Developmental Periods
Pre-embryonic: First 2 weeks after fertilization
Embryonic: Weeks 3-8; organ formation
Fetal: Weeks 9-38; growth and maturation
Neonatal: Birth to 1 month
Infancy: 1 month to 2 years
Childhood: 2 years to puberty
Adolescence: 10-19 years
Adulthood: After adolescence
Fertilization and Early Development
Fertilization: Fusion of gametes forms a diploid zygote
Capacitation: Sperm become motile and capable of fertilization
Acrosomal Reaction: Sperm release enzymes to penetrate oocyte
Cortical Reaction: Prevents polyspermy
Cleavage: Rapid mitotic divisions; formation of morula and blastocyst
Blastocyst: Trophoblast (placenta) and inner cell mass (embryo)
Implantation and Extraembryonic Membranes
Implantation: Blastocyst invades uterine tissue; trophoblast differentiates
Syncytiotrophoblast: Releases hCG, digests uterine wall
Extraembryonic Membranes: Yolk sac, amnion, allantois, chorion
Gastrulation and Germ Layers
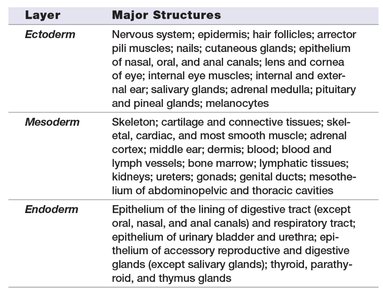
Gastrulation forms three primary germ layers: ectoderm, mesoderm, and endoderm. The primitive streak establishes body axes and guides cell migration.
Germ Layer | Major Structures |
|---|---|
Ectoderm | Nervous system, epidermis, hair follicles, nails, glands, lens/cornea, ear, salivary glands, adrenal medulla, pituitary, pineal glands, melanocytes |
Mesoderm | Skeleton, muscles, dermis, blood, lymphatic system, kidneys, gonads, genitals, connective tissues |
Endoderm | Epithelium of digestive and respiratory tracts, bladder, urethra, thyroid, parathyroid, thymus glands |
Placenta and Fetal Circulation
Placenta: Exchange of oxygen, nutrients, wastes; hormone production; barrier function
Umbilical Artery: Carries deoxygenated blood from fetus to placenta
Umbilical Vein: Carries oxygenated blood from placenta to fetus
Placental Sinus: Maternal blood circulates; chorionic villi contain fetal vessels
Fetal Hemoglobin: Higher affinity for oxygen than maternal hemoglobin
Fetal Period and Neonatal Changes
Fetal Period: Weeks 9-38; rapid growth and organ maturation
IRDS: Infant Respiratory Distress Syndrome due to low surfactant in premature infants
Neonatal Period: Respiratory/circulatory adjustments, temperature regulation, immune protection, kidney function
Maternal Hormones and Physiological Changes
HPL: Breast development, glucose metabolism
Relaxin: Pelvic ligament relaxation, cervical softening
MSH: Pigmentation changes
hCG: Maintains corpus luteum
Prolactin: Milk production
Oxytocin: Uterine contractions, milk let-down
Cortisol: Stress and metabolism regulation
Aldosterone: Blood volume increase
Parturition (Labor) Stages
Stage | Description |
|---|---|
Dilation | Cervix dilates to 10 cm; amnion may rupture; fetus moves into pelvis |
Expulsion | Delivery of newborn; strong contractions; crowning; umbilical cord cut |
Placental | Expulsion of placenta and fetal membranes |
Prenatal Testing
Amniocentesis: Sampling of amniotic fluid for genetic testing (14-20 weeks)
Chorionic Villus Sampling: Sampling of placental tissue for genetic testing (10-12 weeks)
Additional info: All content is expanded and structured for clarity and completeness, suitable for ANP college exam preparation.
