 Back
BackSelf-Care and Pathophysiology of Dermatitis: ANP Study Guide
Study Guide - Smart Notes

Dermatitis: Overview and Classification
Definition and Types
Dermatitis is a dermatologic condition characterized by erythema (redness) and inflammation of the skin. It is classified into several types based on etiology and clinical presentation:
Irritant Contact Dermatitis (ICD): Caused by direct exposure to irritants.
Allergic Contact Dermatitis (ACD): Resulting from immunogenic reaction to antigens.
Atopic Dermatitis (AD): Also known as eczema, associated with hereditary and environmental factors.
Diaper Dermatitis: A subset of ICD, commonly seen in infants.
Irritant Contact Dermatitis (ICD)
Pathophysiology and Etiology
ICD is an inflammatory reaction resulting from tissue damage when the skin is exposed to an irritant. Common occupational exposures include agriculture, healthcare, and manufacturing, where repeated contact with chemicals, acids, soaps, and sanitizers is frequent.
Exposure: Can be single (strong irritants) or multiple (mild irritants).
Localization: Symptoms are typically limited to the area exposed.
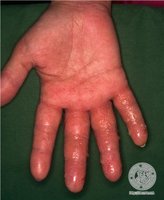


Clinical Presentation
ICD presents with erythema, edema, and stinging/burning of the affected skin. Lesions and rash are localized to the contact area. 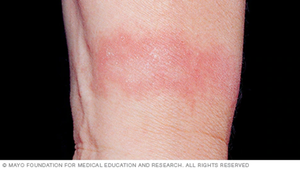
Treatment Goals and Approaches
Remove Irritant: Wash exposed area with tepid water and mild soap to reduce contact time.
Symptom Relief: Use astringent soaks (e.g., Burow’s solution) for drying and cooling effects.
Protect Skin: Apply emollients (petrolatum, ceramides) to restore moisture and prevent further exposure. Products with high lipid content are preferred.
Itch Relief: Colloidal oatmeal can be used for itching; pat skin dry after use.



Prevention and Products to Avoid
Prevention: Wear protective clothing, use emollients and barrier creams.
Avoid: Topical corticosteroids (hydrocortisone) and anesthetics (caines) due to risk of allergic reactions.


When to Refer
Children under 2 years
Large body surface area involved
Involvement of mouth, face, eyes, neck, or genitals
Symptoms persist beyond 7 days
Chronic symptoms
Diaper Dermatitis
Definition and Epidemiology
Diaper dermatitis is acute inflammation of the skin in the diaper area, primarily caused by urine and feces. It is the most common dermatologic issue in infants, but can occur in any age group with incontinence. 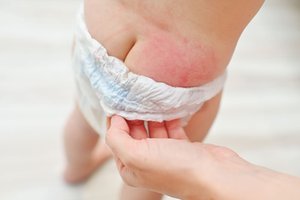
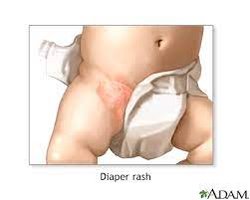
Clinical Presentation and Complications
Red patches and lesions, maroon or purplish on darker skin
Rapid onset
If untreated, can lead to ulcerations, skin infections, or urinary/genital tract infections
Treatment Approach (Mnemonic: ABCDE)
A: Air – allow diaper area to dry, include diaper-free time
B: Barrier – use barrier cream liberally
C: Clean – use soft cloth and warm water or appropriate baby wipe
D: Diaper – change frequently, disposable preferred
E: Educate – adults on hygiene and treatment options
Skin Protectants
Skin protectants provide a physical barrier and lubrication, decreasing friction and promoting healing. Common ingredients include petrolatum, zinc oxide, dimethicone, and lanolin. 


Products and Ingredients to Avoid
Powders: Cornstarch and talc pose inhalation risk.
Hydrocortisone: Not recommended without medical referral due to risk of secondary infection and increased absorption.
Caine ingredients: Risk of allergic reactions.



When to Refer
Rash persists after 7 days of treatment
Possible bacterial or fungal infection
Broken skin or rash extends beyond diaper area
Frequent recurrence
Comorbid conditions causing immunosuppression
Allergic Contact Dermatitis (ACD)
Pathophysiology and Triggers
ACD is an immunogenic reaction when skin is exposed to an antigen. The reaction does not appear on first contact but develops after sensitization.
Onset: 24 hours to 21 days in naïve patients; 24-48 hours in sensitized patients
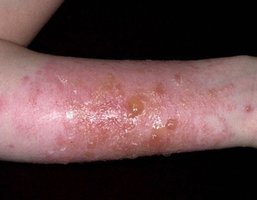
Clinical Presentation
Itching, erythema, edema
Vesicles, bullae, papules (not seen in ICD)
May or may not have burning/stinging
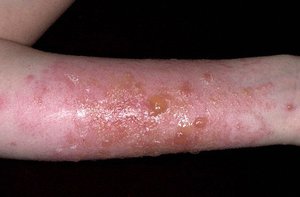
Urushiol-Induced ACD
Urushiol is found in poison ivy, oak, and sumac. Sensitivity is common, and cross-sensitivity occurs. The rash changes appearance over time and can be widespread. 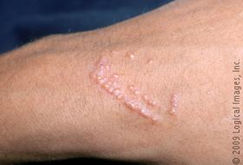
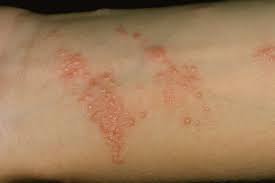
Severe Cases and Complications
Extensive edema, eyelid involvement, intense pruritus
Numerous vesicles and bullae
Secondary infections: S. aureus, Group A Streptococcus, E. coli


Treatment Goals and Approaches
Remove Allergen: Wash contaminated items and exposed skin with mild soap and water within 30 minutes.
Products: Dishwashing soap, urushiol-specific products, oil-removing cleansers (Goop).




