 Back
BackStudy Guide: The Male Reproductive System
Study Guide - Smart Notes

The Male Reproductive System
Overview and Functions
The male reproductive system consists of organs responsible for the production, nourishment, and transport of gametes (sperm), as well as the secretion of hormones necessary for reproduction. Sexual maturation and gamete production are essential for propagation and offspring generation.
Production of Gametes: Testes produce sperm cells.
Hormone Secretion: Testosterone is produced to regulate male reproductive functions.
Transport and Nourishment: Sperm is transported and nourished by accessory organs and glands.
Support of Offspring: Male system contributes to fertilization; female system supports embryo development.
Homology of Male and Female Reproductive Systems
Both male and female reproductive systems develop from the same embryonic tissues, making them homologous. Early in development, the reproductive structures are indistinguishable between sexes.
Homologous Structures: Organs in both sexes share common origins and functions.
Developmental Similarity: Males and females appear similar for several weeks during embryogenesis.
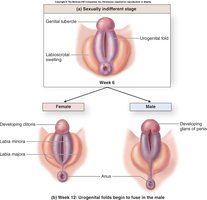
Reproductive System Homologues Table
This table compares homologous organs in male and female reproductive systems and their functions.
Female Organ | Male Organ Homologue | Common Function |
|---|---|---|
Ovary | Testis | Produce gametes and sex hormones |
Clitoris | Glans of penis | Contain autonomic nervous system axons that stimulate arousal and sexual climax feelings |
Labia majora | Scrotum | Protect and cover some reproductive structures |
Vestibular glands | Bulbourethral glands | Secrete mucus for lubrication |

Anatomy of the Male Reproductive System
Primary and Secondary Sex Organs
The male reproductive system is composed of primary sex organs (testes), secondary sex organs (ducts and glands), and external genitalia (penis and scrotum).
Testes: Primary site of sperm and testosterone production.
Spermatic Ducts: Transport sperm from testes to urethra.
Secretory Glands: Produce seminal fluid to nourish and protect sperm.
External Organs: Penis and scrotum facilitate sperm delivery and temperature regulation.
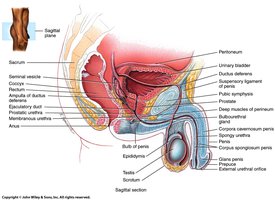
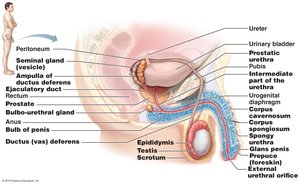
Male Perineum
The perineum is a diamond-shaped area between the thighs, divided into two triangles: the urogenital triangle (contains penis and scrotum) and the anal triangle (contains anus).
Anterior Border: Pubic symphysis
Lateral Borders: Ischial tuberosities
Posterior Border: Coccyx
The Scrotum
The scrotum is a skin-covered sac that encloses and protects the testes, maintaining optimal temperature for sperm production. The midline seam is called the raphe.
Structure: Loose skin, muscle, and connective tissue.
Function: Temperature regulation for spermatogenesis.
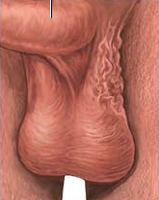
Muscles of the Scrotum
Cremaster Muscle: Skeletal muscle that contracts in cold temperatures, drawing testes closer to the body.
Dartos Muscle: Smooth muscle that wrinkles the scrotal skin, reducing heat loss.
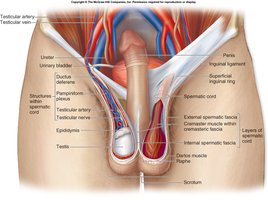
Pampiniform Plexus
The pampiniform plexus is a network of veins surrounding the testicular artery, helping to cool arterial blood before it reaches the testes.
