 Back
BackThe Human Reproductive System: Structure, Function, and Cycles
Study Guide - Smart Notes

Reproductive System Overview
Introduction to Biological Sex and Reproductive Anatomy
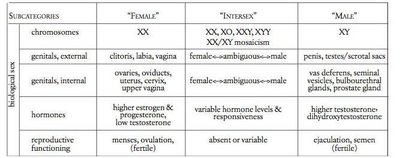
The human reproductive system is responsible for producing gametes, supporting fertilization, and enabling the development of offspring. Biological sex is determined by a combination of chromosomes, hormones, and anatomical sex characteristics. The typical categories are male, female, and intersex, with intersex individuals exhibiting a range of biological variations.
Male typical: XY chromosomes, testes, penis, and associated glands.
Female typical: XX chromosomes, ovaries, uterus, vagina, and associated structures.
Intersex: Variations in chromosomes, gonads, hormones, or genitalia that do not fit typical definitions of male or female.
Note: The presence or absence of specific anatomical structures does not determine gender identity.
Male Reproductive System
Primary and Accessory Organs
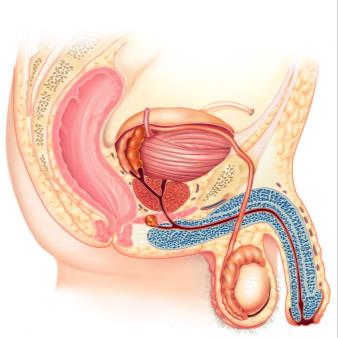
The male reproductive system includes primary organs (testes) that produce sperm and accessory organs that support sperm maturation, storage, and delivery.
Testes: Produce sperm and testosterone.
Epididymis: Stores and matures sperm.
Vas (ductus) deferens: Transports sperm from the epididymis to the urethra.
Seminal vesicles, prostate, bulbourethral glands: Produce seminal fluid that nourishes and protects sperm.
Penis: Organ for copulation and sperm delivery.
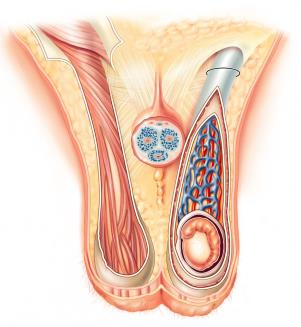
Scrotum and Temperature Regulation
The scrotum houses the testes outside the body cavity, maintaining an optimal temperature (~93°F) for sperm production. Two muscles regulate scrotal temperature:
Dartos muscle: Wrinkles scrotal skin to increase thickness for warmth.
Cremaster muscle: Elevates testes for warmth.
Pampiniform plexus: Venous network that cools arterial blood entering the testes.
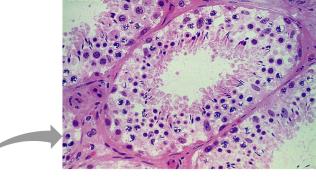
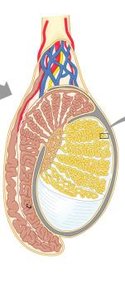
Testicular Structure and Spermatogenesis
The testes are divided into lobules by the tunica albuginea. Each lobule contains seminiferous tubules, the site of sperm production. Sperm travel from the seminiferous tubules to the rete testis and then to the epididymis.
Tunica vaginalis: Serous membrane derived from the peritoneum.
Tunica albuginea: Fibrous capsule surrounding the testis.
Seminiferous tubules: Site of spermatogenesis.
Spermatogenesis
Spermatogenesis is the process of sperm formation, occurring continuously in the seminiferous tubules. It involves mitosis, meiosis, and differentiation:
Spermatogonia: Stem cells that divide by mitosis.
Primary spermatocytes: Undergo meiosis I to form secondary spermatocytes.
Secondary spermatocytes: Undergo meiosis II to form spermatids.
Spermatids: Differentiate into mature spermatozoa.
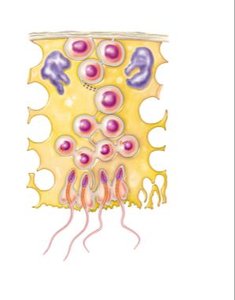
Sperm Maturation and Pathway
Sperm mature in the epididymis, which has three regions: head, body, and tail. Mature sperm are stored in the tail until ejaculation. The spermatic cord contains the vas deferens, blood vessels, and nerves.
Epididymis: Sperm gain motility and are stored.
Vas deferens: Transports sperm during ejaculation.
Spermatic cord: Contains vas deferens, blood vessels, and nerves.
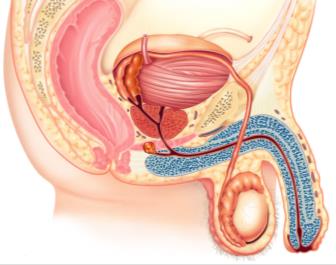
Accessory Glands and Semen Production
Accessory glands produce seminal fluid, which combines with sperm to form semen:
Seminal vesicles: Produce ~60% of seminal fluid, rich in fructose and prostaglandins.
Prostate gland: Produces ~30% of seminal fluid, enhances sperm motility.
Bulbourethral glands: Secrete basic fluid to neutralize acidic urine and lubricate the urethra.
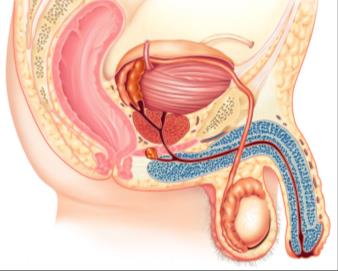
Male Urethra and Erectile Tissue
The male urethra transports both urine and semen and is divided into three segments:
Prostatic urethra: Passes through the prostate gland.
