 Back
BackThe Cardiovascular System: The Heart – Structure, Function, and Physiology
Study Guide - Smart Notes

The Cardiovascular System: The Heart
Location and Basic Structure of the Heart
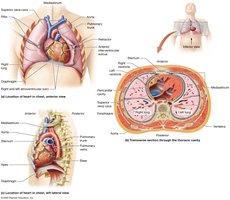
The heart is a muscular organ responsible for pumping blood throughout the body. It is located in the mediastinum, a subdivision of the thoracic cavity, and sits slightly to the left within the pericardial cavity. The heart is cone-shaped, with its apex pointing toward the left hip and its base facing the posterior rib cage. It is about the size of a fist and weighs between 250–350 grams.
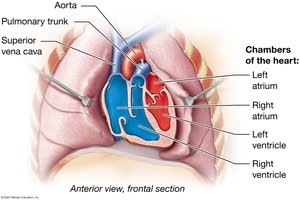
Chambers: The heart consists of four hollow chambers: the right and left atria (superior) and the right and left ventricles (inferior).
Major Sulci: The atrioventricular sulcus separates the atria from the ventricles, while the interventricular sulcus separates the right and left ventricles.
Functions of the Heart
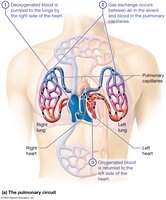
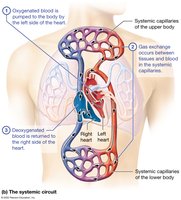
The heart functions as two pumps that propel blood through two distinct circuits:
Pulmonary Circuit: The right side pumps deoxygenated blood to the lungs for gas exchange (low-pressure circuit).
Systemic Circuit: The left side pumps oxygenated blood to the rest of the body (high-pressure circuit).
Homeostasis: The heart helps maintain blood pressure and acts as an endocrine organ by releasing atrial natriuretic peptide (ANP), which lowers blood pressure by reducing sodium and water retention.
The Pericardium, Heart Wall, and Heart Skeleton
The Pericardium
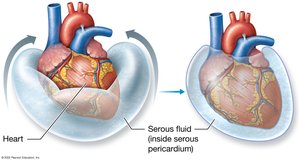
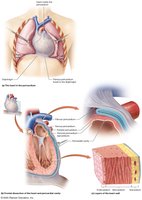
The pericardium is a double-layered membranous sac that surrounds the heart, providing protection and reducing friction during heartbeats.
Fibrous Pericardium: Tough outer layer that anchors the heart to surrounding structures.
Serous Pericardium: Thin inner layer, consisting of the parietal pericardium (outer) and visceral pericardium (epicardium, inner).
Pericardial Cavity: Space between the layers, filled with serous fluid for lubrication.
Heart Wall and Heart Skeleton
Epicardium: Outermost layer, also known as the visceral pericardium.
Myocardium: Thick middle layer composed of cardiac muscle cells (myocytes) arranged in a spiral pattern.
Fibrous Skeleton: Dense irregular connective tissue that provides structural support and electrical insulation.
Endocardium: Innermost layer made of endothelial cells and connective tissue, forming a barrier to regulate the chemical environment of the myocardium.
The Great Vessels, Chambers, and Valves of the Heart
The Great Vessels
Veins: Superior and inferior venae cavae (drain into right atrium), pulmonary veins (drain into left atrium).
Arteries: Pulmonary trunk (from right ventricle to lungs), aorta (from left ventricle to body).
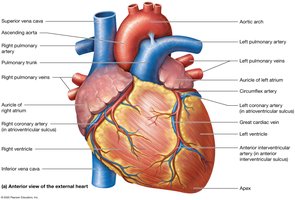
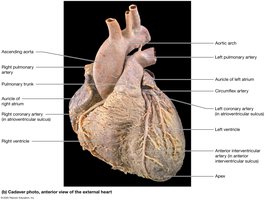
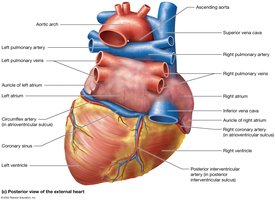
Chambers of the Heart
Atria: Right atrium (large, thin-walled, anterior), left atrium (smaller, thicker-walled, posterior). Both have auricles for expansion.
Ventricles: Right ventricle (wider, thinner walls), left ventricle (thicker walls, pumps against higher resistance).
Internal Features: Pectinate muscles (right atrium), trabeculae carneae (ventricles), papillary muscles and chordae tendineae (anchor AV valves).
