 Back
BackThe Integumentary System: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

The Integumentary System
Overview and Components
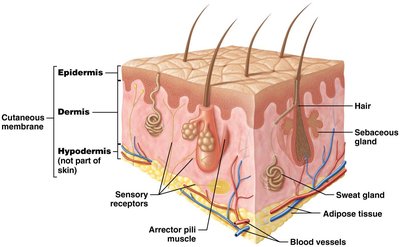
The integumentary system is the body's largest organ system, consisting of the skin and its accessory structures, including hair, nails, and glands. It serves as a protective barrier and plays vital roles in sensation, thermoregulation, excretion, and synthesis of essential molecules.
Skin (cutaneous membrane): Comprises 10–15% of total body weight.
Two main regions:
Epidermis: Keratinized stratified squamous epithelium; avascular.
Dermis: Loose connective tissue (CT) and dense irregular CT; vascular.
Hypodermis: Also called superficial fascia or subcutaneous fat; not part of skin, anchors skin to deeper structures; composed of loose CT and adipose tissue; vascular.
Accessory structures: Sweat glands, sebaceous glands, hair, nails.
Sensory receptors: Detect heat, cold, pain, and pressure.
Arrector pili muscles: Small bands of smooth muscle associated with hair.
Functions of the Integumentary System
The integumentary system performs several essential functions for maintaining homeostasis and overall health.
Protection: Shields against mechanical trauma, pathogens, and environmental hazards.
Sensation: Sensory receptors perceive changes in internal and external environments.
Thermoregulation: Maintains stable internal temperature via negative feedback loops.
Excretion: Eliminates waste products and toxins through sweat.
Synthesis: Produces vitamin D and its active form, calcitriol, necessary for calcium absorption.
Thermoregulation: Negative Feedback Mechanisms
Thermoregulation is achieved through negative feedback loops that respond to changes in body temperature.
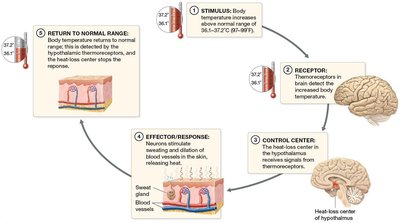
When body temperature is above normal:
Thermoreceptors detect increased temperature.
Hypothalamus (control center) stimulates sweating and vasodilation of dermal vessels.
Body temperature returns to normal; feedback reduces output to glands and vessels.
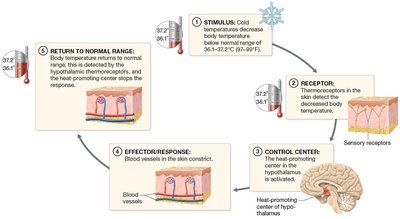
When body temperature is below normal:
Thermoreceptors detect decreased temperature.
Hypothalamus stimulates vasoconstriction, decreased sweating, and shivering.
Body temperature returns to normal; feedback reduces output to vessels and muscles.
Vitamin D Synthesis
Vitamin D is synthesized in the skin upon exposure to UV light, which converts a precursor molecule to vitamin D3 (cholecalciferol). This is further processed in the liver and kidneys to form calcitriol, a hormone essential for calcium absorption in the small intestine.
Calcium (Ca++): Necessary for nerve function, muscle contraction, and bone health.
Structure of the Skin
The Epidermis
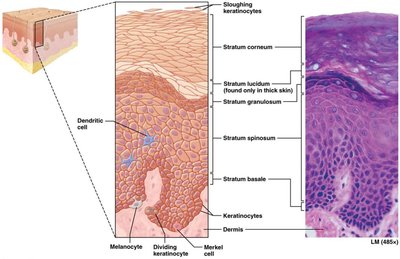
The epidermis is the most superficial region of the skin, composed primarily of keratinocytes that produce keratin, a protective protein. It is organized into five distinct layers (strata):
Stratum basale (germinativum): Deepest layer; most metabolically and mitotically active; produces keratin and vitamin D precursors.
Stratum spinosum: Close to blood supply; metabolically and mitotically active.
Stratum granulosum: Three to five layers; cells filled with keratin, providing water resistance.
Stratum lucidum: Narrow layer of clear, dead keratinocytes; found only in thick skin.
Stratum corneum: Outermost layer; several layers of dead, flattened cells; sloughed off mechanically.
Keratinocyte Life Cycle
Keratinocytes are replaced by mitosis in the stratum basale and spinosum. As they divide, cells are pushed into more superficial layers, completing the cycle in 40–50 days.
