 Back
BackThe Integumentary System: Structure and Function
Study Guide - Smart Notes

The Integumentary System
Overview
The integumentary system consists of the skin and its accessory organs, including hair, nails, and cutaneous glands. It is the body's most exposed organ system and plays a critical role in protection, sensation, and homeostasis. Dermatology is the scientific study and medical treatment of this system.
Skin is the most vulnerable organ, exposed to radiation, trauma, infection, and chemicals.
Inspection of skin, hair, and nails is a significant part of physical exams.
Receives more medical treatment than any other organ system.
Structure of the Skin
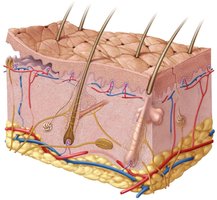
The skin is composed of three main layers:
Epidermis: The outermost layer, primarily protective.
Dermis: The middle layer, providing structural support and housing accessory structures.
Hypodermis: The deepest layer, mainly for fat storage and insulation.
Skin Types
Thick skin: Found on palms, soles, fingers, and toes; epidermis is about 0.5 mm thick.
Thin skin: Covers the rest of the body; epidermis is about 0.1 mm thick.
Functions of the Skin
The skin performs several essential functions:
Resistance to trauma and infection: Keratin and acid mantle provide protection.
Barrier functions: Waterproofing, UV protection, and defense against chemicals.
Vitamin D synthesis: Initiates the first step in vitamin D production.
Sensation: Contains extensive sensory receptors.
Thermoregulation: Thermoreceptors and blood vessel adjustments regulate temperature.
Nonverbal communication: Skin markings, acne, scars, and birthmarks convey information.
Transdermal absorption: Allows certain drugs to be administered through the skin.
Epidermis
Structure and Cell Types
The epidermis is a keratinized stratified squamous epithelium lacking blood vessels and relying on diffusion for nutrients. It contains five main cell types:
Stem cells: Undifferentiated cells in the stratum basale that give rise to keratinocytes.
Keratinocytes: The majority of epidermal cells, synthesizing keratin.
Melanocytes: Located in the stratum basale, produce melanin pigment.
Tactile (Merkel) cells: Touch receptor cells in the basal layer.
Dendritic (Langerhans) cells: Macrophages found in the stratum spinosum and granulosum.
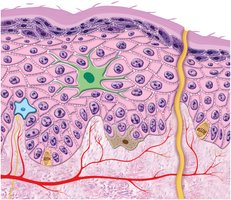
Layers of the Epidermis
The epidermis is organized into distinct layers:
Stratum basale: Single layer of cuboidal/columnar stem cells and keratinocytes; contains melanocytes and tactile cells.
Stratum spinosum: Several layers of keratinocytes; thickest layer in most skin; contains dendritic cells.
Stratum granulosum: 3-5 layers of flat keratinocytes; contains keratohyalin granules and lamellar granules for waterproofing.
Stratum lucidum: Thin, translucent layer seen only in thick skin; densely packed keratinocytes with eleidin.
Stratum corneum: Up to 30 layers of dead, scaly, keratinized cells; forms a durable, protective surface.
Life History of Keratinocytes
Keratinocytes are produced in the stratum basale and pushed upward as new cells form.
Mitosis requires abundant oxygen and nutrients.
Cells flatten and produce lamellar granules as they move upward.
Keratinocyte life cycle is about 30-40 days, faster in injured or stressed skin.
Epidermal Water Barrier
The water barrier forms between the stratum granulosum and stratum spinosum, consisting of lipids, tight junctions, and insoluble proteins.
Prevents dehydration by retaining water.
Cells above the barrier die and exfoliate as dander.
Dermis
Structure and Components
The dermis is a connective tissue layer beneath the epidermis, ranging from 0.2 mm to 4 mm thick.
Composed mainly of collagen, elastic fibers, reticular fibers, and fibroblasts.
Contains blood vessels, sweat glands, sebaceous glands, and nerve endings.
Hair follicles and nail roots are embedded in the dermis.
Piloerector muscles cause goose bumps in response to stimuli.
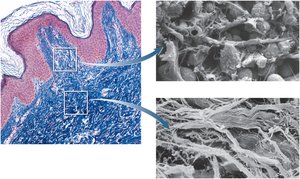
Dermal Layers
The dermis is divided into two main layers:
Papillary layer: Superficial zone of areolar tissue near dermal papillae; allows mobility of defense cells and is rich in small blood vessels.
Reticular layer: Deeper, thicker layer of dense, irregular connective tissue; stretch marks (striae) result from tears in collagen fibers.
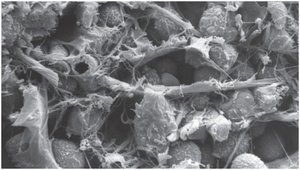

Hypodermis
Structure and Function
The hypodermis, or subcutaneous tissue, lies beneath the dermis and contains more areolar and adipose tissue.
Pads the body and binds skin to underlying tissues.
Highly vascular, making it suitable for drug injections.
Subcutaneous fat serves as an energy reservoir and provides thermal insulation.
Fat layer is about 8% thicker in women.
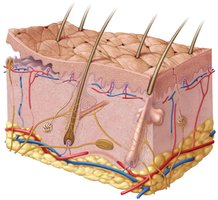
Summary Table: Layers of the Skin
Layer | Main Components | Functions |
|---|---|---|
Epidermis | Keratinocytes, melanocytes, stem cells, tactile cells, dendritic cells | Protection, waterproofing, sensation, vitamin D synthesis |
Dermis | Collagen, elastic fibers, blood vessels, glands, nerve endings | Structural support, sensation, thermoregulation, housing hair/nail roots |
Hypodermis | Areolar and adipose tissue, blood vessels | Padding, energy storage, thermal insulation, drug absorption |
Key Terms and Concepts
Keratin: A tough, fibrous protein providing strength and waterproofing.
Melanin: Pigment produced by melanocytes, responsible for skin color.
Dermal papillae: Fingerlike projections forming fingerprints and increasing surface area for nutrient exchange.
Lamellar granules: Organelles in keratinocytes releasing lipids for waterproofing.
Striae: Stretch marks caused by tearing of dermal collagen fibers.
Equations and Scientific Principles
Surface Area of Skin:
Percentage of Body Weight:
Examples and Applications
Transdermal drug delivery: Medications such as nicotine patches utilize the skin's absorption properties.
Thermoregulation: Vasoconstriction reduces blood flow to skin, conserving heat; vasodilation increases blood flow, releasing heat.
Nonverbal communication: Skin conditions like acne or scars can convey health status or emotional state.
Additional info:
Calluses and corns are examples of increased keratinocyte proliferation in response to mechanical stress.
Dandruff consists of exfoliated dead cells from the stratum corneum.
