 Back
BackStudy Notes: The Reproductive System (Human Anatomy & Physiology, Ch. 27)
Study Guide - Smart Notes

The Reproductive System: Overview
Introduction
The reproductive system is unique among organ systems in that it does not function continuously and becomes active only at puberty. Its primary roles are the production of gametes, the facilitation of fertilization, and the support of fetal development. Both male and female systems share fundamental tasks but differ significantly in structure and function.
Common Features of Male and Female Reproductive Systems
Gonads and Accessory Organs
Gonads are the primary sex organs: testes in males and ovaries in females.
They produce two main products:
Gametes: sperm (male), ova (female), formed by meiosis.
Sex hormones: testosterone (male), estrogens and progesterone (female).
Accessory reproductive organs include ducts, glands, and external genitalia.
Male and female reproductive structures are homologous (e.g., testes and ovaries, penis and clitoris).
Regulation of Reproductive Hormones
The Hypothalamic-Pituitary-Gonadal (HPG) Axis
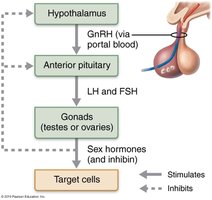
The HPG axis regulates the production of gametes and sex hormones through a sequence of hormonal signals involving the hypothalamus, anterior pituitary, and gonads.
GnRH (Gonadotropin-releasing hormone) is released from the hypothalamus and stimulates the anterior pituitary.
The anterior pituitary releases FSH (Follicle-stimulating hormone) and LH (Luteinizing hormone).
FSH and LH act on the gonads to stimulate gamete production and hormone secretion.
Sex hormones exert negative feedback on the hypothalamus and pituitary to regulate the cycle.
Inhibin is released from the gonads and specifically inhibits FSH release.
Meiosis: Formation of Gametes
Overview and Terminology
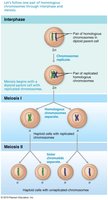
Meiosis is a specialized form of cell division that reduces the chromosome number by half, producing haploid gametes. This process is essential for sexual reproduction and genetic diversity.
Diploid (2n): Normal chromosome number in body cells (46 in humans).
Haploid (n): Chromosome number in gametes (23 in humans).
Homologous chromosomes: One from each parent, carry genes for the same traits.
Sister chromatids: Identical copies of a chromosome joined at the centromere.
Crossing over: Exchange of genetic material between nonsister chromatids, increasing genetic variability.
Phases of Meiosis
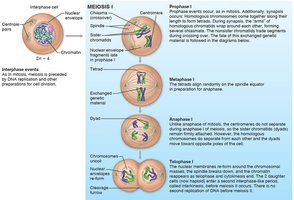
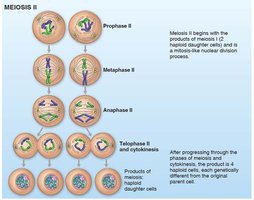
Meiosis consists of two divisions: Meiosis I (reduction division) and Meiosis II (equational division).
Each division includes prophase, metaphase, anaphase, and telophase.
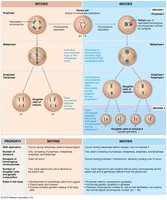
Comparison: Mitosis vs. Meiosis
Mitosis: Produces two identical diploid cells for growth and repair.
Meiosis: Produces four genetically unique haploid cells for reproduction.
Genetic diversity arises from random alignment and crossing over in meiosis.
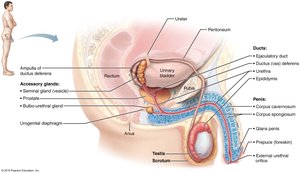
Anatomy of the Male Reproductive System
Testes and Scrotum
Testes: Sperm-producing organs housed in the scrotum.
Scrotum: Sac that maintains testes at a temperature lower than body core, essential for sperm production.
Muscles (dartos and cremaster) regulate testicular temperature by moving the testes closer or further from the body.
