 Back
BackThe Autonomic Nervous System and Higher-Order Functions: ANP Study Notes
Study Guide - Smart Notes

Chapter 16: The Autonomic Nervous System and Higher-Order Functions
Introduction to the Autonomic Nervous System (ANS) and Higher-Order Functions
The autonomic nervous system (ANS), also known as the visceral motor system, operates without conscious instruction and regulates the function of visceral effectors such as smooth muscle, glands, cardiac muscle, and adipocytes. Higher-order functions include consciousness, learning, and intelligence, which require complex neural processing.
Organization of the Autonomic Nervous System
Somatic vs. Autonomic Nervous System
Somatic Nervous System (SNS): Controls voluntary movements of skeletal muscles.
Autonomic Nervous System (ANS): Controls involuntary actions of visceral effectors.
Integration Center: The hypothalamus contains integrative centers for the ANS, analogous to upper motor neurons in the SNS.
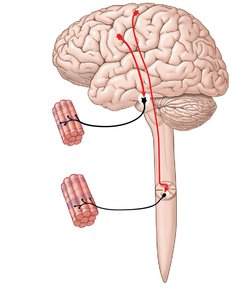
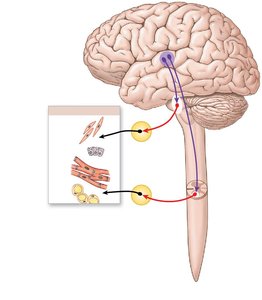
Visceral Motor Neurons and Pathways
Preganglionic Neurons: Located in the brainstem and spinal cord; their axons (preganglionic fibers) synapse on ganglionic (postganglionic) neurons in autonomic ganglia.
Autonomic Ganglia: Contain ganglionic neurons that innervate visceral effectors.
Postganglionic Fibers: Axons of ganglionic neurons that extend to target organs.
Divisions of the ANS
Sympathetic Division: "Fight or flight"—prepares the body for emergencies by increasing alertness, metabolic rate, and muscular abilities.
Parasympathetic Division: "Rest and digest"—conserves energy and maintains resting metabolic rate.
These divisions often have opposing effects but may also work independently or together in complex processes.
The Sympathetic Division
Organization and Pathways
The sympathetic division (thoracolumbar division) has short preganglionic fibers originating from the thoracic and lumbar segments (T1–L2) of the spinal cord, and long postganglionic fibers extending to target organs.
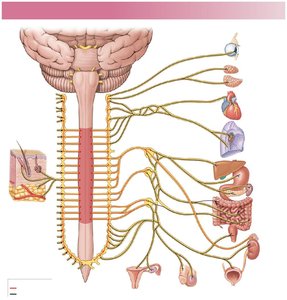
Sympathetic Chain Ganglia: Located on either side of the vertebral column; control effectors in the body wall, thoracic cavity, head, neck, and limbs.
Collateral Ganglia: Anterior to vertebral bodies; innervate abdominopelvic tissues and viscera.
Adrenal Medullae: Modified sympathetic ganglia in the adrenal glands; release epinephrine and norepinephrine into the bloodstream as hormones.
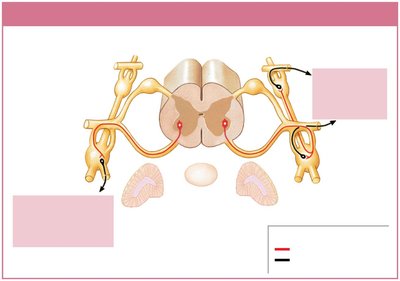
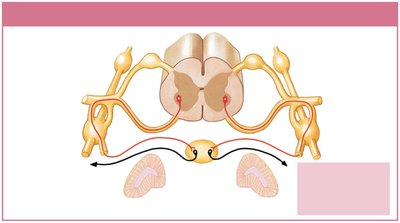
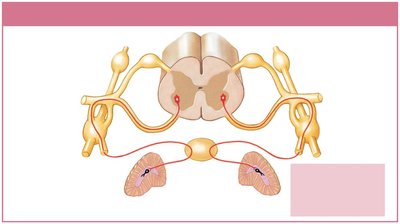
Sympathetic Effects and Neurotransmitters
Preganglionic Neurons: Release acetylcholine (ACh) at synapses with ganglionic neurons (always excitatory).
