 Back
BackThe Autonomic Nervous System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Autonomic Nervous System (ANS)
Overview of the Autonomic Nervous System
The autonomic nervous system (ANS) is a division of the peripheral nervous system that innervates most effector organs and tissues, including cardiac muscle, smooth muscle, glands, and adipose tissue. Its primary function is to regulate involuntary physiological processes to maintain homeostasis. The ANS operates largely below the level of conscious awareness and is sometimes referred to as the involuntary nervous system.
Dual Innervation: Most organs receive input from both the sympathetic and parasympathetic branches, often with opposing effects.
Homeostasis: The ANS maintains internal stability by adjusting organ function in response to internal and external changes.
Sympathetic Division: Most active during stress or physical activity ("fight-or-flight" response).
Parasympathetic Division: Most active during rest ("rest and digest" state).
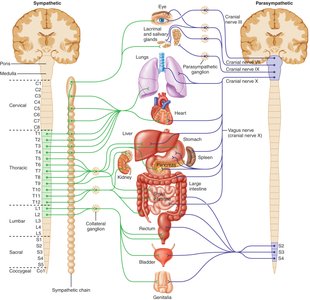
Anatomy of the Autonomic Nervous System
General Organization
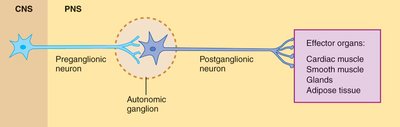
The ANS consists of two-neuron efferent pathways: a preganglionic neuron (originating in the CNS) and a postganglionic neuron (located in autonomic ganglia in the PNS). These neurons synapse in autonomic ganglia before reaching the effector organ.
Preganglionic neuron: Cell body in CNS; axon projects to autonomic ganglion.
Postganglionic neuron: Cell body in ganglion; axon projects to effector organ.
Intrinsic neurons: Located within ganglia, modulate information flow.
Sympathetic Nervous System Anatomy
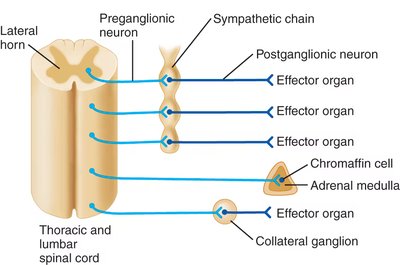
The sympathetic division is also known as the thoracolumbar division because its preganglionic neurons originate in the thoracic and lumbar spinal cord. There are three main anatomical arrangements:
Sympathetic chain (paravertebral ganglia): Preganglionic neurons synapse with postganglionic neurons in chains running parallel to the spinal cord, allowing widespread activation.
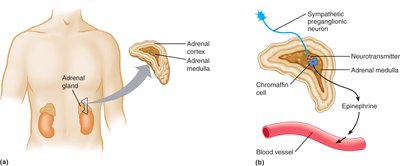
Adrenal medulla pathway: Preganglionic neurons synapse directly on chromaffin cells in the adrenal medulla, causing release of catecholamines (mainly epinephrine) into the bloodstream.
Collateral (prevertebral) ganglia: Preganglionic neurons pass through the sympathetic chain without synapsing and synapse in collateral ganglia closer to target organs, allowing more discrete control.
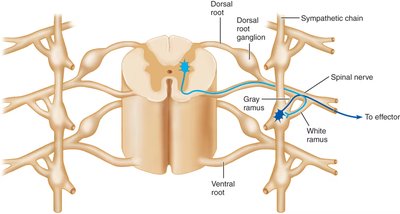
Parasympathetic Nervous System Anatomy
The parasympathetic division is also known as the craniosacral division because its preganglionic neurons originate in the brainstem and sacral spinal cord. Preganglionic fibers are long and synapse in ganglia near or within the effector organs.
Cranial nerves: Oculomotor (III), Facial (VII), Glossopharyngeal (IX), and Vagus (X) nerves carry parasympathetic fibers to various organs.
Sacral nerves: Form pelvic nerves to innervate the colon, bladder, and reproductive organs.
Mixed Composition of Autonomic Nerves
Autonomic nerves are typically mixed nerves, containing both efferent (motor) and afferent (sensory) fibers. Afferent fibers relay information from visceral receptors to the CNS, providing feedback for homeostatic regulation.
Autonomic Neurotransmitters and Receptors
Primary Neurotransmitters
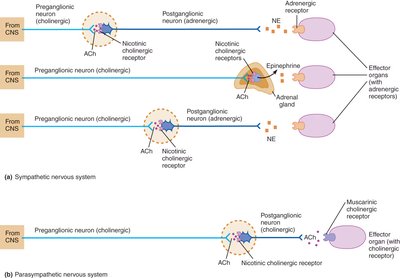
Acetylcholine (ACh): Released by all preganglionic neurons (sympathetic and parasympathetic) and parasympathetic postganglionic neurons.
Norepinephrine (NE): Released by most sympathetic postganglionic neurons.
Epinephrine: Released by the adrenal medulla into the bloodstream.
Cholinergic Receptors
Nicotinic receptors: Found on postganglionic neurons and adrenal medulla chromaffin cells; ligand-gated ion channels causing depolarization (excitation).
Muscarinic receptors: Found on effector organs of the parasympathetic system; G protein-coupled, can be excitatory or inhibitory depending on the target cell.
