 Back
BackThe Cardiovascular System: Blood and Blood Vessels
Study Guide - Smart Notes

The Cardiovascular System: Blood and Blood Vessels
Overview of the Cardiovascular System
The cardiovascular system is essential for transporting nutrients, gases, hormones, and waste products throughout the body. It consists of the heart (a muscular pump), blood vessels (arteries, veins, and capillaries), and blood (a connective tissue composed of plasma and formed elements). The system maintains homeostasis, supports cellular metabolism, and provides defense mechanisms.
Blood Composition and Functions
Blood is a specialized connective tissue with two main components: plasma and formed elements. Plasma is the liquid matrix, while formed elements include erythrocytes (red blood cells), leukocytes (white blood cells), and thrombocytes (platelets).
Plasma: Makes up about 55% of blood volume; contains water, electrolytes, nutrients, gases, hormones, and plasma proteins.
Formed Elements: Comprise about 45% of blood volume; include erythrocytes, leukocytes, and platelets.
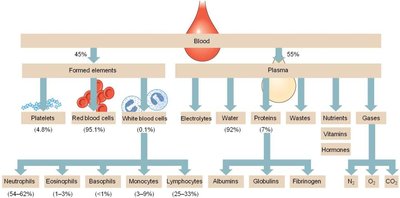
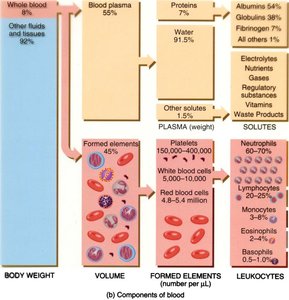
Plasma and Its Constituents
Plasma is primarily water (about 92%) and serves as a transport medium for blood cells and dissolved substances. It contains electrolytes, nutrients, gases, hormones, and plasma proteins such as albumins, globulins, and fibrinogen.
Albumins: Maintain osmotic pressure and transport hydrophobic molecules.
Globulins: Include antibodies and transport proteins.
Fibrinogen: Essential for blood clotting.
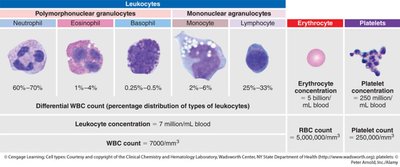
Formed Elements of Blood
The formed elements are produced in the bone marrow through the process of hematopoiesis. They include erythrocytes, leukocytes, and platelets.
Erythrocytes (RBCs): Transport oxygen and carbon dioxide; contain hemoglobin.
Leukocytes (WBCs): Defend against pathogens and remove debris. Subtypes include neutrophils, eosinophils, basophils, monocytes, and lymphocytes.
Platelets (Thrombocytes): Involved in hemostasis and blood clotting.
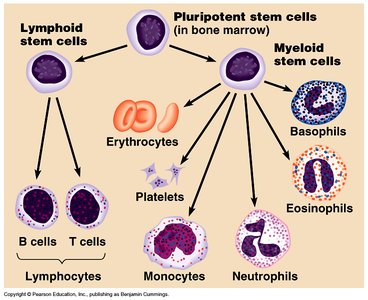
Hematopoiesis and Erythropoiesis
Hematopoiesis is the process of blood cell formation, occurring primarily in the bone marrow. Erythropoiesis is the specific formation of red blood cells, regulated by erythropoietin (EPO) in response to low oxygen levels.
Stages of Erythropoiesis: Hemocytoblast → Proerythroblast → Erythroblast → Normoblast (nucleus expelled) → Reticulocyte → Erythrocyte.
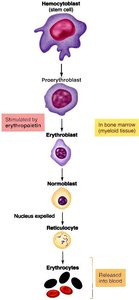
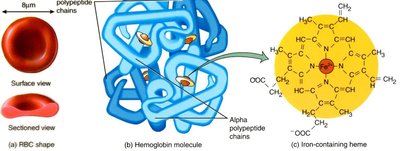
Structure and Function of Erythrocytes
Erythrocytes are biconcave, anucleate cells specialized for gas transport. Their shape increases surface area for gas exchange and allows flexibility to pass through capillaries. Each erythrocyte contains about 250 million hemoglobin molecules, each capable of binding four oxygen molecules.
Leukocytes: Types and Functions
Leukocytes are divided into granulocytes (neutrophils, eosinophils, basophils) and agranulocytes (monocytes, lymphocytes). They play roles in immune defense, phagocytosis, and antibody production.
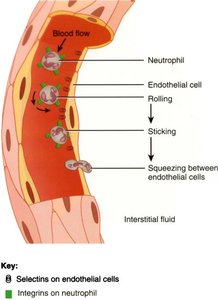
Neutrophils: Phagocytize bacteria and debris.
Eosinophils: Combat parasites and participate in allergic reactions.
Basophils: Release histamine and heparin during inflammatory responses.
Monocytes: Differentiate into macrophages for phagocytosis.
Lymphocytes: Include B cells (produce antibodies) and T cells (mediate immune responses).
Platelets and Hemostasis
Platelets are cell fragments derived from megakaryocytes. They play a critical role in hemostasis by forming a platelet plug and participating in the coagulation cascade to form a stable fibrin clot.
