 Back
BackThe Cardiovascular System: Blood Vessels – Structure, Function, and Hemodynamics
Study Guide - Smart Notes

The Blood Vessels: Overview and Functions
Introduction to the Vasculature
The vasculature is a complex network of blood vessels responsible for transporting blood throughout the body. This system ensures the delivery of oxygen, nutrients, and the removal of waste products, while also playing a role in regulating blood flow, blood pressure, and chemical secretion.
Arteries: Carry blood away from the heart; systemic arteries carry oxygenated blood, pulmonary arteries carry deoxygenated blood.
Veins: Return blood to the heart; systemic veins carry deoxygenated blood, pulmonary veins carry oxygenated blood.
Capillaries: Facilitate exchange of gases, nutrients, and wastes between blood and tissues.
Structure and Function of Arteries and Veins
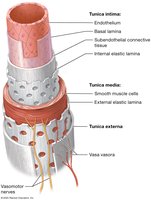
Blood Vessel Wall Layers (Tunics)
Blood vessels are composed of three main layers, or tunics, surrounding a central lumen:
Tunica Intima: Innermost layer; consists of endothelium (simple squamous epithelium), basal lamina, subendothelial connective tissue, and internal elastic lamina. Provides a smooth, low-friction surface and produces regulatory chemicals.
Tunica Media: Middle layer; composed of smooth muscle cells and elastic fibers (external elastic lamina). Responsible for vasoconstriction and vasodilation, regulated by the sympathetic nervous system.
Tunica Externa (Adventitia): Outermost layer; dense irregular connective tissue that supports and protects the vessel. Contains vasa vasorum, small vessels that supply the outer layers of large vessels.
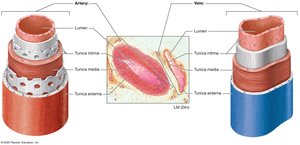
Comparison of Arteries and Veins
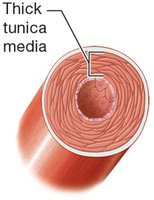
Arteries have thicker tunica media and more elastic fibers to withstand higher pressures.
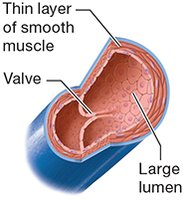
Veins have thinner walls, larger lumens, and often contain valves to prevent backflow.
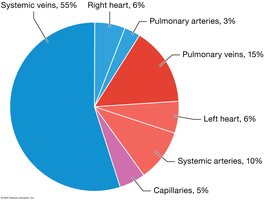
Blood Distribution
Systemic veins serve as blood reservoirs, holding about 55% of total blood volume.
Arteries, capillaries, and the heart contain the remainder.
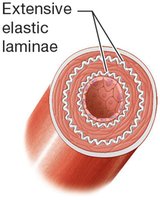
Types of Arteries
Elastic (Conducting) Arteries: Largest diameter, extensive elastic laminae, withstand highest pressure (e.g., aorta).
Muscular (Distributing) Arteries: Medium diameter, thick tunica media, regulate blood flow to organs.
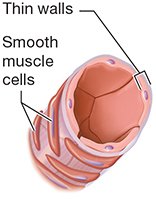
Arterioles: Smallest arteries, control blood flow into capillary beds via precapillary sphincters.
Types of Veins
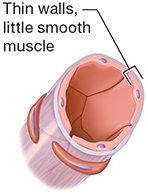
Venules: Smallest veins, drain capillary beds, allow some exchange.
Medium and Large Veins: Thin walls, large lumens, contain valves (especially in limbs) to prevent backflow.
Hemodynamics: Blood Flow and Pressure
Basic Principles
Blood Pressure (BP): The force blood exerts on vessel walls, measured in mm Hg.
Blood Flow: Volume of blood moving through a vessel per minute; directly proportional to pressure gradient and inversely proportional to resistance.
Resistance: Opposition to flow, affected by vessel radius, blood viscosity, and vessel length.
Cross-Sectional Area and Velocity
As vessels branch, total cross-sectional area increases and blood velocity decreases.
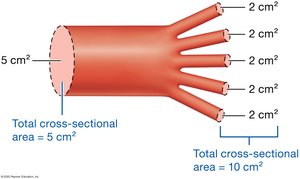
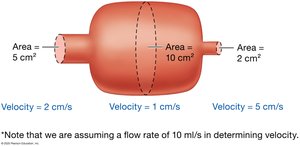
Factors Affecting Blood Pressure
