 Back
BackSkeletal, Cardiac, and Smooth Muscle: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue Overview
Major Functions of Muscle Tissue
Muscle tissue is essential for movement, posture, and the generation of heat. It is characterized by several unique properties that enable its function:
Contractility: The ability of muscle cells to contract, drawing proteins together. Contraction does not always mean shortening of the cell.
Excitability: Muscle cells respond to stimuli such as chemical signals, mechanical stretch, or electrical signals, generating electrical changes across their plasma membrane.
Conductivity: Electrical changes are rapidly conducted along the plasma membrane, similar to electrical impulses in wires.
Distensibility: Muscle cells can be stretched up to three times their resting length without damage.
Elasticity: Muscle cells return to their original shape after being stretched.
Skeletal Muscle Fiber Structure
Structural Elements and Properties
Skeletal muscle fibers are long, cylindrical cells with multiple nuclei and striations. Their structure is specialized for contraction and force generation.
Cell Shape and Size: Thin cylinders, much longer than most cells (up to 30 cm).
Striations: Striped appearance due to the arrangement of contractile proteins.
Multiple Nuclei: Result from the fusion of myoblasts during development.
Organization of a Myofibril
Myofibrils are composed of hundreds to thousands of protein bundles called myofilaments, which are classified as contractile, regulatory, or structural proteins.
Thick, Thin, and Elastic Filaments
Three types of myofilaments are found in skeletal muscle:
Thick Filaments: Composed primarily of myosin proteins, which have heads that bind to actin and hydrolyze ATP.
Thin Filaments: Composed of actin, troponin, and tropomyosin. Actin contains active sites for myosin binding.
Elastic Filaments: Composed of titin, which provides elasticity and stabilizes the myofibril.
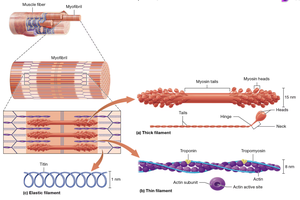
Myofibril and Muscle Fiber Organization
Muscle fibers are organized into fascicles, which are bundled together to form muscles. Each fiber contains myofibrils, which are made up of repeating units called sarcomeres.
Electrophysiology of Muscle Fibers
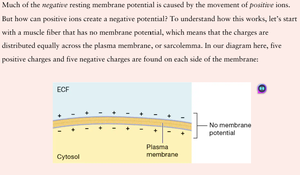
Resting Membrane Potential (RMP)
The resting membrane potential is generated by the movement of ions across the sarcolemma. The sodium-potassium pump (Na+/K+ ATPase) maintains concentration gradients by moving three sodium ions out and two potassium ions in, powered by ATP hydrolysis.
Concentration Gradient: Difference in ion concentration across the membrane.
Electrochemical Gradient: Combined effect of concentration and electrical gradients.
Sequence of Events in Muscle Action Potential
Depolarization: Voltage-gated sodium channels open, sodium enters, membrane potential becomes less negative.
Repolarization: Sodium channels close, potassium channels open, potassium exits, membrane potential returns to negative.
Muscle Contraction and Relaxation
Anatomy of the Neuromuscular Junction
Axon Terminal: Contains synaptic vesicles with acetylcholine (ACh).
Synaptic Cleft: Space between axon terminal and muscle fiber, contains enzymes to break down ACh.
Motor End Plate: Specialized region of sarcolemma with ACh receptors (ligand-gated ion channels).
Excitation-Contraction Coupling
End-plate potential stimulates an action potential.
Action potential propagates down T-tubules.
Depolarization opens calcium channels in the sarcoplasmic reticulum, releasing calcium into the cytosol.
Contraction Cycle
Calcium binds to troponin, exposing actin active sites.
Myosin heads bind to actin, forming crossbridges.
ATP hydrolysis powers the movement of myosin heads.
Muscle contracts and generates tension.
Energy Sources for Muscle Contraction
Immediate, Glycolytic, and Oxidative Mechanisms
Muscle fibers use several energy sources to generate ATP:
Immediate: Creatine phosphate donates phosphate to ADP to form ATP.