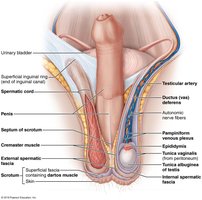
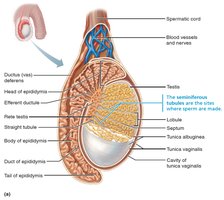
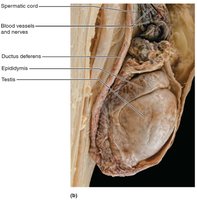
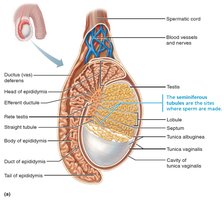
Testicular Structure
Each testis is divided into lobules containing seminiferous tubules, the site of sperm production.
Sperm travels from seminiferous tubules to the epididymis via a series of ducts.
Blood supply is provided by testicular arteries and veins, with the pampiniform plexus helping to cool arterial blood.
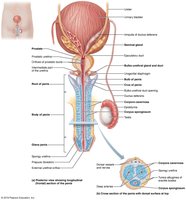
Male Duct System
Epididymis: Site of sperm maturation and storage.
Ductus deferens (vas deferens): Transports sperm during ejaculation; vasectomy involves cutting this duct.
Ejaculatory duct: Formed by the union of the ductus deferens and seminal vesicle duct.
Urethra: Conveys both urine and semen (at different times).
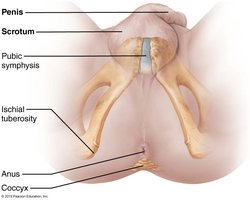
Penis and Male Perineum
Penis: Male copulatory organ, composed of erectile tissues (corpora cavernosa and corpus spongiosum).
Perineum: Diamond-shaped region containing the root of the penis and anus.
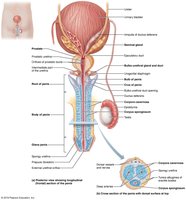
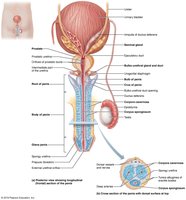
Accessory Glands
Seminal glands: Produce alkaline seminal fluid, contributing 70% of semen volume.
Prostate: Secretes a milky, slightly acidic fluid that activates sperm.
Bulbo-urethral glands: Produce mucus for lubrication and neutralization of acidic urine.
Male Sexual Response and Spermatogenesis
Erection and Ejaculation
Erection: Parasympathetic stimulation leads to vasodilation and engorgement of erectile tissues with blood.
Ejaculation: Sympathetic reflex propels semen through the duct system, followed by a refractory period.
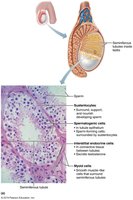
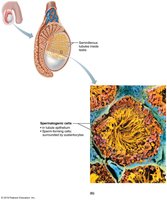
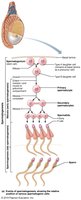
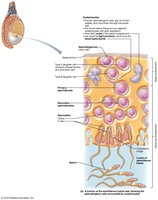
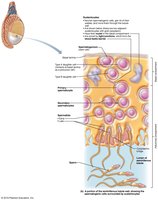
Spermatogenesis
Spermatogenesis is the process of sperm formation in the seminiferous tubules, beginning at puberty and continuing throughout life.
Three main steps:
Mitosis of spermatogonia (stem cells) produces primary spermatocytes.
Meiosis: Primary spermatocytes undergo meiosis I and II to form spermatids.
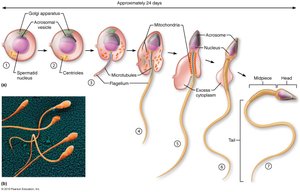
Spermiogenesis: Spermatids mature into spermatozoa (sperm cells).
Sustentocytes (Sertoli cells) support and nourish developing sperm, form the blood-testis barrier, and secrete regulatory factors.
Hormonal Regulation of Male Reproduction
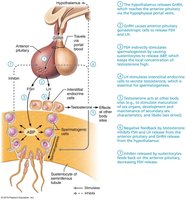
HPG Axis in Males
GnRH from the hypothalamus stimulates FSH and LH release from the anterior pituitary.
