 Back
BackStudy Guide: Immune Response, Blood, and Cardiovascular Physiology
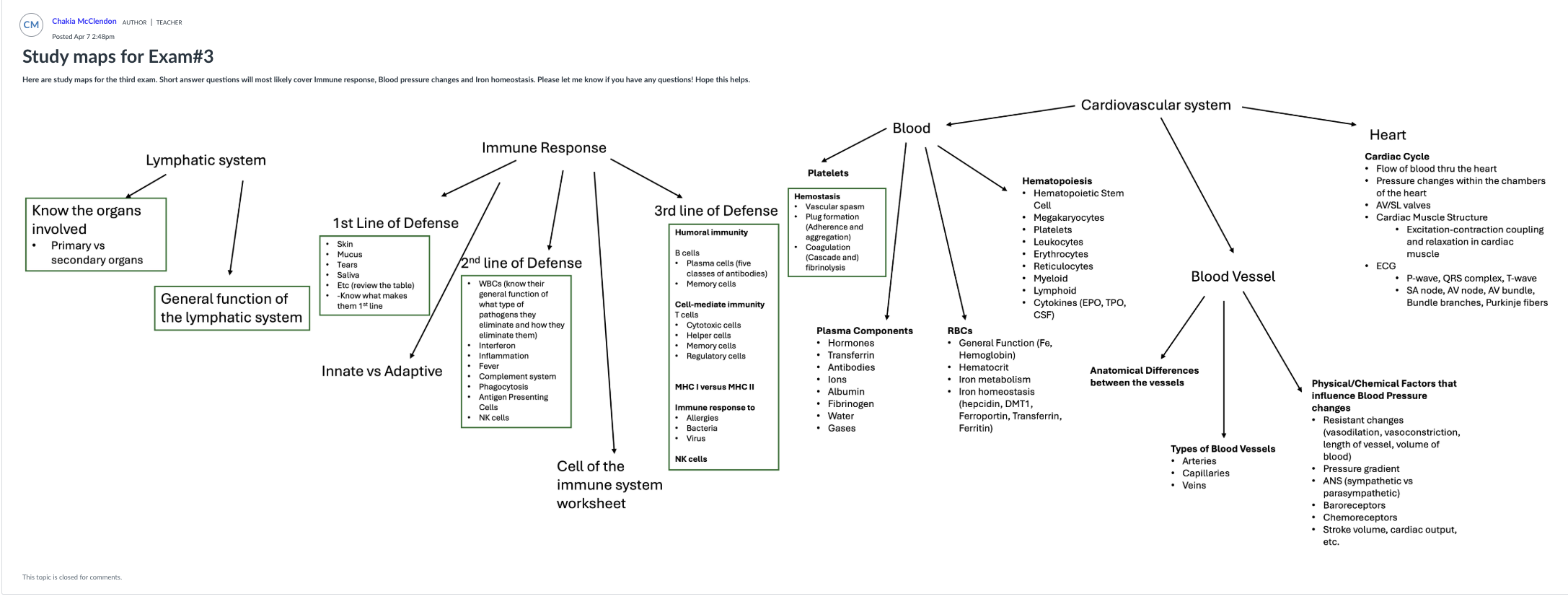
Study Guide - Smart Notes

Lymphatic System
General Function of the Lymphatic System
The lymphatic system is a network of tissues and organs that help rid the body of toxins, waste, and other unwanted materials. Its primary function is to transport lymph, a fluid containing infection-fighting white blood cells, throughout the body.
Immune Surveillance: Monitors and responds to pathogens.
Fluid Balance: Returns excess interstitial fluid to the bloodstream.
Absorption: Absorbs fats and fat-soluble vitamins from the digestive system.
Organs Involved: Primary vs Secondary
The lymphatic system consists of primary and secondary organs, each with distinct roles in immunity.
Primary Organs: Bone marrow and thymus (sites of lymphocyte production and maturation).
Secondary Organs: Lymph nodes, spleen, tonsils, and MALT (sites where immune responses are initiated).
Immune Response
1st Line of Defense
The first line of defense consists of physical and chemical barriers that prevent pathogens from entering the body.
Skin: Acts as a physical barrier.
Mucus: Traps pathogens.
Tears and Saliva: Contain enzymes (e.g., lysozyme) that destroy bacteria.
Other Barriers: Include stomach acid and cilia in the respiratory tract.
Innate vs Adaptive Immunity
Immunity is classified into innate (nonspecific) and adaptive (specific) responses.
Innate Immunity: Rapid, nonspecific response (includes 1st and 2nd lines of defense).
Adaptive Immunity: Slower, specific response involving lymphocytes (3rd line of defense).
2nd Line of Defense
The second line of defense involves cellular and chemical responses to pathogens that breach the initial barriers.
