 Back
BackThe Digestive System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Digestive System
Overview and Functions
The digestive system is responsible for the breakdown of food, absorption of nutrients, and elimination of waste. It consists of the digestive tract (alimentary canal) and accessory organs that aid in digestion.
Ingestion: Intake of food and liquids into the oral cavity.
Mechanical Digestion: Physical breakdown of food by chewing and muscular contractions.
Chemical Digestion: Enzymatic breakdown of food into absorbable molecules.
Secretion: Release of water, acids, enzymes, and buffers to aid digestion.
Absorption: Movement of nutrients, water, and electrolytes into the blood or lymph.
Defecation: Elimination of indigestible substances as feces.
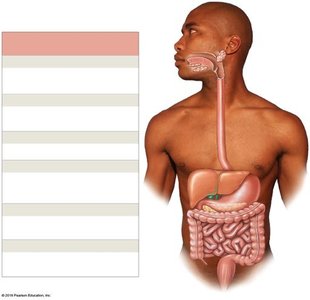
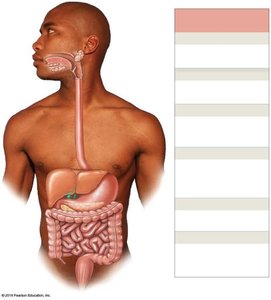
Anatomy of the Digestive Tract
Major Organs and Accessory Structures
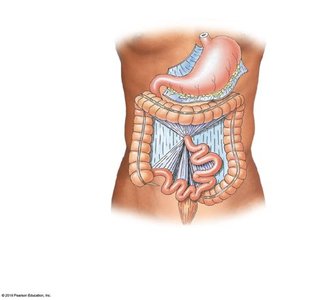
The digestive tract is a continuous muscular tube extending from the oral cavity to the anus. Accessory organs include the teeth, tongue, salivary glands, liver, gallbladder, and pancreas.
Oral Cavity (Mouth): Ingestion, mechanical digestion, and mixing with saliva.
Pharynx: Muscular propulsion of food into the esophagus.
Esophagus: Transports food to the stomach.
Stomach: Chemical and mechanical digestion; forms chyme.
Small Intestine: Enzymatic digestion and absorption of nutrients.
Large Intestine: Absorption of water, compaction of feces.
Anus: Terminal opening for defecation.
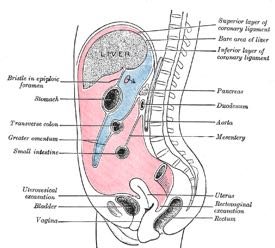
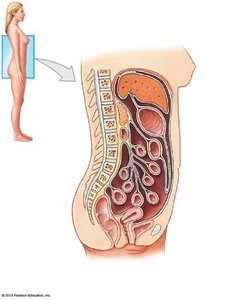
Peritoneum and Mesenteries
Serous Membranes and Organ Support
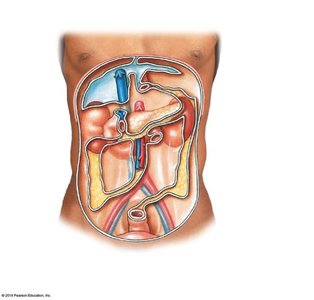
The peritoneum is a serous membrane lining the abdominal cavity and covering abdominal organs. Mesenteries are double layers of peritoneum that support and stabilize the digestive organs, providing a pathway for blood vessels, nerves, and lymphatics.
Parietal Peritoneum: Lines the inner surface of the body wall.
Visceral Peritoneum: Covers the external surfaces of digestive organs.
Mesenteries: Suspend portions of the digestive tract and prevent entanglement of intestines.
Histological Organization of the Digestive Tract
Four Major Layers
The wall of the digestive tract consists of four main layers, each with specialized functions:
Mucosa: Inner lining; mucous membrane with epithelium, lamina propria, and muscularis mucosae.
Submucosa: Dense irregular connective tissue containing blood vessels, lymphatics, and nerves.
Muscular Layer (Muscularis Externa): Smooth muscle responsible for peristalsis and segmentation; contains myenteric plexus.
Serosa: Serous membrane covering most of the digestive tract within the peritoneal cavity.