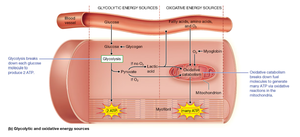
Glycolytic: Glycolysis breaks down glucose to produce ATP and lactic acid.
Oxidative: Oxidative catabolism in mitochondria uses oxygen to produce large amounts of ATP.
Muscle Fiber Types
Type I and Type II Muscle Fibers
Type I (Slow-Twitch): Small to intermediate diameter, slow contraction, high endurance, rich in myoglobin and mitochondria, red color.
Type II (Fast-Twitch): Larger diameter, rapid contraction, fatigues quickly, relies on glycolytic energy, less myoglobin, white color. Subtypes: IIa (fast oxidative glycolytic), IIx (fast glycolytic).
Muscle Tension and Performance
Muscle Tension at Fiber and Organ Level
Twitch Contractions: Response to a single action potential, includes latent, contraction, and relaxation periods.
Motor Unit: A single motor neuron and all the muscle fibers it innervates. Fine motor control uses small units; gross motor uses large units.
Muscle Tone: Involuntary activation of motor units maintains posture, stabilizes joints, generates heat, and keeps muscles ready for action.
Effects of Physical Conditioning
Endurance Training: Increases oxidative capacity, mitochondria, and blood supply.
Resistance Training: Increases muscle fiber size and strength.
Muscle Fatigue
Causes: Depletion of metabolites, decreased oxygen, accumulation of chemicals, environmental stress.
Recovery: Excess postexercise oxygen consumption (EPOC), heat dissipation, restoration of ion concentrations.
Smooth and Cardiac Muscle
Cardiac Muscle Overview
Striated, with sarcomeres, T-tubules, and extensive sarcoplasmic reticulum.
Short, branched cells with one or two nuclei, abundant myoglobin and mitochondria.
Intercalated discs connect cells for coordinated contraction.
Autorhythmic due to pacemaker cells; does not require nervous system stimulation.
Smooth Muscle Contraction
Contraction involves myosin light-chain kinase and calmodulin.
Does not have sarcomeres; contraction is slower and sustained.
Clinical and Applied Concepts
Duchenne Muscular Dystrophy (DMD)
Caused by defective gene for dystrophin (structural protein).
Symptoms: Weakness, gait abnormalities, life expectancy ~20 years.
Rigor Mortis
Stiffening of muscles after death due to lack of ATP for calcium reuptake and myosin detachment.
Botulism and Botox
Botulinum toxin blocks ACh release at NMJ, causing paralysis.
Medical uses: Migraine relief, muscle spasm treatment, cosmetic applications.
Delayed Onset Muscle Soreness (DOMS)
Caused by minor structural damage and remodeling of myofibrils, especially after isotonic eccentric contractions.
Review and Study Questions
Which muscle is voluntary? Skeletal muscle.
Which property is not common to all muscle cells? Polarity.
What happens if a muscle cell is distensible but not elastic? It will not return to its resting length.
What is a triad? A T-tubule and two terminal cisternae.
Which protein is found in thick filaments? Myosin.
What happens if thin and thick filaments cannot move relative to each other? No contraction or tension generation.
Electrochemical gradient for potassium drives potassium out of the cell; for sodium, into the cell.
During depolarization: Sodium ion channels open and sodium enters the cell.
Immediate energy source for contraction: Creatine phosphate.
Oxidative catabolism is "aerobic" because mitochondrial reactions require oxygen.
Contraction in response to a single action potential: Twitch.
Compared to Type I, Type II fibers: Generate more force.
Motor unit: A single motor neuron and all the muscle fibers it innervates.
Lowering a weight slowly: Isotonic eccentric contraction.
Muscle fatigue: Inability to maintain exercise intensity.
Muscle after cast removal: Atrophied.
Rapid breathing after exercise: All of the above (CO2 removal, ATP production, heat loss).
Smooth muscle contraction involves myosin light-chain kinase.
Cardiac muscle cells do not contain abundant hemoglobin.
Asthma response: False (calcium binding causes contraction, not relaxation).
