 Back
BackThe Human Reproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Human Reproductive System
Overview of Sexual Reproduction
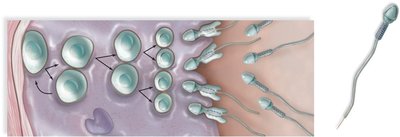
The human reproductive system enables the production of new life by combining genetic material from two individuals of different sexes. Sexual reproduction involves the formation of specialized cells called gametes—sperm in males and eggs in females—produced in the gonads. Fertilization in humans is internal, with the union of sperm and egg occurring inside the female body.
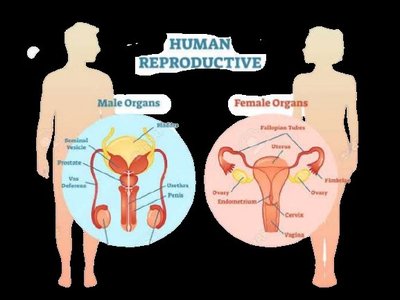
Male gametes: Sperm, produced in the testes
Female gametes: Eggs (ova), produced in the ovaries
Copulation: The act of sexual intercourse, facilitating internal fertilization
Male Reproductive System
Structure and Function of Male Organs
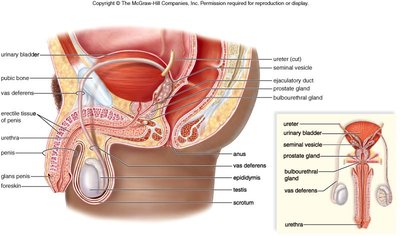
The male reproductive system is specialized for the production, maturation, and delivery of sperm. It consists of primary and accessory organs that work together to ensure reproductive success.
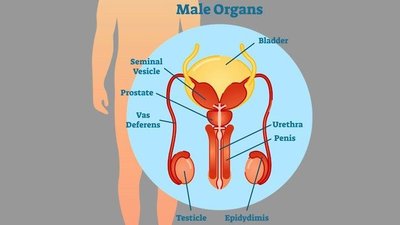
Testes: Primary sex organs producing sperm and testosterone
Epididymis: Site of sperm maturation and storage
Vas deferens: Muscular tube transporting sperm from the epididymis to the urethra
Urethra: Conducts sperm (and urine) out of the body
Penis: Organ of copulation
Accessory glands: Seminal vesicles, prostate gland, and bulbourethral glands contribute fluids to semen
Organ | Function |
|---|---|
Testes | Produce sperm and sex hormones |
Epididymides | Sites of maturation and storage of sperm |
Vasa deferentia | Conduct and store sperm |
Seminal vesicles | Contribute fluid to semen |
Prostate gland | Contributes fluid to semen |
Urethra | Conducts sperm (and urine) |
Bulbourethral glands | Contribute fluid to semen |
Penis | Organ of copulation |

The Testes and Spermatogenesis
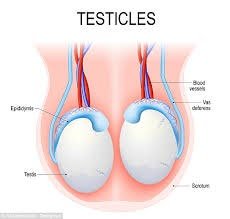
The testes are paired organs suspended in the scrotum, responsible for producing sperm and testosterone. Sperm production occurs in the seminiferous tubules through a process called spermatogenesis.
Spermatogenesis: The process of forming mature sperm from spermatogonia, beginning at puberty and taking about 64 days.
Spermiogenesis: The maturation of spermatids into spermatozoa (mature sperm cells).
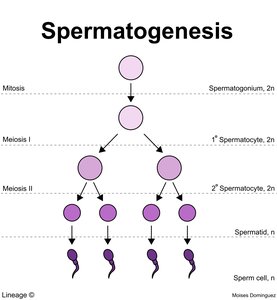
Phases of Spermatogenesis
Mitosis: Spermatogonia (diploid, 2n) divide to produce primary spermatocytes.
Meiosis I: Primary spermatocytes undergo meiosis I to form two secondary spermatocytes (haploid, n).
Meiosis II: Each secondary spermatocyte divides to form two spermatids (total of four haploid cells).
Spermiogenesis: Spermatids mature into spermatozoa, developing a flagellum (tail) and acrosome (cap).
Key equation: Chromosome number after meiosis:
Example: Human sperm and egg each have 23 chromosomes; fertilization restores the diploid number (46).
Accessory Glands and Semen Composition
Accessory glands secrete fluids that support sperm viability and mobility, forming semen.
Seminal vesicles: Produce about 60% of semen volume, containing fructose (energy), alkaline fluids (neutralize acidity), proteins, and prostaglandins (reduce female immune response).
Prostate gland: Secretes slightly acidic fluid that nourishes and protects sperm; contracts during ejaculation to propel semen.
Bulbourethral glands: Secrete mucus-like fluid for lubrication and neutralization of urethral acidity.