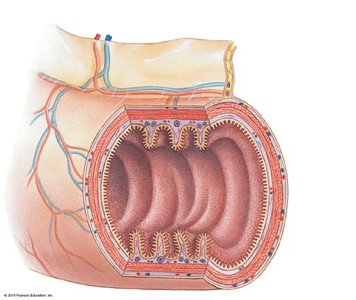
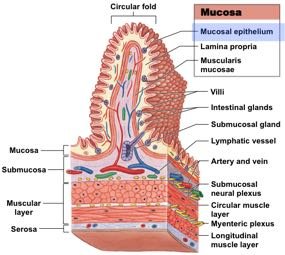
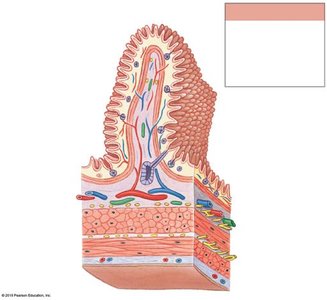
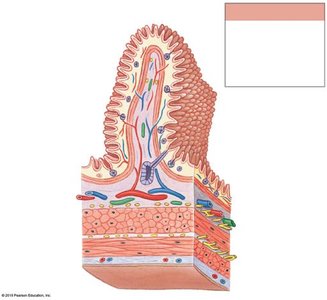
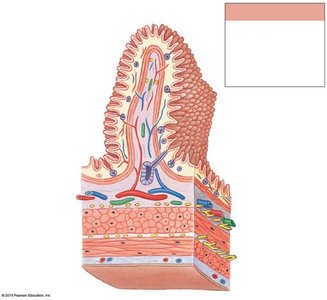
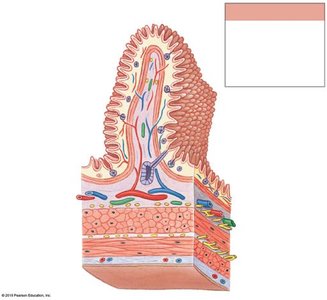
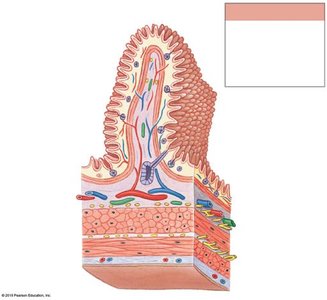
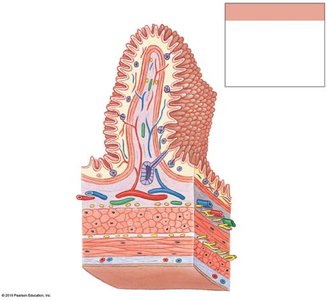
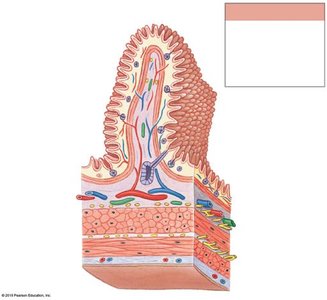
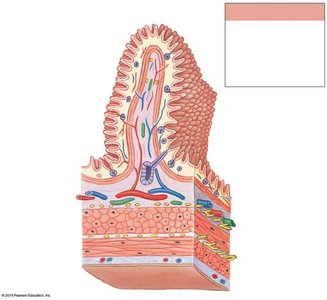
Table: Layers of the Digestive Tract
Layer | Main Components | Function |
|---|---|---|
Mucosa | Epithelium, lamina propria, muscularis mucosae | Secretion, absorption, protection |
Submucosa | Connective tissue, blood vessels, nerves | Support, nutrient supply, innervation |
Muscular Layer | Circular and longitudinal smooth muscle, myenteric plexus | Motility (peristalsis, segmentation) |
Serosa | Serous membrane | Protection, reduces friction |

Motility: Peristalsis and Segmentation
Movement of Digestive Contents
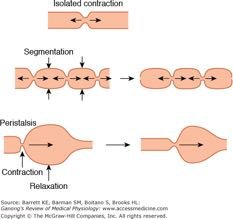
Motility in the digestive tract is achieved by coordinated contractions of smooth muscle layers, primarily through peristalsis and segmentation.
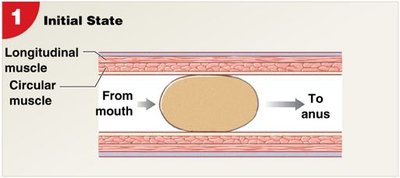
Peristalsis: Waves of muscular contractions that propel a bolus through the digestive tract.
