 Back
BackSkeletal, Muscular, and Nervous System Essentials: Structure, Function, and Physiology
Study Guide - Smart Notes

Functions of the Skeletal System
Overview of Skeletal Functions
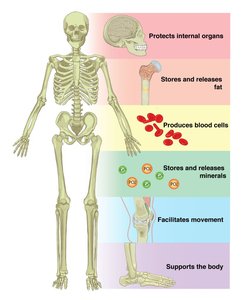
The skeletal system provides the framework for the body and supports a variety of essential physiological functions. Bones are dynamic organs that contribute to movement, protection, and homeostasis.
Support: Bones form the structural framework for the body and support soft tissues and organs.
Protection: The skeleton protects vital organs such as the brain (skull), spinal cord (vertebrae), and thoracic organs (rib cage).
Anchorage: Bones act as levers for muscle action, enabling movement.
Mineral Storage: Bones store minerals, primarily calcium and phosphorus, which are released into the bloodstream as needed.
Blood Formation: Hematopoiesis, the production of blood cells, occurs in red bone marrow.
Fat Storage: Yellow bone marrow stores triglycerides, serving as an energy reserve.
Hormone Production: Osteocalcin, produced by bones, helps regulate insulin secretion, glucose homeostasis, and energy expenditure.
Bone Structure and Composition
Compact Bone
Compact bone forms the dense outer layer of bones, providing strength and protection. It is organized into cylindrical units called osteons, which resemble tree rings and are composed of concentric layers (lamellae) surrounding a central canal containing blood vessels and nerves. Osteocytes reside in lacunae between the lamellae.
Bone Matrix
The bone matrix is a composite material that gives bone its unique properties:
Organic Component (1/3): Mainly collagen and other proteins, providing flexibility and tensile strength.
Inorganic Component (2/3): Primarily calcium phosphate and other minerals, conferring hardness and resistance to compression.
Bone Growth and Remodeling
Growth and Remodeling Processes
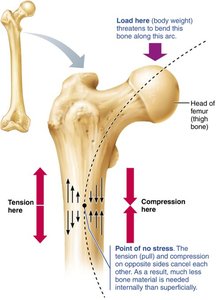
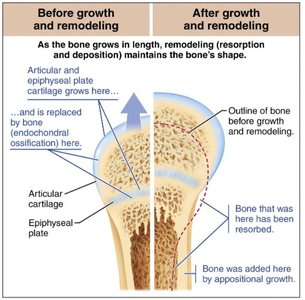
Bones are dynamic and remodel throughout life in response to mechanical stress and physiological needs. Osteoblasts deposit new bone matrix, while osteoclasts resorb bone tissue. This process allows bones to adapt to changing forces and repair microdamage.
Appositional Growth: Bones increase in diameter as new bone is added beneath the periosteum.
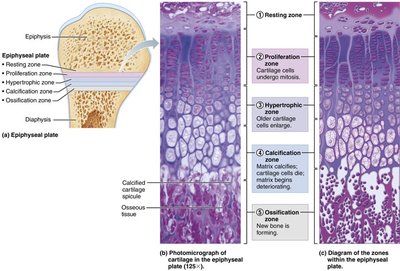
Epiphyseal Plate: Longitudinal growth occurs at the epiphyseal plate (growth plate) until it closes after adolescence.
Hormonal Regulation of Bone Growth
Bone growth is regulated by several hormones:
Growth Hormone: Stimulates epiphyseal plate activity in children.
Thyroid Hormone: Modulates growth hormone activity for proportional growth.
Sex Hormones (Testosterone and Estrogens): Promote growth spurts and induce epiphyseal plate closure at puberty.
Imbalances in these hormones can lead to abnormal skeletal development.
