 Back
BackThe Heart: Structure, Function, and Physiology
Study Guide - Smart Notes

Chapter 19: The Heart
Overview of the Heart and Circulatory Pathways
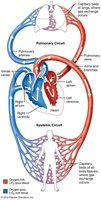
The heart is a muscular organ responsible for pumping blood throughout the body via two main circuits: the pulmonary and systemic circulations. Understanding the anatomy and physiology of the heart is essential for comprehending cardiovascular function and homeostasis.
Pulmonary Circulation: Sends deoxygenated blood from the right side of the heart to the lungs for oxygenation and returns oxygenated blood to the left side of the heart.
Systemic Circulation: Delivers oxygenated blood from the left side of the heart to the body and returns deoxygenated blood to the right side of the heart.
Arteries carry blood away from the heart; veins carry blood towards the heart.
Anatomy of the Heart
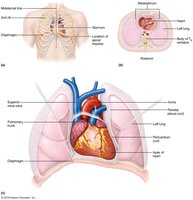
The heart is located in the mediastinum, between the lungs, with its apex pointing towards the left hip. It is divided into four chambers: two atria (superior) and two ventricles (inferior). The heart is surrounded by a double-layered pericardium that reduces friction during contraction.
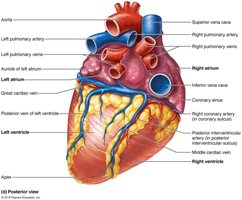
Right Atrium: Receives deoxygenated blood from the body via the superior and inferior vena cava.
Right Ventricle: Pumps deoxygenated blood to the lungs via the pulmonary trunk and arteries.
Left Atrium: Receives oxygenated blood from the lungs via the pulmonary veins.
Left Ventricle: Pumps oxygenated blood to the body via the aorta.
Heart Wall and Pericardium
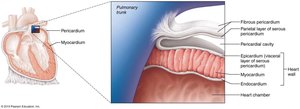
The heart wall consists of three layers: the epicardium (outer), myocardium (muscular middle), and endocardium (inner). The pericardium has two main layers: fibrous and serous (with parietal and visceral components), separated by serous fluid to minimize friction.
Epicardium: Also known as the visceral layer of the serous pericardium.
Myocardium: Composed of cardiac muscle fibers responsible for contraction.
Endocardium: Thin inner lining of the heart chambers.
Heart Valves
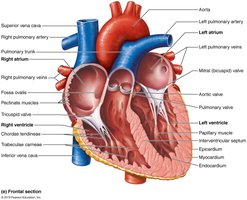
Valves ensure unidirectional blood flow through the heart. There are two types: atrioventricular (AV) valves and semilunar valves.
Right AV Valve (Tricuspid): Between right atrium and right ventricle.
Left AV Valve (Mitral/Bicuspid): Between left atrium and left ventricle.
Pulmonary Semilunar Valve: Between right ventricle and pulmonary trunk.
Aortic Semilunar Valve: Between left ventricle and aorta.
Chordae Tendineae and Papillary Muscles: Prevent AV valve prolapse during ventricular contraction.
Blood Flow Through the Heart
Blood flows through the heart in a specific sequence, passing through each chamber and valve to ensure efficient circulation.
Deoxygenated blood enters the right atrium from the body (via superior and inferior vena cava).
Passes through the tricuspid valve into the right ventricle.
Pumped through the pulmonary semilunar valve into the pulmonary trunk and arteries to the lungs.
Oxygenated blood returns via pulmonary veins to the left atrium.
Passes through the mitral valve into the left ventricle.
Pumped through the aortic semilunar valve into the aorta and systemic circulation.
