 Back
BackThe Human Reproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Reproductive System Overview
Functions of the Reproductive System
The reproductive system ensures the continuation of the species by producing, nurturing, and transporting gametes, facilitating fertilization, and supporting the development of offspring.
Genetic Continuity: Passes genetic material to the next generation.
People with testes: Produce and deliver sperm to the partner.
People with ovaries: Produce eggs, receive sperm, support fertilization, protect and nourish the embryo/fetus, give birth, and nourish offspring.
Primary and Secondary Sex Organs
Primary Sex Organs (Gonads)
The primary sex organs are the gonads: testes in people assigned male at birth and ovaries in people assigned female at birth. These organs produce gametes and secrete sex hormones.
Testes: Produce sperm (male gametes) and secrete testosterone.
Ovaries: Produce eggs (female gametes) and secrete estrogen and progesterone.
Secondary (Accessory) Sex Organs
Accessory sex organs support the storage, survival, and transport of gametes, and facilitate fertilization and development.
People with testes: Epididymis, vas deferens, ejaculatory duct, urethra, seminal vesicles, prostate, bulbo-urethral glands, penis.
People with ovaries: Uterine tubes, uterus, vagina, labia, clitoris.
Male Reproductive Anatomy and Physiology
Testes: Structure and Cell Types
The testes are divided into lobules containing seminiferous tubules, where sperm production occurs. Three main cell types are present:
Spermatogenic (germ) cells: Undergo meiosis to form sperm.
Sustentacular (Sertoli) cells: Support and nourish developing sperm; form the blood-testis barrier.
Interstitial (Leydig) cells: Produce testosterone.
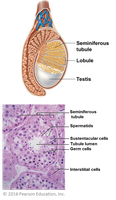
Accessory Duct System for Sperm
Sperm travel through a series of ducts:
Epididymis: Site of sperm maturation and storage.
Vas deferens: Transports sperm from the epididymis to the ejaculatory duct.
Ejaculatory duct: Passageway for sperm and seminal fluid into the urethra.
Urethra: Conducts semen to the exterior during ejaculation.
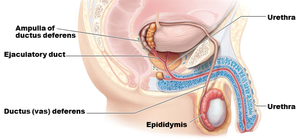
Accessory Glands
Accessory glands produce the bulk of semen, providing nutrients, enzymes, and lubricants for sperm viability and motility.
Seminal vesicles: Secrete fructose-rich fluid for sperm energy.
Prostate gland: Adds enzymes and alkaline fluid to activate sperm.
Bulbo-urethral glands: Secrete mucus for lubrication and neutralization of acidic urine in the urethra.
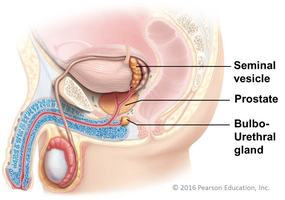
Penis
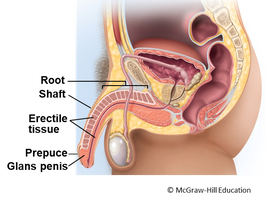
The penis is the copulatory organ, consisting of an internal root, external shaft, and glans penis (tip), surrounded by the foreskin (prepuce). It contains erectile tissue that enables erection for sexual intercourse.
Regulation: Hypothalamic-Pituitary-Gonadal (HPG) Axis
Overview of the HPG Axis
The HPG axis is a hormonal feedback system that regulates the development, function, and hormone production of the gonads.
Hypothalamus: Releases gonadotropin-releasing hormone (GnRH).
Anterior pituitary: Releases follicle-stimulating hormone (FSH) and luteinizing hormone (LH).
Gonads (testes): Produce sperm and secrete testosterone.
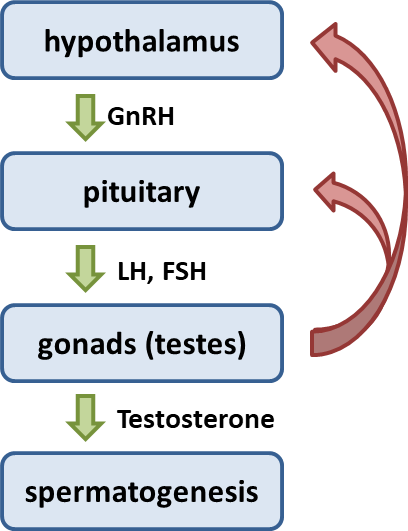
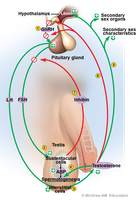
Hormonal Regulation in Testes
GnRH: Stimulates the anterior pituitary to release FSH and LH.
