 Back
BackThe Cardiovascular System I: The Heart – Structure, Function, and Physiology
Study Guide - Smart Notes

The Heart: Overview and Anatomy
Location and General Function
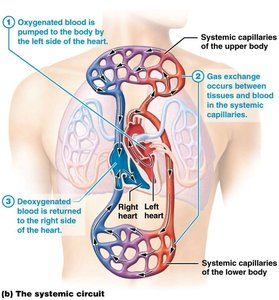
The heart is a muscular organ located within the mediastinum, anterior to the vertebral column, posterior to the sternum, and superior to the diaphragm. Approximately two-thirds of the heart lies to the left of the midline. Its primary function is to pump blood through approximately 60,000 miles of vessels, including both pulmonary and systemic circuits.
Pulmonary circuit: Carries blood between the heart and lungs for gas exchange.
Systemic circuit: Distributes oxygenated blood from the heart to the body and returns deoxygenated blood.
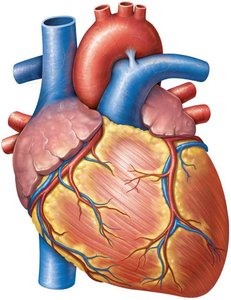
External and Internal Anatomy
The heart consists of four chambers that prevent mixing of oxygen-rich and oxygen-poor blood:
Atria: Two receiving chambers (right and left) with auricles to increase capacity.
Ventricles: Two outgoing chambers (right and left).
Sulci: Grooves on the exterior surface marking the location of coronary vessels.
Heart Wall and Pericardium
Layers of the Heart Wall
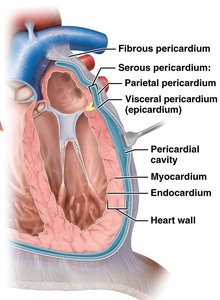
The heart wall is composed of three main layers:
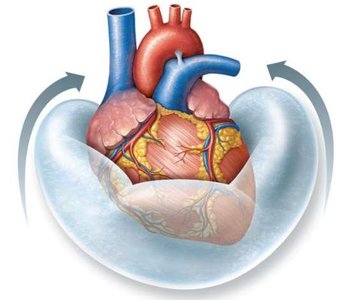
Pericardium: Encloses the heart and consists of two parts: fibrous and serous pericardium. The serous pericardium has parietal and visceral layers, with pericardial fluid between them to reduce friction.
Myocardium: The thick, muscular middle layer responsible for contraction; makes up 95% of heart mass.
Endocardium: The innermost layer lining the heart chambers and valves, continuous with the lining of large vessels.
Heart Valves and Blood Flow
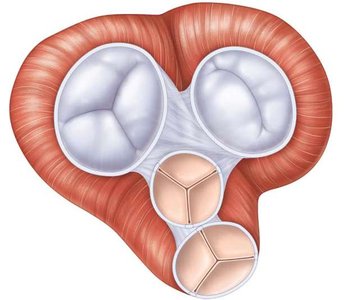
Valves and Associated Structures
Heart valves ensure one-way flow of blood and prevent backflow between chambers.
Atrioventricular (AV) valves: Separate atria from ventricles.
Right: Tricuspid valve
Left: Bicuspid (mitral) valve
Semilunar (SL) valves: Separate ventricles from arteries.
Right: Pulmonary valve
Left: Aortic valve
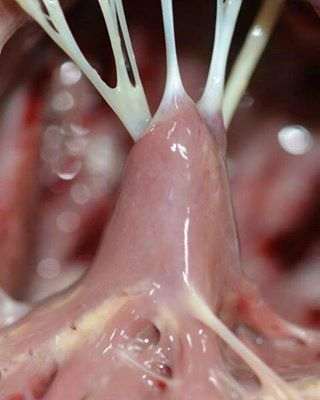
Chordae tendineae: Connect valves to papillary muscles, preventing valve prolapse.
Papillary muscles: Contract to tighten chordae tendineae during ventricular contraction.
Blood Flow Pathway
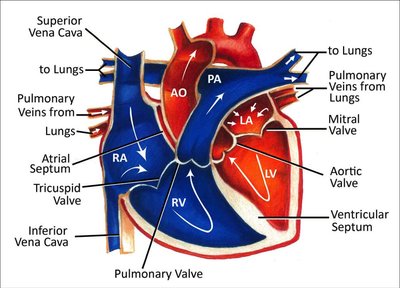
The pathway of blood through the heart ensures unidirectional flow:
Deoxygenated blood enters the right atrium from the vena cavae and coronary sinus.
Blood passes through the tricuspid valve into the right ventricle.
Right ventricle contracts, pumping blood through the pulmonary semilunar valve into the pulmonary trunk and arteries to the lungs.
Oxygenated blood returns from the lungs via pulmonary veins to the left atrium.
Blood passes through the bicuspid (mitral) valve into the left ventricle.
Left ventricle contracts, pumping blood through the aortic semilunar valve into the aorta and systemic circulation.
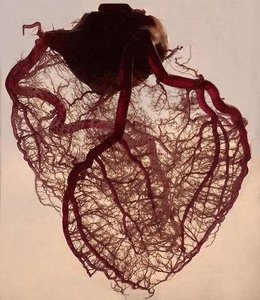
Coronary Circulation
Arteries and Veins
The heart's own tissue receives oxygen and nutrients via the coronary arteries, which branch off the aorta.
Right and left coronary arteries: Supply oxygen-rich blood to heart tissue.
Cardiac veins: Collect deoxygenated blood from heart tissue.
Coronary sinus: Returns deoxygenated blood to the right atrium.
