 Back
BackThe Autonomic Nervous System: Structure, Function, and Control
Study Guide - Smart Notes

The Autonomic Nervous System (ANS)
Overview and Functional Role
The autonomic nervous system (ANS) is a division of the peripheral nervous system responsible for regulating involuntary physiological processes, including heart rate, blood pressure, respiration, digestion, and glandular activity. It operates largely below the level of consciousness to maintain homeostasis and respond to stressors.
Effectors: Innervates smooth muscle, cardiac muscle, and glands.
Function: Adjusts body functions to support activity, shunting blood, adjusting heart rate, and modulating digestive processes.
Control: Operates via subconscious (involuntary) control.
Alternate Names: Involuntary nervous system, visceral motor system.
Comparison: ANS vs. Somatic Nervous System
Key Differences
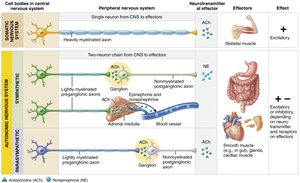
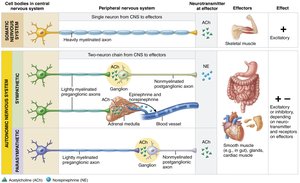
Although both the ANS and somatic nervous system have motor fibers, they differ in effectors, neural pathways, and neurotransmitter actions.
Effectors: Somatic system targets skeletal muscle; ANS targets cardiac muscle, smooth muscle, and glands.
Efferent Pathways:
Somatic: Single, thick, myelinated axon from CNS to muscle.
ANS: Two-neuron chain (preganglionic neuron in CNS, postganglionic neuron in autonomic ganglion).
Neurotransmitters:
Somatic: Acetylcholine (ACh), always excitatory.
ANS: Preganglionic fibers release ACh; postganglionic fibers release norepinephrine (NE, sympathetic) or ACh (parasympathetic), effects can be excitatory or inhibitory depending on receptor type.
Overlap of Somatic and Autonomic Function
Both systems are regulated by higher brain centers.
Most spinal and many cranial nerves contain both somatic and autonomic fibers.
Adaptations often involve both skeletal muscles and visceral organs (e.g., increased heart rate during exercise).
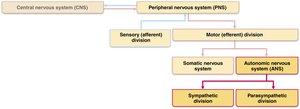
Divisions of the Autonomic Nervous System
Parasympathetic vs. Sympathetic Divisions
The ANS is divided into two main branches that typically have opposing effects on target organs.
Parasympathetic Division: Promotes maintenance functions and conserves energy ("rest-and-digest").
Sympathetic Division: Mobilizes the body during activity ("fight-or-flight").
Dual Innervation: Most visceral organs receive input from both divisions, which act antagonistically to maintain homeostasis.


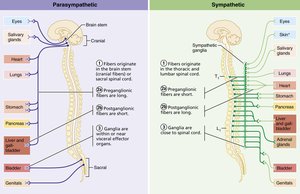
Key Anatomical Differences
Sites of Origin:
Parasympathetic: Craniosacral (brain and sacral spinal cord).
Sympathetic: Thoracolumbar (thoracic and lumbar spinal cord).
Fiber Lengths:
Parasympathetic: Long preganglionic, short postganglionic fibers.
Sympathetic: Short preganglionic, long postganglionic fibers.
Location of Ganglia:
Parasympathetic: In or near visceral effectors.
Sympathetic: Close to spinal cord.
Parasympathetic Division
Organization and Pathways
The parasympathetic division is also called the craniosacral division. Its preganglionic fibers originate from the brainstem and sacral spinal cord, and synapse in terminal ganglia near or within target organs.
Cranial Outflow: Oculomotor, facial, glossopharyngeal, and vagus nerves.
Vagus Nerve: Accounts for most parasympathetic outflow, serving thoracic and abdominal viscera.
Sacral Outflow: Serves pelvic organs and distal large intestine via pelvic splanchnic nerves.
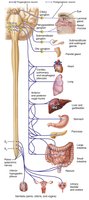
Sympathetic Division
Organization and Pathways
The sympathetic division is more complex, innervating more organs and some structures exclusively (e.g., sweat glands, arrector pili muscles, blood vessels). Preganglionic neurons originate in the thoracolumbar spinal cord and synapse in sympathetic trunk (chain) ganglia or collateral ganglia.
Sympathetic Trunks: Chains of ganglia flanking the vertebral column (23 ganglia per side: 3 cervical, 11 thoracic, 4 lumbar, 4 sacral, 1 coccygeal).
Pathways: Preganglionic fibers may synapse at the same, higher, or lower level in the trunk, or pass through to collateral ganglia (abdomen/pelvis).
