 Back
BackSkeletal Muscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Skeletal Muscle Tissue
Overview of the Muscular System
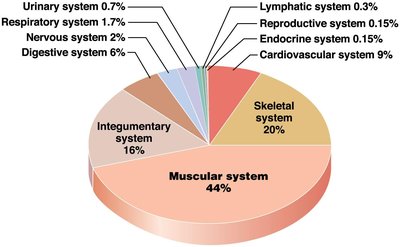
The muscular system comprises nearly half of the body's weight and includes approximately 700 muscles, each varying in size, shape, and function. The performance of muscles depends on their fiber organization and skeletal attachments.
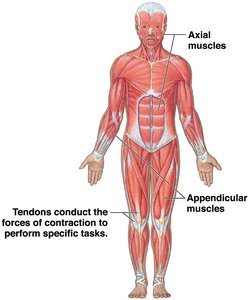
Axial division: Muscles that support and position the axial skeleton.
Appendicular division: Muscles that support, move, and brace the limbs.
Functions of Skeletal Muscle Tissue
Skeletal muscle tissue performs several essential functions:
Produce body movement: Muscle tendons pull and move bones.
Maintain posture and body position: Stabilize joints.
Support soft tissues: Surround, support, and shield internal structures.
Guard body entrances/exits: Sphincters provide voluntary control of swallowing, defecation, and urination.
Maintain body temperature: Muscle contraction generates heat.
Store nutrients: Muscle proteins can break down to release amino acids for energy or glucose synthesis.
Muscle Tissue Types
Classification and Characteristics
Muscle tissue consists of contractile cells and is classified into three types:
Skeletal muscle: Voluntary, attached to bones, produces movement by pulling on bones.
Cardiac muscle: Involuntary, found only in the heart, pumps blood.
Smooth muscle: Involuntary, found in walls of hollow organs and small arteries.
Functional Characteristics of Muscles
Muscle tissue exhibits five key functional characteristics:
Excitability: Ability to receive and respond to stimuli.
Conductivity: Ability to transmit a wave of excitation.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched or extended.
Elasticity: Ability to return to original length after stretching.

Microscopic Anatomy of Skeletal Muscle
Muscle Fiber Structure
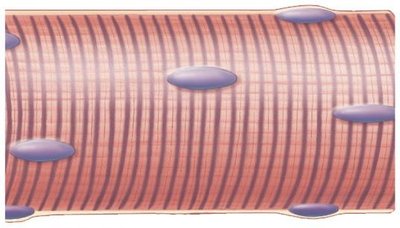
Skeletal muscle fibers are large, multinucleate cells containing bundles of protein filaments called myofibrils. The arrangement of myofibrils gives skeletal muscle its characteristic striations.
Sarcolemma: Plasma membrane of the muscle fiber.
Sarcoplasm: Cytoplasm of the muscle fiber.
Myofibrils: Cylindrical structures running the length of the muscle fiber.
Nuclei: Pushed to the edge of the cell.
Mitochondria: Numerous, providing energy for contraction.

Development and Repair
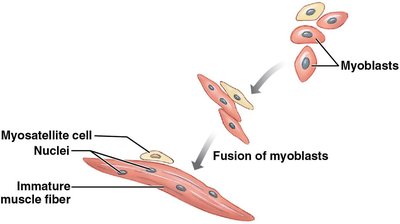
Muscle fibers develop from embryonic cells called myoblasts, which fuse to form multinucleate cells. Some myoblasts remain as myosatellite cells, which aid in muscle repair.
Connective Tissue Organization
Three layers of connective tissue organize skeletal muscle:
Endomysium: Surrounds each muscle fiber.
Perimysium: Surrounds bundles of muscle fibers (fascicles).
Epimysium: Surrounds the entire muscle.
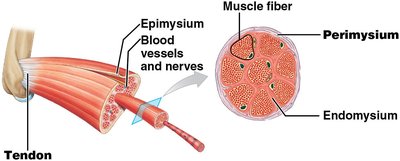
Muscle Fiber Internal Structure
Sarcolemma, T Tubules, and Sarcoplasmic Reticulum
The sarcolemma is the plasma membrane of the muscle fiber, and T tubules are extensions that allow electrical signals to penetrate the cell. The sarcoplasmic reticulum stores calcium ions, which are essential for muscle contraction.
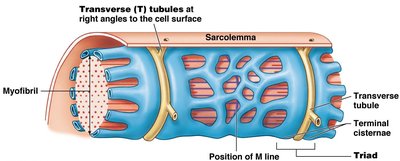
Myofilaments and Sarcomeres
Myofibrils contain myofilaments, which are organized into repeating units called sarcomeres. Sarcomeres are the functional units of muscle contraction.
Thin filaments: Composed mainly of actin.
Thick filaments: Composed mainly of myosin.
Striations: Created by the arrangement of thick and thin filaments.