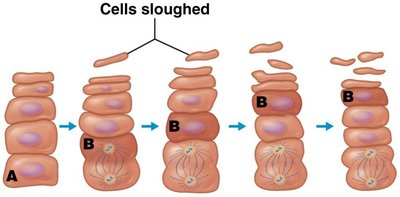
Other Cells of the Epidermis
Dendritic (Langerhans) cells: Located in stratum spinosum; phagocytes of the immune system.
Tactile (Merkel) cells: Located in stratum basale; sensory receptors for light touch.
Melanocytes: Located in stratum basale; produce melanin, the skin pigment.
Thick and Thin Skin
Skin is classified as thick or thin based on the number of epidermal layers and presence of accessory structures.
Thick skin: All five epidermal layers; thick stratum corneum; no hair follicles; many sweat glands.
Thin skin: Four layers (no stratum lucidum); many hair follicles, sweat glands, and sebaceous glands.
Callus: Additional layers of stratum corneum formed due to repetitive pressure.
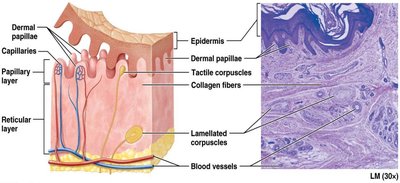
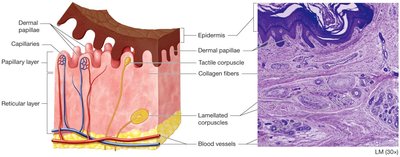
The Dermis
The dermis is a highly vascular layer beneath the epidermis, providing blood supply, sensory receptors, and anchoring the epidermis.
Papillary layer: Composed of loose CT; contains dermal papillae, capillary loops, and tactile (Meissner) corpuscles for light touch.
Reticular layer: Deepest, thicker layer; dense irregular CT with collagen and elastic fibers; rich in proteoglycans; contains lamellated (Pacinian) corpuscles for pressure and vibration, blood vessels, sweat glands, hair, sebaceous glands, and adipose tissue.
Skin Markings and Wrinkles
Skin markings such as epidermal ridges enhance gripping ability and are genetically determined. Wrinkles result from age-related decreases in collagen, elastic fibers, proteoglycans, and adipose tissue, accelerated by UV exposure and smoking.
Delay wrinkles: Avoid sun, use sunscreen, hydrate, and avoid smoking.
Wrinkle treatments: Botox, fillers, topical creams (limited effectiveness).
Skin Color and Pigmentation
Determinants of Skin Color
Skin color is determined by three main pigments:
Melanin: Produced by melanocytes; protects keratinocyte DNA from UV-induced mutations; amount produced varies among individuals.
Carotene: Ingested from yellow-orange vegetables; imparts yellowish color to stratum corneum.
Hemoglobin: Red blood cells; coloration depends on blood flow to dermis.
Skin Color as a Diagnostic Tool
Erythema: Increased blood flow (redness).
Pallor: Decreased blood flow (paleness).
Cyanosis: Low oxygenated blood (bluish color).
Jaundice: Yellow-orange color due to buildup of red blood cell breakdown products.
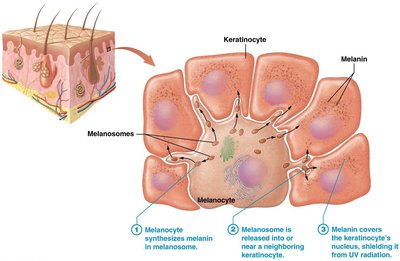
Melanin Production and Function
Melanin is produced in melanosomes within melanocytes and transferred to keratinocytes, where it shields DNA from UV radiation. Melanin synthesis increases with UV exposure but degrades after a few days, requiring replacement.
Common Variations of Pigmentation
Freckle: Small area of increased melanin production.
Mole (nevus): Area of increased melanocyte proliferation.
Albinism: Lack of pigmentation due to absence of tyrosinase enzyme.
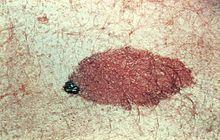
Pseudoscience Exposed: Tanning
There is no such thing as a healthy tan. Both UVA and UVB rays damage DNA, age skin, and increase risk of skin cancer.
Accessory Structures: Hair, Nails, and Glands
Hair
Hair (pili) is derived from epithelium and covers most of the body except thick skin, lips, and parts of external genitalia. It protects against environmental hazards and aids in sensation.