Peripheral Resistance: Increased by smaller vessel radius, higher viscosity, longer vessel length, or obstructions.
Cardiac Output (CO): Product of stroke volume and heart rate; increased CO raises BP.
Blood Volume: More blood increases BP; regulated by water content and vessel compliance.
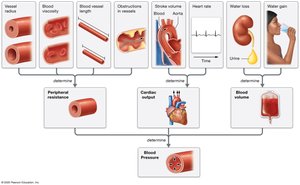
Pressure Changes in Circulation
BP is highest in the aorta and declines through the arterial system, capillaries, and veins.
Mean Arterial Pressure (MAP) is the average pressure in systemic arteries during a cardiac cycle.
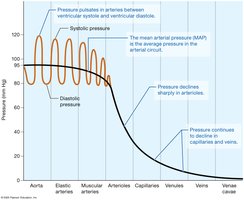
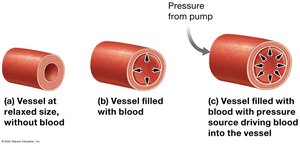
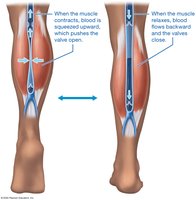
Venous Return Mechanisms
Venous valves, smooth muscle contraction, skeletal muscle pump, and respiratory pump all aid in returning blood to the heart.
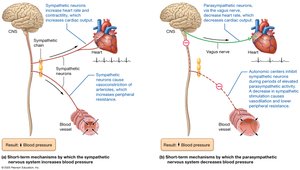
Short- and Long-Term Regulation of Blood Pressure
Short-Term Regulation
Autonomic Nervous System: Sympathetic stimulation increases BP (vasoconstriction, increased CO); parasympathetic stimulation decreases BP (vasodilation, decreased CO).
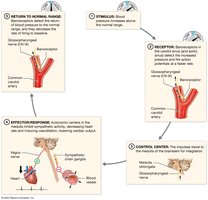
Baroreceptor Reflex: Stretch receptors in carotid and aortic sinuses detect BP changes and adjust heart rate and vessel diameter accordingly.
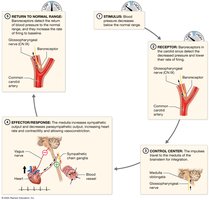
Chemoreceptor Reflexes: Respond to changes in blood O2, CO2, and pH, influencing heart rate and vessel tone.
Hormonal Regulation
Epinephrine, norepinephrine, and thyroid hormone increase cardiac output and resistance.
Angiotensin II increases resistance; atrial natriuretic peptide (ANP) decreases resistance.
Long-Term Regulation
Kidneys regulate blood volume by adjusting water excretion (influenced by ADH, aldosterone, ANP, and the renin-angiotensin-aldosterone system).
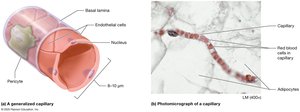
Capillary Structure and Function
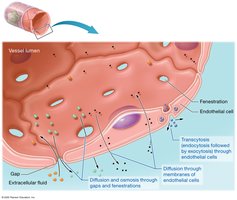
Capillary Exchange Mechanisms
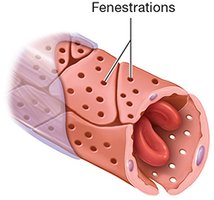
Diffusion and osmosis through gaps and fenestrations
Diffusion through endothelial cell membranes
Transcytosis for larger molecules
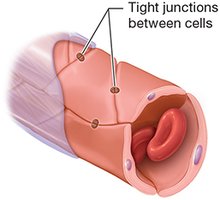
Types of Capillaries
Continuous Capillaries: Least leaky, found in muscle, skin, and brain (blood-brain barrier).
Fenestrated Capillaries: Have pores, found in endocrine glands, kidneys, and small intestine.
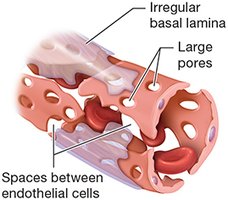
Sinusoidal Capillaries: Large gaps, found in liver, spleen, and bone marrow.
Capillary Beds and Tissue Perfusion
Microcirculation and Regulation
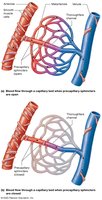
Capillary beds consist of true capillaries and a central vessel (metarteriole/thoroughfare channel).
Precapillary sphincters regulate blood flow into capillary beds.
Autoregulation via myogenic and metabolic mechanisms ensures proper tissue perfusion.
Pressures at Work in Capillaries
Hydrostatic and Osmotic Pressures
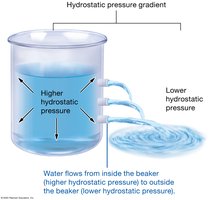
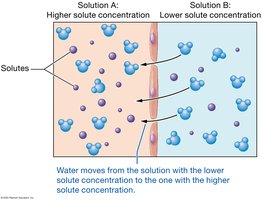
Hydrostatic Pressure (HP): Pushes water out of capillaries (filtration).
Osmotic Pressure (OP): Draws water into capillaries (absorption), mainly due to plasma proteins (colloid osmotic pressure).
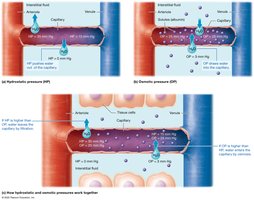
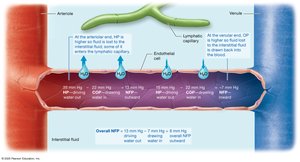
Net Filtration Pressure (NFP)
At the arterial end, HP > OP, so fluid leaves the capillary (filtration).
At the venous end, OP > HP, so fluid enters the capillary (absorption).
Overall, there is a net loss of fluid to the interstitial space, which is returned by the lymphatic system.