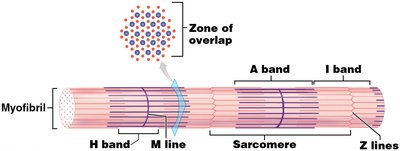
Sliding Filament Theory
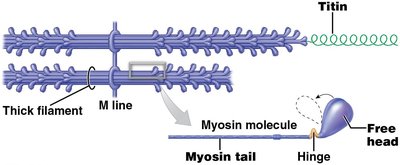
Structure of Thin and Thick Filaments
Thin filaments are attached to Z lines and composed of four main proteins: F-actin, nebulin, tropomyosin, and troponin. Thick filaments are made of myosin molecules and titin, which connects thick filaments to Z lines.
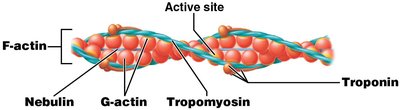
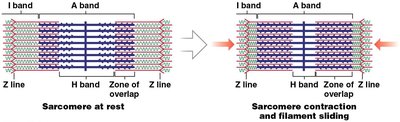
Mechanism of Muscle Contraction
During contraction, thin filaments slide over thick filaments, causing the H and I bands to shrink and Z lines to move closer together. The A band remains unchanged.
Excitable Membranes and Action Potentials
Membrane Potentials
Excitable membranes create electrical changes by distributing charged ions unequally across the cell membrane. The resting membrane potential for skeletal muscle fibers is about –85 mV.
Action Potential Propagation
Action potentials propagate along the plasma membrane, allowing rapid communication and contraction.
Neuromuscular Junction
Structure and Function
The neuromuscular junction (NMJ) is where a motor neuron controls a skeletal muscle fiber. It consists of the axon terminal, motor end plate, and synaptic cleft.
Axon terminal: Contains vesicles with acetylcholine (ACh).
Motor end plate: Has ACh receptors and junctional folds.
Synaptic cleft: Contains acetylcholinesterase (AChE) to break down ACh.
Events at the Neuromuscular Junction
Action potential arrives at axon terminal; ACh released.
ACh binds to receptors on motor end plate; Na+ enters muscle fiber.
Na+ influx generates action potential in sarcolemma.
Action potential spreads across sarcolemma and down T tubules.
Sarcoplasmic reticulum releases Ca2+; contraction begins.
Muscle Contraction Cycle
Steps in the Contraction Cycle
Resting sarcomere: Myosin heads are energized and cocked.
Contraction begins: Ca2+ arrives from SR.
Active sites exposed: Ca2+ binds to troponin, exposing actin sites.
Cross-bridges form: Myosin heads bind to actin.
Power stroke: Myosin heads pivot, pulling Z lines together.
Cross-bridges detach: ATP binds to myosin, releasing it from actin.
Myosin reactivates: ATP is hydrolyzed, re-cocking the myosin head.
Muscle Tension and Contraction Types
Muscle Twitch and Tension
A muscle twitch is a single stimulus-contraction-relaxation sequence. Tension produced depends on the amount of tension per fiber and the number of fibers stimulated.
Types of Contractions
Isotonic contraction: Muscle length changes while tension remains constant.
Isometric contraction: Muscle length does not change; tension is generated but does not exceed the load.
Muscle Activity and Leverage
Muscle Groups and Actions
Agonist (prime mover): Responsible for movement.
Antagonist: Opposes the agonist.
Synergist: Assists the agonist.
Fixator: Stabilizes joints.
Levers in the Body
Levers are rigid structures that move when force is applied. There are three classes of levers:
First-class: Fulcrum between force and load (e.g., head).
Second-class: Load between force and fulcrum (e.g., wheelbarrow).
Third-class: Force between load and fulcrum (most common in body).
Energy for Movement
Sources of ATP
Anaerobic metabolism: Glycolysis produces ATP without oxygen.
Aerobic metabolism: Citric acid cycle and electron transport chain produce most ATP.
Creatine phosphate: Reforms ATP for short bursts of energy.
Metabolic Levels
Low: Muscles burn lipids, ATP surplus.
Moderate: Muscles burn lipids and glucose, ATP production meets needs.
High: Muscles burn mostly glucose, anaerobic metabolism increases, leading to fatigue.
Muscle Recovery and Fatigue
Cori Cycle and Oxygen Debt
The Cori cycle shuttles lactate to the liver, where it is converted to glucose and returned to muscles. Oxygen debt is the amount of oxygen required to restore normal conditions after exertion.
Muscle Fiber Types
Slow, Fast, and Intermediate Fibers
Slow fibers (Type I): Aerobic, fatigue-resistant, dark red, postural muscles.
Fast fibers (Type IIx): Anaerobic, powerful, fatigue quickly, large diameter.
Intermediate fibers (Type IIa): Resemble fast fibers, more capillaries, more fatigue-resistant.
Muscular Disorders
Hypertrophy and Atrophy
Hypertrophy: Muscle enlargement due to increased myofibrils, mitochondria, and glycogen.
Atrophy: Decreased muscle size, tone, and power due to reduced stimulation.
Common Disorders
Muscular dystrophy: Inherited diseases causing progressive weakness.
Polio: Viral disease causing paralysis.
Tetanus: Bacterial toxin causing sustained contractions.
Myasthenia gravis: Autoimmune disease causing loss of ACh receptors.
Rigor mortis: Generalized contraction after death due to ATP depletion.
