 Back
BackThe Integumentary System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

L
The Integumentary System l
Overview and Components
The integumentary system is the body's primary protective barrier and includes the skin, sweat (sudoriferous) glands, oil (sebaceous) l glands, hair, nails, and subcutaneous tissue. It plays a crucial role in protection, sensation, temperature regulation, and metabolic functions.
Skin: The largest organ, serving as a barrier and regulator.
Sweat glands: Control body temperature and excrete waste
11
s.
Oil glands: Lubricate and protect skin and hair.
Hair: Provides protection and sensory input.
Nails: Protect fingertips and enhance sensation.
Subcutaneous tissue: Anchors skin, absorbs shock, and insulates.
Skin Structure
Layers of the Skin
The skin consists of two main layers:
Epidermis: Outermost layer, composed of epithelial tissue, avascular.
Dermis: Underlies the epidermis, made of dense connective tissue, vascular.
The subcutaneous tissue (hypodermis) is not part of the skin but is included in the system due to its functions.
Anchors skin to muscles
Shock absorption and insulation
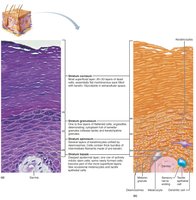
Epidermis
Cell Types
The epidermis is primarily keratinized stratified squamous epithelium and contains four main cell types:
Keratinocytes: Produce keratin, the protein that gives skin its protective properties.
Melanocytes: Produce melanin pigment, protecting against UV damage.
Dendritic (Langerhans) cells: Immune cells that patrol and activate immune responses.
Tactile epithelial (Merkel) cells: Sensory receptors for touch.
Layers of the Epidermis
The epidermis is organized into distinct layers (strata):
Stratum basale: Deepest, mitotically active, contains melanocytes.
Stratum spinosum: Several layers thick, contains pre-keratin filaments and dendritic cells.
Stratum granulosum: Keratinization begins, cells flatten, accumulate granules.
Stratum lucidum: Only in thick skin, clear layer of dead keratinocytes.
Stratum corneum: Outermost, 20–30 rows of dead, keratinized cells.
Dermis
Structure and Layers
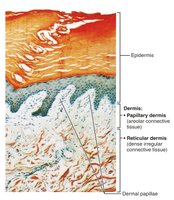
The dermis is strong, flexible connective tissue containing fibroblasts, macrophages, mast cells, and white blood cells. It houses nerves, blood vessels, lymphatics, hair follicles, oil, and sweat glands.
Papillary dermis: Superficial, areolar connective tissue, contains dermal papillae with capillaries and sensory receptors.
Reticular dermis: Deep, dense irregular connective tissue, provides strength and elasticity.
Dermal Modifications
Friction ridges: Enhance grip and touch, form fingerprints.

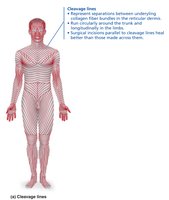
Cleavage (tension) lines: Parallel collagen fibers, important for surgical incisions.
Flexure lines: Dermal folds at joints, visible on hands and feet.

