 Back
BackThe Digestive System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Digestive System
Overview of the Digestive System
The digestive system is responsible for the breakdown and absorption of nutrients necessary for the body’s function. It consists of the alimentary canal (digestive tract) and accessory organs that aid in digestion through secretion and mechanical processing.
Digestive Tract (Alimentary Canal): A continuous tube from the mouth to the anus, including the oral cavity, pharynx, esophagus, stomach, small intestine, and large intestine.
Accessory Organs: Glands and organs such as the salivary glands, liver, gallbladder, and pancreas that secrete fluids and enzymes into the digestive tract.
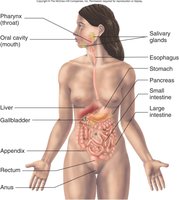
Anatomy of the Digestive Tract
Regions of the Digestive Tract
The digestive tract is divided into several regions, each with specialized functions:
Mouth (Oral Cavity): Involved in ingestion, mastication, and initial digestion.
Pharynx and Esophagus: Transport food from the mouth to the stomach.
Stomach: Mechanically and chemically digests food, forming chyme.
Small Intestine (Duodenum, Jejunum, Ileum): Major site for digestion and absorption.
Large Intestine (Cecum, Colon, Rectum, Anal Canal): Absorbs water and forms feces.
Anus: Terminal opening for elimination of waste.
Functions of the Digestive System
Major Functions
The digestive system performs several essential functions to process food and eliminate waste:
Ingestion: Introduction of food into the mouth.
Mastication: Chewing to increase surface area for chemical digestion.
Propulsion: Movement of food through the tract via swallowing (deglutition) and peristalsis.
Mixing: Segmental contractions mix food with digestive secretions.
Secretion: Release of mucus, water, bile, and enzymes to lubricate, digest, and protect.
Digestion: Mechanical and chemical breakdown of food.
Absorption: Movement of nutrients from the tract into blood or lymph.
Elimination: Removal of indigestible substances as feces.
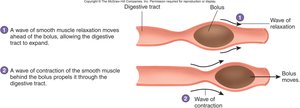
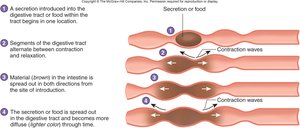
Histology of the Digestive Tract
Layers of the Digestive Tract
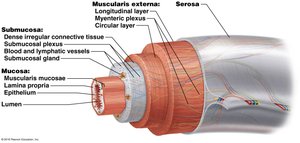
The wall of the digestive tract is composed of four main layers, each with distinct functions:
Mucosa: Innermost layer; includes epithelium (stratified squamous or simple columnar), lamina propria (loose connective tissue), and muscularis mucosae (smooth muscle).
Submucosa: Dense connective tissue containing blood vessels, nerves (submucosal plexus), and glands.
Muscularis: Two or three layers of smooth muscle (circular and longitudinal); contains the myenteric plexus for motility control.
Serosa/Adventitia: Outermost layer; serosa is visceral peritoneum, adventitia blends with surrounding tissues.
Regulation of the Digestive System
Nervous and Chemical Regulation
Digestive processes are regulated by both nervous and chemical mechanisms:
Nervous Regulation: Local (enteric nervous system) and general (central nervous system) control peristalsis, secretion, and blood flow. Parasympathetic input stimulates, while sympathetic input inhibits digestive activity.
Chemical Regulation: Hormones (e.g., gastrin, secretin) and paracrine chemicals (e.g., histamine) modulate secretion and motility.
The Peritoneum and Mesenteries
Structure and Function
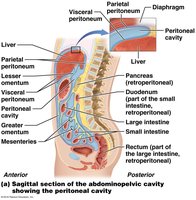
The peritoneum is a serous membrane lining the abdominal cavity and covering abdominal organs. It is divided into:
Visceral Peritoneum: Covers organs.
Parietal Peritoneum: Lines the abdominal wall.
Retroperitoneal Organs: Located behind the peritoneum (e.g., kidneys, pancreas).
Mesenteries: Double layers of peritoneum that support organs and provide routes for vessels and nerves.
Omenta: Greater and lesser omentum connect the stomach to other organs.
Oral Cavity and Associated Structures
Oral Cavity, Lips, Cheeks, and Palate
The oral cavity is the entry point for food and is involved in mechanical and chemical digestion:
Lips and Cheeks: Aid in mastication and speech; contain muscles and fat pads for movement and structure.
Palate: Hard palate (bone-supported) and soft palate (muscle and connective tissue); separates oral and nasal cavities.
Palatine Tonsils: Lymphatic tissue in the lateral walls of the fauces.
Tongue
The tongue is a muscular organ essential for manipulating food, speech, and swallowing:
Intrinsic Muscles: Change the shape of the tongue.
Extrinsic Muscles: Move the tongue in various directions.
Papillae: Projections on the anterior tongue, some with taste buds.
Lingual Tonsil: Lymphoid tissue on the posterior tongue.
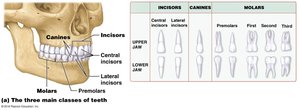
Teeth
Teeth are specialized for cutting, tearing, and grinding food:
Types: Incisors, canines, premolars, and molars.
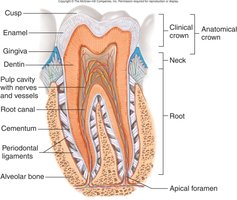
Structure: Crown (enamel-covered), neck, root (embedded in alveolar bone), dentin, pulp cavity, and periodontal ligaments.
