 Back
BackThe Cardiovascular System: The Heart – Structure, Function, and Regulation
Study Guide - Smart Notes

The Cardiovascular System: The Heart
Overview of the Cardiovascular System
The cardiovascular system is responsible for the continuous circulation of blood throughout the body, delivering nutrients and removing wastes. It consists of the heart, a muscular pump, and a network of blood vessels.
Heart: Muscular organ that pumps blood into vessels.
Blood Vessels: Arteries, veins, and capillaries that transport blood to and from body tissues.
Functions: Delivers nutrients, hormones, and electrolytes; removes metabolic and nitrogenous wastes, and carbon dioxide.
Heart Anatomy and Location
The heart is a four-chambered organ located in the mediastinum of the thoracic cavity. It is about the size of a fist and weighs less than 1 pound. Two-thirds of its mass lies to the left of the body midline, with the broad base pointing toward the right shoulder and the apex toward the left hip.
Apical Impulse: The tapping felt when the heart contracts, caused by the apex touching the chest wall, typically at the 5th intercostal space.
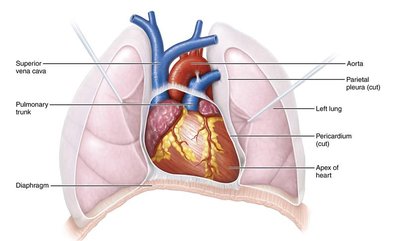
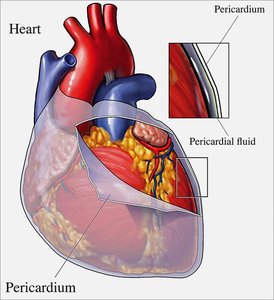
Heart Wall and Pericardium
The heart is enclosed in a double-walled sac called the pericardium, which protects and anchors the heart while preventing overfilling. The heart wall itself is composed of three layers, each with distinct functions.
Fibrous Pericardium: Tough, dense irregular connective tissue; protects, anchors, and prevents overfilling.
Serous Pericardium: Two layers (parietal and visceral/epicardium) with a pericardial cavity containing serous fluid to reduce friction.
Epicardium: Outermost layer, same as visceral serous pericardium.
Myocardium: Middle layer, composed of cardiac muscle cells; responsible for contraction.
Endocardium: Innermost layer, lines chambers and valves; reduces friction between blood and heart tissue.
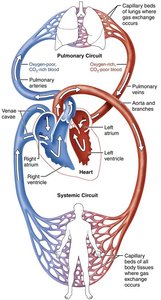
Heart Chambers and Circuits
The heart consists of four chambers: two atria (upper) and two ventricles (lower). It acts as a double pump, with the right side serving the pulmonary circuit (to the lungs) and the left side serving the systemic circuit (to the body).
Right Side (Pulmonary Pump): Pumps deoxygenated blood to the lungs.
Left Side (Systemic Pump): Pumps oxygenated blood to the body; has a thicker myocardium due to higher resistance.
Heart Valves and Blood Flow
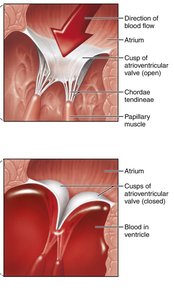
Heart valves ensure unidirectional blood flow through the heart. There are four main valves: two atrioventricular (AV) valves and two semilunar (SL) valves.
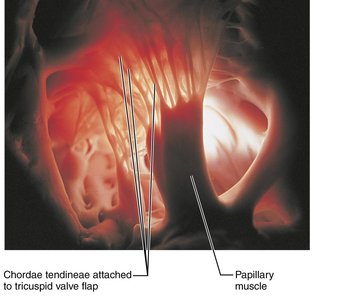
AV Valves: Tricuspid (right) and bicuspid/mitral (left); prevent backflow into atria during ventricular contraction.
Chordae Tendineae: Collagen cords that anchor AV valves to papillary muscles, preventing valve prolapse.
SL Valves: Aortic (left) and pulmonary (right); prevent backflow into ventricles after contraction.
Coronary Circulation
The heart muscle requires its own blood supply, provided by the coronary arteries. Blockage of these arteries can lead to angina pectoris or myocardial infarction (heart attack).
Coronary Arteries: Left and right arteries branch from the aorta and supply the myocardium.
Cardiac Veins: Drain deoxygenated blood from the myocardium into the coronary sinus, which empties into the right atrium.
Cardiac Muscle and Electrical Activity
Cardiac muscle cells are striated, branched, and connected by intercalated discs containing gap junctions and desmosomes. The heart's electrical activity is coordinated by pacemaker cells and the conduction system.
Pacemaker Cells: Autorhythmic cells that generate spontaneous action potentials (e.g., SA node).
Conduction Pathway: SA node → AV node → AV bundle → bundle branches → Purkinje fibers.
Action Potentials: Pacemaker cells have unstable resting potentials; contractile cells have a plateau phase due to Ca2+ influx.
The Cardiac Cycle
The cardiac cycle describes the sequence of mechanical events during one heartbeat, including systole (contraction) and diastole (relaxation).
Ventricular Filling: AV valves open, blood flows into ventricles.
Isovolumetric Contraction: All valves closed, ventricles contract, pressure rises.
Ventricular Ejection: SL valves open, blood ejected into arteries.
Isovolumetric Relaxation: All valves closed, ventricles relax.
Regulation of Cardiac Output
Cardiac output (CO) is the amount of blood pumped by each ventricle per minute. It is regulated by heart rate (HR) and stroke volume (SV).
Formula:
Stroke Volume (SV): (End Diastolic Volume minus End Systolic Volume)
Ejection Fraction:
Regulatory Factors: Preload (stretch), afterload (resistance), and contractility (force of contraction).
Common Heart Defects and Disorders
Pericarditis: Inflammation of the pericardium, causing pain and friction.
Cardiac Tamponade: Fluid accumulation compresses the heart, requiring drainage.
Valve Disorders: Incompetent or prolapsed valves cause backflow and inefficient pumping.
Arrhythmias: Abnormal heart rhythms, including tachycardia, fibrillation, and heart block.
Congestive Heart Failure: Inability of the heart to maintain adequate circulation, leading to pulmonary or peripheral congestion.
