 Back
BackThe Hypothalamus and Pituitary Gland: Structure, Function, and Hormonal Regulation
Study Guide - Smart Notes

The Hypothalamus and Pituitary Gland
Overview
The hypothalamus and pituitary gland are central to the regulation of the endocrine system. The pituitary gland, located in the sella turcica of the sphenoid bone, is connected to the hypothalamus by the infundibulum. It consists of two major lobes: the posterior pituitary (neurohypophysis) and the anterior pituitary (adenohypophysis), each with distinct embryological origins, structures, and functions.
Pituitary-Hypothalamic Relationships
Dual Origin and Structure
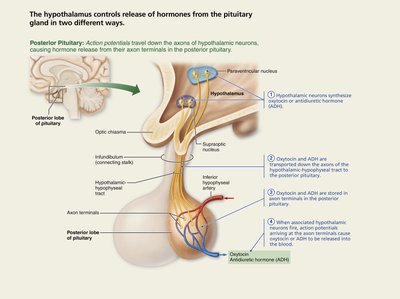
Posterior Pituitary (Neurohypophysis): Composed of neural tissue, including axons and pituicytes. It is an extension of the hypothalamus and stores hormones produced by hypothalamic neurons.
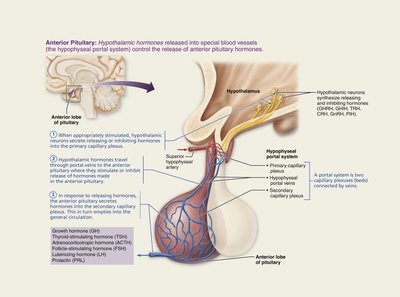
Anterior Pituitary (Adenohypophysis): Composed of glandular epithelial tissue. It synthesizes and releases its own hormones in response to hypothalamic signals.
The two lobes are connected to the hypothalamus by different mechanisms: the posterior lobe by neural connections (hypothalamic-hypophyseal tract) and the anterior lobe by a vascular portal system (hypophyseal portal system).
Posterior Pituitary and Hypothalamic Hormones
Hormone Storage and Release
The posterior pituitary stores and releases two main hormones produced by the hypothalamus:
Oxytocin: Produced mainly by paraventricular neurons. Stimulates uterine contractions during childbirth and milk ejection during breastfeeding. Also acts as a neurotransmitter in the brain, promoting bonding and trust.
Antidiuretic Hormone (ADH, Vasopressin): Produced mainly by supraoptic neurons. Regulates water balance by increasing water reabsorption in the kidneys, thus reducing urine output and preventing dehydration.
Both hormones are released into the bloodstream in response to action potentials from the hypothalamic neurons.
Clinical Correlations
Diabetes Insipidus: Caused by ADH deficiency, leading to excessive urine output and thirst.
SIADH (Syndrome of Inappropriate ADH Secretion): Excess ADH causes fluid retention, hyponatremia, and brain edema.
Anterior Pituitary Hormones
Hormone Synthesis and Regulation
The anterior pituitary synthesizes and releases six major peptide/protein hormones under the control of hypothalamic releasing and inhibiting hormones delivered via the hypophyseal portal system:
Growth Hormone (GH, Somatotropin): Stimulates growth and metabolism in most tissues, especially bone and muscle.
Thyroid-Stimulating Hormone (TSH, Thyrotropin): Stimulates the thyroid gland to produce thyroid hormones.
Adrenocorticotropic Hormone (ACTH, Corticotropin): Stimulates the adrenal cortex to release glucocorticoids.
Follicle-Stimulating Hormone (FSH): Stimulates gamete production in ovaries and testes.
Luteinizing Hormone (LH): Triggers ovulation and stimulates production of gonadal hormones.
Prolactin (PRL): Stimulates milk production in the breasts.
Growth Hormone (GH)
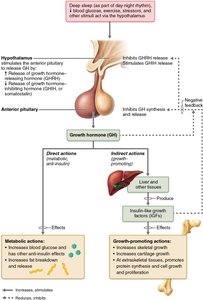
GH has both direct and indirect effects:
Direct Actions: Mobilizes fats, increases blood glucose (anti-insulin effect), and stimulates protein synthesis.
Indirect Actions: Stimulates the liver and other tissues to produce insulin-like growth factors (IGFs), which promote cell division, protein synthesis, and bone growth.
GH secretion is regulated by:
Growth Hormone–Releasing Hormone (GHRH): Stimulates GH release, especially during sleep and adolescence.
Growth Hormone–Inhibiting Hormone (GHIH, Somatostatin): Inhibits GH release in response to high GH and IGF levels.
Clinical Correlations
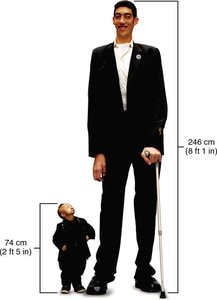
Gigantism: Hypersecretion of GH in children leads to excessive growth.
Acromegaly: Hypersecretion of GH in adults causes enlargement of extremities.
