 Back
BackThe Cardiovascular System: Structure and Function
Study Guide - Smart Notes

The Cardiovascular System
Overview and Functions
The cardiovascular system is a closed system composed of the heart and blood vessels. Its primary function is to transport oxygen, nutrients, cell wastes, and hormones to and from the cells throughout the body.
Heart: Pumps blood throughout the body.
Blood Vessels: Allow blood to circulate to all body parts.
Main Functions: Transport, protection, and regulation of body temperature and pH.
Anatomy of the Heart
Location and Orientation
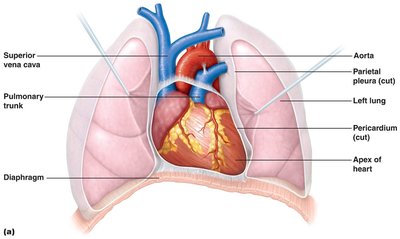
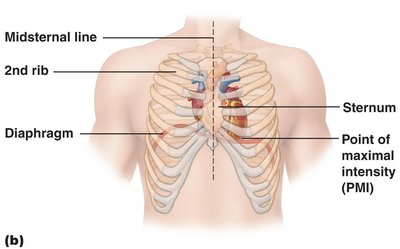
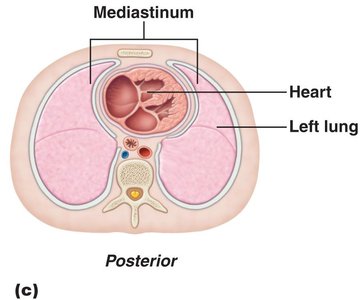
The heart is about the size of a human fist and weighs less than a pound. It is located in the thoracic cavity, between the lungs in the inferior mediastinum. The apex points toward the left hip and rests on the diaphragm, while the base points toward the right shoulder.
Heart Wall and Coverings
The heart wall consists of three layers, and the heart is enclosed by a double-walled sac called the pericardium.
Fibrous Pericardium: Tough, dense connective tissue that anchors the heart and prevents overexpansion.
Serous Pericardium: Has two layers—parietal (lines inside of fibrous pericardium) and visceral (epicardium, covers heart surface).
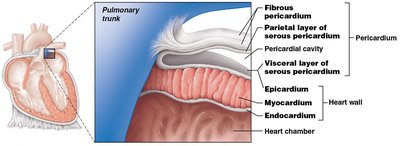
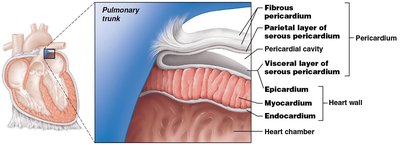
Epicardium: Outermost layer, also known as the visceral pericardium.
Myocardium: Middle layer, composed mostly of cardiac muscle; responsible for contraction.
Endocardium: Inner layer, known as endothelium.

Clinical View: Pericarditis
Pericarditis is inflammation of the pericardium, often caused by infection. It can lead to fluid accumulation, restricting heart movement (cardiac tamponade), and is detected by a friction rub sound.
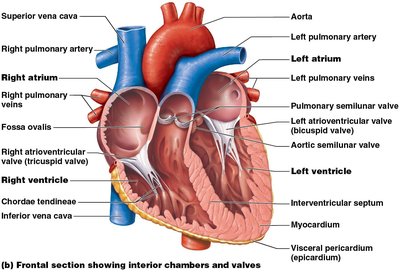
Chambers and Associated Great Vessels
Heart Chambers
The heart has four chambers:
Atria (right and left): Superior receiving chambers; blood enters under low pressure from veins.
Ventricles (right and left): Inferior discharging chambers; thick-walled pumps that propel blood into circulation.
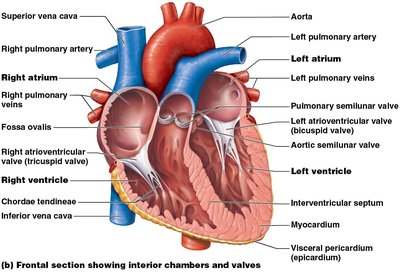
Septum and Circuits
Interatrial Septum: Separates the two atria.