Calcium Homeostasis
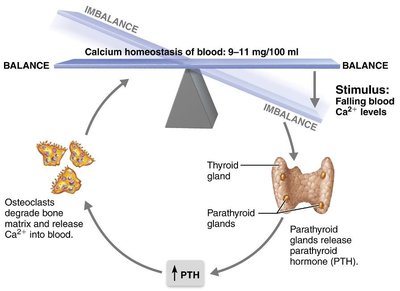
Bone acts as a reservoir for calcium, which is tightly regulated in the blood (9–11 mg/100 mL). When blood calcium levels fall, the parathyroid glands release parathyroid hormone (PTH), stimulating osteoclasts to degrade bone matrix and release calcium into the blood.
Fractures and Bone Repair
Types of Fractures
Fractures are classified by:
Position of Bone Ends: Nondisplaced (normal alignment) or displaced (misaligned).
Completeness: Complete (broken through) or incomplete (partial break).
Skin Penetration: Open (compound) or closed (simple).
Fracture Treatment and Repair
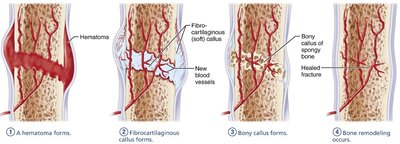
Treatment involves reduction (realignment) and immobilization. Healing occurs in four stages:
Hematoma formation
Fibrocartilaginous callus formation
Bony callus formation
Bone remodeling
Muscle Tissue Types and Function
Types of Muscle Tissue
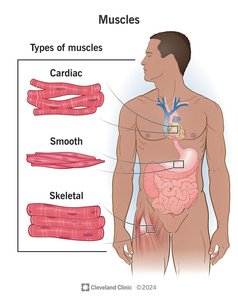
There are three types of muscle tissue:
Skeletal Muscle: Voluntary, striated muscle attached to bones for movement.
Cardiac Muscle: Involuntary, striated muscle found only in the heart.
Smooth Muscle: Involuntary, non-striated muscle found in walls of hollow organs.
The muscular system refers specifically to skeletal muscle.
Muscle Excitation and Contraction
Muscle Excitation
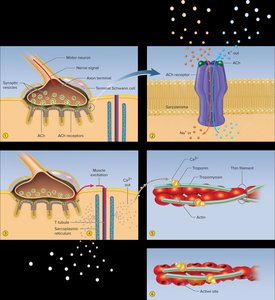
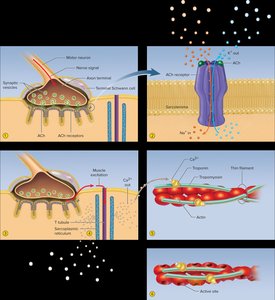
Excitation is the process of converting a nerve signal into a muscle action potential. It occurs in three steps:
Nerve signal arrives at the neuromuscular junction, causing release of acetylcholine (ACh).
ACh binds to receptors on the sarcolemma, opening ion channels and allowing sodium to enter and potassium to exit.
Ion movement generates an action potential that spreads across the muscle fiber.
Preparing for Contraction
Excitation triggers a cascade that allows myosin and actin to interact:
Action potential travels down T tubules, opening calcium channels in the sarcoplasmic reticulum.
Calcium binds to troponin on thin filaments.
Tropomyosin shifts, exposing myosin-binding sites on actin.
Sliding Filament Model of Contraction
Muscle contraction occurs as thick (myosin) and thin (actin) filaments slide past each other, shortening the sarcomere. The cycle involves:
Myosin head hydrolyzes ATP and moves to a high-energy position.
Myosin binds to actin, forming a cross-bridge.
Power stroke: myosin head pivots, pulling actin filament.
ATP binds to myosin, causing it to detach and reset for another cycle.
Muscle Relaxation
Relaxation occurs when nerve stimulation ceases, ACh is broken down, calcium is reabsorbed, and the troponin-tropomyosin complex blocks myosin binding sites. Muscles maintain a state of partial contraction called muscle tone, which stabilizes joints.
Muscle Metabolism
ATP Production Pathways
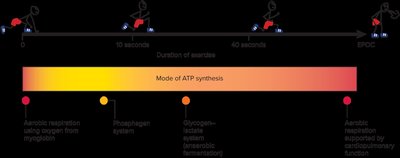
Anaerobic Fermentation: Converts glucose to lactate, yielding 2 ATP per glucose without oxygen. Used for short bursts of activity.