Pituitary Dwarfism: Hyposecretion of GH in children results in short stature with normal proportions.
Thyroid-Stimulating Hormone (TSH)
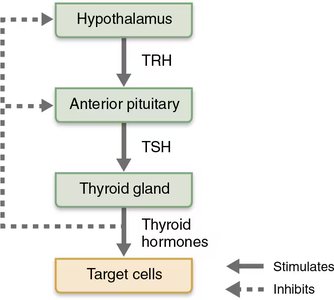
TSH stimulates the thyroid gland to produce thyroid hormones, which regulate metabolism. Its release is controlled by:
Thyrotropin-Releasing Hormone (TRH): From the hypothalamus, stimulates TSH release.
Negative Feedback: Rising thyroid hormone levels inhibit TSH and TRH secretion.
Adrenocorticotropic Hormone (ACTH)
ACTH stimulates the adrenal cortex to release glucocorticoids, which help the body respond to stress. Its release is regulated by:
Corticotropin-Releasing Hormone (CRH): From the hypothalamus, stimulates ACTH release.
Negative Feedback: Rising glucocorticoid levels inhibit CRH and ACTH secretion.
Stressors: Such as fever and hypoglycemia, increase CRH and ACTH release.
Gonadotropins: FSH and LH
FSH and LH regulate the function of the gonads (ovaries and testes):
FSH: Stimulates gamete (egg or sperm) production.
LH: Triggers ovulation and stimulates production of sex hormones (estrogen, progesterone, testosterone).
Both are regulated by Gonadotropin-Releasing Hormone (GnRH) from the hypothalamus and are virtually absent before puberty.
Prolactin (PRL)
PRL stimulates milk production in females. Its release is primarily inhibited by Prolactin-Inhibiting Hormone (PIH, dopamine). Estrogen increases PRL secretion, especially during pregnancy and breastfeeding.
Clinical Correlations
Hyperprolactinemia: Most often due to pituitary tumors, causing inappropriate lactation, infertility, and menstrual disturbances.
Summary Table: Pituitary Hormones
The following tables summarize the regulation, target organs, effects, and clinical consequences of hypo- and hypersecretion for each pituitary hormone.
Hormone | Regulation of Release | Target Organ & Effects | Effects of Hypo-/Hypersecretion |
|---|---|---|---|
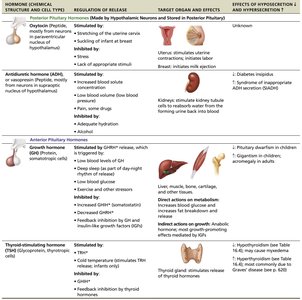
Oxytocin | Stimulated by cervical/uterine stretching, suckling of infant | Uterus: stimulates contractions; Breast: initiates milk ejection | No important effects known |
Antidiuretic Hormone (ADH) | Stimulated by increased blood solute concentration, low blood volume; Inhibited by adequate hydration, alcohol | Kidneys: stimulates water reabsorption | Hypo: Diabetes insipidus; Hyper: SIADH |
Hormone | Regulation of Release | Target Organ & Effects | Effects of Hypo-/Hypersecretion |
|---|---|---|---|
Growth Hormone (GH) | Stimulated by GHRH, deep sleep, stress; Inhibited by GHIH, obesity, high GH/IGF | Liver, muscle, bone, cartilage: stimulates growth, protein synthesis, mobilizes fat, increases blood glucose | Hypo: Pituitary dwarfism in children; Hyper: Gigantism in children, acromegaly in adults |
Thyroid-Stimulating Hormone (TSH) | Stimulated by TRH; Inhibited by thyroid hormones, GHIH | Thyroid gland: stimulates release of thyroid hormones | Hypo: Cretinism in children, myxedema in adults; Hyper: Hyperthyroidism |
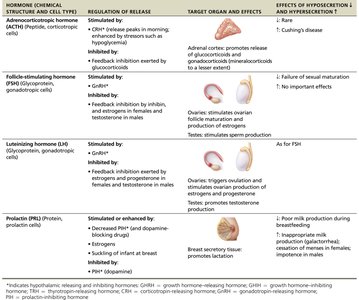
Adrenocorticotropic Hormone (ACTH) | Stimulated by CRH, stress; Inhibited by glucocorticoids | Adrenal cortex: stimulates release of glucocorticoids | Hypo: Rare; Hyper: Cushing's disease |
Follicle-Stimulating Hormone (FSH) | Stimulated by GnRH; Inhibited by inhibin, estrogen, testosterone | Ovaries/testes: stimulates gamete production | Hypo: Failure of sexual maturation |
Luteinizing Hormone (LH) | Stimulated by GnRH; Inhibited by estrogen, progesterone, testosterone | Ovaries: triggers ovulation, hormone production; Testes: stimulates testosterone production | Hypo: Failure of sexual maturation |
Prolactin (PRL) | Inhibited by PIH (dopamine); Stimulated by decreased PIH, estrogen, suckling | Breast: promotes milk production | Hypo: Poor milk production; Hyper: Inappropriate milk production, infertility |