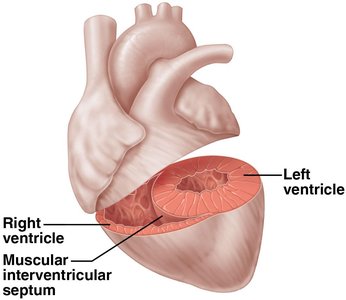
Interventricular Septum: Separates the two ventricles.
Double Pump: Right side pumps to the lungs (pulmonary circuit), left side pumps to the body (systemic circuit).
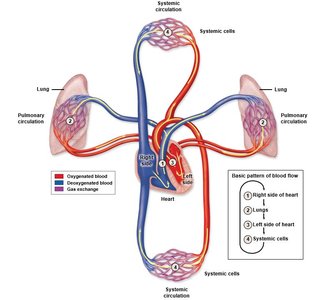
Pulmonary and Systemic Circulation
Pulmonary Circulation: Right side pumps oxygen-poor blood to the lungs via pulmonary arteries; oxygen-rich blood returns via pulmonary veins.
Systemic Circulation: Left side pumps oxygen-rich blood to the body via the aorta; oxygen-poor blood returns via the venae cavae.
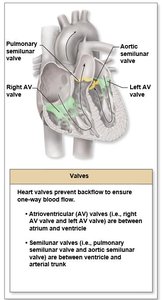
Heart Valves
Types and Functions
Heart valves ensure unidirectional blood flow and prevent backflow.
Atrioventricular (AV) Valves: Between atria and ventricles (right: tricuspid, left: bicuspid/mitral).
Semilunar Valves: Between ventricles and arteries (pulmonary and aortic semilunar valves).
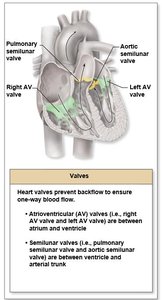
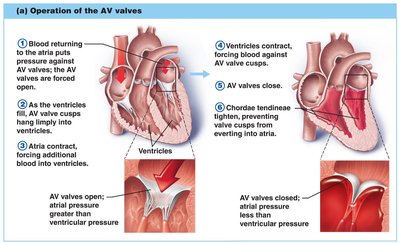
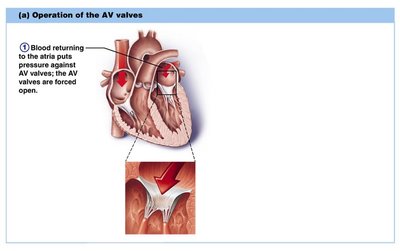
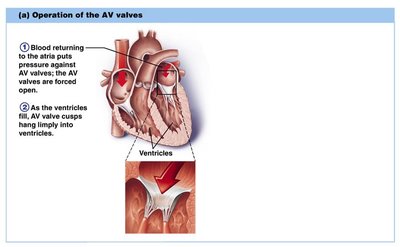
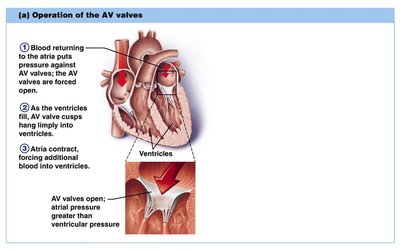
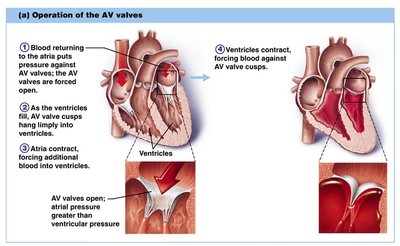
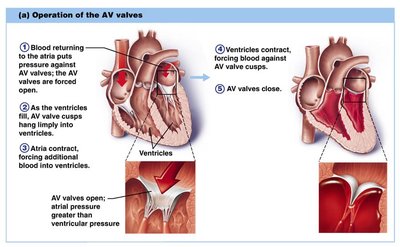
Valve Operation
AV Valves: Open during relaxation, closed during contraction; chordae tendineae anchor cusps.
Semilunar Valves: Closed during relaxation, open during contraction.
Valves open and close in response to pressure changes.
