 Back
BackThe Digestive System: Structure, Function, and Regulation 22.1
Study Guide - Smart Notes

The Digestive System
Overview of the Digestive System
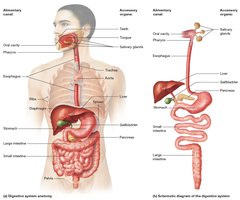
The digestive system is a complex set of organs responsible for breaking down food into nutrients that can be absorbed and utilized by the body. It extends from the head to the abdominopelvic cavity and is composed of the alimentary canal and accessory organs.
Alimentary canal (GI tract): A continuous tube through which food passes, including the oral cavity, pharynx, esophagus, stomach, small intestine, and large intestine.
Accessory organs: Structures that assist in digestion but are not part of the alimentary canal, such as teeth, tongue, salivary glands, liver, gallbladder, and pancreas.
Key Functions:
Breakdown of food into nutrients
Fluid, electrolyte, and acid-base homeostasis
Ingestion of vitamins and minerals
Hormone production
Excretion of metabolic wastes
Basic Digestive Processes
The digestive system performs several essential processes to ensure proper digestion and absorption:
Ingestion: Intake of food and water, primarily through the mouth.
Secretion: Release of substances (mucus, enzymes, acids, hormones) by digestive glands to aid digestion.
Propulsion: Movement of food through the digestive tract, mainly by peristalsis (rhythmic smooth muscle contractions).
Aided by mucus secreted by multiple organs.
Digestion: Breakdown of food by mechanical (chewing, mixing) and chemical (enzymatic) means (breaking down chemical bonds).
Absorption: Movement of nutrients, water, electrolytes, and vitamins into the blood or lymphatic vessels.
Defecation: Elimination of indigestible substances and metabolic wastes as feces.
Specialized form of propulsion.
Organization of Abdominopelvic Digestive Organs
Peritoneal Membranes and Mesenteries
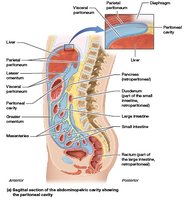
Digestive organs in the abdominopelvic cavity are supported and protected by serous membranes called peritoneal membranes:
Parietal peritoneum: Lines the inner surface of the body wall.
Visceral peritoneum (serosa): Covers the external surfaces of digestive organs.
Peritoneal cavity: Space between the two layers, filled with serous fluid.
Intraperitoneal: Organs located entirely within the peritoneal cavity.
Retroperitoneal: Abdominal organs that are partly or completely outside the peritoneal cavity
Pancreas ; both retroperitoneal and intraperitoneal (lateral section)
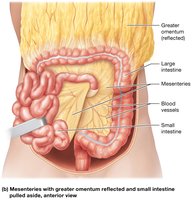
Mesenteries: Folds of visceral peritoneum that support, bind, and stabilize digestive organs, and house blood vessels, nerves, and lymphatics.
Mesocolon: mesentery attached to much of the large intestine
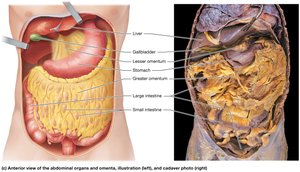
Greater omentum: Large, four-layered mesentery extending from the stomach to the pelvis.
Covers the abdominal organs like an apron
Lesser omentum: Smaller mesentery connecting the stomach to the liver.
Both the greater and lesser omenta generally accumulate adipose tissue between their folds.
Clinical Note: Peritonitis
Peritonitis is inflammation of the peritoneum, often caused by leakage of blood or organ contents into the peritoneal cavity due to trauma or infection.
Symptoms include abdominal pain and rebound tenderness.
Treatment involves antibiotics and sometimes surgery; untreated, it can be fatal.
Blood Supply and Innervation
Splanchnic circulation: Blood supply to digestive organs via branches of the abdominal aorta (celiac trunk, superior and inferior mesenteric arteries).
Venous drainage: Blood from digestive organs drains into the hepatic portal vein, then to the liver, and finally to the inferior vena cava via hepatic veins.
Nerve supply: Digestive organs are innervated by the autonomic nervous system (sympathetic and parasympathetic) and the enteric nervous system (ENS).
The celiac plexus, the superior mesenteric plexus, and the inferior mesenteric plexus.
Nerve plexuses: Celiac, superior mesenteric, and inferior mesenteric plexuses; submucosal and myenteric plexuses (ENS) regulate secretion and motility.
Nerve plexuses of the ENS work with the sympathetic and parasympathetic nervous systems to control the secretions and movement of the alimentary canal.
Histology of the Alimentary Canal
General Structure
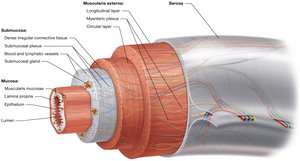
The alimentary canal is composed of four main layers, each with specialized functions:
Mucosa: Innermost layer, consisting of epithelium, lamina propria (loose connective tissue), and muscularis mucosae (smooth muscle- two thin sheets). Contains goblet cells for mucus secretion and regenerative cells for repair.
The epithelium from the stomach to the end of the large intestine is simple columnar epithelium with numerous mucus-secreting cells such as goblet cells.
The mucus secreted by goblet cells are protecting the epithelium and the underlying tissues from ingested food and chemicals secreted by digestive organs
The regenerative cells allow the mucosa to replace epithelial cells as they are damaged or sloughed off in the alimentary canal
The lamina propria houses blood and lymphatic vessels, glands, and mucosa-associated lymphatic tissue (MALT)
The two layers of the muscularis mucosae are arranged in different directions—the inner is circular and the outer is longitudinal
The arrangement allows propulsion.
Submucosa: Dense irregular connective tissue with blood and lymphatic vessels, glands, and the submucosal (Meissner's) plexus.
Each plexus regulates secretion from and blood flow to its area of the alimentary canal.
Muscularis externa: Two layers of smooth muscle (inner circular, outer longitudinal) regulated by the myenteric (Auerbach's) plexus; responsible for peristalsis and mixing and regulating mobility.
Serosa (or adventitia): Outermost layer; serosa is found in organs within the peritoneal cavity (simple squamous epithelium and loose connective tissue), while adventitia (dense irregular connective tissue) is found in organs outside the cavity.
Both structures support digestive organs and anchor them to surrounding structures.
Regulation of Digestive Motility
Nervous and Endocrine Control
Motility (movement) of the alimentary canal is essential for digestion and is regulated by both the nervous and endocrine systems:
Skeletal muscle: Controls motility in the oral cavity, pharynx, upper esophagus, and last portion of the large intestine.
Smooth muscle: Responsible for motility in the rest of the alimentary canal (swallowing, churning, peristalsis, defecation).
Some of these movements propel food through the canal, whereas others mix it as part of mechanical digestion
Autonomic nervous system (ANS): Sympathetic activity inhibits, while parasympathetic activity stimulates digestive motility
(Long reflexes involve the CNS).
Enteric nervous system (ENS): Localized control of motility and secretion (short reflexes).
Local Neurons
Endocrine system: Hormones (often paracrines) produced by digestive organs regulate motility and secretion by binding to target cell receptors.
Example: The hormone gastrin, produced by the stomach, stimulates gastric motility and secretion.
