 Back
BackThe Cardiovascular System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Cardiovascular System
Overview and Functions
The cardiovascular system is a closed system composed of the heart and blood vessels. Its primary function is to deliver oxygen and nutrients to cells and tissues while removing carbon dioxide and other waste products. The heart acts as a pump, and the blood vessels serve as conduits for blood flow throughout the body.
Delivers oxygen and nutrients to cells and tissues
Removes carbon dioxide and metabolic wastes
Structure of the Heart
Location and Orientation
The heart is located in the thorax, between the lungs in the inferior mediastinum. It is about the size of a human fist (approximately 14 cm x 9 cm). The pointed apex is directed toward the left hip, while the base points toward the right shoulder.
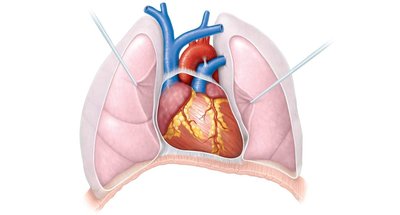
Coverings and Walls of the Heart
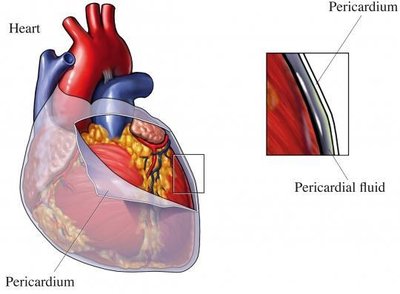
The heart is enclosed by the pericardium, a double-walled sac that protects and anchors the heart. The pericardium consists of:
Fibrous pericardium: Outer, tough, and loose layer
Serous pericardium: Inner, double-layered membrane (parietal and visceral layers)
Pericardial cavity: Space between layers, filled with serous fluid to reduce friction
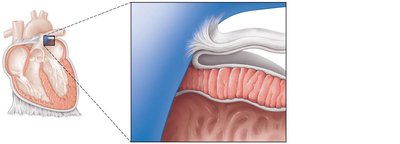
The heart wall has three layers:
Epicardium (visceral pericardium): Outer connective tissue layer
Myocardium: Middle layer, composed of cardiac muscle
Endocardium: Inner endothelial lining
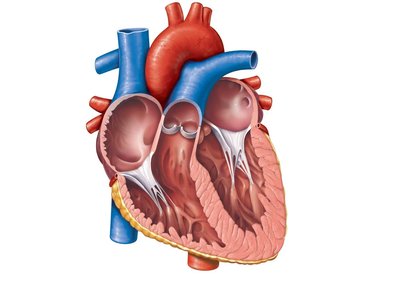
Chambers and Associated Great Vessels
Heart Chambers
The heart has four chambers:
Atria (right and left): Receiving chambers
Ventricles (right and left): Discharging chambers
The interventricular septum separates the two ventricles, and the interatrial septum separates the two atria.
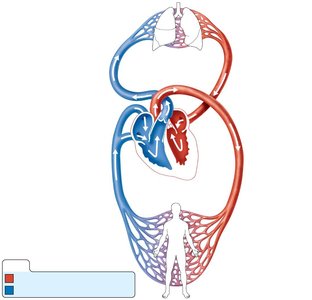
Pulmonary and Systemic Circulation
The heart functions as a double pump:
Pulmonary circulation: Right side pumps oxygen-poor blood to the lungs and returns oxygen-rich blood to the left side.
Systemic circulation: Left side pumps oxygen-rich blood to the body and returns oxygen-poor blood to the right side.
Heart Valves
Types and Functions
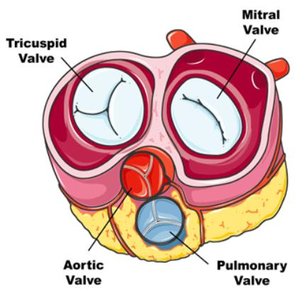
Heart valves ensure unidirectional blood flow and prevent backflow. There are four main valves:
Atrioventricular (AV) valves: Between atria and ventricles
Tricuspid valve: Right side
Bicuspid (mitral) valve: Left side
Semilunar valves: Between ventricles and arteries
Pulmonary semilunar valve
Aortic semilunar valve
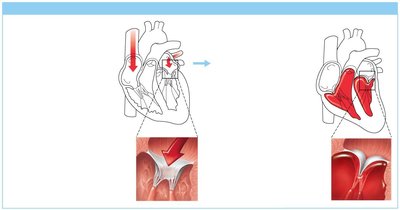
Valve Operation
AV valves are anchored by chordae tendineae and open during relaxation, closing during ventricular contraction. Semilunar valves open during ventricular contraction and close during relaxation, responding to pressure changes.
Blood Flow Through the Heart
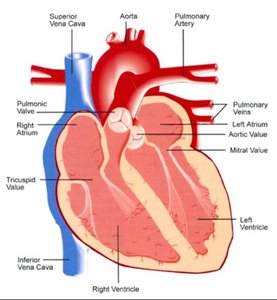
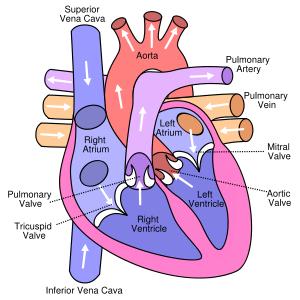
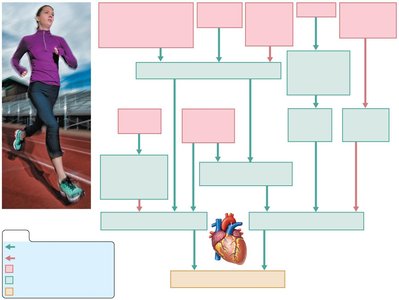
Pathway of Blood
Blood enters the right atrium via the superior and inferior venae cavae.
