 Back
BackThe Autonomic Nervous System: Structure, Function, and Divisions
Study Guide - Smart Notes

The Autonomic Nervous System (ANS)
Overview and Structural Organization
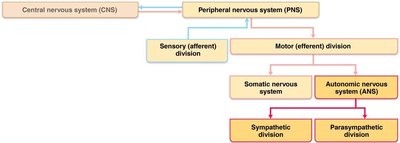
The autonomic nervous system (ANS) is a major component of the peripheral nervous system responsible for involuntary control of smooth muscle, cardiac muscle, and glands. It is also known as the involuntary nervous system or general visceral motor system. The ANS is distinct from the somatic nervous system, which controls voluntary skeletal muscle movements.
Effectors: ANS innervates smooth muscle, cardiac muscle, and glands.
Divisions: The ANS is divided into the sympathetic and parasympathetic divisions, which typically have opposing effects on target organs.
Somatic vs. Autonomic Nervous System
Comparison of Structure and Function
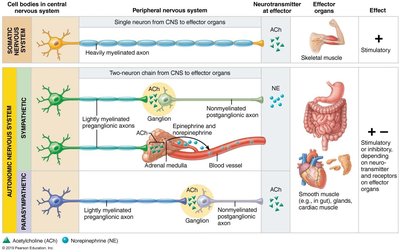
The somatic and autonomic nervous systems differ in their effectors, neural pathways, and neurotransmitters.
Somatic Nervous System: Controls skeletal muscle; consists of a single neuron from CNS to effector; always stimulatory (acetylcholine, ACh).
Autonomic Nervous System: Controls cardiac and smooth muscle, and glands; involves a two-neuron chain (preganglionic and postganglionic neurons); can be stimulatory or inhibitory depending on neurotransmitter and receptor type.
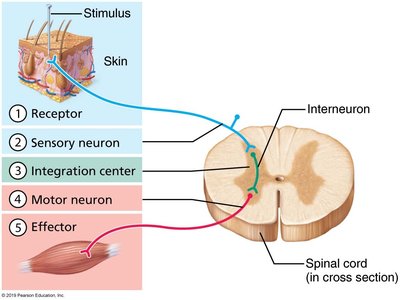
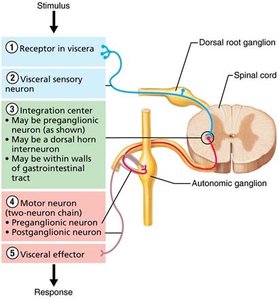
Autonomic Efferent Pathway
Preganglionic neuron: Cell body in CNS; axon extends to autonomic ganglion.
Postganglionic neuron: Cell body in ganglion; axon extends to effector organ.
Neurotransmitters and Effects
Somatic system: All motor neurons release ACh; effect is always stimulatory (muscle contraction).
Autonomic system: Preganglionic fibers release ACh; postganglionic fibers release either norepinephrine (NE) or ACh; effect can be stimulatory or inhibitory depending on receptor type.
Divisions of the Autonomic Nervous System
Parasympathetic Division
The parasympathetic division is also called the craniosacral division. It promotes maintenance functions and conserves energy, often referred to as the "rest-and-digest" system.
Origin: Brain stem and sacral regions of the spinal cord.
Preganglionic fibers: Long; extend from CNS almost to target organs.
Ganglia: Terminal ganglia are close to or within target organs.
Postganglionic fibers: Short; synapse with effectors.
Neurotransmitter: ACh, rapidly destroyed by acetylcholinesterase, leading to short-lived, localized effects.
Sympathetic Division
The sympathetic division is also called the thoracolumbar division. It mobilizes the body during activity, known as the "fight-or-flight" system.
Origin: Spinal cord segments T1–L2 (lateral horns).
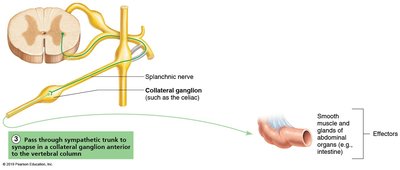
Preganglionic fibers: Short; may synapse in trunk ganglia at the same or different levels, or in collateral ganglia.