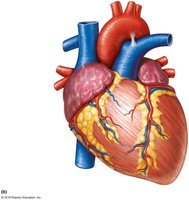
Coronary Circulation
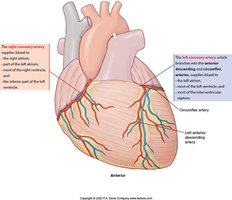
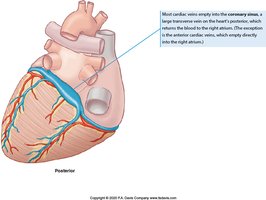
The myocardium receives its own blood supply via the coronary arteries, which branch from the aorta. Cardiac veins collect deoxygenated blood and return it to the right atrium via the coronary sinus.
Left Coronary Artery (LCA): Branches into the left anterior descending (LAD) artery and circumflex artery.
Right Coronary Artery (RCA): Supplies the right side of the heart.
Cardiac Veins: Drain into the coronary sinus.
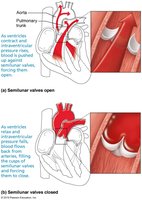
Heart Sounds and the Cardiac Cycle
The heart produces two main sounds: "lub" (S1) and "dup" (S2). S1 is caused by closure of the AV valves at the start of ventricular systole, and S2 by closure of the semilunar valves at the start of ventricular diastole.
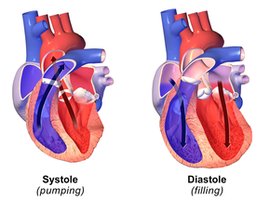
Systole: Contraction phase, blood is ejected from the chambers.
Diastole: Relaxation phase, chambers fill with blood.
Cardiac Muscle Tissue
Cardiac muscle cells are involuntary, striated, and connected by intercalated discs containing gap junctions and desmosomes. This structure allows the heart to contract as a functional syncytium and prevents tetany, ensuring rhythmic contractions.
Autorhythmicity: Pacemaker cells can depolarize spontaneously without neural input.
Gap Junctions: Allow electrical signals to pass rapidly between cells.
Desmosomes: Provide mechanical strength during contraction.
Electrical Activity of the Heart
The heart's intrinsic conduction system coordinates contraction. The main components are:
Sinoatrial (SA) Node: Main pacemaker, initiates each heartbeat.
Atrioventricular (AV) Node: Delays impulse, allowing atrial contraction before ventricular contraction.
Bundle of His, Bundle Branches, Purkinje Fibers: Distribute the impulse through the ventricles.
Electrocardiogram (ECG/EKG)
An ECG records the electrical activity of the heart as a series of waves:
P wave: Atrial depolarization.
QRS complex: Ventricular depolarization (and atrial repolarization).
T wave: Ventricular repolarization.
The Cardiac Cycle
The cardiac cycle includes all events in one heartbeat:
Atrial systole (contraction)
Atrial diastole (relaxation)
Ventricular systole (contraction)
Ventricular diastole (relaxation)
Stroke Volume and Cardiac Output
Stroke volume (SV) is the amount of blood ejected by one ventricle in one contraction. Cardiac output (CO) is the volume ejected by one ventricle in one minute.
Stroke Volume Equation:
Cardiac Output Equation:
Factors Affecting SV: Venous return, preload, afterload, contractility, age, gender, heart size, fitness.
Factors Affecting CO: Anything affecting SV or heart rate (HR), including neural and hormonal influences.
Cardiovascular Homeostasis
The cardiovascular center in the medulla oblongata regulates heart rate and vessel tone via sympathetic and parasympathetic l
]l
. Baroreceptors and chemoreceptors provide feedback to maintain blood pressure and tissue perfusion.
Cardioacceleratory Center: Increases heart rate and contractility (sympathetic).
Cardio inhibitory Center: Decreases heart rate (parasympathetic, vagus nerve).
Vasomotor Center: Regulates vessel diameter (sympathetic).
Clinical Notes
Valve Disorders: Prolapse (regurgitation) and stenosis can impair blood flow and efficiency.
Myocardial Infarction (Heart Attack): Blockage of coronary arteries leads to tissue death.
Cardiac Tamponade: Fluid accumulation in the pericardial sac restricts heart function.
References: Marieb & Hoehn, OpenStax Anatomy & Physiology, F.A. Davis, et al.
