 Back
BackThe Cardiovascular System: The Heart – Structured Study Notes
Study Guide - Smart Notes

The Cardiovascular System: The Heart
Location and Basic Structure of the Heart
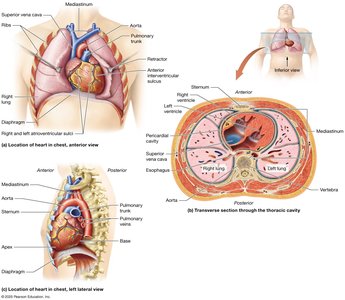
The heart is a muscular organ that functions as a pump to deliver blood throughout the body. It is part of the cardiovascular system, which also includes blood vessels and blood. The heart is located in the chest, slightly to the left, within the mediastinum—a subdivision of the thoracic cavity that contains the great blood vessels, trachea, and esophagus. The heart itself sits in the pericardial cavity, a subcavity of the mediastinum.
Shape and Size: Cone-shaped, with the apex pointing toward the left hip and the base facing the posterior rib cage. It is about the size of a fist and weighs 250–350 grams.
Chambers: Four hollow chambers: right and left atria (superior), right and left ventricles (inferior).
External Features: The atrioventricular sulcus marks the boundary between atria and ventricles; the interventricular sulcus separates the right and left ventricles.
Chambers and Blood Flow
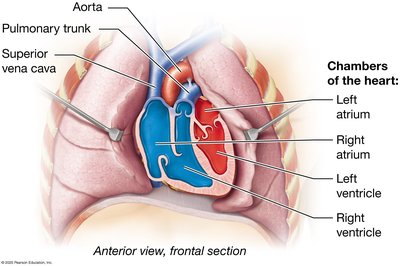
The heart's chambers receive and pump blood in a coordinated manner. Atria receive blood from veins, while ventricles pump blood into arteries. The main veins and arteries are called the great vessels.
Right Atrium: Receives deoxygenated blood from the superior and inferior venae cavae.
Left Atrium: Receives oxygenated blood from the pulmonary veins.
Right Ventricle: Pumps deoxygenated blood into the pulmonary trunk.
Left Ventricle: Pumps oxygenated blood into the aorta.
Functions of the Heart: Pulmonary and Systemic Circuits
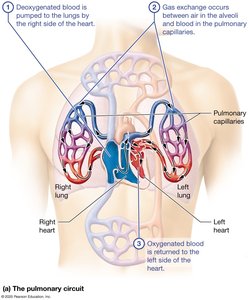
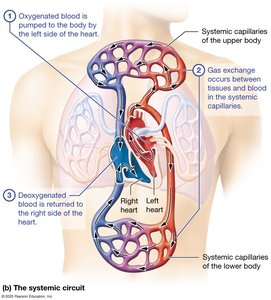
The heart operates two main circuits: the pulmonary circuit (right side) and the systemic circuit (left side). These circuits ensure oxygenation of blood and distribution to tissues.
Pulmonary Circuit: Right side pumps deoxygenated blood to the lungs for gas exchange; oxygenated blood returns to the left side.
Systemic Circuit: Left side pumps oxygenated blood to the body; deoxygenated blood returns to the right side.
Pressure: Pulmonary circuit is low-pressure; systemic circuit is high-pressure.
Pericardium, Heart Wall, and Heart Skeleton
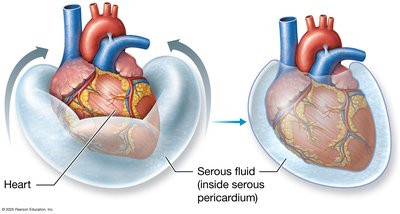
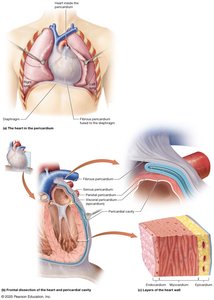
The heart is surrounded by the pericardium, a membranous sac with two layers: the tough fibrous pericardium and the thin serous pericardium. The heart wall consists of three layers: epicardium (visceral pericardium), myocardium (cardiac muscle), and endocardium (endothelial cells).
Fibrous Pericardium: Anchors the heart and limits its expansion.
Serous Pericardium: Parietal layer encases the heart; visceral layer (epicardium) adheres to the heart.
Pericardial Cavity: Contains serous fluid to reduce friction.
Myocardium: Thickest layer, composed of cardiac muscle cells arranged spirally.
Fibrous Skeleton: Dense connective tissue providing structural support and electrical insulation.
Endocardium: Deepest layer, regulates electrolyte and chemical concentrations.
Blood Flow Through the Heart
Blood flows through the heart in a specific sequence, passing through the chambers and valves to ensure unidirectional movement.
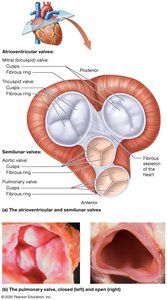
Atrioventricular Valves (AV): Tricuspid (right) and bicuspid/mitral (left) valves prevent backflow into the atria.
Semilunar Valves (SL): Pulmonary (right) and aortic (left) valves prevent backflow into the ventricles.
Chordae Tendineae: Attach AV valve cusps to papillary muscles, preventing eversion.
