 Back
BackThe Autonomic Nervous System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

Chapter 14: The Autonomic Nervous System (ANS)
Overview of the Autonomic Nervous System
The autonomic nervous system (ANS) is a division of the peripheral nervous system responsible for involuntary control of body functions, including the regulation of smooth muscle, cardiac muscle, and glands. It maintains homeostasis by balancing the activities of its two main divisions: the sympathetic and parasympathetic nervous systems.
Differences Between Somatic and Autonomic Nervous Systems
Structural and Functional Differences
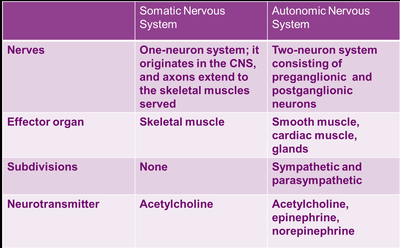
Somatic Nervous System (SNS): Controls voluntary movements via a single neuron pathway from the CNS to skeletal muscle.
Autonomic Nervous System (ANS): Controls involuntary functions using a two-neuron chain (preganglionic and postganglionic neurons) to reach effectors such as smooth muscle, cardiac muscle, and glands.
Neurotransmitters: SNS uses acetylcholine; ANS uses acetylcholine, norepinephrine, and epinephrine depending on the division and effector.
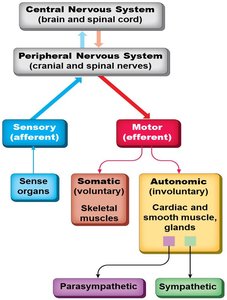
Divisions of the Autonomic Nervous System
Sympathetic and Parasympathetic Divisions
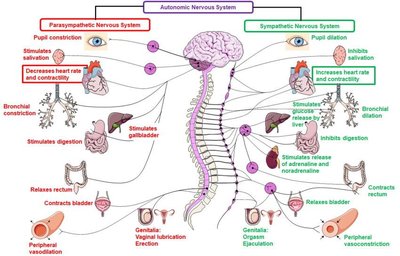
The ANS is divided into the sympathetic and parasympathetic divisions, which typically exert opposing effects on target organs to maintain homeostasis.
Sympathetic Division: Prepares the body for 'fight-or-flight' responses during stress or activity. Increases heart rate, dilates pupils, and mobilizes energy stores.
Parasympathetic Division: Promotes 'rest-and-digest' activities, conserving energy and facilitating digestion, urination, and defecation.
Dual Innervation: Most visceral organs receive input from both divisions, allowing dynamic antagonism for precise control.
Anatomy of the Parasympathetic (Craniosacral) Division
Organization and Pathways
Origin: Preganglionic neurons arise from the brainstem and sacral spinal cord (S2-S4).
Pathways: Long preganglionic fibers synapse in terminal ganglia near or within target organs; short postganglionic fibers innervate effectors.
Cranial Outflow: Includes oculomotor, facial, glossopharyngeal, and vagus nerves.
Sacral Outflow: Innervates pelvic organs and distal large intestine.
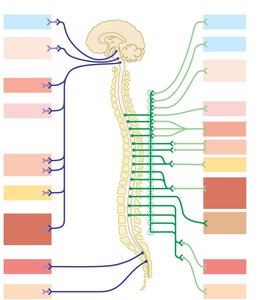
Anatomy of the Sympathetic (Thoracolumbar) Division
Organization and Pathways
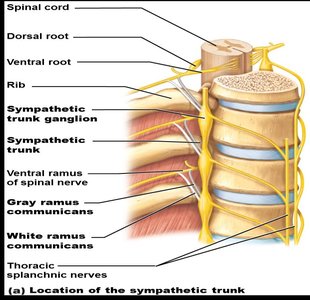
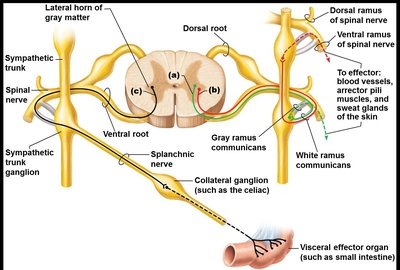
Origin: Preganglionic neurons are located in the lateral horns of spinal cord segments T1–L2.
Sympathetic Trunk: Preganglionic fibers enter the sympathetic trunk ganglia via white rami communicantes and may synapse at the same level, ascend/descend to other levels, or pass through to collateral ganglia.
Postganglionic Pathways: Fibers exit via gray rami communicantes to reach effectors.
