 Back
BackThe Autonomic Nervous System: Structure, Function, and Control
Study Guide - Smart Notes

The Autonomic Nervous System (ANS)
Overview of the ANS
The autonomic nervous system (ANS) is a division of the peripheral nervous system that regulates involuntary physiological processes, including heart rate, blood pressure, respiration, digestion, and glandular activity. It operates largely below the level of consciousness to maintain homeostasis.
Sensory Arm of the ANS
Visceral Sensory Neurons and Receptors
Visceral sensory neurons transmit information about chemical changes, stretch, temperature, and irritation from the viscera to the central nervous system (CNS).
These neurons rely on interoceptors (internal receptors) located in blood vessels, the heart, gastrointestinal tract, and urinary bladder.
Types of interoceptors include:
Chemoreceptors: Detect changes in blood oxygen, pH, and other chemicals.
Mechanoreceptors: Respond to stretch and pressure changes.
Most visceral sensory receptors are free nerve endings scattered throughout visceral organs.
Visceral Reflex Arcs
Components of the Visceral Reflex Arc
Visceral reflex arcs are fundamental to ANS function, mediating automatic responses to internal stimuli.
1. Receptor: Interoceptors that monitor internal conditions.
2. Sensory neuron: Carries information to the CNS.
3. Integration center: May be a preganglionic neuron, a dorsal horn interneuron, or within the walls of the gastrointestinal tract.
4. Motor neuron: Two-neuron chain (preganglionic and postganglionic neurons) from CNS to effectors.
5. Effector: Smooth muscle, cardiac muscle, or glands.
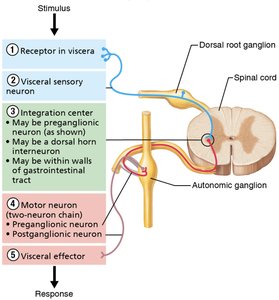
Effectors of the ANS
The main effectors activated by visceral reflex arcs are smooth muscle, cardiac muscle, and glands.
Comparison of Somatic and Autonomic Motor Pathways
Somatic Nervous System (SNS) vs. Autonomic Nervous System (ANS)
SNS: Single, heavily myelinated motor neuron from CNS to skeletal muscle; neurotransmitter is acetylcholine (ACh); always excitatory.
ANS: Two-neuron chain (preganglionic and postganglionic); preganglionic fibers are lightly myelinated, postganglionic are unmyelinated; effectors are smooth muscle, cardiac muscle, and glands; neurotransmitters include ACh and norepinephrine (NE); effects can be excitatory or inhibitory.
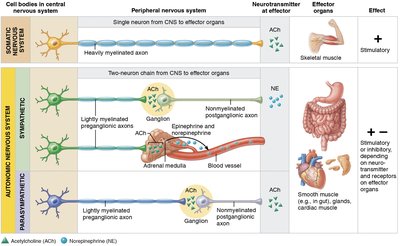
Preganglionic and Postganglionic Neurons
Preganglionic neuron: Cell body in brainstem or spinal cord; axon synapses with postganglionic neuron in an autonomic ganglion.
Postganglionic neuron: Cell body in autonomic ganglion outside CNS; axon extends to effector organ.
Divisions of the ANS: Parasympathetic and Sympathetic
Origins and Pathways
Parasympathetic (Craniosacral) Division: Fibers originate in brainstem and sacral spinal cord; long preganglionic and short postganglionic fibers; ganglia near or within effector organs; neurotransmitter is ACh.
Sympathetic (Thoracolumbar) Division: Fibers originate in thoracic and lumbar spinal cord; short preganglionic and long postganglionic fibers; ganglia close to spinal cord; neurotransmitters are ACh (preganglionic) and NE (postganglionic, except sweat glands which use ACh).
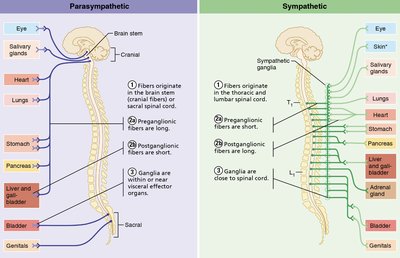
Dual Innervation
Most visceral organs receive input from both divisions, which typically have opposing effects to maintain homeostasis.