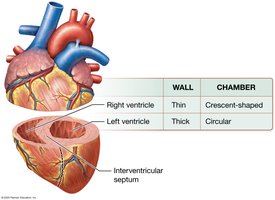
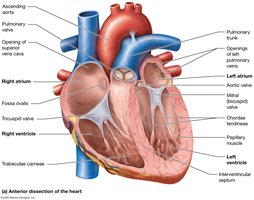
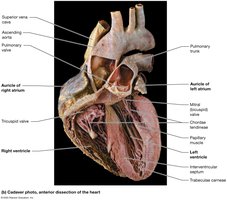
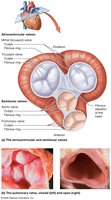
Valves of the Heart
Atrioventricular (AV) Valves: Tricuspid (right), bicuspid/mitral (left); prevent backflow into atria, supported by chordae tendineae and papillary muscles.
Semilunar (SL) Valves: Pulmonary (right ventricle to pulmonary trunk), aortic (left ventricle to aorta); prevent backflow into ventricles.
Coronary Circulation
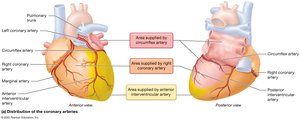
The coronary circulation supplies the heart muscle (myocardium) with oxygen and nutrients and removes waste products.
Coronary Arteries: Right and left coronary arteries branch from the ascending aorta. The right coronary artery gives rise to the marginal and posterior interventricular arteries; the left branches into the anterior interventricular (LAD) and circumflex arteries.
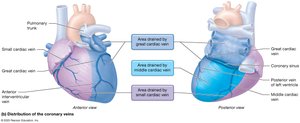
Coronary Veins: Great, small, and middle cardiac veins drain into the coronary sinus, which empties into the right atrium.
Anastomoses: Alternate routes for blood flow, important if a vessel becomes blocked.
Cardiac Muscle Tissue Anatomy and Electrophysiology
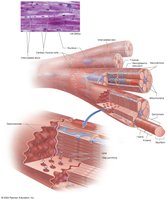
Histology of Cardiac Muscle Tissue
Striations: Cardiac muscle cells have striations due to the arrangement of contractile proteins.
Intercalated Discs: Specialized connections with desmosomes and gap junctions, allowing rapid spread of electrical impulses (functional syncytium).
Ion Channels: Voltage-gated sodium, calcium, and potassium channels, as well as HCN channels in pacemaker cells.
Cardiac Electrophysiology: Pacemaker Cells and the Cardiac Conduction System
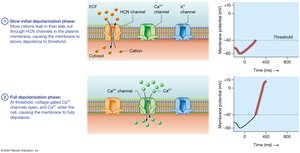
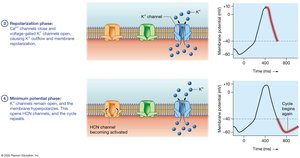
Pacemaker Cells: Generate spontaneous action potentials, setting the heart's rhythm (autorhythmicity).
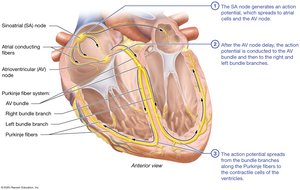
Conduction System: Includes the sinoatrial (SA) node, atrioventricular (AV) node, and Purkinje fiber system (AV bundle, bundle branches, terminal branches).
Sinus Rhythm: Normal rhythm set by the SA node.
Cardiac Electrophysiology: Contractile Cells
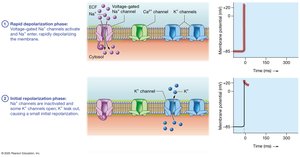
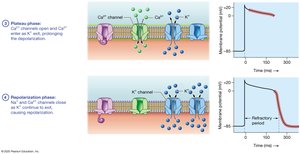
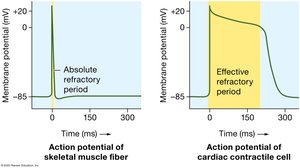
Action Potentials: Rapid depolarization (Na+ influx), initial repolarization (K+ outflow), plateau phase (Ca2+ influx balances K+ outflow), repolarization (K+ outflow).
Plateau Phase: Prolongs action potential, prevents tetany, and allows for effective refractory period.
The Electrocardiogram (ECG/EKG)
P Wave: Atrial depolarization.
QRS Complex: Ventricular depolarization (and atrial repolarization, which is masked).
T Wave: Ventricular repolarization.
Intervals and Segments: R-R (heart rate), P-R (SA to AV node conduction), Q-T (ventricular action potentials), S-T (ventricular plateau phase).
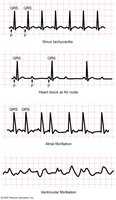
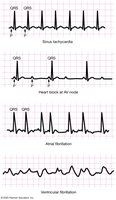
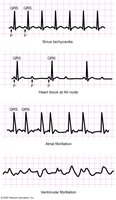
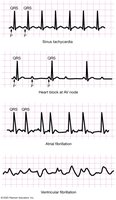
Dysrhythmias
Bradycardia: Heart rate < 60 bpm.
