 Back
BackStudy Guide: Blood Vessels and Hemodynamics in the Cardiovascular System
Study Guide - Smart Notes

Blood Vessels: Structure and Function
Types of Blood Vessels
The cardiovascular system consists of three main types of blood vessels, each with distinct roles in circulation:
Arteries: Carry blood away from the heart. In the pulmonary circuit, arteries transport deoxygenated blood; in the systemic circuit, they carry oxygenated blood.
Capillaries: Serve as the exchange system, allowing rapid transfer of gases, nutrients, and wastes between blood and tissues.
Veins: Return blood to the heart. In the pulmonary circuit, veins carry oxygenated blood; in the systemic circuit, they carry deoxygenated blood. Veins are more numerous and have larger lumens, functioning as blood reservoirs.
Blood Vessel Structure: Tunics and Lumen
All blood vessels are composed of three layers (tunics) surrounding a central lumen:
Tunica intima: Innermost layer, made of simple squamous endothelium. Produces substances like nitric oxide and collagen, and provides a smooth surface for blood flow.
Tunica media: Middle layer, composed of circular smooth muscle and elastic fibers. Regulates vessel diameter via vasoconstriction and vasodilation, controlled by sympathetic nerves.
Tunica externa (adventitia): Outermost layer, made of dense irregular connective tissue. Provides structural support and prevents overstretching.
Differences Between Arteries and Veins
Arteries have thicker tunica media and more elastic fibers, allowing them to withstand higher pressures.
Veins have thinner walls, larger lumens, and often contain valves to prevent backflow, especially in the legs.
Veins serve as blood reservoirs, holding up to 70% of the body's blood volume.
Summary Table: Veins vs. Arteries
Feature | Arteries | Veins |
|---|---|---|
Wall Thickness | Thick | Thin |
Lumen Size | Small | Large |
Valves | Absent | Present (especially in legs) |
Blood Pressure | High | Low |
Blood Reservoir | No | Yes |
Anastomosis
Anastomosis refers to a connection between two normally separate structures, such as blood vessels, allowing alternate routes for blood flow.
Hemodynamics: Blood Flow and Pressure
Blood Pressure and Flow
Blood pressure is the force exerted by blood on vessel walls, measured in mm Hg. It is highest near the heart and decreases as blood moves through the vasculature. Blood flow is driven by a pressure gradient and is directly proportional to the gradient and inversely proportional to resistance.
Blood flow (F): , where is the pressure gradient and is resistance.
Cardiac output: The volume of blood pumped per minute, typically 5–6 liters/min.
Factors Affecting Blood Pressure
Peripheral resistance: Influenced by vessel radius, blood viscosity, and vessel length. Resistance increases as radius decreases, viscosity increases, or length increases.
Blood volume: More blood volume increases pressure; vessel compliance buffers changes.
Cardiac output: Increased output raises blood pressure; decreased output lowers it.
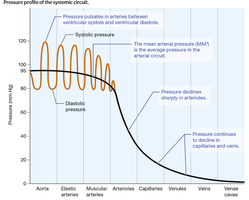
Pressure Profile in the Systemic Circuit
Pressure is highest in the aorta and elastic arteries, declines in muscular arteries and arterioles, and continues to decrease in capillaries and veins.
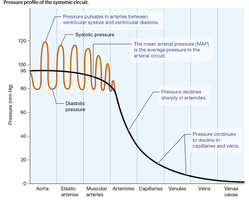
Systolic and Diastolic Pressure
Systolic pressure: Pressure during ventricular contraction (110–120 mm Hg).
Diastolic pressure: Pressure during ventricular relaxation (70–80 mm Hg).
Pulse pressure: Difference between systolic and diastolic pressures (~40 mm Hg).
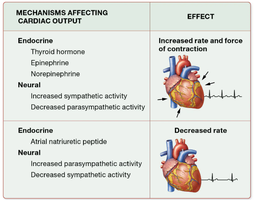
Mechanisms Affecting Cardiac Output and Blood Volume
Mechanism | Effect |
|---|---|
Endocrine (Thyroid hormone, Epinephrine, Norepinephrine) | Increased rate and force of contraction |
Neural (Increased sympathetic activity) | Increased rate and force of contraction |
Endocrine (Atrial natriuretic peptide) | Decreased rate |
Neural (Increased parasympathetic activity) | Decreased rate |
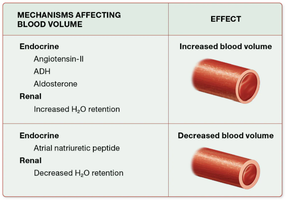
Mechanism | Effect |
|---|---|
Endocrine (Angiotensin-II, ADH, Aldosterone) | Increased blood volume |
Renal (Increased H2O retention) | Increased blood volume |
Endocrine (Atrial natriuretic peptide) | Decreased blood volume |
Renal (Decreased H2O retention) | Decreased blood volume |
Capillaries and Tissue Perfusion
Capillary Structure and Function
Capillaries are thin-walled vessels composed of endothelium and basal lamina, facilitating efficient exchange of substances.