Postganglionic Neurons: Most release norepinephrine (NE, adrenergic); some release ACh (cholinergic) or nitric oxide (NO, nitroxidergic).
Adrenergic Receptors: Alpha (α) and beta (β) receptors mediate effects of NE and epinephrine.
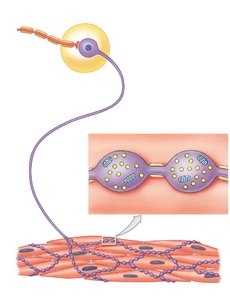
Types of Adrenergic Receptors
Alpha-1 (α1): Excitatory, found in smooth muscle cells.
Alpha-2 (α2): Inhibitory, found on preganglionic sympathetic neurons.
Beta-1 (β1): Increases metabolic activity.
Beta-2 (β2): Relaxes smooth muscle in respiratory tract.
Beta-3 (β3): Stimulates lipolysis in adipocytes.
The Parasympathetic Division
Organization and Pathways
The parasympathetic division (craniosacral division) has long preganglionic fibers originating from the brainstem and sacral spinal cord (S2–S4), and short postganglionic fibers located in or near target organs.
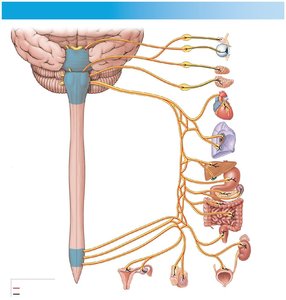
Terminal Ganglia: Located near target organs.
Intramural Ganglia: Embedded within the tissues of target organs.
Cranial Nerves Involved: III (oculomotor), VII (facial), IX (glossopharyngeal), X (vagus).
Vagus Nerve: Provides 75% of parasympathetic outflow to thoracic and abdominopelvic organs.
Sacral Output: Forms pelvic nerves to innervate lower abdominal and pelvic organs.
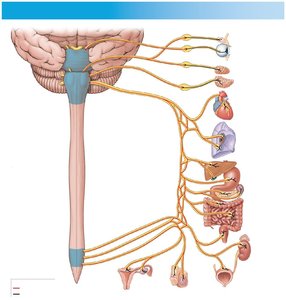
Parasympathetic Effects and Neurotransmitters
All parasympathetic neurons release acetylcholine (ACh).
Nicotinic Receptors: On ganglion cells; always excitatory.
Muscarinic Receptors: On target cells; effects can be excitatory or inhibitory, longer lasting than nicotinic.
Effects are localized and short-lived due to rapid breakdown of ACh by acetylcholinesterase (AChE).
Comparison of Sympathetic and Parasympathetic Divisions
The sympathetic division has widespread effects, extensive divergence, and uses both ACh and NE as neurotransmitters. The parasympathetic division has more specific effects, less divergence, and uses only ACh.
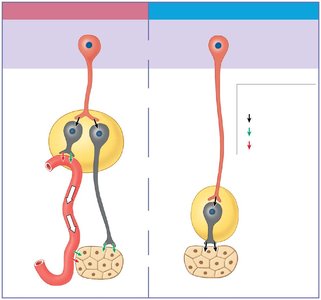
Dual Innervation and Autonomic Tone
Dual Innervation
Most vital organs receive input from both ANS divisions, often with opposing effects.
Autonomic plexuses are networks of sympathetic and parasympathetic fibers that innervate organs.
Examples: Cardiac, pulmonary, esophageal, celiac, inferior mesenteric, and hypogastric plexuses.
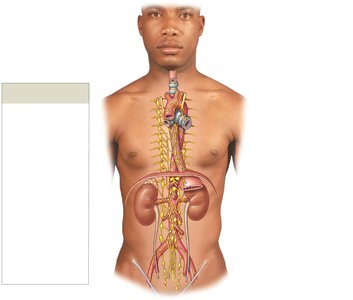
Autonomic Tone
Autonomic motor neurons maintain a resting level of activity, allowing for increases or decreases in activity for greater control.
Some organs (e.g., blood vessels) are innervated by only one division, with tone maintained by continuous neurotransmitter release.
