 Back
BackStudy Guide: Skeletal, Muscular, and Nervous Systems (ANP College Level)
Study Guide - Smart Notes

Chapter 6: The Skeletal System
Functions of the Skeletal System
The skeletal system provides essential support and protection for the body, stores minerals, produces blood cells, and enables movement.
Support: Structural framework for attachment of soft tissues and organs.
Mineral Storage: Calcium and phosphate are stored in the bone matrix.
Blood Cell Production: Red bone marrow is the site of hematopoiesis (formation of blood cells).
Protection: Bones such as the skull, thorax, and pelvis protect internal organs.
Movement: Bones act as levers for muscles to generate body motion.
Structure of a Typical Long Bone
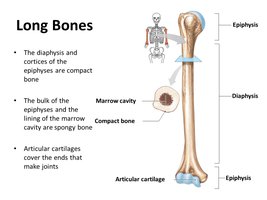
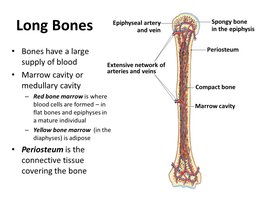
Long bones have distinct regions and internal structures that contribute to their function and growth.
Diaphysis: The central shaft, surrounds the marrow (medullary) cavity filled with bone marrow.
Epiphyses: Expanded ends, covered with articular cartilage for joint formation.
Periosteum: Outer connective tissue covering the bone.
Endosteum: Lines the inner surfaces and spongy bone of the marrow cavity.
Compact Bone: Dense bone forming the diaphysis and cortices of epiphyses.
Spongy Bone: Found in the bulk of epiphyses and lining the marrow cavity.
Bone Cell Types and Calcium Homeostasis
Bone tissue contains three main cell types, each with distinct functions, and calcium levels are tightly regulated by hormones.
Osteocytes: Mature bone cells in lacunae; maintain bone matrix.
Osteoblasts: Bone-forming cells; produce matrix and become osteocytes when surrounded.
Osteoclasts: Large, multinucleated cells; break down bone matrix (osteolysis).
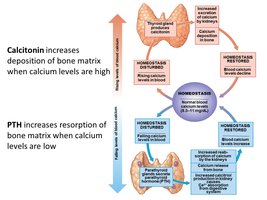
Calcium Homeostasis:
Calcitonin: Promotes calcium deposition in bone when blood calcium is high.
Parathyroid Hormone (PTH): Promotes calcium resorption from bone when blood calcium is low.
Bone Growth and Development
Bones grow and develop through two main processes: intramembranous and endochondral ossification.
Intramembranous Ossification: Formation of flat bones from fibrous connective tissue (e.g., skull, jaw, collarbone).
Endochondral Ossification: Formation of most bones from hyaline cartilage; primary ossification in diaphysis, secondary in epiphyses.
Epiphyseal Cartilage: Growth plate between diaphysis and epiphysis; responsible for lengthening.
Appositional Growth: Increase in bone diameter by adding lamellae under periosteum.
Clinical Disorders of Bone Growth
Abnormal bone growth and development can lead to various clinical disorders.
Osteoporosis: Reduced bone mass and increased fracture risk.
Gigantism: Excess growth hormone before puberty; abnormal height.
Acromegaly: Excess growth hormone after puberty; thickened bones and soft tissues.
Pituitary Growth Failure: Reduced cartilage activity; short bones.
Marfan’s Syndrome: Excessive cartilage at growth plates; tall, slender limbs, cardiovascular issues.
Achondroplasia: Slow growth and early fusion of epiphyseal cartilage; short limbs, normal trunk.
Fibrodysplasia Ossificans Progressiva: Ossification of connective tissue in muscles, tendons, ligaments.
Chapter 7: The Muscular System
Organization of Skeletal Muscle Tissue
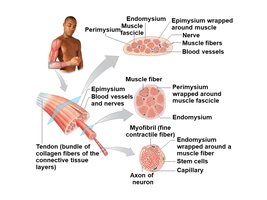
Skeletal muscle is organized into bundles wrapped in connective tissue layers, which provide structure and transmit force.
Endomysium: Surrounds individual muscle fibers.
Perimysium: Bundles fibers into fascicles.
Epimysium: Encloses the entire muscle organ.
Tendon: Cord-like bundle attaching muscle to bone.