Major Systemic Arteries and Veins
Systemic Arteries
Aorta: Main artery leaving the left ventricle, with ascending, arch, thoracic, and abdominal divisions.
Major branches supply the head, neck, upper and lower limbs, thoracic and abdominal organs.
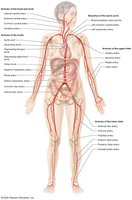
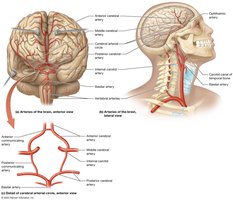
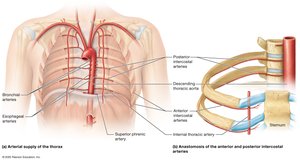
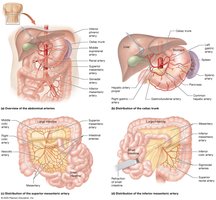
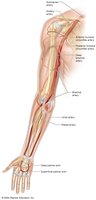
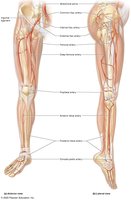
Pulse Points
Locations where arterial pulsations can be palpated, such as carotid, radial, femoral, and dorsalis pedis arteries.
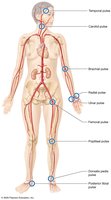
Systemic Veins
Superior and Inferior Vena Cava: Major veins returning blood to the right atrium from the upper and lower body, respectively.
Veins are often paired with arteries and named similarly, but have more anastomoses and variable patterns.
Clinical Correlations
Atherosclerosis
Formation of plaques in arterial walls, leading to reduced blood flow, risk of heart attack, and stroke.
Risk factors include hypertension, high cholesterol, smoking, and diabetes.

Hypertension and Hypotension
Hypertension: Chronic high blood pressure; increases risk of cardiovascular disease, stroke, and kidney failure.
Hypotension: Abnormally low blood pressure; can lead to dizziness, fainting, and organ failure if severe.
Varicose Veins
Enlarged, twisted veins due to valve failure, commonly in the lower limbs.

Cerebrovascular Accident (Stroke)
Disruption of blood flow to the brain, causing neurological deficits or death.
Caused by clot (ischemic) or hemorrhage (hemorrhagic).


Summary Table: Types of Arteries and Veins
Type | Structure | Function |
|---|---|---|
Elastic Artery | Large diameter, many elastic fibers | Conduct blood under high pressure |
Muscular Artery | Thick tunica media, more smooth muscle | Distribute blood to organs, regulate flow |
Arteriole | Small diameter, thin wall | Control flow into capillaries |
Capillary | Single layer endothelium | Exchange of substances |
Venule | Thin wall, little muscle | Drain capillaries |
Vein | Thin wall, large lumen, valves | Return blood to heart |
Additional info: This guide integrates textbook-level explanations, clinical context, and visual aids for comprehensive understanding of blood vessel anatomy and physiology, suitable for ANP college students.