FSH: Acts on sustentacular cells to promote spermatogenesis and release androgen-binding protein (ABP).
LH: Stimulates interstitial cells to produce testosterone.
Testosterone: Stimulates spermatogenesis, development of sex organs, secondary sex characteristics, and libido; inhibits GnRH to regulate hormone levels.
Inhibin: Released by sustentacular cells when sperm count is high; inhibits FSH to reduce spermatogenesis.
Female Reproductive Anatomy and Physiology
Ovaries
The ovaries are paired organs lateral to the uterus, containing follicles at various stages of development. They produce eggs and secrete estrogen and progesterone.
Medulla: Contains blood vessels and nerves.
Cortex: Contains ovarian follicles (developing eggs).
Accessory Sex Organs
Internal genitalia: Uterine tubes (fallopian tubes), uterus, vagina.
External genitalia (vulva): Labia majora, labia minora, clitoris.
Uterine Tubes (Fallopian Tubes)
The uterine tubes transport the oocyte from the ovary to the uterus and are the typical site of fertilization. Their structure, including cilia and smooth muscle, helps move the oocyte toward the uterus.
Uterus
The uterus is a thick-walled muscular organ specialized to receive, retain, and nourish a fertilized egg. The cervix is the lower, narrow portion that opens into the vagina.
Perimetrium: Outer serous layer.
Myometrium: Thick muscular layer responsible for contractions.
Endometrium: Inner mucosal layer that undergoes cyclic changes during the menstrual cycle.
Vagina
The vagina is a thin-walled tube serving as the organ of copulation, the birth canal, and the passageway for menstrual flow. Its acidic environment helps protect against infections.
External Genitalia
Labia majora and minora: Folds of skin protecting the vaginal and urethral openings.
Clitoris: Erectile tissue important for sexual arousal.
Ovarian and Menstrual Cycles (Sexual Cycle)
Overview
The sexual cycle consists of the ovarian cycle (events in the ovaries) and the menstrual cycle (events in the uterus), typically lasting 28 days and regulated by the HPG axis.
Ovarian Cycle Phases
Follicular phase (Day 1-14): Follicle grows and matures; variable in length.
Ovulation (Day 14): Mature follicle ruptures, releasing the oocyte.
Luteal phase (Day 14-28): Corpus luteum forms and secretes estrogen and progesterone; relatively constant in length.
Menstrual Cycle Phases
Menstrual phase (Day 1-5): Shedding of the endometrial lining.
Proliferative phase (Day 6-14): Endometrium rebuilds under estrogen influence.
Secretory phase (Day 14-28): Endometrium thickens and secretes nutrients; if no fertilization, tissue degenerates.
Hormonal Regulation of the Female Cycle
GnRH: Stimulates FSH and LH release from the anterior pituitary.
FSH and LH: Promote follicle growth and estrogen secretion.
Estrogen: Stimulates endometrial growth; high levels trigger LH surge and ovulation.
Progesterone (from corpus luteum): Prepares endometrium for implantation; inhibits GnRH, FSH, and LH to prevent new cycle initiation.
If no fertilization: Corpus luteum degenerates, hormone levels fall, endometrium is shed, and the cycle restarts.
If fertilization occurs: Embryo produces human chorionic gonadotropin (hCG), maintaining corpus luteum and hormone production until placenta takes over.
Fertilization
Fertilization is the union of sperm and egg, typically occurring in the uterine tube. This event restores the diploid chromosome number and initiates embryonic development.
Summary Table: Comparison of Male and Female Reproductive Systems
Feature | People with Testes | People with Ovaries |
|---|---|---|
Primary Sex Organs | Testes | Ovaries |
Gametes Produced | Sperm | Eggs (Oocytes) |
Main Hormones | Testosterone | Estrogen, Progesterone |
Accessory Ducts | Epididymis, Vas deferens, Ejaculatory duct, Urethra | Uterine tubes, Uterus, Vagina |
Accessory Glands | Seminal vesicles, Prostate, Bulbo-urethral glands | None (glands associated with lubrication) |
External Genitalia | Penis, Scrotum | Labia, Clitoris |
Additional info: The above notes integrate foundational concepts from human anatomy and physiology, focusing on the reproductive system as outlined in standard college-level ANP courses. Images were included only when directly relevant to the anatomical or physiological explanation.
