 Back
BackThe Cardiovascular System: Blood Vessels – Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessel Structure and Function
Overview of the Vascular System
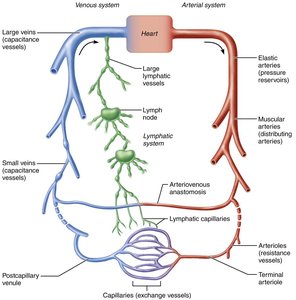
The cardiovascular system is composed of a closed network of blood vessels that transport blood throughout the body, working in conjunction with the lymphatic system to maintain fluid balance and tissue health. Blood vessels are dynamic structures that can constrict, dilate, and adapt to physiological demands.
Arteries: Carry blood away from the heart. Systemic arteries transport oxygenated blood, while pulmonary arteries carry oxygen-poor blood.
Capillaries: Serve as exchange vessels, allowing for the transfer of gases, nutrients, and wastes between blood and tissues.
Veins: Return blood to the heart. Systemic veins carry deoxygenated blood, while pulmonary veins carry oxygenated blood.
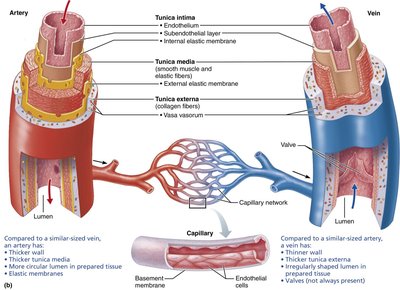
Layers of Blood Vessel Walls
Except for capillaries, most blood vessels have three distinct layers (tunics) surrounding a central lumen:
Tunica intima: Innermost layer, composed of endothelium (simple squamous epithelium) and a subendothelial layer in larger vessels. Provides a smooth, friction-reducing lining.
Tunica media: Middle layer, primarily smooth muscle and elastin. Responsible for vasoconstriction and vasodilation, thus regulating blood flow and pressure.
Tunica externa (adventitia): Outermost layer, mainly collagen fibers that protect, reinforce, and anchor the vessel. Contains nerves, lymphatics, and in large vessels, vasa vasorum (small vessels that nourish the outer wall).
Comparison of Blood Vessel Types
Blood vessels vary in structure and function depending on their type and location. The following table summarizes key anatomical differences:
Vessel Type | Wall Thickness | Lumen Diameter | Key Features |
|---|---|---|---|
Elastic artery | Thick | Largest | Pressure reservoirs, high elastin content |
Muscular artery | Thick (media) | Medium | Distributing arteries, more smooth muscle |
Arteriole | Thin | Smallest | Resistance vessels, control flow to capillaries |
Capillary | Very thin (one cell layer) | Tiny | Exchange vessels |
Venule | Thin | Small | Very porous, allow WBCs/fluid movement |
Vein | Thinner than arteries | Large | Capacitance vessels, valves present |

Types of Capillaries
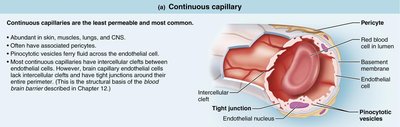
Continuous Capillaries
Continuous capillaries are the most common and least permeable type, found in skin, muscles, lungs, and the central nervous system. They have tight junctions between endothelial cells but also small gaps (intercellular clefts) for limited passage of fluids and small solutes.
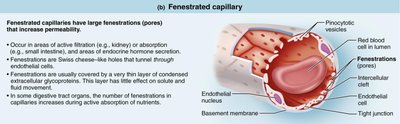
Fenestrated Capillaries
Fenestrated capillaries contain pores (fenestrations) that increase permeability. They are found in areas of active filtration (kidneys), absorption (intestines), and endocrine hormone secretion.
Sinusoidal Capillaries
Sinusoidal capillaries are the most permeable and are found in the liver, bone marrow, spleen, and adrenal medulla. They have large intercellular clefts, fenestrations, and an incomplete basement membrane, allowing passage of large molecules and cells.