Passes through the tricuspid valve to the right ventricle.
Exits through the pulmonary semilunar valve into the pulmonary trunk and arteries to the lungs.
Oxygenated blood returns via pulmonary veins to the left atrium.
Passes through the bicuspid valve to the left ventricle.
Exits through the aortic semilunar valve into the aorta and systemic circulation.
Intrinsic Conduction System
Setting the Basic Rhythm
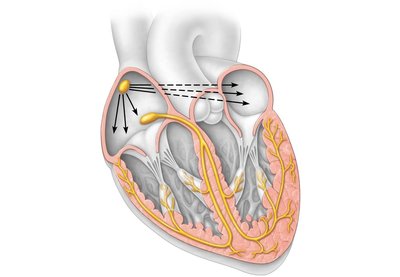
The heart's intrinsic conduction system (nodal system) coordinates the heartbeat. Key components include:
Sinoatrial (SA) node: Pacemaker, initiates heartbeat
Atrioventricular (AV) node: Junction of atria and ventricles
AV bundle (bundle of His): In interventricular septum
Bundle branches: In interventricular septum
Purkinje fibers: Spread within ventricle walls
Heart Contractions
The SA node initiates the impulse, which spreads to the AV node, then through the AV bundle, bundle branches, and Purkinje fibers, resulting in coordinated contraction of the atria and ventricles.
Tachycardia: Rapid heart rate (>100 bpm)
Bradycardia: Slow heart rate (<60 bpm)
Fibrillation: Uncoordinated, rapid contractions
Cardiac Cycle and Heart Sounds
Phases of the Cardiac Cycle
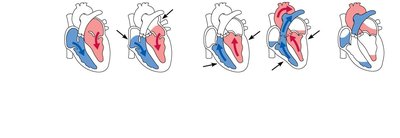
The cardiac cycle consists of one complete heartbeat, including systole (contraction) and diastole (relaxation). The cycle lasts about 0.8 seconds at a normal heart rate of 75 bpm.
Mid-to-late diastole: Ventricles fill passively, AV valves open
Ventricular systole: Ventricles contract, AV valves close ("lub" sound), semilunar valves open
Early diastole: Semilunar valves close ("dup" sound), ventricles relax
Cardiac Output and Regulation
Cardiac Output (CO)
Cardiac output is the amount of blood pumped by each ventricle in one minute. It is calculated as:
HR: Heart rate (beats per minute)
SV: Stroke volume (ml/beat)
Example: If HR = 75 bpm and SV = 70 ml/beat, then ml/min.
Regulation of Heart Rate
Neural controls: Sympathetic (increases HR), parasympathetic (decreases HR)
Hormones and ions: Epinephrine, thyroxine, calcium, potassium
Physical factors: Age, gender, exercise, body temperature
Blood Vessels and Circulation
Types of Blood Vessels
Arteries: Carry blood away from the heart
Arterioles: Small branches of arteries
Capillaries: Sites of exchange between blood and tissues
Venules: Collect blood from capillaries
Veins: Return blood to the heart
Microscopic Anatomy of Blood Vessels
Blood vessels (except capillaries) have three layers:
Tunica intima: Endothelial lining
Tunica media: Smooth muscle and elastic tissue
Tunica externa: Fibrous connective tissue
Structural Differences
Arteries: Thicker tunica media, higher pressure
Veins: Thinner walls, larger lumen, valves to prevent backflow
Capillaries: One cell layer thick for exchange
Capillary Beds
Capillary beds consist of vascular shunts and true capillaries. Precapillary sphincters regulate blood flow through the beds, allowing exchange with tissues or bypassing the area as needed.
Blood Pressure
Definition and Measurement
Blood pressure is the force exerted by blood against vessel walls. It is measured in large arteries and expressed as systolic over diastolic pressure (e.g., 120/80 mm Hg).
Systolic pressure: Peak during ventricular contraction
Diastolic pressure: Lowest during ventricular relaxation
Blood Pressure Gradient
Blood flows along a pressure gradient, highest in arteries and lowest in veins. This gradient is essential for continuous blood flow.
Factors Affecting Blood Pressure
Blood pressure is determined by cardiac output and peripheral resistance:
Neural factors: Sympathetic nervous system (vasoconstriction increases BP)
Renal factors: Kidneys regulate blood volume and release renin
Temperature: Heat causes vasodilation, cold causes vasoconstriction
Chemicals: Epinephrine increases BP
Diet: Low salt, fat, and cholesterol can prevent hypertension
Blood Pressure Variations
Normal range: 140–110 mm Hg systolic, 80–70 mm Hg diastolic
Hypotension: Systolic below 100 mm Hg
Hypertension: Sustained pressure of 140/90 mm Hg or higher
Developmental Aspects and Homeostatic Imbalances
Development
Heart develops as a simple tube and becomes four-chambered by week 7 of embryonic development
Congenital heart defects are a major cause of infant mortality from congenital problems
Age-Related Changes
Weakening of venous valves
Varicose veins
Progressive arteriosclerosis
Hypertension due to loss of vessel elasticity
Coronary artery disease from fatty, calcified deposits
Healthy lifestyle choices, such as a balanced diet, regular exercise, and avoiding smoking, can help maintain cardiovascular health and reduce the risk of disease.