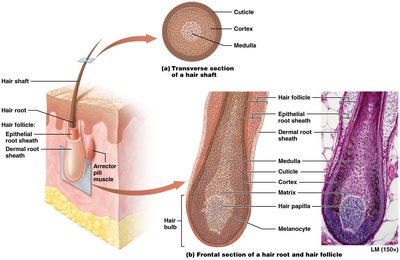
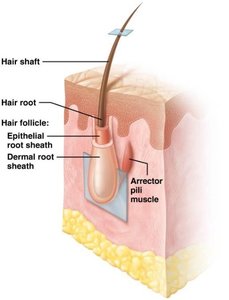
Structure: Stratified squamous keratinized epithelium.
Shaft: Projects from skin surface; composed of dead keratinized cells.
Root: Embedded in dermis; surrounded by sensory neurons; contains hair papilla (blood vessels).
Hair bulb: Root and hair papilla; contains living epithelial cells.
Matrix: Actively dividing keratinocytes at base of root.
Three regions: Inner medulla (soft keratin), middle cortex (hard keratin), outer cuticle (hard keratin).
Arrector pili muscles: Cause piloerection (goosebumps).

Hair Pigment and Texture
Melanin: Determines hair color; blond (little melanin), black (much melanin), red (special pigment with iron), gray/white (less melanin with aging).
Nails
Nails are composed of stratified squamous epithelium filled with hard keratin. They safeguard fingertips and act as tools.
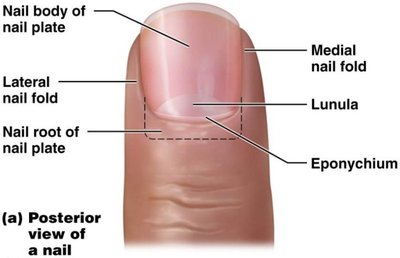
Nail plate: Sits atop nail bed.
Lunula: Half-moon shaped region of proximal nail plate.
Eponychium: Cuticle.
Hyponychium: Stratum corneum under free edge of nail.
Glands
The skin contains several types of glands:
Sweat (sudoriferous) glands:
Eccrine: Widespread; produce mostly water, wastes, electrolytes.
Apocrine: Axillary and anal regions; functional at puberty; odoriferous; associated with hair follicle.
Modified sweat glands: Ceruminous (ear canal, cerumin), mammary (milk).
Sebaceous glands: Produce oily sebum; found in thin skin; create hydrophobic barrier.
Clinical Relevance: Pathologies and Disorders
Acne Vulgaris
Acne is caused by accumulation of sebum and dead cells within sebaceous glands, forming comedones (blackheads). Infection with Propionibacterium acnes leads to inflammation and pustules (pimples), which may cause scarring. Male sex hormones contribute to acne development, especially in puberty.
Wounds and Burns
Wounds are disruptions in skin integrity, involving the epidermis, dermis, or deeper tissues. Types include lacerations (cuts/tears) and burns (first, second, third degree).
Skin Cancer
Skin cancer is caused by mutations in DNA leading to uncontrolled cell division and tumor formation. Tumors may metastasize, spreading to other tissues and organs.
Basal cell carcinoma: Most common; arises from keratinocytes in stratum basale.
Squamous cell carcinoma: Second most common; cancer of keratinocytes in stratum spinosum.
Malignant melanoma: Cancer of melanocytes; highly metastatic.
ABCDE Rule for Melanoma Detection
A: Asymmetrical shape
B: Border irregularity
C: Color (blue-black or varied)
D: Diameter (>6 mm)
E: Evolving shape and size
Summary Table: Layers of the Skin
Layer | Location | Main Features |
|---|---|---|
Epidermis | Superficial | Keratinized stratified squamous epithelium; avascular; five strata |
Dermis | Deep to epidermis | Loose and dense irregular CT; vascular; papillary and reticular layers |
Hypodermis | Deep to dermis | Loose CT and adipose; anchors skin; not part of skin |
Summary Table: Skin Cancer Types
Type | Origin | Features |
|---|---|---|
Basal cell carcinoma | Stratum basale keratinocytes | Most common; rarely metastasizes |
Squamous cell carcinoma | Stratum spinosum keratinocytes | Second most common; may metastasize |
Malignant melanoma | Melanocytes | Highly metastatic; dangerous |
Additional info: These notes provide a comprehensive overview of the integumentary system, including its structure, functions, accessory structures, pigmentation, and clinical relevance. All images included directly reinforce anatomical and physiological concepts discussed in the text.