Cardiac Circulation
Coronary Arteries and Veins
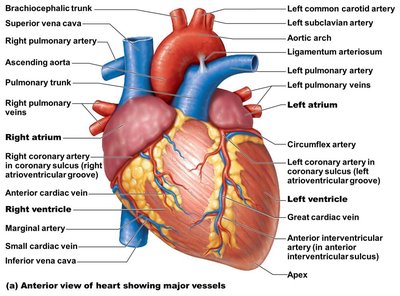
The heart has its own blood supply via the coronary arteries and veins.
Coronary Arteries: Branch from the aorta to supply the heart muscle.
Cardiac Veins: Drain deoxygenated blood from the myocardium into the coronary sinus, which empties into the right atrium.
Clinical Views
Pericarditis: Inflammation of the pericardium, can lead to cardiac tamponade.
Angina Pectoris: Chest pain due to reduced blood flow in coronary arteries.
Myocardial Infarction (Heart Attack): Complete blockage of a coronary artery, leading to tissue death.
Physiology of the Heart
Intrinsic Conduction System
The heart's intrinsic conduction system (nodal system) coordinates the heartbeat, ensuring efficient pumping.
Sinoatrial (SA) Node: Pacemaker, initiates heartbeat.
Atrioventricular (AV) Node: Delays impulse, allowing atria to contract before ventricles.
AV Bundle (Bundle of His), Bundle Branches, Purkinje Fibers: Spread impulse through ventricles.
Cardiac Cycle and Heart Sounds
The cardiac cycle is one complete heartbeat, consisting of systole (contraction) and diastole (relaxation). Heart sounds are produced by valve closures: "lub" (AV valves) and "dup" (semilunar valves).
Cardiac Output
Cardiac Output (CO): Amount of blood pumped by each ventricle per minute.
Formula:
Example Calculation:
Regulation of Stroke Volume and Heart Rate
Starling’s Law: The more cardiac muscle is stretched, the stronger the contraction (preload).
Factors Affecting Heart Rate: Neural (ANS), hormones, ions, age, gender, exercise, temperature.
Blood Vessels
Types and Structure
Blood vessels form a closed system for blood transport. They are classified as arteries, veins, and capillaries.
Arteries: Carry blood away from the heart; thick, elastic walls.
Veins: Return blood to the heart; thinner walls, larger lumen, valves to prevent backflow.
Capillaries: Microscopic vessels for exchange; one cell layer thick.
Blood Vessel Wall Layers
Tunica Intima: Endothelium, reduces friction.
Tunica Media: Smooth muscle and elastic tissue, controls vessel diameter.
Tunica Externa: Fibrous connective tissue, supports and protects.
Capillary Beds and Microcirculation
Capillary beds allow for exchange between blood and tissues. Precapillary sphincters regulate blood flow through the beds.
Gross Anatomy of Blood Vessels
Major Arteries and Veins
Aorta: Largest artery, branches into systemic arteries.
Venae Cavae: Superior and inferior, return blood to the right atrium.
Major Branches: Include coronary, carotid, subclavian, renal, and iliac arteries and veins.
Special Circulations
Cerebral Arterial Circle (Circle of Willis): Provides collateral blood flow to the brain.
Hepatic Portal Circulation: Blood from digestive organs passes through the liver before entering systemic circulation.
Physiology of Circulation
Vital Signs and Blood Pressure
Vital Signs: Pulse, blood pressure, respiratory rate, body temperature.
Blood Pressure (BP): Force exerted by blood against vessel walls; measured as systolic/diastolic (e.g., 120/80 mm Hg).
Formula: (Peripheral Resistance)
Factors Affecting Blood Pressure
Neural: Sympathetic nervous system increases BP via vasoconstriction.
Renal: Kidneys regulate blood volume and pressure via water and sodium balance.
Temperature: Heat causes vasodilation; cold causes vasoconstriction.
Chemicals: Epinephrine increases BP; diet low in salt, saturated fats, and cholesterol helps prevent hypertension.
Capillary Exchange and Fluid Movements
Exchange Mechanisms: Oxygen and nutrients move from blood to tissues; wastes move from tissues to blood.
Fluid Movement: Blood pressure forces fluid out at the arterial end; osmotic pressure draws fluid in at the venous end.
Pressure | Arterial End | Venous End |
|---|---|---|
Blood Pressure | High | Low |
Osmotic Pressure | Low | High |
Net Fluid Movement | Out of capillary | Into capillary |