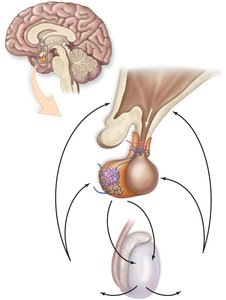
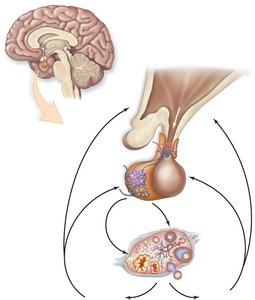
Hormonal Regulation in Males
The hypothalamus and pituitary gland regulate male reproductive function through the release of hormones:
Follicle Stimulating Hormone (FSH): Promotes spermatogenesis by making cells responsive to testosterone.
Luteinizing Hormone (LH): Stimulates testosterone production by the testes.
Testosterone: Major male sex hormone; establishes and maintains secondary sex characteristics (e.g., muscle mass, deeper voice, facial hair).
Female Reproductive System
Structure and Function of Female Organs
The female reproductive system is specialized for the production of eggs, reception of sperm, fertilization, and support of embryonic and fetal development.
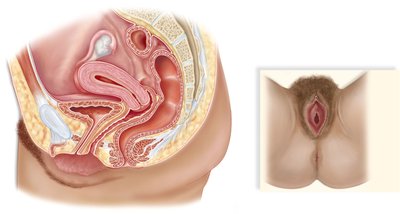
Ovaries: Primary organs producing eggs (oogenesis) and sex hormones (estrogen, progesterone)
Oviducts (fallopian tubes): Conduct eggs from ovary to uterus; site of fertilization
Uterus: Muscular organ housing and nourishing the embryo/fetus
Cervix: Narrow opening between uterus and vagina; produces mucus and dilates during childbirth
Vagina: Muscular canal for copulation, childbirth, and menstrual flow
Vulva: External genitalia including labia majora and minora
Organ | Function |
|---|---|
Ovaries | Produce egg and sex hormones |
Oviducts (fallopian tubes) | Conduct egg; location of fertilization |
Uterus (womb) | Houses developing embryo and fetus |
Vagina | Receives penis during copulation and serves as birth canal |

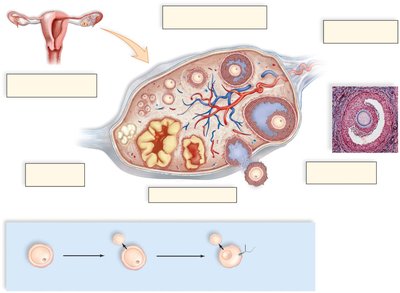
Oogenesis and the Ovarian Cycle
Oogenesis is the process of egg formation in the ovaries. The ovarian (menstrual) cycle is regulated by hormones and consists of several phases:
Follicular phase (days 1–13): FSH stimulates follicle development; follicles secrete estrogen.
Ovulation (day 14): LH surge triggers release of a secondary oocyte from the ovary.
Luteal phase (days 15–28): Corpus luteum forms from the ruptured follicle, secreting progesterone and estrogen to maintain the uterine lining.
Key equation: Chromosome number after meiosis:
Example: Human egg and sperm each have 23 chromosomes; fertilization restores the diploid number (46).
Uterine (Menstrual) Cycle
The uterine cycle prepares the endometrium for possible implantation and is divided into phases:
Menstrual phase (days 1–5): Shedding of the endometrial lining; menstrual flow occurs.
Follicular phase (days 1–13): Endometrial lining rebuilds under estrogen influence.
Ovulation (day 14): Release of the egg into the fallopian tube.
Luteal phase (days 15–28): Progesterone maintains the endometrium; if no fertilization, hormone levels drop and menstruation begins again.
Fertilization, Pregnancy, and Lactation
Fertilization typically occurs in the fallopian tube. The resulting zygote divides and implants in the uterine lining. The placenta produces human chorionic gonadotropin (HCG), which maintains the corpus luteum and is detected in pregnancy tests. After childbirth, prolactin stimulates milk production in the mammary glands.
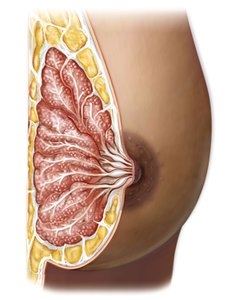
Colostrum: First milk produced, rich in antibodies and nutrients
Nipple and areola: Structures for breastfeeding; areola contains glands to protect the nipple
Mammary glands: Organized into lobules, produce milk in response to prolactin
Summary Table: Key Hormones in Reproduction
Hormone | Source | Main Function |
|---|---|---|
FSH | Pituitary gland | Stimulates gamete production (spermatogenesis/oogenesis) |
LH | Pituitary gland | Stimulates sex hormone production; triggers ovulation |
Testosterone | Testes | Male secondary sex characteristics, spermatogenesis |
Estrogen | Ovaries | Female secondary sex characteristics, endometrial growth |
Progesterone | Ovaries (corpus luteum) | Maintains uterine lining |
HCG | Placenta | Maintains corpus luteum in early pregnancy |
Prolactin | Pituitary gland | Stimulates milk production |
Additional info: The reproductive system is regulated by complex hormonal feedback loops involving the hypothalamus, pituitary gland, and gonads. Disorders such as endometriosis, infertility, and hormonal imbalances can affect reproductive health.
