 Back
BackThe Autonomic Nervous System (ANS): Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Autonomic Nervous System (ANS): Overview
Definition and General Function
The Autonomic Nervous System (ANS) is a division of the peripheral nervous system responsible for regulating involuntary physiological processes, including heart rate, blood pressure, respiration, digestion, and glandular activity. It operates largely below the level of consciousness and is also known as the involuntary nervous system or general visceral motor system.
Effectors: Smooth muscle, cardiac muscle, and glands
Function: Maintains homeostasis by adjusting bodily functions in response to internal and external stimuli
Control: Subconscious, not under voluntary control
Structural Organization of the ANS
Relationship to the Nervous System
The ANS is a component of the motor (efferent) division of the peripheral nervous system, distinct from the somatic nervous system, which controls voluntary skeletal muscle movements.
Somatic Nervous System: Controls skeletal muscles
Autonomic Nervous System: Controls smooth muscle, cardiac muscle, and glands
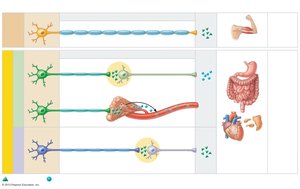
Comparison of Somatic and Autonomic Motor Pathways
Somatic Pathway: Single, heavily myelinated neuron from CNS to effector (skeletal muscle)
Autonomic Pathway: Two-neuron chain (preganglionic and postganglionic neurons) from CNS to effector (smooth/cardiac muscle, glands)
Divisions of the ANS
Sympathetic and Parasympathetic Divisions
The ANS is divided into two main branches that typically exert opposing effects on target organs:
Sympathetic Division: Prepares the body for 'fight-or-flight' responses during stress or activity
Parasympathetic Division: Promotes 'rest-and-digest' activities, conserving energy and maintaining routine functions
Most visceral organs receive dual innervation from both divisions, allowing dynamic antagonism to maintain homeostasis.
Key Anatomical Differences
Sites of Origin: Parasympathetic fibers are craniosacral (brainstem and sacral spinal cord); sympathetic fibers are thoracolumbar (thoracic and lumbar spinal cord)
Fiber Lengths: Parasympathetic has long preganglionic and short postganglionic fibers; sympathetic has short preganglionic and long postganglionic fibers
Ganglia Location: Parasympathetic ganglia are near or within effector organs; sympathetic ganglia are close to the spinal cord
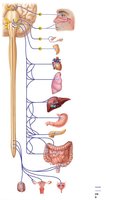
Parasympathetic Division
Organization and Pathways
The parasympathetic division is also called the craniosacral division because its fibers originate from the brainstem and sacral spinal cord. It is responsible for routine maintenance functions.
Cranial Outflow: Preganglionic fibers travel in cranial nerves III, VII, IX, and X to innervate head, thoracic, and most abdominal organs
Sacral Outflow: Preganglionic fibers from S2–S4 innervate pelvic organs
Sympathetic Division
Organization and Pathways
The sympathetic division is also called the thoracolumbar division because its fibers originate from the thoracic and lumbar regions of the spinal cord. It is more complex and innervates more organs than the parasympathetic division.
Preganglionic Neurons: Located in spinal cord segments T1–L2
Sympathetic Ganglia: Located near the spinal cord
Unique Targets: Sweat glands, arrector pili muscles, blood vessels, adrenal medulla
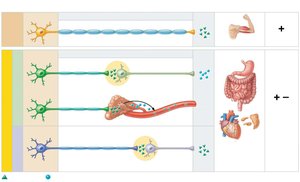
Functional Differences: Somatic vs. Autonomic
Effectors, Pathways, and Neurotransmitters
Somatic Nervous System: Releases acetylcholine (ACh) at neuromuscular junctions; always excitatory
Autonomic Nervous System: Preganglionic fibers release ACh; postganglionic fibers release ACh or norepinephrine (NE); effects can be excitatory or inhibitory depending on receptor type
Neurotransmitters and Receptors in the ANS
Major Neurotransmitters
Acetylcholine (ACh): Released by all preganglionic neurons and parasympathetic postganglionic neurons
Norepinephrine (NE): Released by most sympathetic postganglionic neurons
Cholinergic and Adrenergic Receptors
Cholinergic Receptors: Bind ACh; include nicotinic (always excitatory) and muscarinic (excitatory or inhibitory) types
Adrenergic Receptors: Bind NE or epinephrine; include alpha (α1, α2) and beta (β1, β2, β3) subtypes with varying effects
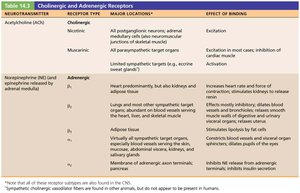
Pharmacology of the ANS
Drug Classes Affecting the ANS
Various drugs can modulate ANS activity by acting on its receptors or neurotransmitter systems. These include agonists, antagonists, and enzyme inhibitors.
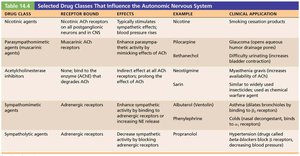
Functional Effects of the Parasympathetic and Sympathetic Divisions
Organ-Specific Effects
The two divisions of the ANS often have opposing effects on the same organs, allowing precise regulation of physiological functions.
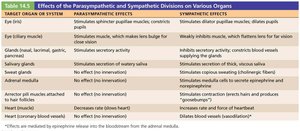
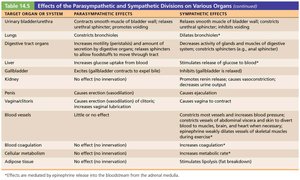
Control of ANS Function
CNS Regulation
The ANS is regulated by several CNS centers, including the hypothalamus (main integrative center), brainstem, spinal cord, and cerebral cortex (via limbic system). These centers coordinate autonomic responses to maintain homeostasis and respond to emotional stimuli.
Visceral Reflexes
Structure and Function
Visceral reflex arcs control many involuntary activities (e.g., emptying the bladder or rectum) and involve two consecutive motor neurons and visceral sensory input. They are similar to somatic reflex arcs but have key differences in their pathways and effectors.
Homeostatic Imbalances of the ANS
Clinical Conditions
Hypertension: Overactive sympathetic vasoconstriction; treated with adrenergic blockers
Raynaud’s Disease: Exaggerated vasoconstriction in extremities; treated with vasodilators
Autonomic Dysreflexia: Life-threatening overactivation of ANS in spinal cord injury patients
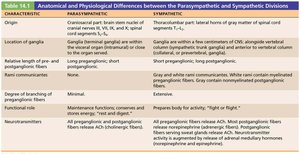
Summary Table: Anatomical and Physiological Differences
Characteristic | Parasympathetic | Sympathetic |
|---|---|---|
Origin | Craniosacral (brainstem and sacral spinal cord) | Thoracolumbar (thoracic and lumbar spinal cord) |
Location of Ganglia | Near or within effector organs | Close to spinal cord |
Fiber Lengths | Long preganglionic, short postganglionic | Short preganglionic, long postganglionic |
Degree of Branching | Minimal | Extensive |
Neurotransmitters | ACh (preganglionic and postganglionic) | ACh (preganglionic), NE (postganglionic) |
Functional Role | Maintenance, conservation, and restoration of energy | Prepares body for activity (fight-or-flight) |