Coronary Circulation
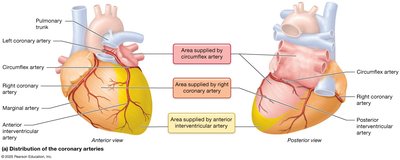
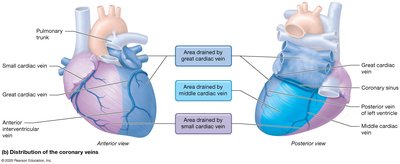
The heart receives its own blood supply via the coronary arteries and is drained by coronary veins. This circulation is essential for the heart's function.
Coronary Arteries: Right and left coronary arteries branch from the ascending aorta; major branches include the marginal, posterior interventricular, anterior interventricular (LAD), and circumflex arteries.
Coronary Veins: Great, small, and middle cardiac veins drain into the coronary sinus, which empties into the right atrium.
Anastomoses: Alternate routes for blood flow, providing collateral circulation.
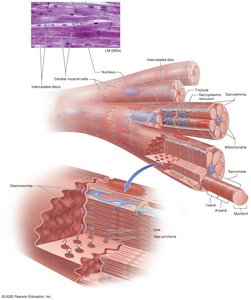
Cardiac Muscle Tissue Anatomy and Electrophysiology
Cardiac muscle cells are striated, short, branched, and interconnected by intercalated discs containing desmosomes and gap junctions. The heart is autorhythmic, meaning it can generate its own rhythm without nervous input.
Pacemaker Cells: Generate spontaneous action potentials, setting the heart's pace.
Contractile Cells: Make up most of the heart muscle and respond to pacemaker cell signals.
Functional Syncytium: Heart contracts as a unit due to gap junctions.
Cardiac Conduction System
The cardiac conduction system consists of specialized pacemaker cells that coordinate the heart's electrical activity.
Sinoatrial (SA) Node: Primary pacemaker, located in the right atrium; fastest rate of depolarization.
Atrioventricular (AV) Node: Slower pacemaker, located near the tricuspid valve.
Purkinje Fiber System: Includes AV bundle, bundle branches, and terminal branches; conducts action potentials rapidly to ventricles.
Cardiac Action Potentials
Cardiac muscle cells generate action potentials with distinct phases, including rapid depolarization, plateau, and repolarization. The plateau phase is unique to cardiac cells and prevents tetany.
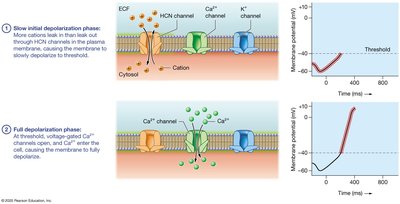
Pacemaker Cell Action Potential: Slow initial depolarization (HCN channels), full depolarization (Ca2+ channels), repolarization (K+ channels), minimum potential phase.
Contractile Cell Action Potential: Rapid depolarization (Na+ channels), initial repolarization, plateau (Ca2+ influx), repolarization (K+ efflux).
The Electrocardiogram (ECG)
An ECG records the electrical activity of the heart, providing information about its structure and function.
P Wave: Atrial depolarization.
QRS Complex: Ventricular depolarization (and atrial repolarization).
T Wave: Ventricular repolarization.
Intervals and Segments: R-R interval (heart rate), P-R interval (depolarization spread), Q-T interval (ventricular action potentials), S-T segment (plateau phase).
Cardiac Cycle and Heart Sounds
The cardiac cycle consists of alternating periods of contraction (systole) and relaxation (diastole) for each chamber. Heart sounds are produced by valve closures.
S1 (Lub): AV valves close.
S2 (Dub): SL valves close.
Phases: Ventricular filling, isovolumetric contraction, ventricular ejection, isovolumetric relaxation.
Cardiac Output and Regulation
Cardiac output (CO) is the amount of blood pumped by the heart per minute. It is determined by heart rate (HR) and stroke volume (SV).
Stroke Volume: SV = EDV – ESV
Cardiac Output: CO = HR × SV
Factors Influencing SV: Preload (stretch), contractility (tension), afterload (back pressure).
Regulation: Nervous system (sympathetic and parasympathetic), endocrine system (hormones), electrolytes, temperature, age, fitness.
Example Equations:
Clinical Connections
Cardiac Tamponade: Excess fluid in the pericardial cavity compresses the heart.
Myocarditis: Inflammation of the myocardium, sometimes due to viral infection (e.g., COVID-19).
Valvular Heart Disease: Insufficient or stenotic valves cause murmurs and may lead to heart enlargement or dysfunction.
Coronary Artery Disease: Plaque buildup leads to myocardial ischemia and infarction (heart attack).
Heart Failure: Reduced pumping ability, leading to pulmonary or peripheral edema.
Summary Table: Heart Chambers and Valves
Chamber | Function | Associated Valve |
|---|---|---|
Right Atrium | Receives deoxygenated blood | Tricuspid (AV) |
Right Ventricle | Pumps blood to lungs | Pulmonary (SL) |
Left Atrium | Receives oxygenated blood | Bicuspid/Mitral (AV) |
Left Ventricle | Pumps blood to body | Aortic (SL) |
Additional info: These notes expand on the original lecture slides by providing definitions, examples, and clinical context for key concepts in cardiac anatomy and physiology. Images are included only where they directly reinforce the explanation of the paragraph.
