 Back
BackThe Digestive System: Structure, Function, and Processes
Study Guide - Smart Notes

The Digestive System
Overview of the Digestive System
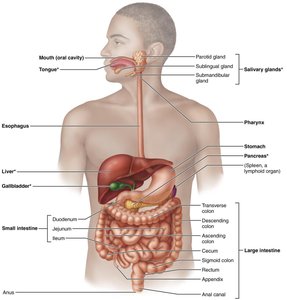
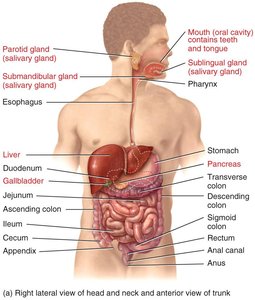
The digestive system is responsible for the breakdown of food, absorption of nutrients, and elimination of waste. It consists of the gastrointestinal (GI) tract and accessory organs that aid in digestion.
GI Tract (Alimentary Canal): Mouth, pharynx, esophagus, stomach, small intestine, large intestine (colon), anus.
Accessory Organs: Teeth, tongue, salivary glands, liver, gallbladder, pancreas.
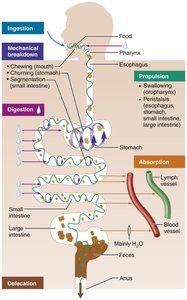
Major Functions of the Digestive System
Ingestion: Taking in food through the mouth.
Mechanical Digestion: Physical breakdown of food (chewing, mixing, churning, segmentation).
Chemical Digestion: Enzymatic breakdown of food into absorbable molecules.
Propulsion: Movement of food along the GI tract (swallowing, peristalsis).
Absorption: Passage of nutrients into blood or lymph.
Defecation: Elimination of indigestible substances as feces.
Anatomy of the Digestive Tract
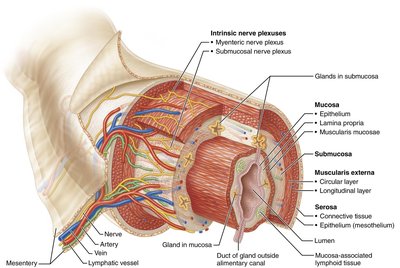
Histological Layers of the GI Tract
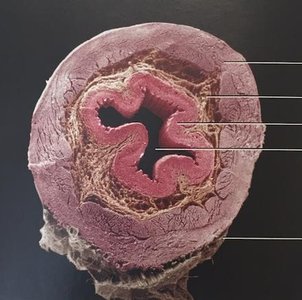
All regions of the GI tract from the lower esophagus to the anal canal share a four-layered structure:
Mucosa: Innermost layer; contains epithelium, lamina propria, and muscularis mucosae.
Submucosa: Connective tissue with blood vessels, nerves, and glands.
Muscularis: Smooth muscle (circular and longitudinal layers) for peristalsis and mixing; in the stomach, an additional oblique layer is present.
Serosa: Outermost layer; visceral peritoneum.
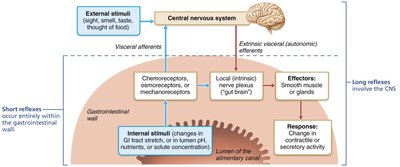
Enteric Nervous System and Autonomic Influence
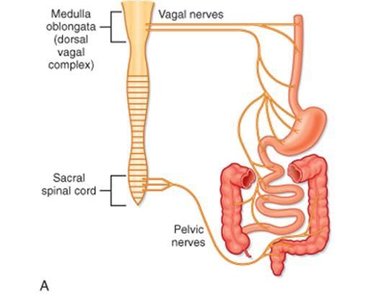
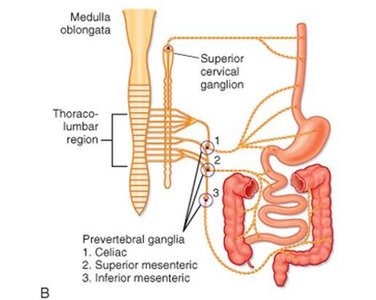
The digestive tract is regulated by the enteric nervous system (ENS), known as the "brain of the gut," and is influenced by the autonomic nervous system (ANS):
Parasympathetic Stimulation: Increases digestive activity (e.g., salivation, peristalsis).
Sympathetic Stimulation: Decreases digestive activity.
Digestive Processes by Region
The Mouth (Oral Cavity)
The mouth is the entry point for food and the site of both mechanical and chemical digestion.
Mechanical Digestion: Mastication (chewing) breaks food into smaller pieces and mixes it with saliva to form a bolus.
Chemical Digestion: Saliva contains enzymes that begin the breakdown of carbohydrates and fats.
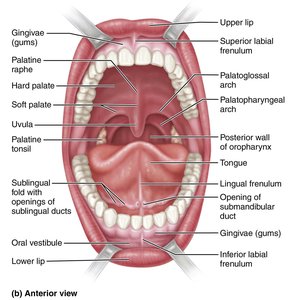
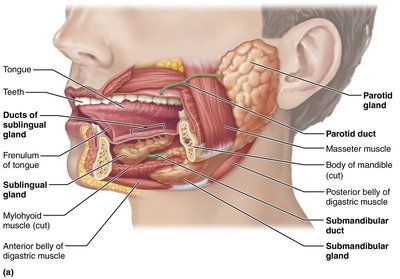
Salivary Enzymes
Salivary Amylase: Begins starch digestion (polysaccharides to smaller sugars).
