 Back
BackRespiratory Physiology: Neural and Chemical Control of Ventilation
Study Guide - Smart Notes

Respiratory System Overview
Comparison of Skeletal Muscles, Heart, and Respiratory Muscles
The respiratory system utilizes skeletal muscles for ventilation, but its control mechanisms differ from those of other muscle systems.
Skeletal Muscles: Controlled by robust neuromuscular junctions (NMJ), respond rapidly and faithfully to motoneuron commands, and are under voluntary control.
Heart: Possesses pacemaker cells, operates autonomously, and is regulated by the autonomic nervous system rather than voluntary control.
Respiratory Muscles: Includes the diaphragm, intercostals, and abdominal muscles. These are under somatic motoneuron control, allowing voluntary actions (e.g., breath holding), but are also driven by respiratory pacemakers in the medulla and pons, enabling automatic breathing.
Neural Control of Ventilation
Central Pattern Generators (CPGs) and Brainstem Networks
Ventilatory movements are generated by neural networks in the brainstem, functioning as central pattern generators (CPGs) that produce rhythmic breathing.
Medullary Respiratory Neurons: Control inspiratory and expiratory muscles.
Pontine Respiratory Groups: Integrate sensory information and modulate medullary neuron activity.
Rhythmic Breathing: Arises from spontaneously discharging neurons.
Modulation: Breathing is continuously adjusted by chemoreceptor and mechanoreceptor reflexes, as well as input from higher brain centers.
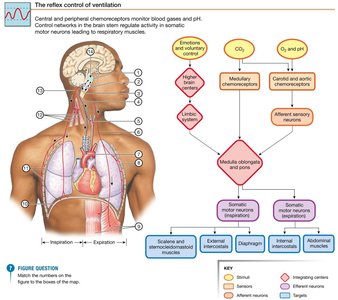
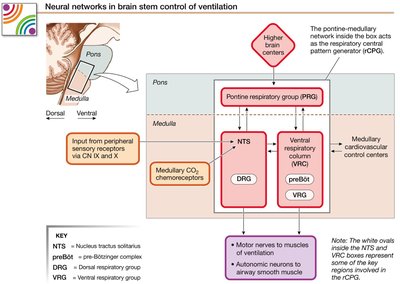
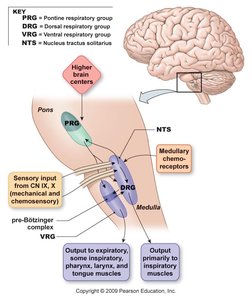
Medullary Respiratory Groups
Dorsal Respiratory Group (DRG): Located in the nucleus tractus solitarius (NTS), sends output to inspiratory muscles via the phrenic and intercostal nerves.
Ventral Respiratory Group (VRG): Includes the pre-Bötzinger complex (basic pacemaker activity), areas for active expiration, and innervates muscles of the larynx, pharynx, and tongue.
Pontine Respiratory Groups (PRG): Modulate the rhythm and depth of breathing.
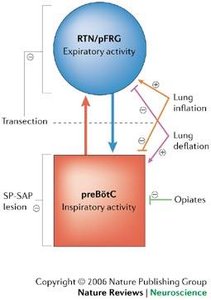
Neural Activity During Quiet Breathing
During quiet breathing, inspiratory neuron activity increases steadily, then shuts off abruptly at the end of inspiration. Expiration occurs passively through elastic recoil of lung tissue.
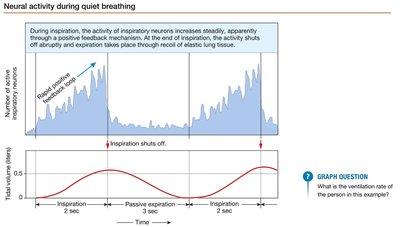
Mechanisms of Rhythmic Breathing
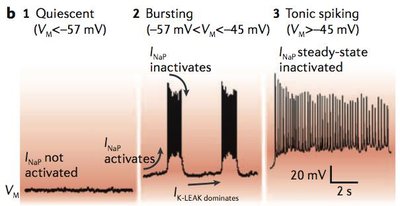
Rhythmic patterns are likely dependent on a persistently active sodium current (INaP), similar to the funny current (If) in cardiac pacemaker cells, but with different voltage dependence.
INaP: Activates during bursting and tonic spiking phases, contributing to the generation of respiratory rhythm.
