 Back
BackThe Digestive System: Structure and Function
Study Guide - Smart Notes

The Digestive System
Overview and Functions
The digestive system is responsible for breaking down food, absorbing nutrients, and eliminating waste. It consists of the alimentary canal (gastrointestinal tract) and accessory digestive organs. The main functions include ingestion, digestion (mechanical and chemical), absorption, and defecation.
Ingestion: Taking in food through the mouth.
Digestion: Mechanical (chewing, churning, segmentation) and chemical (enzymatic breakdown) processes that convert food into absorbable molecules.
Absorption: Movement of nutrients from the digestive tract into the bloodstream or lymphatic system.
Defecation: Elimination of indigestible substances as feces.
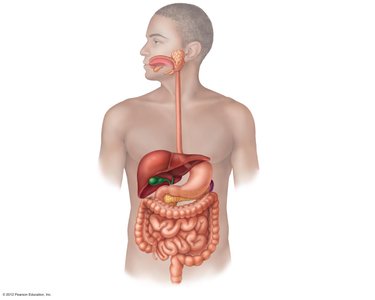
Organs of the Digestive System
Alimentary Canal (GI Tract)
The alimentary canal is a continuous, coiled, hollow tube that includes the mouth, pharynx, esophagus, stomach, small intestine, large intestine, and anus. Its primary roles are ingestion, digestion, absorption, and defecation.
Mouth
Pharynx
Esophagus
Stomach
Small intestine
Large intestine
Anus
Accessory Digestive Organs
Accessory organs assist in the digestive process but are not part of the alimentary canal. They include the tongue, teeth, salivary glands, pancreas, liver, gallbladder, and lymphatic organs (tonsils, appendix).
Histology of the Alimentary Canal
Layers of the Alimentary Canal
The wall of the alimentary canal consists of four main layers, from deep to superficial:
Mucosa: Innermost, moist membrane lining the lumen; consists of surface epithelium, lamina propria (connective tissue), and muscularis interna (thin smooth muscle).
Submucosa: Areolar connective tissue containing blood vessels, nerves, lymphatics, and glands.
Muscularis externa: Smooth muscle responsible for peristalsis and segmentation; has an inner circular and outer longitudinal layer.
Serosa (visceral peritoneum): Outermost layer; secretes serous fluid to reduce friction.
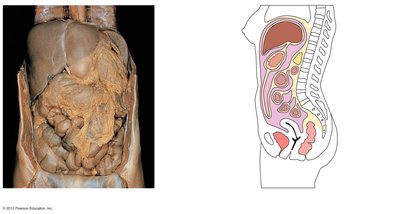
Mesenteries and Peritoneum
The peritoneum is a double-layered serous membrane. Mesenteries are extensions of the peritoneum that anchor organs, store fat, and contain blood vessels, nerves, and lymphatics.
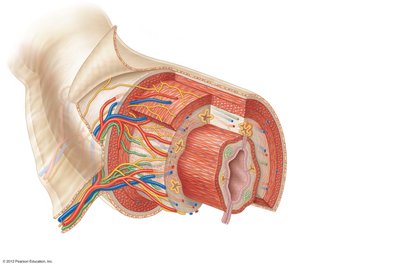
Nerve Plexuses
The alimentary canal contains two major autonomic nerve plexuses: the submucosal and myenteric plexuses. These regulate motility and secretory activity and are collectively called the enteric nervous system or "gut-brain."
The Mouth (Oral Cavity)
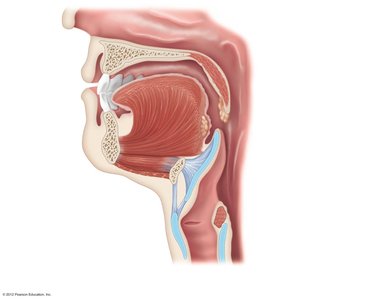
Anatomy of the Mouth
The mouth is the entry point for food and is involved in mechanical digestion (chewing) and chemical digestion (salivary enzymes). Key structures include the lips, cheeks, hard and soft palates, uvula, vestibule, oral cavity proper, and tongue.
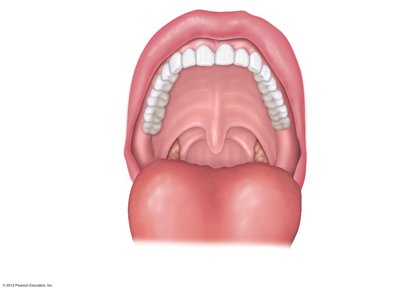
Teeth
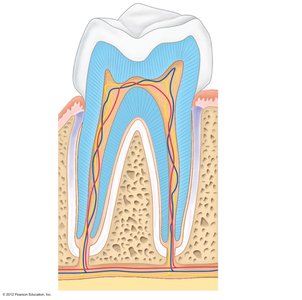
Teeth are essential for mastication (chewing). Humans have two sets: deciduous (baby) teeth and permanent teeth. Types of teeth include incisors (cutting), canines (tearing), premolars (grinding), and molars (grinding).