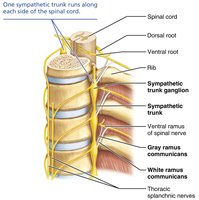
Sympathetic Pathways
To the Head: Synapse in superior cervical ganglion; innervate iris, salivary glands, and blood vessels.
To the Thorax: Synapse in middle/inferior cervical ganglia; innervate heart, lungs, and esophagus.
To the Abdomen: Synapse in celiac and superior mesenteric ganglia; innervate digestive organs.
To the Pelvis: Synapse in inferior mesenteric or pelvic ganglia; innervate pelvic organs.
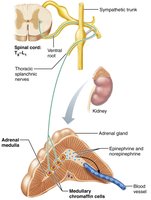
To the Adrenal Medulla: Preganglionic fibers pass directly to adrenal medulla, stimulating release of epinephrine and norepinephrine into the blood.
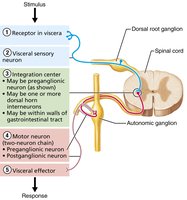
Visceral Reflex Arcs
Structure and Function
Visceral reflex arcs control involuntary responses in visceral organs. They share components with somatic reflex arcs but differ in the number of neurons and effectors involved.
Components: Receptor, sensory neuron, integration center, motor neuron (two-neuron chain), effector (smooth/cardiac muscle or gland).
Examples: Reflexes that empty the rectum and bladder; enteric nervous system reflexes in the GI tract.
Neurotransmitters and Receptors in the ANS
Major Neurotransmitters
Acetylcholine (ACh): Released by all preganglionic axons and all parasympathetic postganglionic axons.
Norepinephrine (NE): Released by most sympathetic postganglionic axons (except sweat glands, which use ACh).
Cholinergic Receptors
Nicotinic Receptors: Found on all postganglionic neurons, adrenal medulla cells, and skeletal muscle cells. Always excitatory (depolarization).
Muscarinic Receptors: Found on all effector cells stimulated by postganglionic cholinergic fibers. Can be excitatory or inhibitory depending on the target organ.
Adrenergic Receptors
Alpha (α) Receptors: Subdivided into α1 and α2; effects depend on location and subclass.
Beta (β) Receptors: Subdivided into β1, β2, and β3; effects depend on location and subclass.
Example: NE binding to β1 receptors increases heart rate; epinephrine binding to β2 receptors causes bronchial relaxation.
Parasympathetic and Sympathetic Interactions
Antagonistic and Cooperative Effects
Antagonistic: Most organs receive dual innervation; sympathetic increases heart rate, parasympathetic decreases it.
Sympathetic Tone: Maintains blood vessel constriction and blood pressure.
Parasympathetic Tone: Dominates heart, digestive, and urinary tracts under resting conditions.
Cooperative Effects: Both divisions cooperate in reproductive functions (e.g., erection and ejaculation).
Unique Roles of the Sympathetic Division
Regulates body temperature, metabolic rate, and blood glucose.
Controls adrenal medulla, sweat glands, arrector pili muscles, kidneys, and most blood vessels exclusively.
Localized vs. Diffuse Effects
Parasympathetic: Short-lived, localized effects (ACh rapidly degraded).
Sympathetic: Long-lasting, widespread effects (NE and epinephrine persist in blood).
Central Control of the ANS
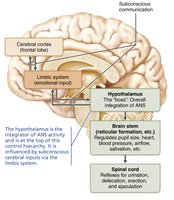
Hierarchy of Control
Hypothalamus: Main integrative center for ANS activity; directs both divisions.
Brain Stem: Regulates heart rate, blood vessel diameter, gastrointestinal activities, pupil and lens muscles.
Spinal Cord: Controls defecation, urination, erection, and ejaculation (subject to conscious override).
Cerebral Cortex: Modifies ANS activity via limbic system connections (e.g., emotional responses).
Developmental Aspects of the ANS
Development and Aging
Preganglionic neurons derive from the neural tube; postganglionic neurons, adrenal medulla, and ganglia from neural crest.
ANS efficiency declines with age, leading to issues such as constipation, dry eyes, and orthostatic hypotension.
Summary Table: Key Differences Between Parasympathetic and Sympathetic Divisions
Feature | Parasympathetic Division | Sympathetic Division |
|---|---|---|
Origin | Craniosacral (brainstem & sacral spinal cord) | Thoracolumbar (thoracic & lumbar spinal cord) |
Fiber Lengths | Long preganglionic, short postganglionic | Short preganglionic, long postganglionic |
Location of Ganglia | In/near effector organs | Close to spinal cord |
Neurotransmitter (Postganglionic) | Acetylcholine (ACh) | Norepinephrine (NE) or ACh (sweat glands) |
General Function | Rest-and-digest | Fight-or-flight |