Salivary Glands and Saliva
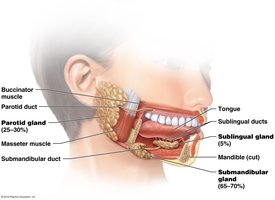
Major Salivary Glands
Three pairs of major salivary glands secrete saliva into the oral cavity:
Parotid Glands: Largest, serous secretion, located anterior to the ear.
Submandibular Glands: Mixed secretion, located beneath the mandible.
Sublingual Glands: Primarily mucous secretion, located under the tongue.
Functions of Saliva
Lubrication: Moistens food and oral cavity.
Digestion: Contains salivary amylase for starch breakdown.
Protection: Contains lysozyme, IgA, and bicarbonate ions to prevent infection and neutralize acids.
Swallowing (Deglutition)
Phases of Swallowing
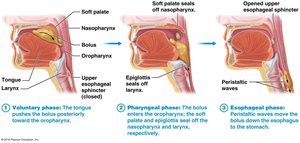
Swallowing is a complex process involving voluntary and reflex actions:
Voluntary Phase: Tongue pushes bolus to the pharynx.
Pharyngeal Phase: Reflex; soft palate and epiglottis close off nasal and respiratory passages, pharyngeal muscles push bolus into esophagus.
Esophageal Phase: Reflex; peristalsis moves bolus to the stomach.
Stomach
Anatomy and Histology
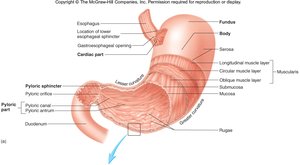
The stomach is a muscular organ that stores, mixes, and digests food:
Regions: Cardiac, fundus, body, pyloric (antrum and canal).
Sphincters: Cardiac (lower esophageal) and pyloric sphincters regulate entry and exit of food.
Layers: Mucosa (with rugae), submucosa, muscularis (three layers), serosa.
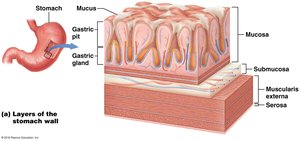
Gastric Glands and Secretions
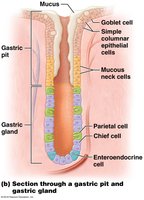
Surface Mucous Cells: Secrete protective mucus.
Parietal Cells: Secrete hydrochloric acid (HCl) and intrinsic factor.
Chief Cells: Secrete pepsinogen (converted to pepsin for protein digestion).
Endocrine Cells: Secrete hormones such as gastrin and somatostatin.
Phases of Gastric Secretion
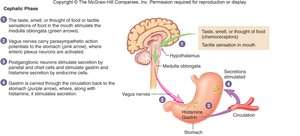
Cephalic Phase: Initiated by sight, smell, or thought of food; mediated by the vagus nerve and stimulates gastric secretion.
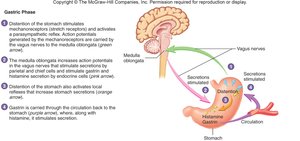
Gastric Phase: Triggered by stomach distention and food presence; enhances secretion via local and central reflexes.
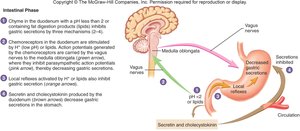
Intestinal Phase: Initiated by chyme entering the duodenum; inhibits gastric secretion via neural and hormonal mechanisms (secretin, cholecystokinin).
Small Intestine
Structure and Function
The small intestine is the primary site for digestion and absorption of nutrients:
Divisions: Duodenum, jejunum, ileum.
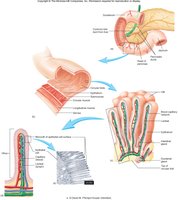
Surface Area Modifications: Plicae circulares, villi, and microvilli increase absorptive surface area.
Cell Types: Absorptive cells, goblet cells, endocrine cells, granular (Paneth) cells.
Motility and Secretions
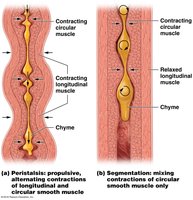
Segmental Contractions: Mix chyme with digestive juices.
Peristalsis: Propels chyme toward the large intestine.
Secretions: Mucus, digestive enzymes (disaccharidases, peptidases, nucleases), and hormones.
Large Intestine
Structure and Function
The large intestine absorbs water and electrolytes, forms and stores feces, and houses beneficial bacteria:
Regions: Cecum (with appendix), colon (ascending, transverse, descending, sigmoid), rectum, anal canal.
Movements: Mass movements and local reflexes move fecal material toward the rectum.
Secretions: Mucus for protection; bacterial action produces vitamins and gases.
Digestion and Absorption
Carbohydrates, Lipids, and Proteins
Carbohydrates: Broken down by amylases and disaccharidases into monosaccharides for absorption.
Lipids: Emulsified by bile salts, digested by lipases, absorbed as micelles and chylomicrons.
Proteins: Digested by pepsin and proteolytic enzymes into amino acids, dipeptides, and tripeptides for absorption.
Water and Ions
Water: Absorbed or secreted based on osmotic gradients.
Ions: Actively transported across the intestinal wall.
Summary Table: Hormones and Paracrines in Digestive Regulation
Hormone | Stimulus for Production | Effects |
|---|---|---|
Gastrin | Partially digested proteins, vagal stimulation | Increases acid secretion by parietal cells |
Histamine | Food in stomach | Increases acid secretion by parietal cells |
Somatostatin | Decreasing stomach pH | Decreases acid secretion by parietal cells |
Secretin | Partially digested proteins and lipids in duodenum | Inhibits gastric motility, stimulates bicarbonate secretion from pancreas |
Cholecystokinin (CCK) | Partially digested proteins and lipids in duodenum | Stimulates gallbladder contraction, pancreatic enzyme secretion |