Autonomic Ganglia
Terminal ganglia: Parasympathetic; within or near effector organs.
Paravertebral (chain) ganglia: Sympathetic; paired, beside spinal cord.
Prevertebral (collateral) ganglia: Sympathetic; unpaired, anterior to spinal cord.
Sympathetic Pathways and the Adrenal Medulla
Sympathetic Preganglionic Fiber Pathways
Preganglionic fibers may synapse in the same-level ganglion, ascend/descend to another ganglion, or pass through to a collateral ganglion.
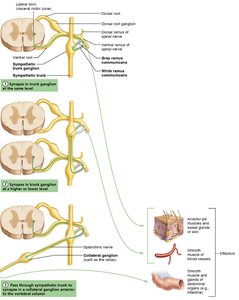
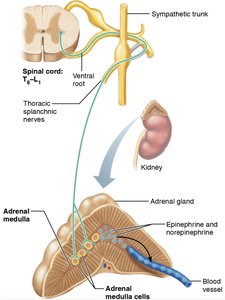
Adrenal Medulla Pathway
Some sympathetic preganglionic fibers pass directly to the adrenal medulla, where they synapse with hormone-secreting cells that release epinephrine and norepinephrine into the bloodstream.
These cells are considered modified sympathetic postganglionic neurons.
Neurotransmitters and Receptors in the ANS
Cholinergic and Adrenergic Fibers
Cholinergic fibers: Release ACh; include all ANS preganglionic axons and all parasympathetic postganglionic axons.
Adrenergic fibers: Release NE; most sympathetic postganglionic axons (except those to sweat glands).
Cholinergic Receptors
Nicotinic receptors: Found at neuromuscular junctions, all postganglionic neurons, and adrenal medulla cells; always excitatory.
Muscarinic receptors: Found on all parasympathetic target organs; effect can be excitatory or inhibitory depending on the organ.
Adrenergic Receptors
Alpha (α) receptors: α1 (generally excitatory), α2 (generally inhibitory).
Beta (β) receptors: β1 (excitatory, especially in heart), β2 (inhibitory, especially in smooth muscle), β3 (stimulates lipolysis in adipose tissue).
Physiological Effects of ANS Activation
Sympathetic Activation
Prepares the body for "fight or flight" responses: increases heart rate, dilates bronchioles, mobilizes energy stores, and redirects blood flow to muscles.
Effects are longer-lasting and more widespread due to hormone release from the adrenal medulla and slower breakdown of NE.
Parasympathetic Activation
Promotes "rest and digest" activities: stimulates digestion, reduces heart rate, and conserves energy.
Effects are short-lived and localized due to rapid breakdown of ACh.
ANS Tone and Control
Sympathetic (vasomotor) tone: Maintains partial constriction of blood vessels.
Parasympathetic (vagal) tone: Maintains resting heart rate below the intrinsic rate of the heart.
Hierarchy of ANS Control
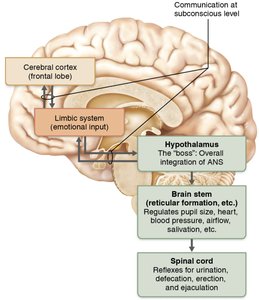
Central Nervous System Regulation
Hypothalamus: Main integration center for ANS activity; coordinates heart rate, blood pressure, temperature, water balance, and endocrine activity.
Brain stem (reticular formation): Directly regulates heart rate, blood pressure, respiration, and digestive activities.
Spinal cord: Controls reflexes for urination, defecation, erection, and ejaculation.
Cerebral cortex and limbic system: Influence ANS activity through emotional and conscious input.
Summary Table: Comparison of Parasympathetic and Sympathetic Divisions
Feature | Parasympathetic | Sympathetic |
|---|---|---|
Origin | Craniosacral (brainstem, sacral spinal cord) | Thoracolumbar (thoracic, lumbar spinal cord) |
Length of Fibers | Long preganglionic, short postganglionic | Short preganglionic, long postganglionic |
Location of Ganglia | Near or within effector organs | Close to spinal cord |
Neurotransmitter (postganglionic) | ACh | NE (most), ACh (sweat glands) |
General Function | Rest and digest | Fight or flight |
Additional info: This guide expands on the original notes with definitions, examples, and a summary table for clarity and exam preparation.