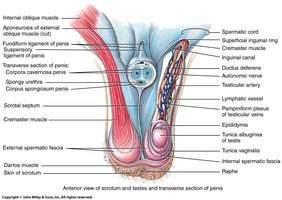
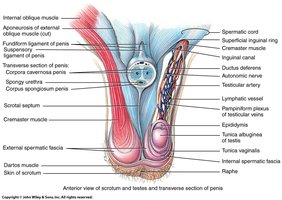
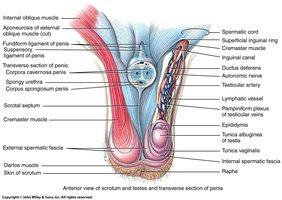
The Testes (Testicles)
The testes are paired, oval organs located in the scrotum. They descend from the abdomen during development. Failure to descend results in cryptorchidism.
Primary Functions: Sperm and hormone production.
Coverings: Tunica vaginalis and tunica albuginea.
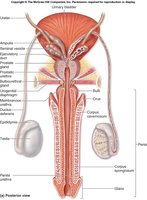
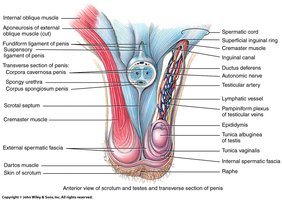
Tunica Albuginea
The tunica albuginea is a dense connective tissue layer that forms lobules within the testes, each containing seminiferous tubules.
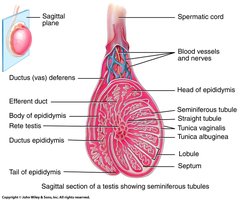
Seminiferous Tubules
Seminiferous tubules are tightly coiled structures within each lobule, serving as the site of sperm cell production. Two main cell types are present:
Sertoli Cells (Sustentacular Cells): Nourish and protect maturing sperm; form blood-testes barrier.
Interstitial (Leydig) Cells: Located between tubules; produce testosterone.
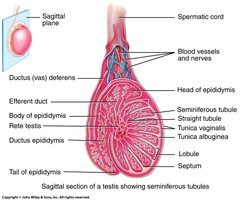
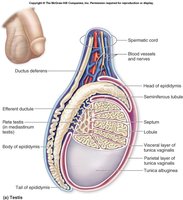
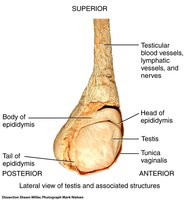
Epididymis
The epididymis is a highly coiled, comma-shaped organ attached to the posterior aspect of each testis. It is the site of sperm maturation and storage.
Receives sperm: From seminiferous tubules via efferent ducts.
Function: Sperm matures and is stored until ejaculation.
Vas (Ductus) Deferens
The vas deferens are paired ducts that store and propel sperm toward the urethra during ejaculation. They join with the seminal vesicle to form the ejaculatory duct.
Storage: Sperm can remain viable for months.
Reabsorption: Non-ejaculated sperm is reabsorbed.
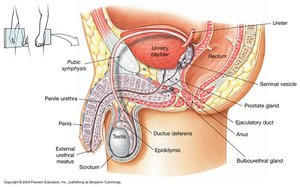
Ejaculatory Ducts and Urethra
Ejaculatory ducts carry sperm from the vas deferens through the prostate gland to the urethra. The urethra serves as a passageway for both semen and urine, divided into prostatic, membranous, and penile portions.
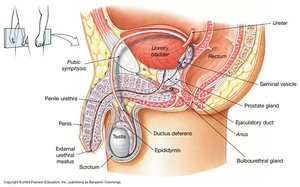
Accessory Glands
Accessory glands produce seminal fluid to nourish and protect sperm, neutralizing the acidic environment of the female reproductive tract.
Seminal Vesicles: Secrete viscous fluid (60% of semen volume), rich in fructose and alkaline substances.
Prostate Gland: Secretes citric acid, seminalplasmin (antibiotic), and prostate-specific antigen (liquefies semen).
Bulbourethral (Cowper's) Glands: Secrete clear mucus for lubrication and neutralization of acidic male urethra.