Regulation of Autonomic Functions
Visceral Reflexes
Autonomic, polysynaptic reflexes that provide automatic motor responses.
Can be long reflexes (involving CNS) or short reflexes (bypassing CNS, especially in the digestive tract).
The enteric nervous system in the digestive tract can function independently of the CNS.
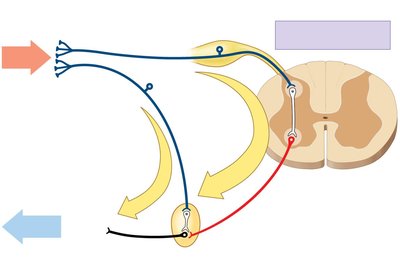
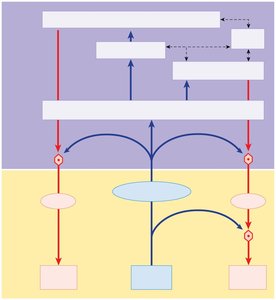
Integration of ANS and SNS
Both systems are integrated at the brainstem and are under higher center control.
Higher-Order Functions
Memory and Learning
Require the cerebral cortex and involve both conscious and unconscious processing.
Fact Memories: Specific bits of information.
Skill Memories: Learned motor behaviors, often unconscious.
Short-Term Memory: Temporary, easily lost unless consolidated into long-term memory.
Long-Term Memory: Includes secondary (fade with time) and tertiary (permanent) memories.
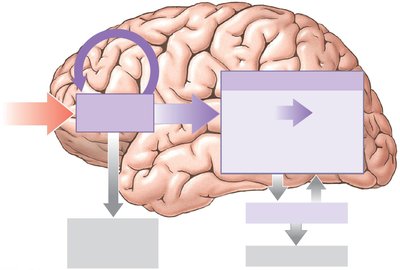
Brain Regions Involved in Memory
Amygdaloid Body and Hippocampus: Essential for memory consolidation.
Nucleus Basalis: Involved in memory storage and retrieval.
Cerebral Cortex: Stores most long-term memories.
Cellular Mechanisms of Memory
Increased neurotransmitter release, facilitation at synapses, and formation of additional synaptic connections are key mechanisms.
Memory engrams are neural circuits formed through experience and repetition.
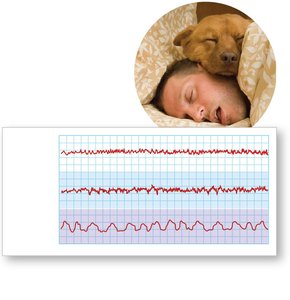
States of Consciousness and Sleep
Consciousness is graded by CNS activity; deep sleep (NREM) and REM sleep alternate during the sleep cycle.
REM sleep is associated with dreaming and increased brain activity.
The reticular activating system (RAS) in the brainstem regulates arousal and sleep-wake cycles.
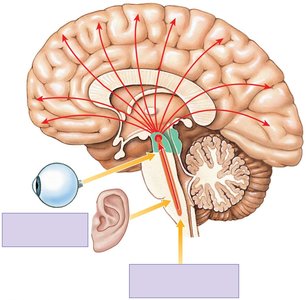
Neurotransmitters and Brain Function
Serotonin affects mood and sensory interpretation; dopamine is involved in motor control and reward pathways.
Imbalances can lead to disorders such as Parkinson's disease, schizophrenia, and depression.
Effects of Aging on the Nervous System
Brain size and weight decrease, especially in the cerebral cortex.
Number of neurons declines, synaptic connections are lost, and neurotransmitter production decreases.
Accumulation of intracellular deposits (lipofuscin, neurofibrillary tangles) and extracellular plaques (amyloid proteins) occurs.
Functional changes include memory loss, slower reflexes, and decreased sensory acuity.
Senile dementia (e.g., Alzheimer's disease) may develop in some individuals.
Integration of the Nervous System with Other Body Systems
The nervous system interacts with all other organ systems, coordinating responses and maintaining homeostasis.
Examples: Controls muscle contraction, gland secretion, and receives sensory input from the integumentary system.
Additional info: The above notes are structured to provide a comprehensive overview of the autonomic nervous system and higher-order functions, suitable for ANP college students preparing for exams.