Tachycardia: Heart rate > 100 bpm.
Heart Block: Conduction delays, often at the AV node.
Fibrillation: Disorganized electrical activity; atrial fibrillation is less dangerous than ventricular fibrillation, which is life-threatening.




Mechanical Physiology of the Heart: The Cardiac Cycle
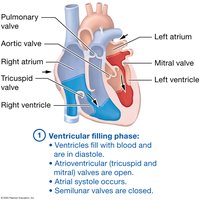
Cardiac Cycle Phases
Ventricular Filling: Ventricles fill with blood during diastole; AV valves open, SL valves closed.
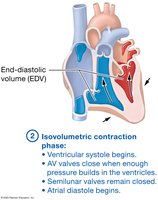
Isovolumetric Contraction: Ventricular systole begins; AV valves close, SL valves still closed.
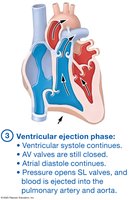
Ventricular Ejection: Ventricular systole continues; SL valves open, blood ejected.
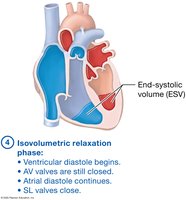
Isovolumetric Relaxation: Ventricular diastole begins; all valves closed.
Heart Sounds
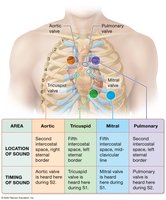
S1 (Lub): Closure of AV valves.
S2 (Dub): Closure of SL valves.
Heart Murmurs: Abnormal sounds due to turbulent blood flow, often from defective valves.

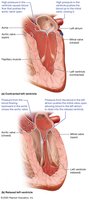
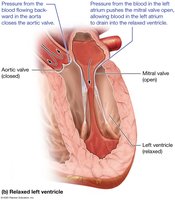
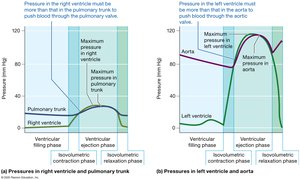
Pressure Changes and Valve Function
Pressure changes in the ventricles drive the opening and closing of heart valves, ensuring unidirectional blood flow.
The left ventricle generates higher pressures than the right due to the greater resistance in the systemic circuit.
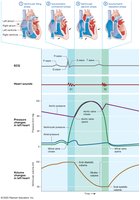
Cardiac Cycle Diagram (Wiggers Diagram)
Integrates electrical events (ECG), heart sounds, pressure changes, and volume changes in the left ventricle during the cardiac cycle.
Cardiac Output and Its Regulation
Definitions and Formulas
Heart Rate (HR): Number of beats per minute (bpm).
Stroke Volume (SV): Amount of blood pumped by one ventricle in one beat.
Cardiac Output (CO): Amount of blood pumped by each ventricle in one minute.
Formulas:
Stroke Volume:
Cardiac Output:
Factors Influencing Stroke Volume
Preload: Degree of stretch of cardiac muscle cells before contraction (Frank-Starling Law).
Contractility: Intrinsic ability of cardiac muscle to contract; influenced by inotropic agents.
Afterload: Pressure the ventricles must overcome to eject blood.
Factors Influencing Heart Rate
Chronotropic Agents: Factors that alter the rate of SA node firing (e.g., sympathetic/parasympathetic stimulation, hormones, temperature).
Regulation of Cardiac Output
Nervous System: Sympathetic nerves increase HR and contractility; parasympathetic nerves (vagus) decrease HR.
Endocrine System: Epinephrine, norepinephrine, thyroid hormone, glucagon, aldosterone, antidiuretic hormone, and ANP all influence cardiac output.
Other Factors: Electrolyte concentrations, body temperature, age, and physical fitness.
Heart Failure
Definition: Any condition that reduces the heart’s ability to function as a pump.
Left Ventricular Failure: Leads to pulmonary congestion and edema.
Right Ventricular Failure: Leads to peripheral edema (systemic congestion).
Treatment: Lifestyle modifications, medications, and surgery to increase cardiac output and reduce congestion.
Summary Table: Key Heart Structures and Functions
Structure | Function |
|---|---|
Right Atrium | Receives deoxygenated blood from body |
Left Atrium | Receives oxygenated blood from lungs |
Right Ventricle | Pumps deoxygenated blood to lungs |
Left Ventricle | Pumps oxygenated blood to body |
Tricuspid Valve | Prevents backflow into right atrium |
Bicuspid (Mitral) Valve | Prevents backflow into left atrium |
Pulmonary Valve | Prevents backflow into right ventricle |
Aortic Valve | Prevents backflow into left ventricle |
Additional info: This guide integrates and expands upon the provided lecture slides, including definitions, examples, and clinical context for a comprehensive understanding of the heart's anatomy and physiology.