Aponeurosis: Sheet-like connective tissue attachment.
Types of Muscle Tissue
Muscle tissue is classified as skeletal, cardiac, or smooth, each with unique structural and functional characteristics.
Cardiac Muscle: Short, branched, striated cells; involuntary; found in heart; intercalated discs for communication.
Smooth Muscle: Short, spindle-shaped, unstriated cells; involuntary; found in hollow organs; controls movement through tubes.
Skeletal Muscle: Long, cylindrical, striated, multinucleate fibers; voluntary; attached to skeleton; responsible for movement, posture, and heat production.
Structure of Skeletal Muscle Fiber and Neuromuscular Junction
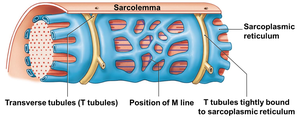
Skeletal muscle fibers contain specialized structures for contraction, and are controlled by the nervous system via the neuromuscular junction.
Sarcolemma: Plasma membrane of muscle fiber.
Sarcoplasm: Cytoplasm of muscle fiber.
Sarcoplasmic Reticulum (SR): Calcium reservoir wrapped around myofibrils.
Myofibril: Contractile organelle made of sarcomeres.
Transverse Tubules (T-tubules): Connect sarcolemma with SR.
Thin Filament: Actin, tropomyosin, troponin.
Thick Filament: Myosin; forms cross-bridges with actin.
Neuromuscular Junction: Connection between neuron and muscle fiber; site of neurotransmitter release.
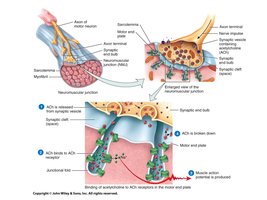
Excitation-Contraction Coupling
Muscle contraction is initiated by nerve signals and involves a series of events leading to filament sliding and tension generation.
Neurotransmitter (ACh) Release: From axon terminal to sarcolemma.
ACh Binding: Opens sodium channels, depolarizes sarcolemma.
Action Potential: Spreads across sarcolemma and down T-tubules.
Calcium Release: From SR into myofibrils.
Troponin Activation: Calcium binds, tropomyosin moves, myosin binds actin.
Cross-Bridge Cycling: Myosin heads pull actin, detach, and reset (requires ATP).
Sliding Filament Theory: Sarcomeres shorten, muscle contracts.
Relaxation: Occurs via gravity, opposing muscle, or elastic recoil.
Motor Unit Recruitment and Tension Generation
Muscle tension is regulated by the recruitment of motor units, which are groups of fibers controlled by a single neuron.
Motor Unit: One neuron and all fibers it controls.
Recruitment: Activation of additional motor units increases tension.
Muscle Tone: Resting tension from partial activation of motor units.
Muscle Hypertrophy, Atrophy, and Rigor Mortis
Muscle size and function can change due to activity, inactivity, or post-mortem processes.
Hypertrophy: Increase in muscle size due to activity.
Atrophy: Decrease in muscle size due to inactivity.
Rigor Mortis: Stiffening of muscles after death due to lack of ATP.
Chapter 8: The Nervous System
Functional and Structural Divisions
The nervous system is divided into central and peripheral components, each with specialized functions.
Central Nervous System (CNS): Brain and spinal cord; integration and processing.
Peripheral Nervous System (PNS): Cranial and spinal nerves; sensory and motor divisions.
Somatic Nervous System (SNS): Controls skeletal muscle; mostly voluntary.
Autonomic Nervous System (ANS): Controls smooth/cardiac muscle, glands; involuntary.
Sympathetic: Fight or flight.
Parasympathetic: Rest and digest.
Neuron Structure and Classification
Neurons are specialized cells for impulse transmission, with distinct structural types and synaptic connections.
Cell Body: Contains nucleus and organelles.
Dendrites: Branched receiving ends.
Axon: Long process for impulse transmission.
Axon Hillock: Transition from cell body to axon.
Axon Terminal: Contains neurotransmitter vesicles.
Types: Unipolar, bipolar, multipolar neurons.
Synapse: Junction between neurons; presynaptic and postsynaptic cells.
Neuroglia and Their Functions
Neuroglia are support cells in the CNS and PNS, with roles in myelination, protection, and maintenance.
Myelin: Lipid-rich sheath speeding impulse conduction.
Nodes of Ranvier: Gaps between myelin sheaths.