FSH stimulates sustentocytes to produce ABP, maintaining high testosterone levels for spermatogenesis.
LH stimulates interstitial endocrine cells (Leydig cells) to produce testosterone.
Testosterone and inhibin provide negative feedback to regulate hormone levels.
Anatomy of the Female Reproductive System
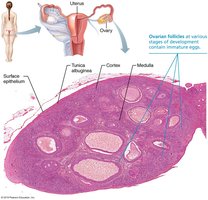
Ovaries and Duct System
Ovaries: Produce ova and secrete estrogens and progesterone.
Held in place by ligaments (ovarian, suspensory, mesovarium).
Ovarian follicles contain oocytes at various stages of development.
Each month, a mature follicle releases an oocyte (ovulation).
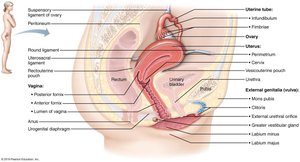
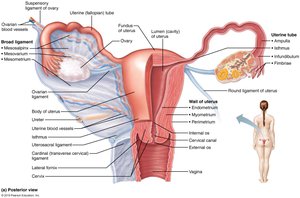
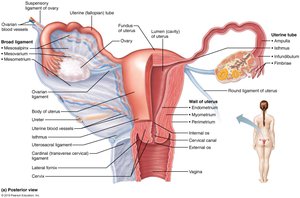
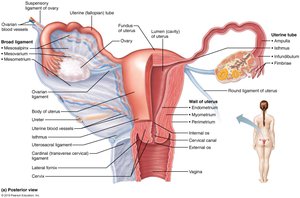
Uterine Tubes, Uterus, and Vagina
Uterine tubes (fallopian tubes): Site of fertilization; transport oocyte to uterus.
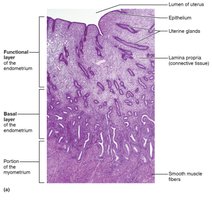
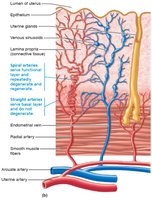
Uterus: Receives, retains, and nourishes fertilized ovum; composed of three layers (perimetrium, myometrium, endometrium).
Vagina: Birth canal and organ of copulation.
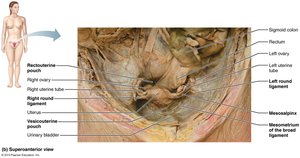
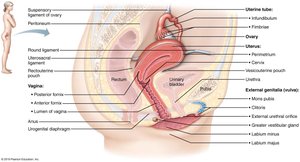
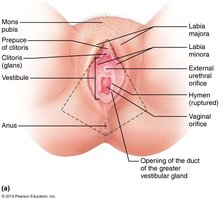
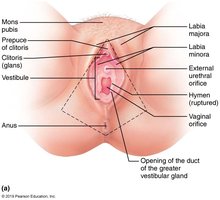
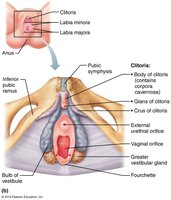
External Genitalia and Mammary Glands
Vulva: Includes mons pubis, labia majora, labia minora, clitoris, and vestibular glands.
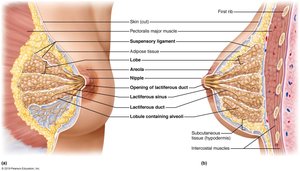
Mammary glands: Modified sweat glands for milk production.
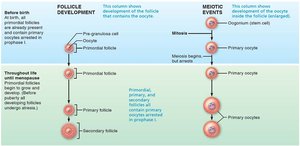
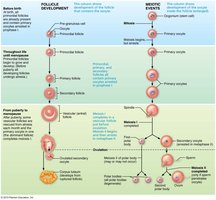
Oogenesis and Follicle Development
Oogenesis
Oogenesis is the production of female gametes, beginning in the fetal period.
