 Back
BackThe Cardiovascular System: The Heart – Study Notes
Study Guide - Smart Notes

The Cardiovascular System: The Heart
Introduction to the Heart's Role
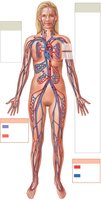
The heart is a muscular organ responsible for pumping blood throughout the body, ensuring the delivery of oxygen and nutrients and the removal of waste products. It operates within two main circuits: the pulmonary circuit (to and from the lungs) and the systemic circuit (to and from the rest of the body).
Beats per day: ~100,000 times
Blood pumped per day: ~8,000 liters
Four chambers: Right atrium, right ventricle, left atrium, left ventricle
Pulmonary circuit: Carries blood to/from lungs
Systemic circuit: Carries blood to/from body tissues
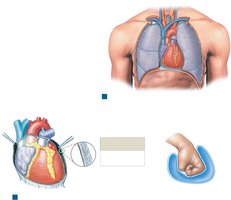
Location and Orientation of the Heart
The heart is located in the mediastinum, behind the sternum, and between the lungs. Its base is superior, where major vessels attach, and its apex points inferiorly and to the left.
Base: Superior end, where great vessels connect
Apex: Inferior, pointed tip
Orientation: Tilted left, with most mass left of midline
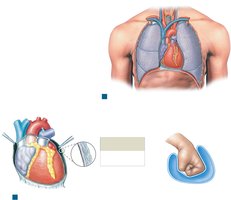
Pericardial Layers of the Heart
The heart is enclosed in the pericardium, a double-layered serous membrane that reduces friction and protects the heart.
Parietal pericardium: Lines inner surface of pericardial sac
Visceral pericardium (epicardium): Covers the heart's surface
Pericardial fluid: Found between layers, reduces friction
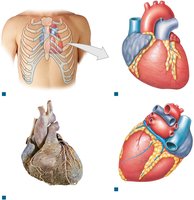
Surface Anatomy of the Heart
The heart's external features include auricles, sulci, and visible vessels. Sulci mark the boundaries between chambers and contain blood vessels and fat.
Auricle: Expandable extension of each atrium
Coronary sulcus: Separates atria from ventricles
Anterior/posterior interventricular sulci: Separate left and right ventricles
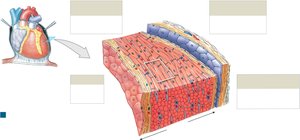
Layers of the Heart Wall
The heart wall consists of three layers, each with distinct structure and function.
Epicardium: Outer layer (visceral pericardium), epithelium + areolar tissue
Myocardium: Middle, muscular layer; contains cardiac muscle, blood vessels, nerves
Endocardium: Inner layer; simple squamous epithelium + areolar tissue, lines chambers and valves
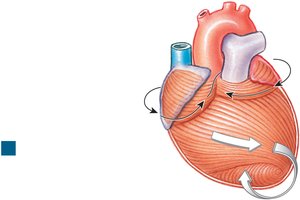
Cardiac Muscle Tissue Arrangement
Cardiac muscle fibers are arranged in spiral and concentric layers, enhancing the heart's pumping efficiency by producing a twisting and squeezing motion during contraction.
Atrial musculature: Bands wrap around atria in a figure-eight pattern
Ventricular musculature: Bands spiral around ventricles
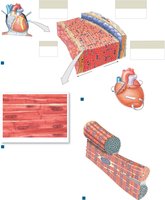
Cardiac Muscle Cells
Cardiac muscle cells are specialized for endurance and coordinated contraction.
Single central nucleus
Intercalated discs: Connect cells, contain desmosomes and gap junctions for electrical and mechanical coupling
Abundant mitochondria: Depend on aerobic respiration
Myofibrils organized into sarcomeres
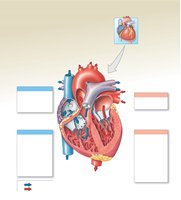
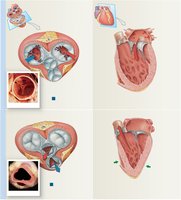
Internal Anatomy and Blood Flow Through the Heart
The heart's internal structure ensures unidirectional blood flow through its four chambers and associated valves.
Right atrium: Receives deoxygenated blood from superior/inferior vena cava and coronary sinus
Right ventricle: Pumps blood to lungs via pulmonary trunk
Left atrium: Receives oxygenated blood from pulmonary veins
Left ventricle: Pumps blood to systemic circuit via aorta
Valves: Atrioventricular (tricuspid, mitral) and semilunar (pulmonary, aortic) valves prevent backflow
Heart Valves and Their Function
Valves ensure one-way flow of blood through the heart, preventing regurgitation.