Neurotransmitters and Receptors in the ANS
Types and Effects
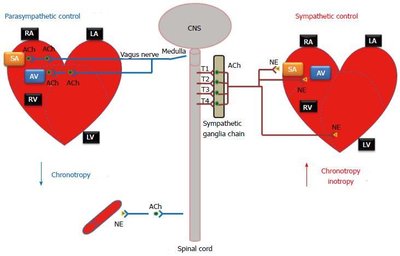
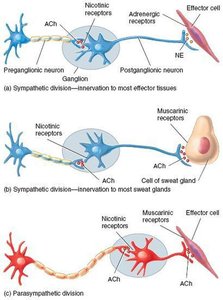
Cholinergic Fibers: Release acetylcholine (ACh). Includes all preganglionic neurons and parasympathetic postganglionic neurons.
Adrenergic Fibers: Release norepinephrine (NE). Most sympathetic postganglionic neurons are adrenergic, except those innervating sweat glands (which release ACh).
Receptors:
Cholinergic Receptors: Nicotinic (always excitatory) and muscarinic (excitatory or inhibitory depending on target).
Adrenergic Receptors: Alpha (α1, α2) and beta (β1, β2, β3) with varying effects on target organs.
Functional Interactions and Controls of the ANS
Dual Innervation and Central Control
Dual Innervation: Most organs receive both sympathetic and parasympathetic input, allowing for antagonistic or cooperative effects.
Central Control: The hypothalamus is the main integration center for ANS activity, with input from the limbic system, cerebral cortex, reticular formation, and spinal cord.
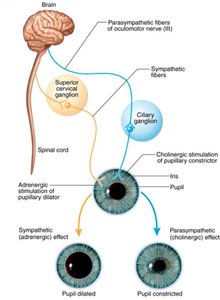
Sympathetic and Parasympathetic Tone
Baseline Activity and Modulation
Sympathetic Tone: Maintains partial constriction of blood vessels (vasomotor tone) and regulates blood pressure. Increased firing causes vasoconstriction; decreased firing causes vasodilation.
Parasympathetic Tone: Dominates heart rate, digestive, and urinary tract activity under resting conditions. Can be overridden by sympathetic activity during stress.
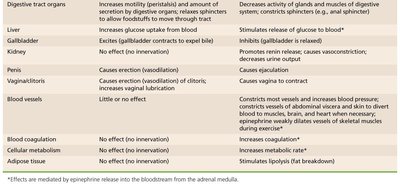
Cooperative and Unique Roles of the Sympathetic Division
Specialized Effects
Cooperative Effects: Both divisions work together in reproductive functions (e.g., erection by parasympathetic, ejaculation by sympathetic).
Unique Sympathetic Roles: Only the sympathetic division innervates the adrenal medulla, sweat glands, arrector pili muscles, kidneys, and most blood vessels. It also mediates thermoregulation, renin release, and metabolic effects (e.g., increased glucose, fat mobilization).
Pharmacology: Drugs Affecting the ANS
Drug Classes and Effects
Adrenergic Blockers: Used to treat hypertension by inhibiting sympathetic vasoconstriction.
Cholinergic Blockers: Increase heart rate and cause urinary/fecal retention by inhibiting parasympathetic effects.
Developmental Aspects and Disorders of the ANS
Development and Clinical Conditions
Development: Preganglionic neurons derive from the embryonic neural tube; postganglionic neurons and ganglia from neural crest cells.
Aging: ANS efficiency declines with age, leading to constipation, dry eyes, and orthostatic hypotension.
Disorders:
Hypertension: Often due to overactive sympathetic vasoconstriction; treated with adrenergic blockers.
Raynaud’s Disease: Exaggerated vasoconstriction in extremities, triggered by cold or stress; treated with vasodilators.
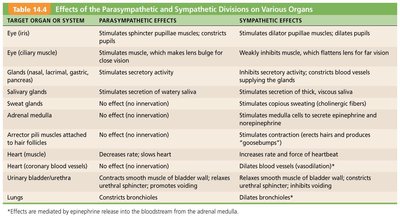
Summary Table: Effects of Parasympathetic and Sympathetic Divisions
Target Organ/System | Parasympathetic Effects | Sympathetic Effects |
|---|---|---|
Eye (pupil) | Constricts pupil | Dilates pupil |
Heart | Slows heart rate | Increases heart rate and force |
Digestive Tract | Increases motility and secretion | Decreases motility and secretion |
Blood Vessels | Little or no effect | Vasoconstriction (increases BP) |
Adrenal Medulla | No effect | Secretes epinephrine and norepinephrine |
Genitalia | Erection (vasodilation) | Ejaculation (male), vaginal contraction (female) |
Key Learning Objectives
Describe the differences between the somatic and autonomic nervous systems.
Identify the two main divisions of the ANS and their roles.
Explain the anatomy and pathways of the craniosacral (parasympathetic) and thoracolumbar (sympathetic) divisions.
Describe the role of neurotransmitters and receptors in the ANS.
Understand the interactions and controls of the ANS, including effects on various organs.
Identify the features of sympathetic and parasympathetic tone, cooperative effects, and unique roles of the sympathetic division.
Recognize drug classes affecting the ANS and their effects.
Discuss developmental aspects and disorders of the ANS.