Primary oocytes are arrested in prophase I until puberty.
Each month, a few primary oocytes resume meiosis; usually only one completes meiosis I to become a secondary oocyte.
Meiosis II is completed only if fertilization occurs.
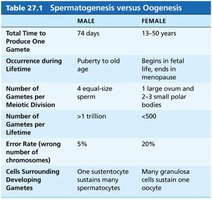
Comparison: Spermatogenesis vs. Oogenesis
Feature | Male (Spermatogenesis) | Female (Oogenesis) |
|---|---|---|
Total Time to Produce One Gamete | 74 days | 13–50 years |
Occurrence during Lifetime | Puberty to old age | Begins in fetal life, ends in menopause |
Number of Gametes per Meiotic Division | 4 equal-size sperm | 1 large ovum and 2–3 small polar bodies |
Number of Gametes per Lifetime | >1 trillion | <500 |
Error Rate | 5% | 20% |
Cells Surrounding Developing Gametes | One sustentocyte sustains many spermatocytes | Many granulosa cells sustain one oocyte |

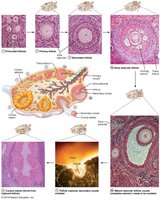
Follicle Development
Follicles mature through primordial, primary, secondary, and vesicular (antral) stages.
Ovulation releases the secondary oocyte; the ruptured follicle becomes the corpus luteum.
Ovarian and Uterine (Menstrual) Cycles
Ovarian Cycle
Follicular phase (days 1–14): Follicle growth and maturation.
Ovulation (day 14): Release of secondary oocyte.
Luteal phase (days 14–28): Corpus luteum activity.
Hormonal Regulation
GnRH stimulates FSH and LH release.
FSH and LH promote follicle growth and estrogen production.
Estrogen exerts negative and then positive feedback, triggering the LH surge and ovulation.
Progesterone from the corpus luteum maintains the uterine lining.
Uterine (Menstrual) Cycle
Menstrual phase (days 1–5): Shedding of the functional layer of the endometrium.
Proliferative phase (days 6–14): Regeneration of the endometrium under estrogen influence.
Secretory phase (days 15–28): Preparation for implantation under progesterone influence; if no fertilization, the cycle restarts.
Summary Table: Hormonal Effects
Hormone | Main Effects |
|---|---|
Estrogen | Promotes oogenesis, follicle growth, secondary sex characteristics, maintains cholesterol and bone health |
Progesterone | Regulates uterine cycle, prepares breasts for lactation, maintains pregnancy |
Testosterone | Promotes spermatogenesis, secondary sex characteristics, libido |
Developmental Aspects of the Reproductive System
Genetic Determination of Sex
Sex is determined by the combination of sex chromosomes (XX = female, XY = male).
The SRY gene on the Y chromosome initiates male development.
Sexual Differentiation and Development
Embryos initially have both male (Wolffian) and female (Müllerian) ducts.
Testosterone presence leads to male development; absence leads to female development.
External genitalia differentiate by week 8 of development.
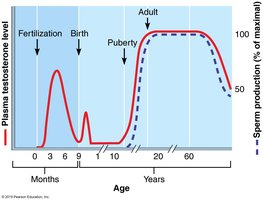
Puberty and Menopause
Puberty: Period of reproductive organ maturation and onset of gamete production.
Menopause: Cessation of menstruation and reproductive capability in females; associated with decreased estrogen levels and systemic effects.
Key Clinical Correlations
Testicular cancer: Most common in young men; high cure rate with early detection.
Benign prostatic hyperplasia: Age-related prostate enlargement causing urinary issues.
Infertility: Can result from environmental toxins, hormonal imbalances, or anatomical defects.
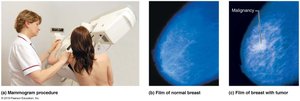
Breast cancer: Most common malignancy in women; early detection is critical.
Sexually transmitted infections (STIs): Major cause of reproductive disorders; prevention and early treatment are essential.