Crown: Exposed part covered by enamel (hardest substance in the body).
Neck: Region in contact with the gum; connects crown to root.
Root: Anchored in the jawbone; covered by cementum and attached by the periodontal membrane.
Salivary Glands and Saliva
Three pairs of salivary glands (parotid, submandibular, sublingual) secrete saliva, which contains mucin, antibacterial proteins, and salivary amylase (initiates starch digestion). Saliva moistens food and aids in forming a bolus for swallowing.
Pharynx and Esophagus
Pharynx
The pharynx serves as a common passageway for food and air. It consists of the oropharynx and laryngopharynx (the nasopharynx is not part of the digestive system). Food is propelled by peristalsis—alternating contractions of muscle layers.
Deglutition (Swallowing)
Swallowing occurs in two phases:
Buccal phase: Voluntary; food is formed into a bolus and pushed into the pharynx by the tongue.
Pharyngeal-esophageal phase: Involuntary; all passageways except the esophagus are blocked, and peristalsis moves the bolus toward the stomach.
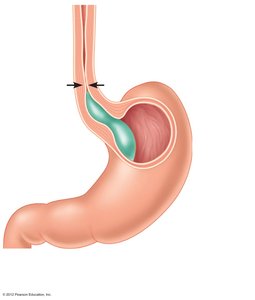
Esophagus
The esophagus is a muscular tube (~10 inches) that conducts food from the pharynx to the stomach via peristalsis. It passes through the diaphragm and ends at the cardioesophageal sphincter.
Stomach
Anatomy of the Stomach
The stomach is a J-shaped organ located on the left side of the abdominal cavity. It has several regions: cardiac, fundus, body, and pylorus. The stomach is bounded by the cardioesophageal and pyloric sphincters. Internal folds called rugae allow expansion.
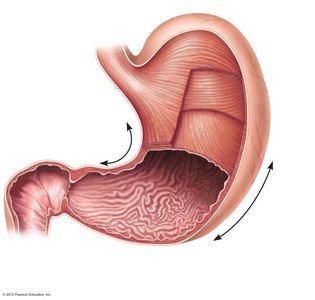
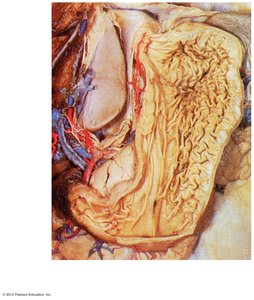
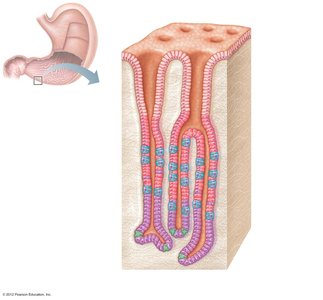
Stomach Wall and Mucosa
The stomach wall contains three layers of smooth muscle (including an oblique layer for churning). The mucosa is lined with simple columnar epithelium and contains gastric glands that secrete gastric juice.
Mucous neck cells: Produce alkaline mucus.
Chief cells: Secrete pepsinogen (inactive enzyme).
Parietal cells: Secrete hydrochloric acid (HCl).
Enteroendocrine cells: Secrete gastrin (hormone).
Stomach Physiology
The stomach acts as a temporary storage tank, mixes and churns food, and begins protein digestion. Gastric juice secretion is regulated by neural and hormonal factors (e.g., gastrin). HCl activates pepsinogen to pepsin for protein digestion and creates an acidic environment hostile to microbes.
Protein digestion: Pepsin digests proteins; rennin digests milk protein in infants.
Absorption: Only alcohol, aspirin, and some drugs are absorbed in the stomach.
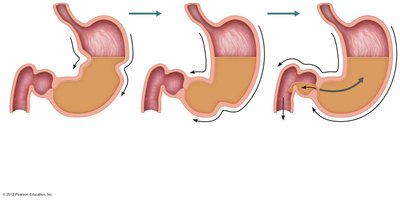
Propulsion in the Stomach
Peristaltic waves mix and propel food. The pylorus meters chyme into the small intestine (about 3 mL at a time). The stomach empties in 4–6 hours.
Small Intestine
Anatomy and Subdivisions
The small intestine is the major digestive organ and the site of most chemical digestion and nutrient absorption. It extends from the pyloric sphincter to the ileocecal valve and is divided into three regions: duodenum, jejunum, and ileum.
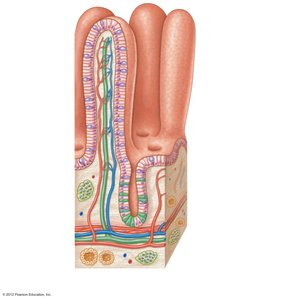
Surface Area Adaptations
Three structural modifications increase the surface area for absorption:
Circular folds (plicae circulares): Deep folds of mucosa and submucosa.
Villi: Fingerlike projections of the mucosa.
