 Back
BackThe Cardiovascular System: Blood Vessels – Structure and Function
Study Guide - Smart Notes

The Cardiovascular System: Blood Vessels
Introduction
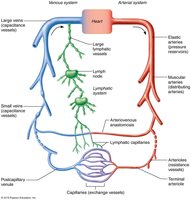
The cardiovascular system is responsible for the transport of blood throughout the body, ensuring the delivery of oxygen, nutrients, and the removal of waste products. Blood vessels form a dynamic network that begins and ends at the heart, working closely with the lymphatic system to maintain fluid balance and tissue health.
Blood Vessel Structure and Function
Types of Blood Vessels
Arteries: Carry blood away from the heart; typically oxygenated except in pulmonary circulation and fetal umbilical vessels.
Capillaries: Microscopic vessels in direct contact with tissue cells; primary site for exchange of substances.
Veins: Carry blood toward the heart; typically deoxygenated except in pulmonary circulation and fetal umbilical vessels.
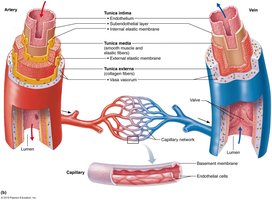
Structure of Blood Vessel Walls
All blood vessels (except capillaries) have three layers, or tunics, surrounding a central lumen:
Tunica intima: Innermost layer; consists of endothelium (simple squamous epithelium) that reduces friction and is continuous with the heart's endocardium. In larger vessels, a subendothelial layer of connective tissue is present.
Tunica media: Middle layer; composed mainly of smooth muscle and elastin. Controlled by sympathetic vasomotor nerves, it regulates vasoconstriction (narrowing) and vasodilation (widening) of the vessel, thus maintaining blood flow and pressure.
Tunica externa (adventitia): Outermost layer; made of loose collagen fibers that protect, reinforce, and anchor the vessel. Contains nerve fibers, lymphatic vessels, and in large veins, elastic fibers. The vasa vasorum nourishes the outer layers of large vessels.
Summary Table: Blood Vessel Anatomy
Vessel Type | Diameter & Wall Thickness | Relative Tissue Makeup |
|---|---|---|
Elastic artery | 1.0–2.5 cm | High elastin, moderate smooth muscle, thick wall |
Muscular artery | 0.3 mm–1.0 cm | Thick smooth muscle, less elastin |
Arteriole | 10 μm–0.3 mm | Thin wall, mostly smooth muscle |
Capillary | 8–10 μm | Endothelium only |
Venule | 8–100 μm | Endothelium, some smooth muscle in larger venules |
Vein | 0.1 mm–2.5 cm | Thin tunica media, thick tunica externa, large lumen |


Arteries
Classification of Arteries
Elastic arteries: Largest arteries (e.g., aorta); thick-walled, low-resistance, act as pressure reservoirs to maintain continuous blood flow.
Muscular arteries: Distribute blood to organs; thickest tunica media, active in vasoconstriction.
Arterioles: Smallest arteries; control blood flow into capillary beds via vasodilation and vasoconstriction, thus regulating resistance.
Capillaries
Structure and Function
Capillaries are microscopic vessels with walls consisting of a thin tunica intima, sometimes only a single endothelial cell thick. They allow for the exchange of gases, nutrients, wastes, and hormones between blood and interstitial fluid. Pericytes are contractile cells that help stabilize capillary walls and regulate permeability.
Types of Capillaries
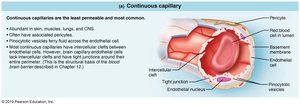
Continuous capillaries: Most common; found in skin, muscles, lungs, and CNS. Endothelial cells joined by tight junctions with intercellular clefts for limited permeability. In the brain, they form the blood-brain barrier with no clefts.
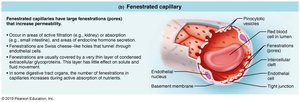
Fenestrated capillaries: Found in kidneys, intestines, and endocrine glands; have pores (fenestrations) for increased permeability, facilitating filtration and absorption.
Sinusoidal capillaries: Found in liver, bone marrow, spleen, and adrenal medulla; large, irregular lumens, fewer tight junctions, and large intercellular clefts for passage of large molecules and cells. Contain macrophages for immune defense.
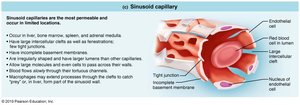
Capillary Beds and Microcirculation
Capillary beds are networks of capillaries between arterioles and venules. Microcirculation refers to the flow of blood from arterioles through capillary beds to venules. The flow is regulated by the diameter of arterioles and local chemical signals.
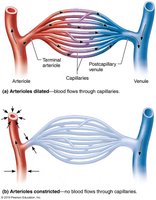
Special Capillary Arrangements
Vascular shunt: Direct connection between arteriole and venule, bypassing true capillaries (metarteriole-thoroughfare channel).
Precapillary sphincters: Rings of smooth muscle that regulate blood flow into true capillaries, controlled by local chemical conditions.
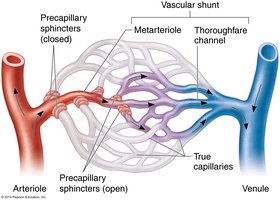
Veins
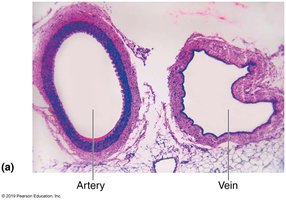
Structure and Function
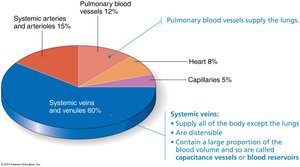
Veins form as venules merge and carry blood back to the heart. They have thinner walls and larger lumens than arteries, making them effective blood reservoirs (capacitance vessels), containing up to 65% of the body's blood supply. The tunica externa is the thickest layer, providing structural support.
Venous Adaptations
Venous valves: Prevent backflow of blood, especially in limbs.
Venous sinuses: Flattened veins with very thin walls, found in the heart (coronary sinus) and brain (dural sinuses).
Blood Volume Distribution
Veins contain the majority of the blood volume in the cardiovascular system, highlighting their role as blood reservoirs.
Clinical Application: Varicose Veins and Hemorrhoids
Varicose veins: Dilated, painful veins due to incompetent valves, often caused by prolonged standing, obesity, or pregnancy.
Hemorrhoids: Varicosities in anal veins due to increased intra-abdominal pressure (e.g., straining during childbirth or bowel movements).
Anastomoses
Vascular Anastomoses
Arterial anastomoses: Provide alternate pathways (collateral channels) for blood flow, common in joints, abdominal organs, brain, and heart.
Arteriovenous anastomoses: Shunts in capillaries (e.g., metarteriole–thoroughfare channel).
Venous anastomoses: Very abundant; occlusion rarely blocks blood flow.
Summary Table: Blood Vessel Anatomy (continued)


Additional info: The structure and function of blood vessels are essential for understanding cardiovascular physiology and pathology. Knowledge of vessel anatomy aids in clinical diagnosis and treatment of vascular diseases.