Lingual Lipase: Begins fat digestion (triglycerides to diglycerides and fatty acids); activated in the acidic environment of the stomach.
Saliva is 99.5% water and 0.5% solutes (ions, enzymes, lysozymes). Salivation is regulated by the ANS: parasympathetic stimulation increases, sympathetic decreases secretion.
The Pharynx and Esophagus
The pharynx serves as a passageway for food from the mouth to the esophagus. The esophagus is a muscular tube that transports food to the stomach via peristalsis.
Upper Esophageal Sphincter: Skeletal muscle, voluntary control.
Lower Esophageal Sphincter (LES): Smooth muscle, involuntary control; prevents reflux of stomach contents.
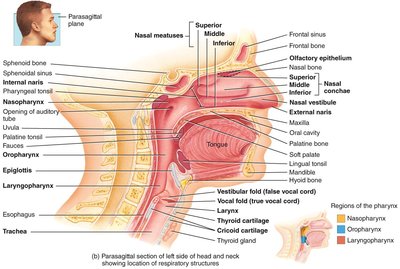
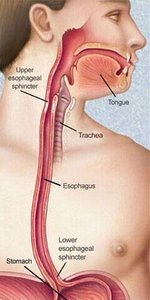
Deglutition (Swallowing)
Oral Phase: Voluntary; tongue pushes bolus into the pharynx.
Pharyngeal Phase: Involuntary; soft palate and epiglottis close off airways, pharyngeal muscles push bolus into esophagus.
Esophageal Phase: Involuntary; peristalsis moves bolus to stomach, LES relaxes to admit bolus.
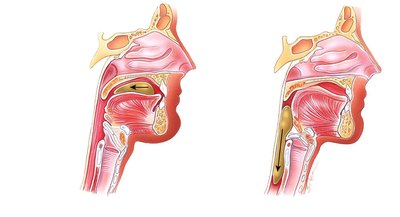
Gastroesophageal Reflux Disease (GERD)
Occurs when the LES fails to close properly, allowing stomach acid to enter the esophagus (heartburn).
Aggravated by certain foods (coffee, chocolate, fatty foods), alcohol, and smoking.

The Stomach
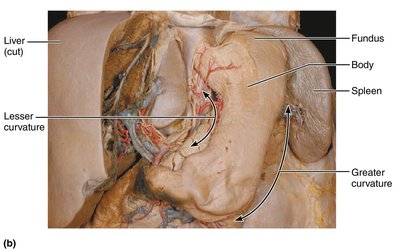
Structure and Function
The stomach stores, mixes, and digests food both mechanically and chemically. It is highly distensible due to rugae (folds) in its mucosa.
Mechanical Digestion: Mixing waves (propulsion and retropulsion) churn food into chyme.
Chemical Digestion: Gastric juice (HCl, pepsin, gastric lipase, intrinsic factor) breaks down proteins and fats.

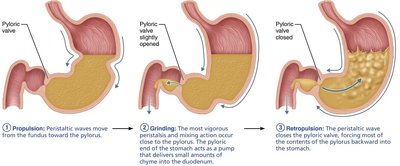
Gastric Glands and Secretions
Parietal Cells: Secrete HCl (activates pepsinogen, kills microbes) and intrinsic factor (vitamin B12 absorption).
Chief Cells: Secrete pepsinogen (converted to pepsin, digests proteins) and gastric lipase (digests fats).
Mucous Cells: Secrete alkaline mucus to protect the stomach lining.
G Cells: Secrete gastrin (stimulates gastric activity).
Absorption in the Stomach
Limited absorption: water, ions, short-chain fatty acids, some drugs (aspirin), and alcohol.
Gastric emptying: Carbohydrates empty fastest, followed by proteins, then fats.
Peptic Ulcer Disease
Caused by Helicobacter pylori infection, which disrupts the mucosal barrier.
Risk factors: NSAIDs, alcohol, smoking, stress (exacerbating factors).
Vomiting (Emesis)
Triggered by stomach irritation, unpleasant stimuli, or drugs.
Controlled by the medulla oblongata; involves contraction of GI muscles, diaphragm, and abdominal muscles.
Prolonged vomiting can cause metabolic alkalosis and dehydration.
The Pancreas
Structure and Function
The pancreas is an accessory organ that secretes digestive enzymes and bicarbonate into the small intestine.
Exocrine Function: Acini cells produce pancreatic juice (enzymes and bicarbonate).
Endocrine Function: Islets of Langerhans secrete hormones (insulin, glucagon).
Pancreatic Juice Composition
Enzymes: Pancreatic amylase (starch), trypsin/chymotrypsin/carboxypeptidase/elastase (proteins), pancreatic lipase (fats), ribonuclease and deoxyribonuclease (nucleic acids).