Postganglionic fibers: Long; extend to effector organs.
Neurotransmitter: Most postganglionic fibers release NE; some (e.g., to sweat glands) release ACh.
Neurotransmitters and Receptors in the ANS
Cholinergic and Adrenergic Fibers
Cholinergic fibers: Release ACh; include all ANS preganglionic axons and all parasympathetic postganglionic axons.
Adrenergic fibers: Release NE; include most sympathetic postganglionic axons (except those to sweat glands).
Cholinergic Receptors
Nicotinic receptors: Always stimulatory; found on all postganglionic neurons, adrenal medulla cells, and skeletal muscle cells at neuromuscular junctions.
Muscarinic receptors: Can be inhibitory or excitatory; found on all effector cells stimulated by postganglionic cholinergic fibers.
Adrenergic Receptors
Alpha (α) receptors: Subclasses α1, α2; effects depend on subclass and organ.
Beta (β) receptors: Subclasses β1, β2, β3; effects depend on subclass and organ.
Example: NE binding to β1 increases heart rate; epinephrine binding to β2 causes bronchial relaxation.
Interactions of Parasympathetic and Sympathetic Divisions
Dual Innervation and Tone
Most visceral organs receive dual innervation from both divisions, which typically have antagonistic effects.
Sympathetic tone: Maintains partial constriction of blood vessels; increases or decreases blood pressure as needed.
Parasympathetic tone: Dominates heart, digestive, and urinary organs under resting conditions; can be overridden by sympathetic division during stress.
Cooperative Effects
Some functions require cooperation between divisions, such as sexual function: parasympathetic fibers cause erection, sympathetic fibers cause ejaculation or vaginal contraction.
Effects of the Parasympathetic and Sympathetic Divisions on Various Organs
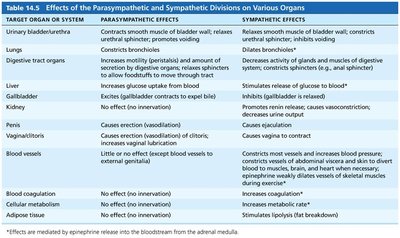
The following table summarizes the effects of each division on major organs and systems:
Target Organ or System | Parasympathetic Effects | Sympathetic Effects |
|---|---|---|
Urinary bladder/urethra | Contracts smooth muscle of bladder wall; relaxes urethral sphincter; promotes voiding | Relaxes smooth muscle of bladder wall; constricts urethral sphincter; inhibits voiding |
Lungs | Constricts bronchioles | Dilates bronchioles |
Digestive tract organs | Increases motility (peristalsis) and amount of secretion by digestive organs; relaxes sphincters to allow foodstuffs to move through tract | Decreases activity of glands and muscles of digestive system; constricts sphincters |
Liver | Increases glucose uptake from blood | Stimulates release of glucose to blood |
Gallbladder | Excites (gallbladder contracts to expel bile) | Inhibits (gallbladder is relaxed) |
Kidney | No effect (no innervation) | Promotes renin release; causes vasoconstriction; decreases urine output |
Vagina/uterus | Causes erection (vasodilation) of clitoris; increases vaginal lubrication | Causes vagina to contract |
Blood vessels | Little or no effect (except blood vessels to external genitalia) | Constriction most vessels; increases blood pressure; diverts blood to muscles, brain, and heart when necessary |
Penis | Causes erection (vasodilation) | Causes ejaculation |
Blood coagulation | No effect (no innervation) | Increases coagulation |
Cellular metabolism | No effect (no innervation) | Increases metabolic rate |
Adipose tissue | No effect (no innervation) | Stimulates lipolysis (fat breakdown) |
Additional info: The effects of the sympathetic division are often more widespread and longer-lasting than those of the parasympathetic division due to the release of hormones (epinephrine and norepinephrine) from the adrenal medulla into the bloodstream.