Tricuspid valve: Right AV valve, three cusps
Mitral (bicuspid) valve: Left AV valve, two cusps
Chordae tendineae: Fibrous cords attaching valve cusps to papillary muscles
Pulmonary and aortic semilunar valves: Prevent backflow into ventricles
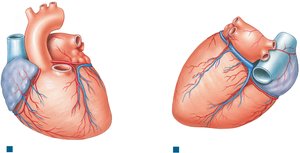
Coronary Circulation
The heart muscle (myocardium) receives its own blood supply via the coronary arteries and veins.
Right coronary artery: Supplies right atrium and parts of both ventricles
Left coronary artery: Supplies left atrium, left ventricle, and interventricular septum
Coronary veins: Drain into coronary sinus, returning blood to right atrium
Anastomoses: Interconnections between arteries provide alternate pathways
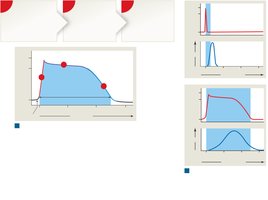
Action Potentials in Cardiac Muscle
Cardiac muscle action potentials are longer than those in skeletal muscle, preventing tetanus and ensuring rhythmic contractions.
Phases: Rapid depolarization (Na+ influx), plateau (Ca2+ influx), repolarization (K+ efflux)
Refractory period: Extended, prevents summation and tetanus
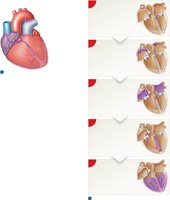
The Conducting System of the Heart
The heart's conducting system coordinates the sequence of cardiac muscle contraction, allowing for automaticity (autorhythmicity).
Sinoatrial (SA) node: Pacemaker, initiates heartbeat
Atrioventricular (AV) node: Delays impulse, ensures atria contract before ventricles
AV bundle (bundle of His), bundle branches, Purkinje fibers: Distribute impulse through ventricles
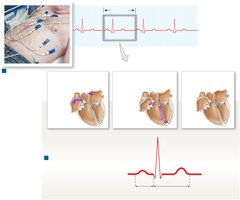
Electrocardiogram (ECG/EKG)
An ECG records the electrical activity of the heart, useful for diagnosing arrhythmias and other cardiac conditions.
P wave: Atrial depolarization
QRS complex: Ventricular depolarization (and atrial repolarization)
T wave: Ventricular repolarization
P-R interval: Start of atrial to start of ventricular depolarization
Q-T interval: Duration of ventricular depolarization and repolarization
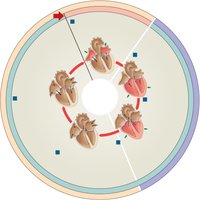
The Cardiac Cycle
The cardiac cycle is the sequence of events in one heartbeat, including periods of contraction (systole) and relaxation (diastole).
Atrial systole: Atria contract, push blood into ventricles
Ventricular systole: Ventricles contract, eject blood into arteries
Diastole: Chambers relax and fill with blood
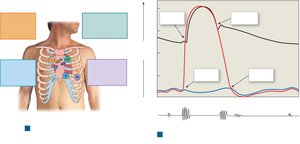
Heart Sounds
Heart sounds are produced by the closing of valves during the cardiac cycle and can be heard with a stethoscope.
S1 ("lubb"): Closure of AV valves
S2 ("dupp"): Closure of semilunar valves
S3, S4: Usually faint, associated with blood flow and atrial contraction
Heart Dynamics: Stroke Volume and Cardiac Output
Cardiac output is the volume of blood ejected by the left ventricle per minute and is a key indicator of cardiovascular health.
Stroke volume (SV): Volume ejected per beat (average ~70 mL)
Heart rate (HR): Beats per minute (normal 60–100 bpm)
Cardiac output (CO):
Regulation: Adjusted by autonomic nervous system, hormones, and venous return
Regulation of Cardiac Function
Cardiac output and heart rate are regulated by neural, hormonal, and intrinsic mechanisms.
Atrial (Bainbridge) reflex: Increases HR in response to increased venous return
Frank-Starling principle: Increased venous return stretches myocardium, increasing SV
Autonomic innervation: Sympathetic (increases HR and contractility), parasympathetic (decreases HR)
Hormones: Epinephrine, norepinephrine, thyroid hormones, and glucagon increase HR and contractility
Summary Table: Key Structures and Functions of the Heart
Structure | Function |
|---|---|
Right Atrium | Receives deoxygenated blood from body |
Right Ventricle | Pumps blood to lungs |
Left Atrium | Receives oxygenated blood from lungs |
Left Ventricle | Pumps blood to systemic circuit |
Tricuspid Valve | Prevents backflow into right atrium |
Mitral Valve | Prevents backflow into left atrium |
Pulmonary Valve | Prevents backflow into right ventricle |
Aortic Valve | Prevents backflow into left ventricle |
Key Equations
Cardiac Output:
Additional info: The above notes integrate foundational concepts from the cardiovascular system, focusing on the heart's anatomy, physiology, and regulatory mechanisms, suitable for introductory college-level anatomy and physiology courses.