Segmentation: Cycles of contraction that mix and churn contents, enhancing digestion and absorption.
Regulation of Digestive Functions
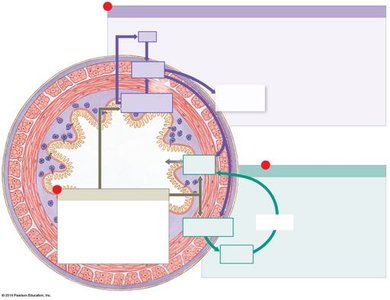
Local, Neural, and Hormonal Mechanisms
Digestive activities are regulated by a combination of local factors, neural reflexes, and hormones.
Local Factors: pH, stretch, and chemical composition directly affect digestive activity.
Neural Mechanisms: Short reflexes (local, ENS) and long reflexes (CNS involvement) control motility and secretion.
Hormonal Mechanisms: Enteroendocrine cells release peptide hormones that modulate digestive processes.
Oral Cavity and Associated Structures
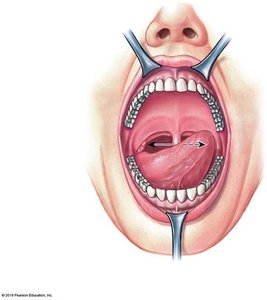
Functions and Anatomy
The oral cavity is the entry point for food and is involved in sensory analysis, mechanical digestion, lubrication, and limited chemical digestion.
Teeth: Responsible for mastication (chewing).
Tongue: Assists in mechanical digestion, manipulation, sensory analysis, and secretion of enzymes.
Salivary Glands: Produce saliva containing enzymes (e.g., amylase) for carbohydrate digestion.
Histology of the Small Intestine
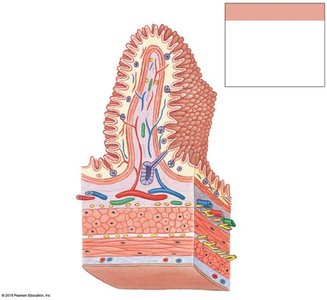
Villi and Microvilli
The small intestine is specialized for absorption, with fingerlike projections called villi and microscopic microvilli forming the brush border. These structures increase surface area for efficient nutrient absorption.
Villi: Covered by simple columnar epithelium; contain capillaries and a central lacteal for nutrient transport.
Microvilli: Form the brush border, containing enzymes for final stages of digestion.
Lacteal: Lymphatic vessel in each villus for absorption of lipids as chylomicrons.

Summary Table: Digestive Tract Layers and Functions
Layer | Location | Main Function |
|---|---|---|
Mucosa | Innermost lining | Secretion, absorption, protection |
Submucosa | Between mucosa and muscular layer | Support, vascular supply, innervation |
Muscular Layer | Between submucosa and serosa | Motility (peristalsis, segmentation) |
Serosa | Outermost layer | Protection, reduces friction |

Peristalsis: Stepwise Process
Initial state: Bolus is positioned between circular and longitudinal muscle layers.
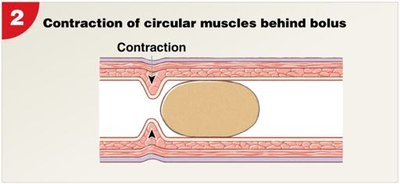
Circular muscles behind bolus contract, pushing it forward.
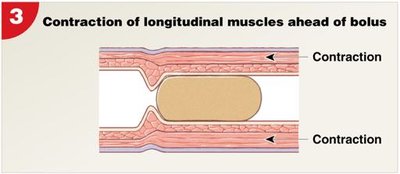
Longitudinal muscles ahead of bolus contract, shortening the tract segment.
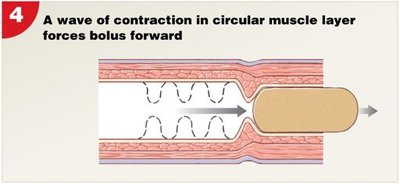
Wave of contraction in circular muscle layer propels bolus forward.




Additional info:
The enteric nervous system (ENS) is a major intrinsic nerve supply of the gastrointestinal tract and can function independently of the central nervous system.
Segmentation is important for mixing chyme with digestive juices and increasing contact with absorptive surfaces.
Accessory organs such as the liver, pancreas, and gallbladder play critical roles in digestion by producing bile, enzymes, and buffers.