Capillary Exchange Mechanisms
Diffusion and osmosis: Through gaps and fenestrations in the endothelium.
Transcytosis: Larger substances cross endothelial cells via endocytosis and exocytosis.
Blood Flow Through Capillary Beds
Microcirculation includes true capillaries (exchange sites) and central vessels (metarterioles). Precapillary sphincters regulate blood flow into capillaries.
Local Regulation of Tissue Perfusion
Tissue perfusion is regulated by arterial blood pressure and local autoregulatory mechanisms:
Myogenic mechanism: Arteriolar smooth muscle contracts in response to increased pressure, adjusting resistance and perfusion.
Metabolic controls: Local chemical changes (O2, CO2, H+) cause vasodilation or constriction to match tissue activity.
Tissue Perfusion in Special Circuits
Heart: Perfusion peaks during diastole; regulated by metabolic controls.
Brain: Highly sensitive to ischemia; autoregulation maintains steady perfusion.
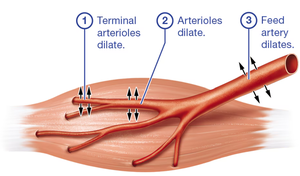
Skeletal Muscle: Exercise increases perfusion via dilation of feed arteries and arterioles.
Skin: Blood flow regulated by temperature and sympathetic nervous system.
Capillary Pressures and Water Movement
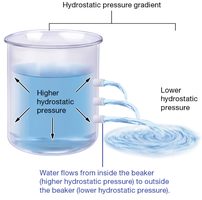
Hydrostatic Pressure
Hydrostatic pressure is the force exerted by blood on capillary walls, driving water out of capillaries via filtration.
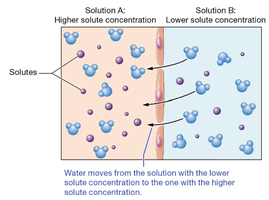
Osmotic Pressure
Osmotic pressure is the force needed to prevent water from entering a solution via osmosis. In capillaries, it is mainly due to plasma proteins (e.g., albumin) that cannot cross the endothelium.
Edema
Edema is excess water in interstitial fluid, caused by increased hydrostatic pressure, decreased colloid osmotic pressure, or both. Common causes include hypertension, liver failure, and protein malnutrition.
Clinical Concepts
Hypertension and Hypotension
Hypertension: Chronic high blood pressure, risk factor for heart, vascular, and kidney diseases.
Hypotension: Abnormally low blood pressure (systolic < 90 mm Hg, diastolic < 60 mm Hg). Causes include blood loss, decreased cardiac output, and excessive vasodilation.
Atherosclerosis
Atherosclerosis is the buildup of plaques in arterial walls, leading to narrowing and reduced flexibility. Risk factors include high blood pressure, cholesterol, smoking, and diabetes. Treatment focuses on lifestyle changes and managing risk factors.
Varicose Veins
Varicose veins are dilated, bulging veins, often in the lower limbs, caused by decreased venous return and weakened vessel walls.
Vasovagal Syncope
Vasovagal syncope is fainting due to sudden autonomic imbalance, resulting in decreased cardiac output and peripheral resistance, and a dramatic drop in blood pressure.
Key Equations and Concepts
Blood flow:
Cross-sectional area:
Mean arterial pressure (MAP):
Review Questions
The tunica intima is composed primarily of endothelium.
Arteries deal with higher blood pressure than veins.
Atherosclerosis narrows arteries and reduces flexibility.
If resistance increases, blood flow decreases.
Decreased vessel radius increases blood pressure.
Severe blood loss decreases blood pressure.
Sympathetic nervous system is activated after a sudden drop in blood pressure.
Atrial Natriuretic Peptide (ANP) decreases blood pressure.
Beta blockers decrease cardiac output, treating hypertension.
Sinusoidal capillaries are the leakiest type.
Coronary perfusion peaks during diastole.
Stratified epithelium in capillaries would reduce exchange efficiency (True).
Hydrostatic pressure gradient drives water out of capillaries.
Net absorption of water occurs at the venular end of capillaries (negative net filtration pressure).
Hypotension causes a weaker capillary hydrostatic pressure gradient.