White Blood Cells (WBCs): Phagocytes (neutrophils, macrophages) engulf pathogens.
Interferons: Proteins that inhibit viral replication.
Inflammation: Localized response to injury or infection.
Fever: Elevated body temperature to inhibit pathogen growth.
Complement System: Proteins that enhance phagocytosis and lyse pathogens.
Antigen Presenting Cells: Present antigens to lymphocytes to initiate adaptive immunity.
Natural Killer (NK) Cells: Destroy infected or abnormal cells.
3rd Line of Defense
The third line of defense is the adaptive immune response, which targets specific pathogens.
Humoral Immunity: B cells produce antibodies (five classes: IgG, IgA, IgM, IgE, IgD) and memory cells.
Cell-mediated Immunity: T cells (cytotoxic, helper, memory, regulatory) target infected cells.
MHC I vs MHC II: Major histocompatibility complex molecules present antigens to T cells.
Immune Response to: Allergies, bacteria, viruses.
Example: During a viral infection, cytotoxic T cells recognize and destroy infected cells, while B cells produce antibodies to neutralize the virus.
Blood
Platelets and Hemostasis
Platelets are cell fragments essential for blood clotting (hemostasis).
Vascular Spasm: Constriction of blood vessels to reduce blood loss.
Plug Formation: Platelets adhere and aggregate at the injury site.
Coagulation: Cascade of reactions leading to fibrin clot formation.
Fibrinolysis: Breakdown and removal of the clot.
Plasma Components
Blood plasma is the liquid component of blood, containing various substances.
Hormones: Regulatory molecules.
Transferrin: Iron transport protein.
Antibodies: Immune proteins.
Ions: Electrolytes (Na+, K+, Ca2+).
Albumin: Maintains osmotic pressure.
Fibrinogen: Precursor to fibrin in clotting.
Water: Solvent.
Gases: O2, CO2.
Hematopoiesis
Hematopoiesis is the process of blood cell formation from hematopoietic stem cells.
Stem Cells: Differentiate into all blood cell types.
Megakaryocytes: Produce platelets.
Leukocytes: White blood cells.
Erythrocytes: Red blood cells.
Reticulocytes: Immature RBCs.
Myeloid/Lymphoid Lineages: Two main differentiation pathways.
Cytokines: EPO (erythropoietin), TPO (thrombopoietin), CSF (colony-stimulating factors).
RBCs: Function and Iron Homeostasis
Red blood cells (RBCs) transport oxygen and maintain iron balance.
Hemoglobin: Oxygen-carrying protein.
Hematocrit: Percentage of RBCs in blood.
Iron Metabolism: Involves hepcidin, DMT1, ferroportin, transferrin, ferritin.
Equation: Hemoglobin binding:
Example: Iron deficiency leads to decreased hemoglobin and anemia.
Cardiovascular System
Heart: Cardiac Cycle and ECG
The heart pumps blood through a cycle of contraction and relaxation, regulated by electrical signals.
Flow of Blood: Blood moves through chambers and valves (AV and SL valves).
Pressure Changes: Occur during systole and diastole.
Cardiac Muscle Structure: Excitation-contraction coupling enables contraction.
ECG: Electrocardiogram records electrical activity (P-wave, QRS complex, T-wave).
Conduction System: SA node, AV node, AV bundle, bundle branches, Purkinje fibers.
Equation: Cardiac output:
Example: Increased heart rate or stroke volume raises cardiac output.
Blood Vessels: Types and Anatomical Differences
Blood vessels transport blood throughout the body and differ in structure and function.
Arteries: Carry blood away from the heart; thick, muscular walls.
Capillaries: Site of exchange between blood and tissues; thin walls.
Veins: Carry blood toward the heart; thinner walls, valves present.
Physical/Chemical Factors Influencing Blood Pressure
Blood pressure is regulated by multiple factors affecting vessel resistance and cardiac function.
Resistance Changes: Vasodilation, vasoconstriction, vessel length, blood volume.
Pressure Gradient: Drives blood flow.
Autonomic Nervous System (ANS): Sympathetic increases, parasympathetic decreases BP.
Baroreceptors: Detect changes in blood pressure.
Chemoreceptors: Monitor blood chemistry.
Stroke Volume and Cardiac Output: Affect overall blood pressure.
Equation: Blood pressure: (Total Peripheral Resistance)
Example: Vasoconstriction increases resistance and blood pressure.
Table: Comparison of Blood Vessel Types
Type | Main Function | Wall Structure | Direction of Flow |
|---|---|---|---|
Arteries | Carry blood away from heart | Thick, muscular | Away from heart |
Capillaries | Exchange of gases/nutrients | Thin, single layer | Between arteries and veins |
Veins | Carry blood to heart | Thin, less muscular, valves | Toward heart |