Adrenergic Receptors
Alpha (α) receptors: Subtypes α1 (excitatory) and α2 (inhibitory); found in smooth muscle, glands, and other tissues.
Beta (β) receptors: Subtypes β1 (excitatory), β2 (inhibitory), and β3 (excitatory); found in heart, smooth muscle, adipose tissue, etc.
Adrenergic receptors are G protein-coupled and activate or inhibit second messenger systems (e.g., cAMP, IP3).
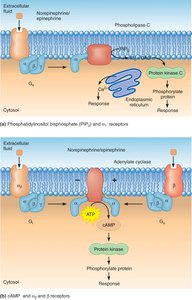
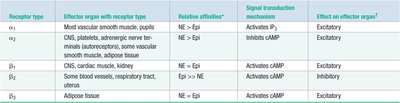
Table: Adrenergic Receptor Properties
Receptor type | Effector organ (with receptor type) | Relative affinities | Signal transduction mechanism | Effect on effector organ |
|---|---|---|---|---|
α1 | Most vascular smooth muscle, pupil | NE > Epi | Activates IP3 | Excitatory |
α2 | CNS, platelets, adrenergic nerve terminals, some vascular smooth muscle, adipose tissue | NE > Epi | Inhibits cAMP | Excitatory |
β1 | CNS, cardiac muscle, kidney | NE = Epi | Activates cAMP | Excitatory |
β2 | Some blood vessels, respiratory tract, uterus | Epi >> NE | Activates cAMP | Inhibitory |
β3 | Adipose tissue | NE = Epi | Activates cAMP | Excitatory |
Drugs Affecting the Autonomic Nervous System
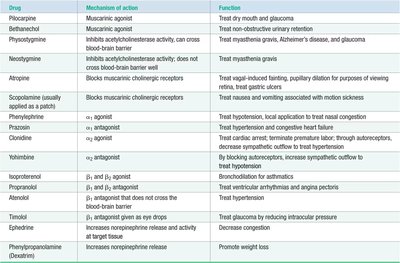
Various drugs can modulate autonomic function by acting as agonists or antagonists at cholinergic or adrenergic receptors. These drugs are used clinically to treat conditions such as asthma, hypertension, glaucoma, and overactive bladder.
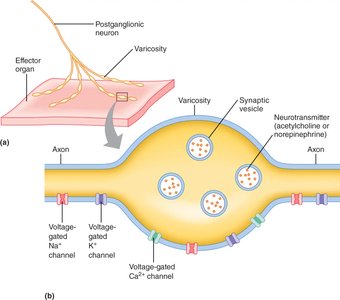
Autonomic Neuroeffector Junctions
Structure and Function
The synapse between an autonomic postganglionic neuron and its effector organ is called a neuroeffector junction. Unlike typical neuron-to-neuron synapses, neurotransmitters are released from multiple swellings called varicosities along the axon, allowing widespread and diffuse signaling to the effector tissue.
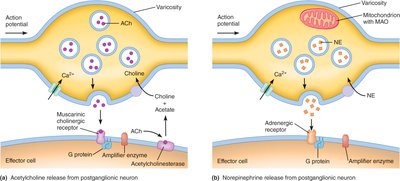
Regulation of Autonomic Function
Visceral Reflexes
Most autonomic responses are mediated by visceral reflexes, which are automatic adjustments in organ function in response to changes in the internal environment. For example, standing up quickly triggers a reflex to maintain blood pressure and prevent fainting.
CNS Control of Autonomic Function
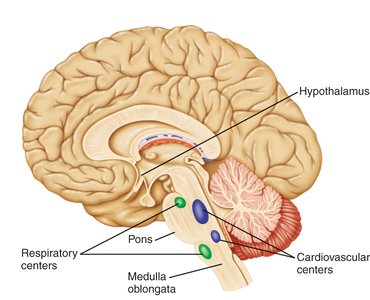
Major brain regions involved in autonomic regulation include:
Hypothalamus: Coordinates the fight-or-flight response and regulates body temperature, food intake, and water balance.
Medulla oblongata and pons: Contain cardiovascular and respiratory centers for automatic control of heart rate, blood pressure, and breathing.
Limbic system: Influences autonomic responses associated with emotions.
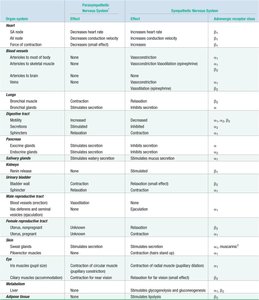
Summary Table: Effects of Autonomic Innervation
The table below summarizes the effects of parasympathetic and sympathetic innervation on various organs and tissues, including the receptor types involved.
Key Terms and Concepts
Dual innervation: Most organs receive both sympathetic and parasympathetic input.
Fight-or-flight response: Sympathetic activation prepares the body for emergency action.
Rest-and-digest state: Parasympathetic activation promotes maintenance and energy conservation.
Neurotransmitters: Acetylcholine and norepinephrine are the main chemical messengers of the ANS.
Receptors: Cholinergic (nicotinic, muscarinic) and adrenergic (α, β) receptors mediate the effects of neurotransmitters.
Neuroeffector junctions: Specialized synapses for autonomic signaling to effector organs.
Visceral reflexes: Automatic responses that regulate organ function.