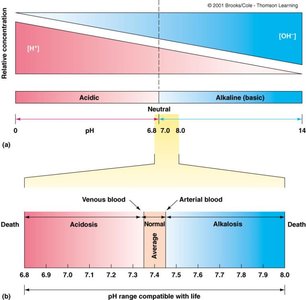
Blood pH and Homeostasis
Blood pH is tightly regulated between 7.35 and 7.45. Deviations can result in acidosis (pH < 7.35) or alkalosis (pH > 7.45), both of which can be life-threatening. Buffers in plasma, such as bicarbonate, help maintain pH homeostasis.
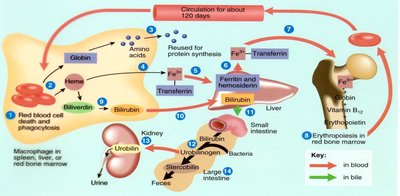
Blood Cell Lifespan and Recycling
Red blood cells have a lifespan of about 120 days. Senescent erythrocytes are removed by macrophages in the spleen and liver. Hemoglobin is broken down, and its components are recycled or excreted as bilirubin in bile and urine.
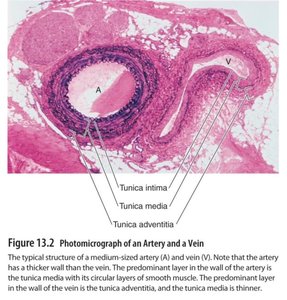
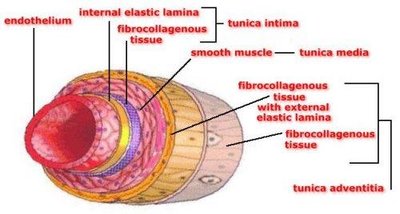
Blood Vessel Structure
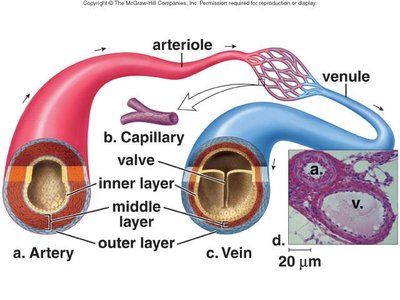
Blood vessels (except capillaries) have three layers: tunica intima (endothelium), tunica media (smooth muscle), and tunica adventitia (connective tissue). Arteries have thicker tunica media for resistance, while veins have larger lumens and valves for compliance and unidirectional flow.
Types of Capillaries
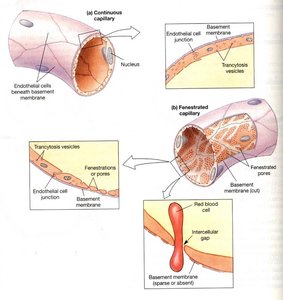
Capillaries are the site of exchange between blood and tissues. There are three types:
Continuous Capillaries: Most common; tight junctions; found in muscle, skin, and brain.
Fenestrated Capillaries: Have pores; found in kidneys, intestines, and endocrine glands.
Sinusoidal (Discontinuous) Capillaries: Large gaps; found in liver, bone marrow, and spleen.
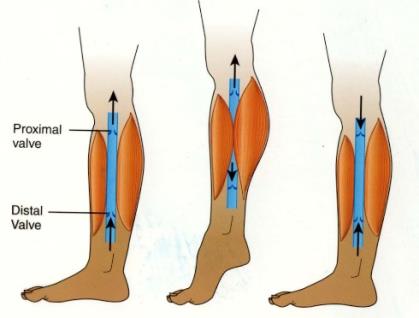
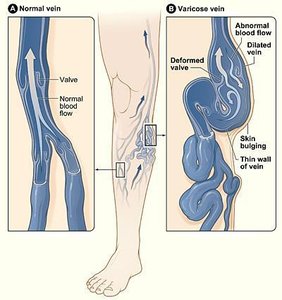
Venous Return Mechanisms
Venous return is aided by skeletal muscle contraction, respiratory pump, venous valves, and sympathetic vasoconstriction. These mechanisms ensure efficient return of blood to the heart, especially from the lower extremities.
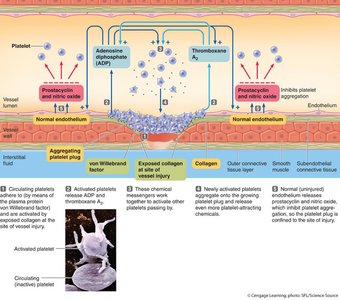
Hemostasis: Stopping Blood Loss
Hemostasis involves three main steps: vascular spasm (vasoconstriction), platelet plug formation, and coagulation (clotting cascade). The coagulation cascade involves intrinsic and extrinsic pathways, converging on the activation of thrombin, which converts fibrinogen to fibrin, forming a stable clot.
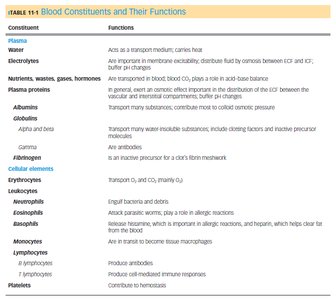
Summary Table: Blood Constituents and Their Functions
Constituent | Functions |
|---|---|
Plasma | Transport medium, carries heat, maintains osmotic balance, buffers pH |
Albumins | Osmotic pressure, transport hydrophobic molecules |
Globulins | Antibodies, transport proteins |
Fibrinogen | Clotting factor |
Erythrocytes | Transport O2 and CO2 |
Leukocytes | Immune defense |
Platelets | Hemostasis |
Additional info: This table summarizes the main functions of blood constituents for quick review.