Microvilli: Tiny projections of the plasma membrane (brush border).
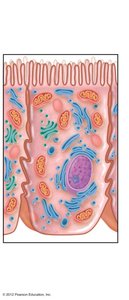
Chemical Digestion in the Small Intestine
Most chemical digestion occurs in the small intestine, aided by enzymes from the pancreas and bile from the liver. Pancreatic juice contains enzymes for all food categories and bicarbonate to neutralize acidic chyme. Bile emulsifies fats for digestion and absorption.
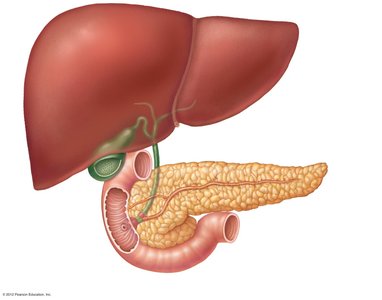
Absorption in the Small Intestine
Most nutrients are absorbed into the blood by active transport, while lipids are absorbed into lymph by diffusion. Water is absorbed along the length of the small intestine. Absorbed substances are transported to the liver via the hepatic portal vein or lymphatic system.
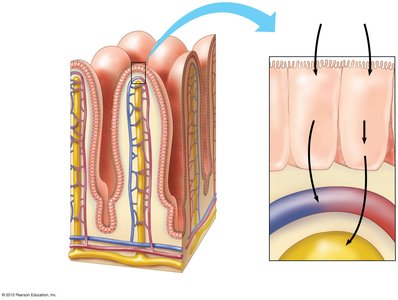
Liver, Gallbladder, and Pancreas
Liver
The liver is the largest gland in the body and has many metabolic and regulatory functions. It produces bile, processes nutrient-laden blood, stores glycogen, synthesizes proteins, and detoxifies substances.
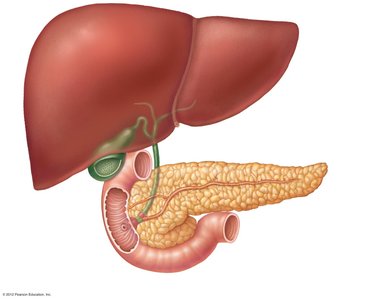
Bile and Gallbladder
Bile is produced by the liver and stored in the gallbladder. It contains bile salts, pigments, cholesterol, phospholipids, and electrolytes. Bile emulsifies fats, aiding in their digestion and absorption. The gallbladder releases bile into the duodenum during digestion of fatty foods.
Pancreas
The pancreas secretes pancreatic juice into the duodenum. This juice contains digestive enzymes for all food categories and bicarbonate to neutralize stomach acid. Its secretion is regulated by the vagus nerve and hormones (secretin and cholecystokinin).
Metabolic Functions of the Liver
Carbohydrate Metabolism
Glycogenesis: Formation of glycogen from glucose.
Glycogenolysis: Breakdown of glycogen to release glucose.
Gluconeogenesis: Formation of glucose from non-carbohydrate sources (fats and proteins).
Lipid and Cholesterol Metabolism
Fats are oxidized for energy or converted to other compounds.
Cholesterol is used for steroid hormone and vitamin D synthesis and as a membrane component.
Lipoproteins transport cholesterol and fats: LDLs (to cells, "bad"), HDLs (to liver, "good").
Large Intestine
Anatomy and Subdivisions
The large intestine is wider but shorter than the small intestine. It extends from the ileocecal valve to the anus and includes the cecum, appendix, colon (ascending, transverse, descending, sigmoid), rectum, and anal canal.
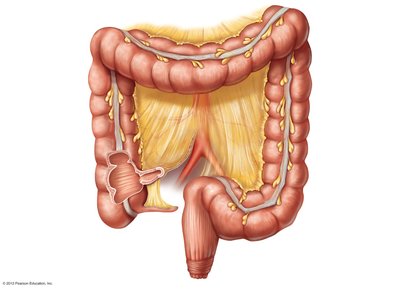
Functions of the Large Intestine
Absorbs remaining water and vitamins K and B produced by resident bacteria.
Forms and eliminates feces (undigested food, pigments, mucus, bacteria, water).
Propulsion is sluggish; mass movements occur a few times daily, and defecation is triggered by the presence of feces in the rectum.
Summary Table: Digestion and Absorption of Major Nutrients
Foodstuff | Enzyme(s) & Source | Site of Action |
|---|---|---|
Carbohydrates | Salivary amylase (mouth), Pancreatic amylase (small intestine), Brush border enzymes (small intestine) | Mouth, Small intestine |
Proteins | Pepsin (stomach), Pancreatic enzymes (trypsin, chymotrypsin, carboxypeptidase), Brush border enzymes | Stomach, Small intestine |
Fats | Bile salts (emulsification), Pancreatic lipase | Small intestine |
Absorption: Monosaccharides and amino acids enter blood capillaries; fatty acids and monoglycerides enter lacteals (lymphatics).