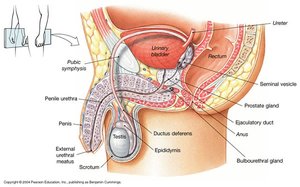
Semen
Semen is a fluid mixture of sperm cells and secretions from the seminal vesicles, prostate gland, and bulbourethral glands. Each ejaculation releases 2-6 mL of semen, containing 50-100 million sperm cells.
Infertility: Less than 20 million sperm per emission is a contributing factor.
Penis
The penis consists of three portions: root (internal), shaft, and glans penis (tip). It functions to deposit sperm into the female vagina and excrete urine.
Root: Contains the bulb.
Shaft: Contains two corpus cavernosa and one corpus spongiosum layer.
Glans Penis: Covered by foreskin (prepuce).
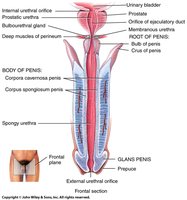
Travel of Sperm: SEVEN UP Mnemonic
Sperm travels through the following structures:
Seminiferous Tubules
Epididymis
Vas Deferens
Ejaculatory Duct
Nothing
Urethra
Penis
Physiology of the Male Reproductive System
Male Erection and Orgasm
Erection is the engorgement of blood in erectile tissues, controlled by the parasympathetic nervous system. Orgasm and ejaculation are controlled by the sympathetic nervous system, resulting in the emission of seminal fluid.
Erection: Blood fills arteries, veins are compressed.
Orgasm: Ejaculation occurs, bladder sphincter contracts to prevent urine mixing.
Hormonal Control
Hormones regulate the male reproductive system:
Luteinizing Hormone (LH): Stimulates testosterone production.
Follicle-Stimulating Hormone (FSH): Stimulates sperm production in seminiferous tubules.
Secondary Male Sex Characteristics
Testosterone is responsible for secondary sex characteristics:
Growth of body hair
Prominence of thyroid cartilage (Adam's apple)
Deepening of voice
Increase in muscle mass and skeleton
Oiling of skin
Spermatogenesis
Spermatogenesis is the process of sperm cell production, occurring in the seminiferous tubules via meiosis. The chromosome number is reduced from 46 to 23, producing four haploid sperm cells from one diploid cell.
Meiosis I: Primary spermatocyte divides into two secondary spermatocytes.
Meiosis II: Each secondary spermatocyte divides into two spermatids.
Physical Changes: Spermatids mature into spermatozoa in the epididymis.
Key Equation:
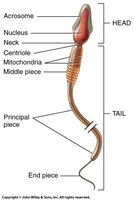
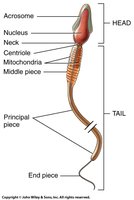
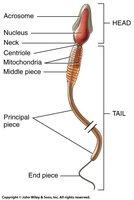
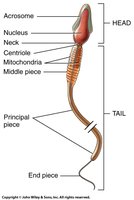
Spermatozoa Structure
Mature sperm cells (spermatozoa) have three main parts:
Head: Contains nucleus (23 chromosomes) and acrosome (digestive enzymes).
Midpiece: Contains mitochondria for ATP production.
Tail: Flagellum for motility.
Male Reproductive Conditions & Diseases
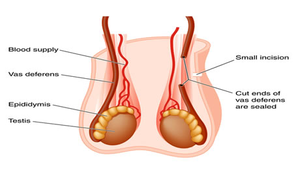
Vasectomy
Vasectomy is a permanent male sterilization procedure where the vas deferens is cut and sealed, preventing sperm from exiting the body.
Benign Prostatic Hyperplasia (BPH)
BPH is the enlargement of the prostate gland, which can impede the urethra and ejaculatory ducts, affecting urination and ejaculation.
Penile Cancer
Penile cancer is rare, most commonly affecting uncircumcised individuals. The 5-year survival rate is 85%.
Testicular Cancer
Testicular cancer most commonly affects males aged 15-35, with cryptorchidism as a risk factor. The 5-year survival rate is 95.3%.
Prostate Cancer
Prostate cancer is common, with a 5-year survival rate of 99%. The average age of diagnosis is 66 years.