Treat Inflammation
Hydrocortisone cream (not ointment) for moderate, isolated rash
Suppresses cytokines, histamine, and prostaglandins
Do not use bandages or dressings
Rx strength may be required for urushiol ACD

Hydrocortisone Adverse Effects
Short-term use is key
Topical withdrawal syndrome with continuous use
Thinning of skin/atrophy (rare with OTC strength)
Do not use on eyes/eyelids
Itch Relief and Debris Removal
Cold or tepid soap-less showers
Trim fingernails
Colloidal oatmeal, calamine for drying lesions
First-generation oral antihistamines for sleep
Products to Avoid
Topical anesthetics and antihistamines: Increase sensitization/allergy
Hydrocortisone for children under 2 years without referral
Ointment formulation when oozing is present
Preventative Measures
Identify Toxicodendron plants
Wear protective clothing
Wash clothing and skin after exposure
Clip and clean nails
When to Refer
Children under 2 years
Numerous large bullae
Intense pruritus, severe vesicle/bullae formation
Swelling of body/extremity
Eye/eyelid involvement
Mucous membrane involvement
Signs of infection
No improvement within 7 days
Atopic Dermatitis (AD)
Definition and Epidemiology
Atopic dermatitis, or eczema, is characterized by erythematous, edematous, papular, and crusty skin. Patients often have xerosis (dry skin).
10-20% of children affected
80% have mild form
Increased risk for asthma and allergic rhinitis
Pathophysiology
Inflammation due to overexpression of inflammatory factors
Mutation in filaggrin protein reduces skin barrier effectiveness
Decreased lipids and ceramides impair moisture retention
Hereditary: Family history in 70% of cases
Clinical Presentation
Intense pruritus
Dry, scaly, crusty skin
Lesions may be papular and edematous
Treatment Approach
Stop itch-scratch cycle: Trim fingernails, use colloidal oatmeal
Moisturizing: Emollient application 3-4 times daily, especially post-shower
Anti-inflammatory: Hydrocortisone topical (>2 years old), cream/lotion for weeping lesions, ointment for dry/scaly skin
Barrier restoration: Creams and ointments preferred over lotions
Hydrocortisone Use
Safe in children >2 years
Apply thin film 1-2 times daily for 7 days
Avoid eyes, eyelids, and compromised skin
Do not wrap or band area
Do not apply to diaper area
Improvement expected in 24-48 hours
Skin Hydration
Short baths (lukewarm), pat dry
Drink plenty of water
Maintain humid environment
Avoid Triggers
Excessive skin washing
Dyes, preservatives, irritating clothes
Irritating soaps/detergents
Hot showers
Allergens, cosmetics/fragrances
Cold/dry environment
Prevent Infections and Flare-Ups
Trim, clean fingernails
Sleep in "kid mittens"
Maintain skin hydration
Avoid triggers
Products to Avoid
Topical antihistamines and caine products: Increase sensitization
When to Refer
Moderate-severe condition with intense pruritus
Large area involvement
Children <1 year (or <2 years in practice)
Signs of infection
Face involvement
Involvement of areas that rub together (axilla, groin, skin folds)
No improvement after 2-3 days of treatment
Summary Table: Dermatitis Types and Key Features
Type | Etiology | Clinical Features | Treatment | When to Refer |
|---|---|---|---|---|
Irritant Contact Dermatitis | Direct exposure to irritants | Erythema, edema, localized rash | Remove irritant, emollients, avoid corticosteroids | <2 years, large area, face/genitals, no improvement in 7 days |
Diaper Dermatitis | Urine/feces, occlusion | Red patches, lesions in diaper area | Barrier creams, frequent diaper changes, avoid powders | Persistent rash, infection, broken skin, recurrence |
Allergic Contact Dermatitis | Immunogenic reaction to antigen | Itch, erythema, vesicles/bullae | Remove allergen, hydrocortisone cream, avoid anesthetics | <2 years, severe symptoms, eye/mucous membrane involvement |
Atopic Dermatitis | Hereditary, environmental | Pruritus, dry/scaly skin, papular lesions | Moisturizers, hydrocortisone, avoid triggers | Moderate-severe, infection, face, no improvement |
Case Studies: Application of Concepts
Case of JD
54 y/o surgical nurse with irritated, dry, cracked hands, pruritus, erythema
Likely ICD due to occupational exposure
Self-treatment: Remove irritant, emollients, avoid corticosteroids
Education: Protective measures, skin hydration, avoid triggers
Case of AJ
21 y/o college student with erythema, swelling, pruritus on ears after wearing new earrings
Likely ACD due to sensitization to metal
Self-treatment: Remove allergen, hydrocortisone cream, avoid triggers
Education: Allergen identification, skin care, when to refer
Case of CS
28 y/o with persistent itching, dry/thickened skin, yellow exudates, crusting
Symptoms worsened after moving; tried hydrocortisone without relief
Not eligible for self-treatment due to infection signs
Recommendation: Refer to PCP, maintain skin hydration, avoid triggers