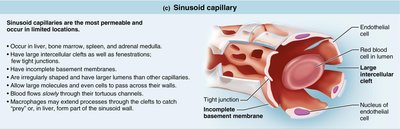
Capillary Beds and Microcirculation
Structure and Regulation of Capillary Beds
Capillary beds are networks of capillaries between arterioles and venules, facilitating exchange with tissues. Blood flow through these beds is regulated by the diameter of arterioles and the presence of precapillary sphincters.
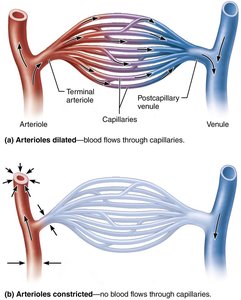
Specialized Capillary Bed Features
In some tissues, such as the intestinal mesenteries, capillary beds include vascular shunts (metarteriole-thoroughfare channels) and precapillary sphincters that regulate flow into true capillaries.
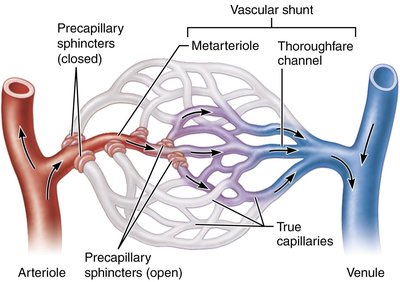
Veins and Venous Return
Structure and Function of Veins
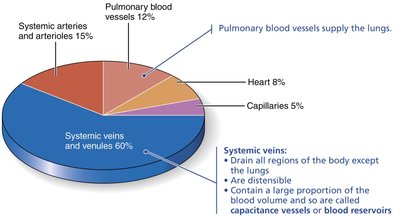
Veins return blood to the heart and act as blood reservoirs, containing up to 65% of the blood supply at any time. They have thinner walls, larger lumens, and lower pressure compared to arteries. Adaptations such as valves prevent backflow, especially in the limbs.
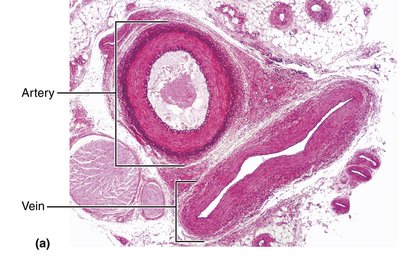
Blood Flow, Pressure, and Resistance
Key Hemodynamic Principles
Blood flow (F) is the volume of blood moving through a vessel or the entire circulation per unit time. Blood pressure (BP) is the force per unit area exerted on a vessel wall by the blood. Resistance (R) is the opposition to flow, mainly due to vessel diameter, blood viscosity, and vessel length.
Relationship:
Blood flow is directly proportional to the pressure gradient and inversely proportional to resistance.
Small changes in vessel diameter have a large effect on resistance (inversely proportional to the fourth power of the radius).

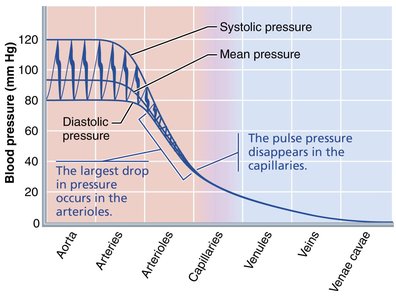
Blood Pressure Changes in the Systemic Circulation
Blood pressure is highest in the aorta and decreases through the arterial system, capillaries, and veins. The steepest drop occurs in the arterioles, which are the main resistance vessels.