CNS Neuroglia: Astrocytes, microglia, ependymal cells, oligodendrocytes.
PNS Neuroglia: Satellite cells (in ganglia), Schwann cells (myelination).
Functional Anatomy of Brain and Spinal Cord
The brain and spinal cord have distinct regions and structures for processing, coordination, and control.
Cerebrum: Conscious thought, memory, sensory processing, muscle control.
Cerebellum: Motor coordination, balance.
Diencephalon: Thalamus (sensory relay), hypothalamus (emotions, autonomic, hormones).
Brain Stem: Midbrain (reflexes), pons (relay), medulla oblongata (vital functions).
Spinal Cord: Cervical/lumbar enlargements, conus medullaris, cauda equina.
Reflex Arc Components
Reflexes are rapid, involuntary responses to stimuli, preserving homeostasis.
Components: Receptor, sensory neuron, information processing, motor neuron, effector.
Monosynaptic Reflex: Simple, fast (e.g., stretch reflex).
Polysynaptic Reflex: Complex, slower (e.g., withdrawal reflex).
Autonomic Nervous System: Sympathetic vs. Parasympathetic
The ANS controls involuntary functions, with two divisions that have distinct effects and anatomical features.
Sympathetic: Thoracolumbar origin, short preganglionic/long postganglionic fibers, widespread response, fight or flight.
Parasympathetic: Craniosacral origin, long preganglionic/short postganglionic fibers, localized response, rest and digest.
Chapter 9: The General and Special Senses
General and Special Senses
Sensory information is detected by specialized receptors, enabling perception of internal and external stimuli.
General Senses: Temperature, pain, touch, pressure, vibration, proprioception.
Receptors:
Nociceptors: Pain.
Thermoreceptors: Temperature.
Mechanoreceptors: Stretch, compression, twisting.
Proprioceptors: Position/movement.
Baroreceptors: Pressure.
Tactile Receptors: Touch, vibration.
Chemoreceptors: Chemical concentrations.
Functional Anatomy of Special Sense Organs
Special senses are detected by complex organs in the head, each with unique structures and pathways.
Olfaction: Smell; receptor cells in nasal cavity, olfactory nerve (CN I).
Gustation: Taste; taste buds in papillae, nerves CN VII, IX, X.
Vision: Eye structures, photoreceptors (rods/cones), optic nerve (CN II).
Hearing: Ear structures, cochlea, hair cells.
Equilibrium: Vestibule, semicircular canals for balance.
Chapter 10: The Endocrine System
Hormones and Endocrine Functions
The endocrine system regulates body functions through hormones produced by various glands.
Posterior Pituitary: ADH (water retention), oxytocin (contractions, bonding).
Anterior Pituitary: TSH, ACTH, MSH, GH, PRL, FSH, LH.
Thyroid: T3, T4 (metabolic rate, heart rate, sensitivity).
Parathyroid: Calcitonin (deposition), PTH (resorption).
Pancreatic Islets: Glucagon (raises glucose), insulin (lowers glucose).
Pineal: Melatonin (circadian rhythm).
Gonads: Testosterone, estrogen, progesterone (secondary sex characteristics).
Adrenal: Cortex (steroids), medulla (epinephrine, norepinephrine).
Mechanism of Hormone Action
Hormones act on target cells via distinct mechanisms depending on their chemical nature.
Nonsteroid Hormones: Bind to cell surface receptors, activate second messengers (e.g., cAMP), fast but short-lived.
Steroid Hormones: Pass through membranes, bind to nuclear receptors, activate transcription, slow but long-lasting.
Endocrine Disorders
Endocrine disorders result from abnormal hormone production, either excess (hypersecretion) or deficiency (hyposecretion).
Primary Hyposecretion: Problem at hormone-producing gland.
Secondary Hyposecretion: Problem with stimulating hormone production.
Nervous vs. Endocrine System Control
Both systems use chemical messengers to maintain homeostasis, but differ in connectivity and speed.
Nervous System: Fast, point-to-point, short-lived effects.
Endocrine System: Slow, widespread, long-term effects.
Key Equation: Calcium Homeostasis
Blood calcium levels are regulated by negative feedback:
Additional info: This study guide covers the main topics from chapters 6-10 of an ANP college course, with expanded academic context and relevant images for anatomical and physiological understanding.