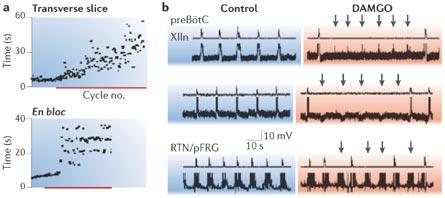
Effects of µ-Opiate Agonists
µ-opiate agonists, such as fentanyl, slow the frequency of inspiration but do not affect active expiration. These drugs are potent and can cross the blood-brain barrier efficiently.
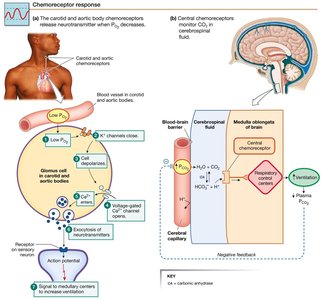
Chemical Control of Ventilation
Role of Chemoreceptors
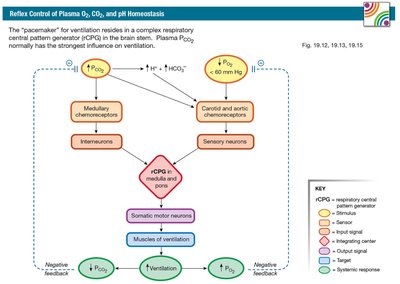
The nervous system detects changes in O2, CO2, and pH to regulate ventilation. Central pattern generators respond to these changes via chemoreceptor input.
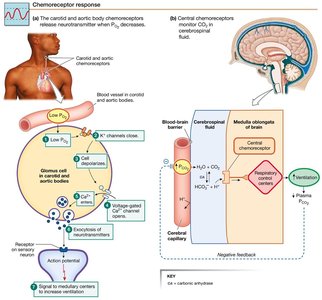
Peripheral Chemoreceptors: Located in carotid bodies, sense changes in PO2, pH, and PCO2. Specialized glomus cells trigger increased ventilation when O2 falls below 60 mm Hg.
Central Chemoreceptors: Located in the CNS, respond to changes in PCO2 by detecting H+ generated from CO2 conversion in brain extracellular fluid.
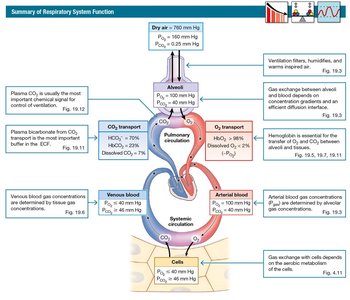
Summary of Respiratory System Function
The respiratory system filters, humidifies, and warms inspired air. Gas exchange occurs between alveoli and blood, and is influenced by diffusion distance and concentration gradients.
CO2 Transport: Most CO2 is carried in plasma as HCO3-, requiring red blood cells for conversion and Cl- for exchange.
O2 Transport: Hemoglobin (Hb) is the major carrier of O2 and a minor carrier of CO2. Hb delivers O2 poorly, unloading only 20-25%.
CO Poisoning: CO binds to Hb at the O2 site with over 200 times higher affinity, making it a silent killer.
Protective Reflexes and Higher Brain Center Influence
Protective Reflexes
Bronchoconstriction: Triggered by irritant receptors in airway mucosa.
Sneezing and Coughing: Protective responses to physical injury or irritation.
Hering-Breuer Inflation Reflex: Prevents over-inflation of the lungs.
Higher Brain Centers
Cerebrum and Hypothalamus: Can modify breath rate and depth, but are not required for ventilation.
Limbic System: Emotional states can affect breathing patterns.
Chemoreceptor Reflexes: Cannot be overridden by higher brain centers.
Summary of Key Concepts
Air Flow: Moves from high to low pressure, governed by physics laws such as Boyle’s Law (), Dalton’s Law (), and Poiseuille’s equation ().
Radius Control: The radius of airways is the major variable under hormonal, paracrine, and autonomic control, mediated by smooth muscles.
Hemoglobin: Major carrier of O2, minor carrier of CO2, and subject to competitive binding by CO.
Ventilation Control: Mediated by skeletal muscles and motoneurons, regulated by CPGs in the brainstem.
Quality Control: Monitored by peripheral and central chemoreceptors.
Respiratory and Cardiovascular Coordination: Both systems work together to meet physiological needs.
Additional info: The notes expand on brief lecture points to provide a comprehensive overview of neural and chemical control of ventilation, including relevant physiological laws and mechanisms.
