 Back
BackSkeleton of the Thorax and Structure of the Human Breast
Study Guide - Smart Notes

Skeleton of the Thorax
Structure of the Thoracic Skeleton
The thoracic skeleton forms the protective cage of the thorax and is essential for respiration and protection of vital organs. It is an osteocartilaginous structure, meaning it is composed of both bone and cartilage.
Bony components: 12 thoracic vertebrae, 12 pairs of ribs, and the sternum.
Cartilaginous components: 10 pairs of costal cartilages (hyaline cartilage); the last two pairs of ribs do not have costal cartilages.
Function: The cartilage joints provide flexibility and slight movement during breathing.
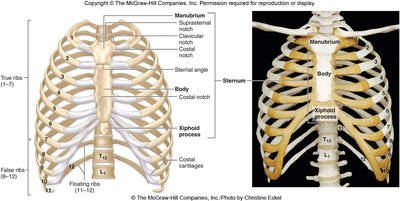
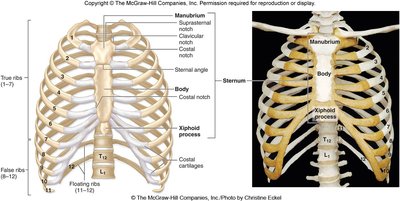
Structure of the Sternum
The sternum is a flat bone located in the center of the chest, divided into three main sections:
Manubrium: Superior section; articulates with clavicles and first costal cartilages. Features the sternal (jugular) notch.
Body: Middle and largest section; articulates with costal cartilages of ribs 2-7 and the xiphoid process.
Xiphoid process: Inferior section; serves as a clinical marker for the superior surface of the liver, apex of the heart, and central tendon of the diaphragm.
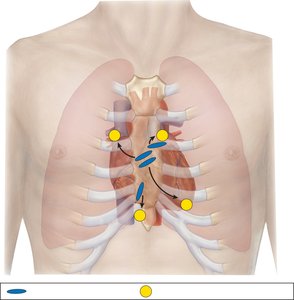
Clinical Importance of Locating the 2nd Rib
The sternal angle (junction of manubrium and body) is a key landmark for identifying the second rib. This is important for auscultation of heart valves, as the second intercostal space is the location for listening to major heart valves.
Stethoscope placement: Used to listen to heart valve sounds at specific intercostal spaces.
Types of Ribs
Ribs are classified based on their attachments and structure:
True ribs (Vertebrosternal, 1–7): Attach directly to the sternum via their own costal cartilage.
False ribs (8–12): Do not attach directly to the sternum. Ribs 8–10 (vertebrochondral) attach to rib 7's cartilage; ribs 11–12 (floating) have no anterior attachment.
Floating ribs (11–12): End in the muscles of the lower lumbar area and do not attach to the sternum.
Structure of a Typical Rib
Ribs 3–9 are considered typical ribs and share common features:
Head: Articulates with thoracic vertebral bodies; has flattened articular facets.
Neck: Connects the head to the tubercle.
Tubercle: (Ribs 1–10) Articulates with the transverse process of the vertebra.
Angle: The point where the rib curves.
Costal groove: Houses the intercostal vein, artery, and nerve (VAN).
Posterior and Anterior Rib Joints
Ribs form joints at both their posterior and anterior ends:
Posterior joints: Heads of ribs articulate with vertebral bodies (demifacets for ribs 2–9; single facet for ribs 1, 10–12). Tubercle articulates with transverse costal facet (ribs 1–10).
Anterior joints: Costal cartilages of ribs 1–10 attach to the sternum (directly or indirectly).
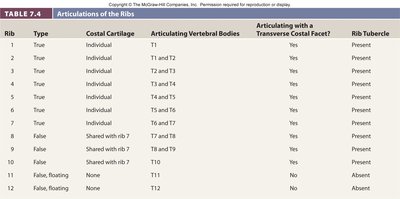
Summary Table: Articulations of the Ribs
The following table summarizes the articulations and features of each rib:
Rib | Type | Costal Cartilage | Articulating Vertebral Bodies | Articulating with a Transverse Costal Facet? | Rib Tubercle |
|---|---|---|---|---|---|
1 | True | Individual | T1 | Yes | Present |
2 | True | Individual | T1 and T2 | Yes | Present |
3 | True | Individual | T2 and T3 | Yes | Present |
4 | True | Individual | T3 and T4 | Yes | Present |
5 | True | Individual | T4 and T5 | Yes | Present |
6 | True | Individual | T5 and T6 | Yes | Present |
7 | True | Individual | T6 and T7 | Yes | Present |
8 | False | Shared with rib 7 | T7 and T8 | Yes | Present |
9 | False | Shared with rib 7 | T8 and T9 | Yes | Present |
10 | False | Shared with rib 7 | T10 | Yes | Present |
11 | False, floating | None | T11 | No | Absent |
12 | False, floating | None | T12 | No | Absent |
Atypical Ribs
Some ribs differ from the typical structure:
Rib 1: Shortest and most curved; has grooves for subclavian vessels; articulates only with T1 vertebra.
Ribs 11 and 12: Single facet on head, no tubercle, and articulate only with their respective vertebral bodies.
Structure of the Human Breast
Gross Anatomy and Functional Structure
The human breast is a modified apocrine sweat gland found in both genders but functional only in females. It is located on the fascia covering the pectoralis major muscle.
Lobules: Milk-secreting cells are organized into small oval lobules, drained by lactiferous ducts into lactiferous sinuses beneath the nipple.
Support: Surrounded by adipose tissue and supported by suspensory ligaments.
Areola: Pigmented area around the nipple containing glands for lubrication during lactation.
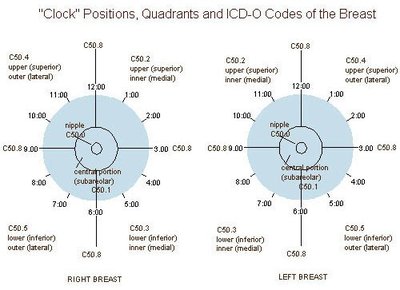
Quadrants: The breast is divided into upper/lower and inner/outer quadrants for clinical reference.
Axillary tail: Extension of breast tissue into the axilla (armpit).
Blood and Lymphatic Supply
The breast receives blood from the internal thoracic and lateral thoracic arteries. Lymphatic drainage is primarily to axillary lymph nodes, with some drainage to parasternal nodes. This is clinically important for the spread of breast cancer (metastasis).
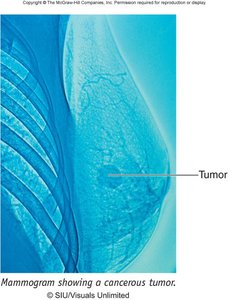
Breast Cancer
Breast cancer usually begins in the cells of the lobules or lactiferous sinuses. It can present as a painless or painful lump, swelling, skin changes, or nipple discharge. Lymphatic spread is a key concern, with the sentinel lymph node being the first node in the drainage pathway.
Metastasis: Cancer cells can spread to axillary and parasternal lymph nodes, and potentially to the opposite breast.
Sentinel lymph node biopsy: Used to assess the spread of cancer and guide surgical treatment.
Lymphedema: Swelling of the limb can occur if lymph nodes are removed during surgery.
Example: A patient with a lump in the upper outer quadrant of the right breast may have cancer that spreads first to the axillary lymph nodes.
Additional info: Regular self-examination and screening mammography are important for early detection of breast cancer in both men and women.