Aerobic Respiration: Oxidizes glucose to CO2 and H2O in mitochondria, yielding about 30 ATP per glucose. Requires oxygen and is more efficient.
Phosphagen System: Uses creatine phosphate to rapidly regenerate ATP for short, intense activity (about 6 seconds of sprinting).
Muscle Fatigue and Endurance
Fatigue results from prolonged muscle use and is caused by depletion of energy stores, ion imbalances, and accumulation of metabolic byproducts. Endurance depends on myoglobin and glycogen stores, capillary density, mitochondrial number, oxygen uptake, and psychological factors.
Nervous System Structure and Function
Cerebrospinal Fluid (CSF)
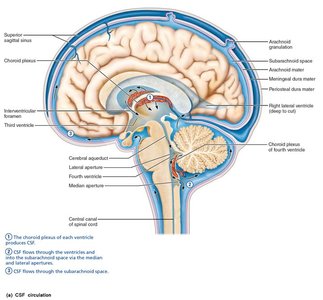
CSF is produced by ependymal cells lining the brain's ventricles. It provides a stable chemical environment, removes wastes, cushions the brain, and provides buoyancy.
Overview and Functions of the Nervous System
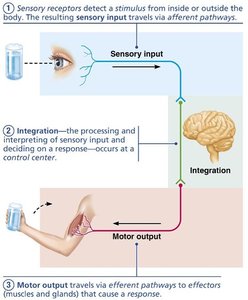
The nervous system is the body's master control and communication system, using electrical and chemical signals for rapid, specific responses.
Sensory Input: Gathering information from sensory receptors about internal and external changes.
Integration: Processing and interpreting sensory input to determine a response.
Motor Output: Activating effectors (muscles and glands) to produce a response.
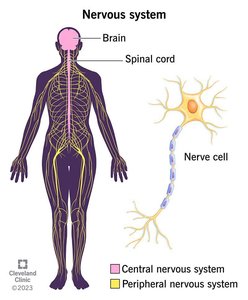
Anatomical Subdivisions
Central Nervous System (CNS): Brain and spinal cord; processes and integrates information.
Peripheral Nervous System (PNS): All neural tissue outside the CNS; relays information to and from the CNS.
Neurons and Action Potentials
Neuron Structure: Dendrites
Dendrites are branched extensions of neurons that receive input from other neurons. Dendritic spines increase connectivity and are involved in learning and memory.
Generating an Action Potential
Action potentials are rapid changes in membrane potential that transmit signals along neurons. The process involves four steps:
Resting State: All voltage-gated Na+ and K+ channels are closed; resting membrane potential is maintained.
Depolarization: Na+ channels open, Na+ enters, and the membrane potential becomes positive.
Repolarization: Na+ channels inactivate, K+ channels open, and K+ exits, restoring negativity.
Hyperpolarization: Some K+ channels remain open, causing a slight dip below resting potential before returning to baseline.
Conducting a Nerve Signal
Action potentials propagate along axons by depolarizing adjacent regions. In unmyelinated axons, this is continuous conduction; in myelinated axons, action potentials jump between nodes of Ranvier (saltatory conduction), greatly increasing speed.
Synaptic Transmission
Neurons communicate at synapses, which can be electrical (via gap junctions) or chemical (via neurotransmitters). Chemical synapses are most common and allow for complex signaling.
Nerve Repair
CNS: Nerves do not regenerate due to inhibitory factors and scar formation.
PNS: Schwann cells and macrophages facilitate axon regeneration and remyelination.
Sensory Receptors
Types of Sensory Receptors by Stimulus
Mechanoreceptors: Respond to mechanical forces (touch, pressure, vibration, stretch).
Thermoreceptors: Respond to temperature changes.
Photoreceptors: Respond to light (e.g., in the retina).
Chemoreceptors: Respond to chemical stimuli (e.g., taste, smell, blood chemistry).
Nociceptors: Respond to damaging stimuli that result in pain.