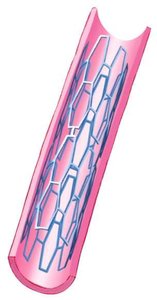
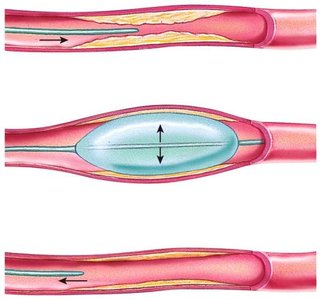
Coronary Artery Disease (CAD)
CAD is caused by obstructions such as atherosclerosis or clots, reducing blood and oxygen supply to heart tissue.
Angioplasty: Procedure to remove obstructions and restore blood flow.
Stent: Device used to strengthen vessels after angioplasty.
Myocardial infarction: Heart attack, the most dangerous consequence of CAD.
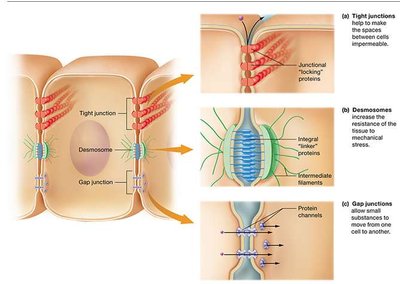
Cardiac Muscle Tissue and Electrophysiology
Histology and Cell Types
Cardiac muscle tissue is striated and involuntary, with cells that have a single nucleus, branching structure, and abundant mitochondria. Cells are connected by intercalated discs containing gap junctions and desmosomes, allowing rapid electrical communication and mechanical strength.
Pacemaker cells: Autorhythmic cells that generate spontaneous action potentials.
Contractile cells: Responsible for the force of contraction.
Action Potential Phases
Cardiac muscle action potentials have distinct phases:
Depolarization: Rapid influx of Na+ ions.
Plateau phase: Ca2+ influx maintains depolarization, prolonging contraction.
Repolarization: K+ efflux restores resting potential.
The plateau phase is crucial for preventing tetanus and ensuring proper heart function.
Cardiac Conduction System
The conduction system coordinates the heartbeat:
Sinoatrial (SA) node: Pacemaker in the right atrium.
Atrioventricular (AV) node: Located between atria and ventricles.
AV Bundle (Bundle of His): Transmits signal to ventricles.
Purkinje fibers: Spread signal throughout ventricles.
Electrocardiogram (ECG) and Arrhythmias
ECG Waveforms
An ECG records the electrical activity of the heart, showing three main waveforms:
P wave: Atrial depolarization
QRS complex: Atrial repolarization and ventricular depolarization
T wave: Ventricular repolarization
Arrhythmias
Abnormal heart rhythms can result from defects in the conduction system:
Bradycardia: Slow heart rate
Tachycardia: Fast heart rate
AV block: Prolonged PQ interval, slow conduction through AV node
Atrial fibrillation: Asynchronous atrial contraction, no P wave
Ventricular fibrillation: No waves or complexes, life-threatening
Mechanical Physiology: The Cardiac Cycle
Phases of the Cardiac Cycle
The cardiac cycle includes all electrical, pressure, volume, and auditory events of one heartbeat.
Systole: Contraction phase, blood is forced from areas of high pressure to low pressure.
Diastole: Relaxation phase.
Events of the Cardiac Cycle
Atrial systole: Increased pressure in atria opens AV valves; ventricles in diastole. End-diastolic volume (EDV) is the amount of blood in the ventricle at the end of relaxation.
Ventricular systole: Increased pressure closes AV valves and opens SL valves. End-systolic volume (ESV) is the volume remaining in the ventricle after contraction. Stroke volume (SV) is calculated as .
Relaxation: Both atria and ventricles relax; all four valves closed during isovolumetric relaxation. Falling pressure in ventricles opens AV valves.
Heart Sounds
Lubb: First sound, caused by closing of AV valves at the beginning of ventricular systole.
Dupp: Second sound, caused by closing of SL valves at the end of ventricular systole.
Cardiac Output and Regulation
Cardiac Output Calculation
Cardiac output (CO) is the amount of blood pumped by a ventricle in one minute.
Formula:
Example:
Regulation of Stroke Volume and Heart Rate
Preload: The effect of stretching; increased preload increases force of contraction and stroke volume (Frank-Starling Law).
Afterload: The back pressure that must be exceeded to eject blood; decreased afterload increases stroke volume.
Autonomic regulation: The cardiovascular center in the medulla oblongata integrates sensory inputs.
Sympathetic impulses increase heart rate, contractility, and stroke volume.
Parasympathetic impulses (via vagus nerve) decrease heart rate.
Factors Affecting Cardiac Output
Chronotropic agents: Short-term changes in heart rate.
Chemical agents: Hormones (epinephrine, norepinephrine, thyroid hormones, ADH), electrolyte concentrations (Ca2+, Na+, K+).
Other factors: Body temperature, age, fitness.
Congestive Heart Failure
Reduced cardiac output in failing hearts.
Cardiac myopathy (diseased heart muscle) leads to pulmonary congestion, edema, and peripheral edema.
Improving cardiac output may involve moderate activity, drug therapy, pacemakers, stents, or transplant.
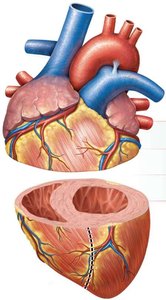
Comparison Table: Right vs. Left Ventricle
Ventricle | Wall | Chamber |
|---|---|---|
Right ventricle | Thin | Crescent-shaped |
Left ventricle | Thick | Circular |
Summary
The heart is a complex organ with specialized structures and functions that ensure efficient circulation of blood throughout the body. Understanding its anatomy, physiology, and regulatory mechanisms is essential for comprehending cardiovascular health and disease.
