 Back
BackThe Digestive System: Structure, Function, and Organization
Study Guide - Smart Notes

The Digestive System
Overview of the Gastrointestinal (GI) Tract and Accessory Organs
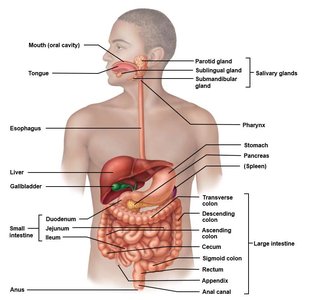
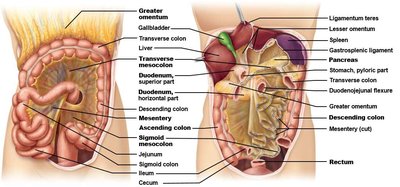
The digestive system is composed of the gastrointestinal (GI) tract, also known as the alimentary canal, and various accessory organs. Together, these structures are responsible for the breakdown, absorption, and elimination of food substances.
GI Tract (Alimentary Canal): A continuous tube extending from the mouth to the anus, approximately 9 meters long in a relaxed state. It includes the mouth, pharynx, esophagus, stomach, small intestine, and large intestine.
Accessory Organs: These organs are not part of the GI tract itself but play essential roles in digestion. They include the teeth and tongue (within the oral cavity), and organs connected via ducts such as the salivary glands, liver, gallbladder, and pancreas.
Function: The GI tract is specialized for ingestion, propulsion, digestion (mechanical and chemical), absorption, and elimination of waste.
The Peritoneum and Peritoneal Cavity
Structure and Development of the Peritoneum
The peritoneum is a serous membrane that lines the abdominal cavity and covers most abdominal organs. It forms a double-layered structure, creating a peritoneal cavity between the layers.
Visceral Peritoneum: Covers the external surfaces of most digestive organs.
Parietal Peritoneum: Lines the body wall of the abdominal cavity.
Peritoneal Cavity: The space between the visceral and parietal layers, containing a small amount of lubricating fluid.
Development: All digestive organs are initially intraperitoneal (within the peritoneal cavity) during embryonic development.
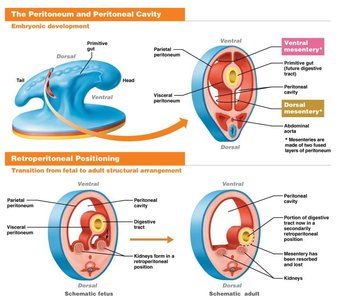
Retroperitoneal Positioning
During development, some organs shift position and become secondarily retroperitoneal, meaning they are located behind the peritoneum and lose their mesenteries. Examples include the pancreas and parts of the duodenum. Organs outside the digestive system, such as the kidneys, are also retroperitoneal.
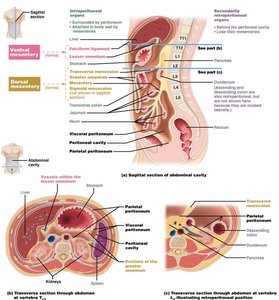
Mesenteries
Definition and Functions of Mesenteries
Mesenteries are double layers of peritoneum that extend from the body wall to the digestive organs. They serve several important functions:
Fat Storage: Mesenteries contain adipose tissue for energy storage and protection.
Route for Vessels: They provide a pathway for blood vessels, lymphatics, and nerves to reach the digestive organs.
Organ Support: Mesenteries help anchor organs in place within the abdominal cavity.
Types of Mesenteries
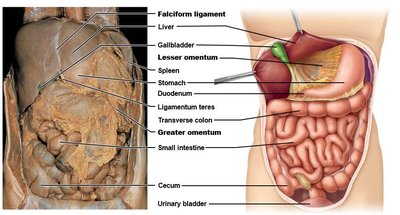
Ventral Mesenteries: Attach the stomach and liver to the anterior abdominal wall.
Lesser Omentum: Connects the liver, lesser curvature of the stomach, and duodenum to the anterior wall.
Falciform Ligament: Attaches the anterior liver to the abdominal wall.
Dorsal Mesenteries: Attach organs to the posterior abdominal wall.
Greater Omentum: Hangs from the greater curvature of the stomach and drapes over the intestines.
Mesentery Proper: Fan-shaped structure attaching the jejunum and ileum to the posterior wall.
Transverse Mesocolon: Connects the transverse colon to the posterior wall.
Sigmoid Mesocolon: Attaches the sigmoid colon to the posterior wall.
Structure and Function of the GI Tract
Major Functions of the GI Tract
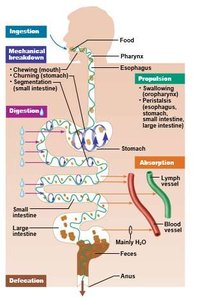
The GI tract performs several essential functions to process food and absorb nutrients:
Ingestion: Taking in food through the mouth.
Motility/Propulsion: Movement of food along the tract via swallowing, peristalsis, and segmentation.
Mechanical and Chemical Digestion: Physical breakdown (chewing, churning) and enzymatic breakdown of food.
Absorption: Uptake of nutrients, water, and electrolytes into blood and lymph vessels.
Elimination: Removal of indigestible substances as feces.
Histological Layers of the GI Tract
The wall of the GI tract is organized into four main layers, each with distinct functions:
Mucosa: The innermost layer, consisting of epithelium, lamina propria (connective tissue), and muscularis mucosae (thin muscle layer). It is involved in secretion, absorption, and protection.
Submucosa: A layer of connective tissue containing blood vessels, lymphatics, and nerves (submucosal plexus).
Muscularis Externa: Two layers of smooth muscle (circular and longitudinal) responsible for peristalsis and segmentation. Contains the myenteric nerve plexus.
Adventitia/Serosa: The outermost layer. Called adventitia when in contact with other organs, and serosa when covered by peritoneum.
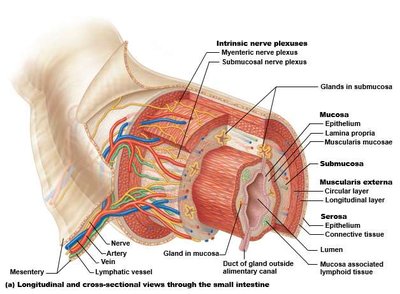
Table: Summary of GI Tract Layers
Layer | Main Components | Function |
|---|---|---|
Mucosa | Epithelium, lamina propria, muscularis mucosae | Secretion, absorption, protection |
Submucosa | Connective tissue, blood vessels, nerves | Support, nutrient supply, innervation |
Muscularis externa | Circular and longitudinal muscle, myenteric plexus | Motility (peristalsis, segmentation) |
Adventitia/Serosa | Connective tissue (adventitia) or serous membrane (serosa) | Protection, structural support |
Example: The small intestine has a highly developed mucosa with villi and microvilli to maximize nutrient absorption, while the stomach has a thick muscularis externa for churning food.