Regulation of Blood Pressure
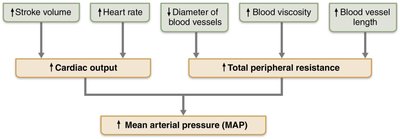
Major Factors Affecting Mean Arterial Pressure (MAP)
MAP is determined by cardiac output (CO), total peripheral resistance (TPR), and blood volume. The relationship can be expressed as:
CO is the product of stroke volume (SV) and heart rate (HR):
Short-Term Regulation: Neural and Hormonal Controls
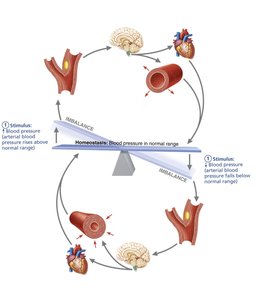
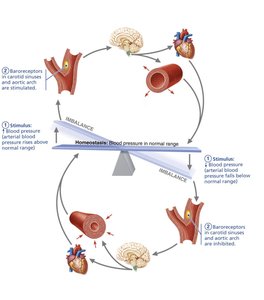
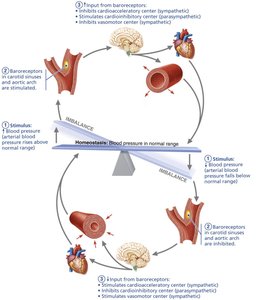
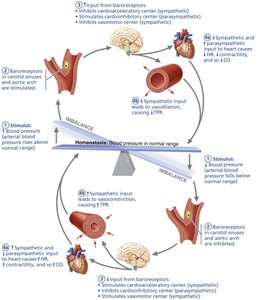
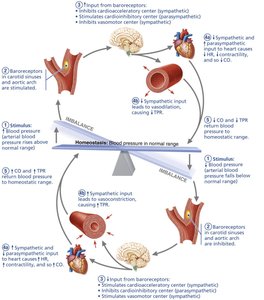
Neural controls (baroreceptor and chemoreceptor reflexes) and hormones (e.g., epinephrine, norepinephrine, angiotensin II, ADH, ANP) regulate blood pressure by altering vessel diameter, heart rate, and blood volume.
Baroreceptors in the carotid sinuses and aortic arch detect changes in pressure and adjust sympathetic/parasympathetic output accordingly.
Chemoreceptors respond to changes in blood CO2, pH, and O2 levels.
Long-Term Regulation: Renal Mechanisms
Kidneys regulate blood pressure by controlling blood volume through direct (filtration and urine formation) and indirect (renin-angiotensin-aldosterone system) mechanisms.
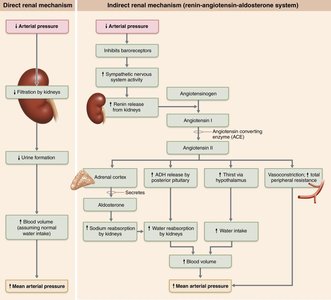
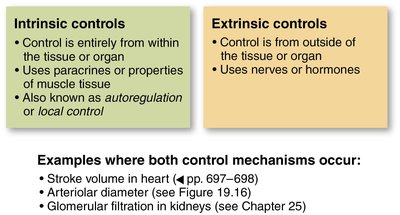
Intrinsic and Extrinsic Control of Blood Flow
Autoregulation and Tissue Perfusion
Blood flow to tissues is regulated by intrinsic (local) and extrinsic (systemic) mechanisms. Intrinsic controls (autoregulation) adjust flow based on local metabolic needs, while extrinsic controls (nervous and endocrine) maintain systemic blood pressure and redistribute blood as needed.

Capillary Exchange and Bulk Flow
Mechanisms of Capillary Exchange
Capillary exchange occurs via diffusion, transcytosis, and bulk flow. Bulk flow is driven by hydrostatic and osmotic pressures, determining the movement of fluid into and out of capillaries.
Net Filtration Pressure (NFP):
Filtration occurs at the arterial end; reabsorption at the venous end.
Clinical Correlations
Homeostatic Imbalances
Varicose veins: Result from incompetent valves, leading to dilated, tortuous veins.
Edema: Excess interstitial fluid due to increased filtration or decreased reabsorption, often from increased capillary hydrostatic pressure, decreased plasma proteins, or lymphatic obstruction.
Summary Table: Blood Vessel Types and Functions
Vessel Type | Main Function | Key Structural Features |
|---|---|---|
Elastic arteries | Pressure reservoirs | Thick walls, high elastin |
Muscular arteries | Distributing vessels | Thick tunica media, more smooth muscle |
Arterioles | Resistance vessels | Small diameter, control flow to capillaries |
Capillaries | Exchange vessels | Single endothelial layer |
Venules | Collect blood from capillaries | Very porous, thin walls |
Veins | Capacitance vessels | Large lumens, valves, thin walls |