Membranous urethra: Passes through the pelvic floor.
Spongy urethra: Passes through the penis.
The penis contains erectile tissues: corpus cavernosum (paired, primary erectile bodies) and corpus spongiosum (surrounds urethra and forms the glans penis).
Female Reproductive System
Primary and Accessory Organs
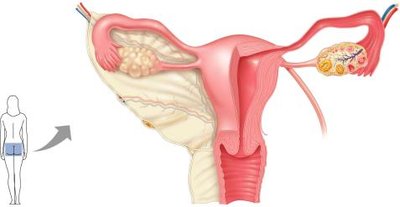
The female reproductive system includes the ovaries (primary organs) and accessory structures that support oocyte transport, fertilization, and fetal development.
Ovaries: Produce oocytes and hormones (estrogen, progesterone).
Uterine (fallopian) tubes: Transport oocyte; site of fertilization.
Uterus: Site of implantation and fetal development.
Vagina: Receives sperm and serves as the birth canal.
Vulva: External genitalia, including labia majora, labia minora, and clitoris.
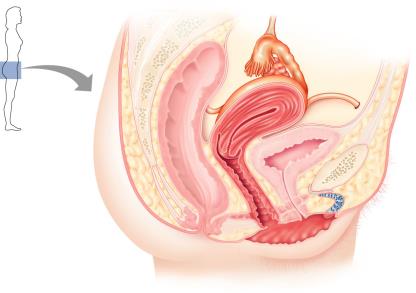
External Genitalia and Mammary Glands
Labia majora: Outer folds, homologous to the scrotum.
Labia minora: Inner folds, homologous to corpus spongiosum.
Clitoris: Erectile tissue, homologous to corpus cavernosa.
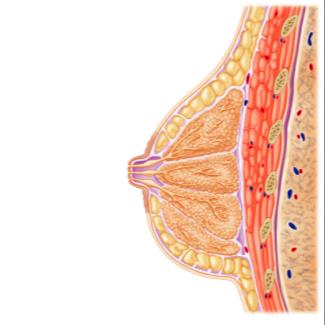
Mammary glands: Modified sweat glands that produce milk; composed of lobules drained by lactiferous ducts.
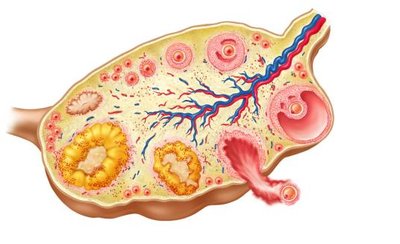
Oogenesis and the Ovarian Cycle
Oogenesis is the process of egg formation in the ovaries. The ovarian cycle is divided into two phases:
Follicular phase (days 1–14): Follicles mature; ends with ovulation (release of secondary oocyte).
Luteal phase (days 14–28): Corpus luteum forms from the empty follicle, secreting hormones to prepare the uterus for implantation.
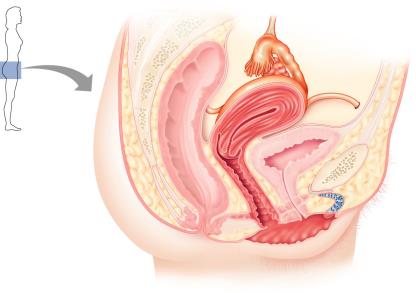
Uterine (Fallopian) Tubes and Uterus
The uterine tubes carry the oocyte from the ovary to the uterus and are the typical site of fertilization. The uterus is where a fertilized embryo implants and develops.
Fimbriae: Ciliated projections that help capture the oocyte.
Uterus: Sits atop the bladder; consists of three layers: perimetrium (outer), myometrium (muscle), and endometrium (inner lining).
Endometrial Structure and Menstrual Cycle
The endometrium is the inner lining of the uterus and undergoes cyclic changes in response to hormones:
Stratum functionalis: Sheds during menstruation; rebuilt during the proliferative phase.
Stratum basalis: Remains after menstruation and regenerates the functionalis.
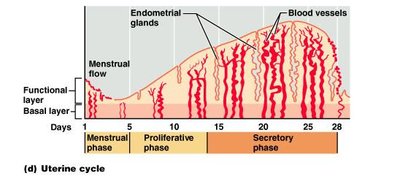
The Menstrual (Uterine) Cycle
The menstrual cycle consists of three phases:
Menstrual phase (days 1–6): Shedding of the stratum functionalis.
Proliferative phase (days 6–14): Rebuilding of the endometrium; ends with ovulation.
Secretory phase (days 15–28): Endometrium prepares for implantation; corpus luteum secretes progesterone and estrogen.
Hormonal Regulation of the Ovarian and Uterine Cycles
Fluctuating levels of pituitary gonadotropins (FSH and LH) and ovarian hormones (estrogen and progesterone) regulate the ovarian and uterine cycles. The follicular phase corresponds to the menstrual and proliferative phases, while the luteal phase corresponds to the secretory phase.
FSH (Follicle-Stimulating Hormone): Stimulates follicle development.
LH (Luteinizing Hormone): Triggers ovulation and corpus luteum formation.
Estrogen: Promotes endometrial growth and LH surge.
Progesterone: Maintains endometrium for implantation.
Vagina and Cervix
The vagina is the muscular canal leading from the cervix (lower part of the uterus) to the external body. It is lined by stratified squamous epithelium and serves as the site for sperm deposition and the birth canal.