Clinical Aspects
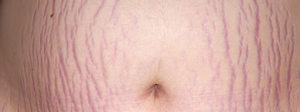
Striae (stretch marks): Dermal tears from extreme stretching.
Blisters: Fluid-filled pockets separating epidermal and dermal layers.
Skin Color
Pigments. ''
Skin color is determined by three main pigments:
Melanin: Produced by melanocytes, shields DNA from UV.
Carotene: Yellow-orange pigment, accumulates in stratum corneum and subcutaneous tissue.
Hemoglobin: Gives pinkish hue to fair skin.
Clinical Color Changes
Cyanosis: Bluish color, low oxygenation.
Pallor: Pale color, stress or anemia.
Erythema: Redness, inflammation or fever.
Jaundice: Yellow color, liver disorders.
Bruises (hematomas): Blood leakage under skin.
Hair
Structure and Function
Hair consists of dead, keratinized cells and is produced by hair follicles. Functions include protection, sensation, and filtering.
Root: Within scalp, keratinization ongoing.
Shaft: Extends above scalp, keratinization complete.
Medulla: Central core.
Cortex: Surrounds medulla.
Cuticle: Outer layer.
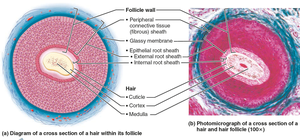
Hair Follicle
Follicle wall: Peripheral connective tissue sheath, glassy membrane, epithelial root sheath.
Hair bulb: Expanded area at deep end, contains hair matrix (actively dividing cells).
Arrector pili: Smooth muscle causing "goose bumps".
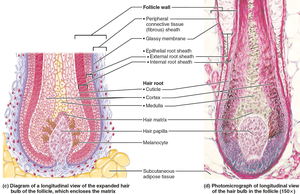
Types and Growth
Vellus hair: Fine, pale body hair.
Terminal hair: Coarse, long hair (scalp, eyebrows, pubic regions).
Clinical Aspects
Hirsutism: Excessive hair growth in females, often due to androgen excess.
Baldness: Age-related hair loss, male pattern baldness is hormone and genetically influenced.
Telogen effluvium: Abrupt hair thinning due to stress or illness.
Nails
Structure and Function
Nails are scale-like modifications of the epidermis containing hard keratin. They protect the distal phalanges and enhance sensation.
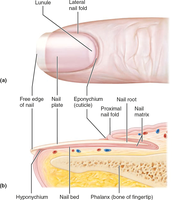
Root: Embedded in skin.
Nail plate/body: Visible attached portion.
Free edge: Extends beyond finger.
Nail bed: Epidermis under nail plate.
Nail matrix: Responsible for nail growth.
Nail folds: Skin folds overlapping nail border.
Cuticle (eponychium): Projects onto nail surface.
Hyponychium: Area under free edge.
Lunule: White, thickened nail matrix.
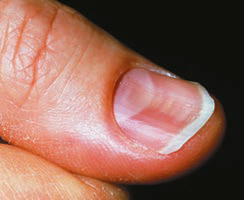
Clinical Aspects
Koilonychia (spoon nail): Outward concavity, may signal iron deficiency.
Beau’s lines: Horizontal lines, may indicate severe illness.
Skin Appendages: Glands
Sweat Glands
Eccrine (merocrine) glands: Most numerous, thermoregulation, secrete watery sweat.
Apocrine glands: Located in axillary/anogenital areas, secrete viscous sweat, function as scent glands.
Modified apocrine glands: Ceruminous (earwax) and mammary (milk) glands.
Oil (Sebaceous) Glands
Holocrine glands: Secrete sebum into hair follicles.
Functions: Lubricate skin/hair, bactericidal properties.
Clinical Aspects
Acne: Infectious inflammation of sebaceous glands.
Seborrhea (cradle cap): Overactive sebaceous glands in infants.
Functions of Skin
Protection
Skin acts as a barrier against microorganisms, chemicals, and physical damage.
Chemical barriers: Sweat, sebum, acid mantle, melanin.
Physical barriers: Keratinized cells, glycolipids.
Biological barriers: Dendritic cells, macrophages.
Body Temperature Regulation
Insensible perspiration: Baseline sweat production.
Sensible perspiration: Increased sweat for cooling.
Vasoconstriction: Reduces heat loss in cold environments.
Cutaneous Sensations
Sensory receptors in skin detect touch, pressure, pain, and temperature.
Tactile corpuscles: Touch.
Lamellar corpuscles: Deep pressure.
Hair follicle receptors: Hair movement.
Free nerve endings: Pain.
Metabolic Functions
Vitamin D synthesis: Required for calcium absorption.
Activation of hormones: Keratinocytes convert cortisone to hydrocortisone.
Collagenase production: Aids in collagen turnover.
Blood Reservoir and Excretion
Blood reservoir: Skin holds up to 5% of blood volume.
Excretion: Removal of nitrogenous wastes and salts via sweat.
Skin Disorders: Cancer and Burns
Skin Cancer
Basal cell carcinoma: Most common, least malignant, arises from stratum basale.
Squamous cell carcinoma: Second most common, can metastasize, arises from stratum spinosum.
Melanoma: Most dangerous, arises from melanocytes, highly metastatic.
ABC(D) Rule for Detection
A: Asymmetry
B: Border irregularity
C: Color variation
D: Diameter > 6 mm
E: Evolution (changes over time)
Burns
First-degree: Epidermal damage only.
Second-degree: Epidermal and upper dermal damage, blisters.
Third-degree: Entire skin thickness, nerve destruction, requires grafting.
Rule of Nines
Used to estimate fluid loss and burn severity.
Body divided into 11 sections, each representing 9% of surface area.
Genitals account for 1%.
Developmental Aspects
Embryonic Development
Epidermis: Develops from ectoderm.
Dermis and subcutaneous tissue: Develop from mesoderm.
Lanugo: Fine hair covering fetus, replaced by vellus hair.
Infancy to Adulthood
Vernix caseosa: Protective substance from sebaceous glands.
Milia: Small white spots on newborn skin.
Skin thickens, gland activity increases, acne may develop.
Aging Skin
Epidermal replacement slows: Skin becomes thin, dry, itchy.
Subcutaneous fat and elasticity decrease: Wrinkles, cold intolerance.
Increased cancer risk: Fewer melanocytes and dendritic cells.
Hair thinning: Common with age.
UV protection delays aging: UVA causes aging, UVB causes burning.