Bicarbonate (NaHCO3): Neutralizes acidic chyme from the stomach.
Pancreatic Disorders
Pancreatitis: Inflammation due to autodigestion by trypsin; causes include alcohol, gallstones, cystic fibrosis.
Pancreatic Cancer: High mortality, associated with fatty diet, alcohol, genetics, smoking, chronic pancreatitis.
The Liver and Gallbladder
Liver Functions
Metabolic: Carbohydrate, lipid, and protein metabolism; storage of glycogen, vitamins, and minerals.
Secretory: Secretes bile for fat emulsification.
Detoxification: Removes drugs, alcohol, and toxins.
Phagocytosis: Removes old blood cells and pathogens.
Vitamin D Activation: Converts vitamin D to its active form.
Gallbladder Functions
Stores and concentrates bile produced by the liver.
Releases bile into the duodenum in response to cholecystokinin (CCK) after fatty meals.
Bile
Alkaline solution containing water, bile salts, cholesterol, and bile pigments (bilirubin).
Emulsifies fats, aiding in their digestion and absorption.
Bilirubin is a breakdown product of hemoglobin; stercobilin (from bilirubin) gives feces their brown color.
Gallstones
Formed from crystallized cholesterol due to insufficient bile salts or excessive cholesterol.
May block bile flow, causing pain and indigestion, especially after fatty meals.
Treatment: Drugs, shock-wave therapy, or surgical removal (cholecystectomy).
The Small Intestine
Structure and Function
The small intestine is the primary site for digestion and absorption. It is divided into three regions: duodenum, jejunum, and ileum.
Circular folds (plicae circulares): Increase surface area and mix chyme.
Villi and microvilli: Further increase surface area for absorption.
Mechanical Digestion
Segmentation: Localized contractions mix chyme with digestive juices and bring it into contact with the mucosa.
Peristalsis: Propels chyme forward through the intestine.
Chemical Digestion
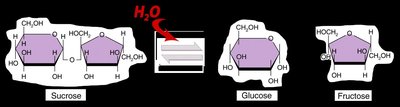
Carbohydrates: Pancreatic amylase and brush border enzymes (maltase, sucrase, lactase, α-dextrinase) break down polysaccharides to monosaccharides.
Proteins: Pancreatic proteases (trypsin, chymotrypsin, carboxypeptidase, elastase) and brush border enzymes (aminopeptidase, dipeptidase) complete protein digestion.
Lipids: Bile salts emulsify fats; pancreatic lipase digests triglycerides to fatty acids and monoglycerides.
Nucleic Acids: Pancreatic ribonuclease and deoxyribonuclease, brush border nucleosidases and phosphatases digest nucleic acids.
Lactose Intolerance
Deficiency of lactase enzyme leads to undigested lactose in the colon, causing diarrhea, gas, and bloating.
Absorption in the Small Intestine
90% of nutrient absorption occurs here.
Absorption methods: diffusion, facilitated diffusion, osmosis, active transport.
Carbohydrates and proteins are absorbed into blood capillaries; lipids are absorbed into lymphatic capillaries (lacteals) as chylomicrons.
All water absorption occurs via osmosis.
The Large Intestine
Structure and Function
The large intestine absorbs water and electrolytes, forms and stores feces, and houses beneficial bacteria.
Regions: Cecum, colon (ascending, transverse, descending, sigmoid), rectum, anal canal.
Mechanical Digestion: Haustral churning, peristalsis, mass movements (gastrocolic reflex).
Chemical Digestion: No digestive enzymes; bacteria ferment remaining carbohydrates, producing gases and vitamins (K, biotin, some amino acids).
Defecation Reflex: Triggered by rectal wall distension.
Histology of the Large Intestine
No villi or circular folds; many goblet cells secrete mucus.
Absorptive epithelium for water and electrolyte absorption.
Intestinal Flora
Trillions of bacteria (flora) aid in digestion, produce vitamins, and contribute to fecal mass.
Bacterial fermentation produces gases (hydrogen, carbon dioxide, methane) and flatulence.
Summary Table: Digestive Enzymes and Their Actions
Enzyme | Source | Substrate | Product | Site of Action |
|---|---|---|---|---|
Salivary Amylase | Salivary glands | Starch | Maltose, dextrins | Mouth |
Lingual Lipase | Lingual glands | Triglycerides | Fatty acids, diglycerides | Stomach |
Pepsin | Stomach (chief cells) | Proteins | Peptides | Stomach |
Pancreatic Amylase | Pancreas | Starch | Maltose, dextrins | Small intestine |
Trypsin, Chymotrypsin, Carboxypeptidase, Elastase | Pancreas | Proteins | Peptides, amino acids | Small intestine |
Pancreatic Lipase | Pancreas | Triglycerides | Fatty acids, monoglycerides | Small intestine |
Brush Border Enzymes (maltase, sucrase, lactase, peptidases, nucleosidases, phosphatases) | Small intestine | Disaccharides, peptides, nucleotides | Monosaccharides, amino acids, nitrogenous bases, phosphates | Small intestine |
